Functions of Antibodies
1/17
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
18 Terms
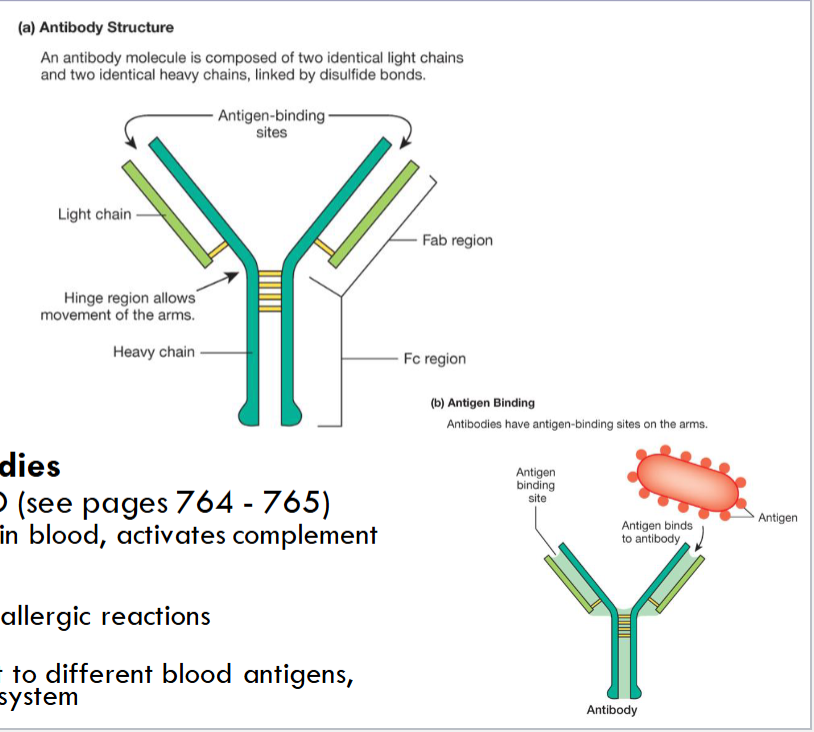
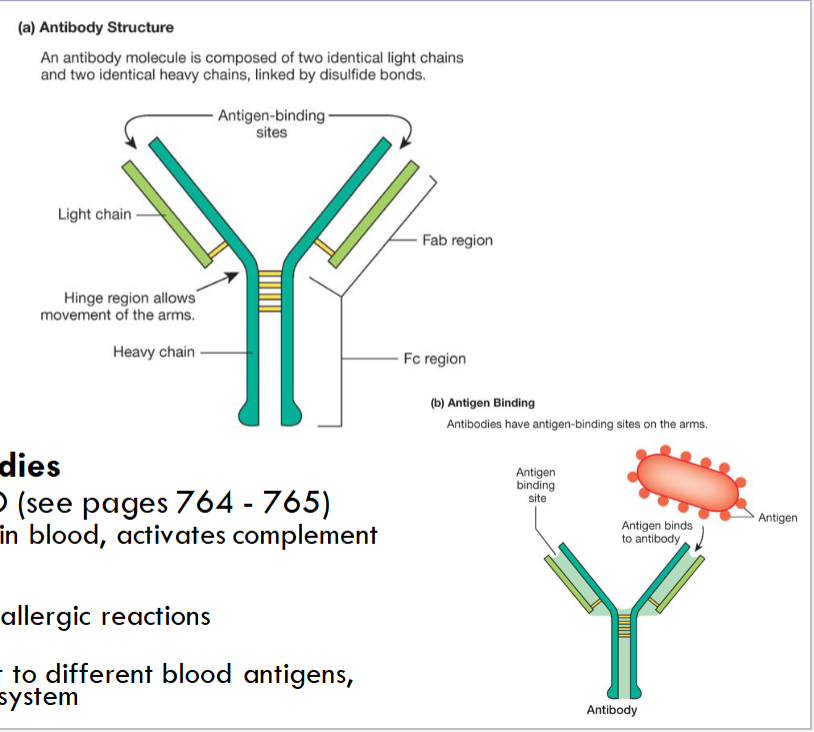
Antigen binding sites are variable
differ based on which antigen they are designed to bind
Fab regions bind to antigens
Fc region binds to phagocytes and activates them
5 classes of antibodies
IgG, IgA, IgE, IgM, IgD
IgG - most abundant in blood, activates complement sys
IgE - associated w/ allergic reactions
IgM - those that react to different blood antigens, activate complement system
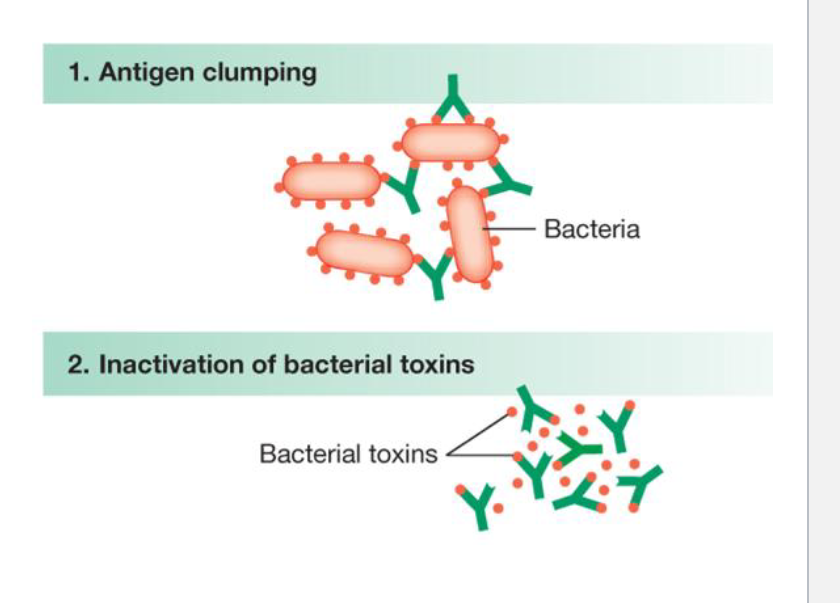
Agglutination
Because of the two binding on each antibody, they can bind two foreign antigens each
this allows antibodies to bind or “glue” foreign antigens into a clump, which immobilizes them so that other immune cells can engulf and destroy them
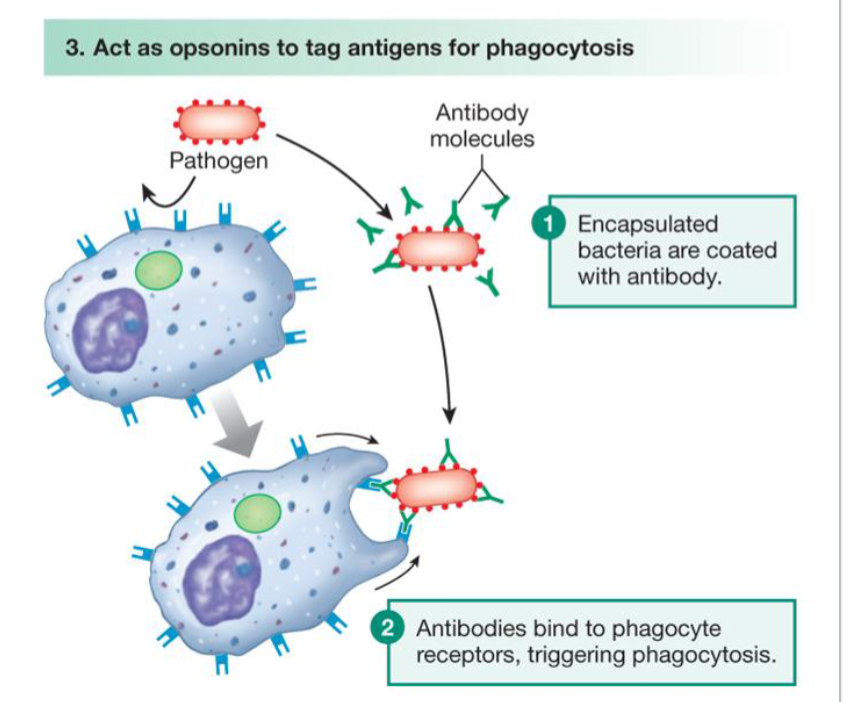
Opsonization
Enhancement of immune reaction against bacteria by antibodies or portions of the complement cascade
bacteria coated or “tagged” with antibodies are easier for phagocytes to find and ingest
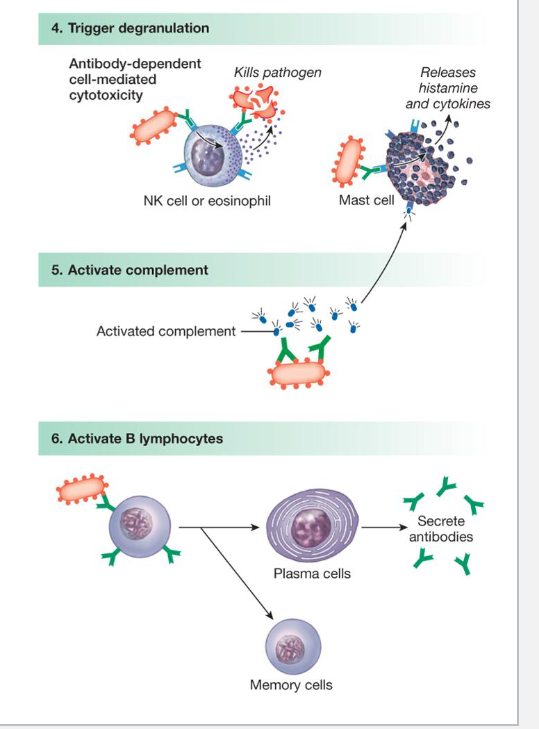
Activate other components of the immune system
Antibodies attached to foreign antigens can trigger the release of cytotoxins from Natural Killer cells or eosinophils or cytokines from Mast cells
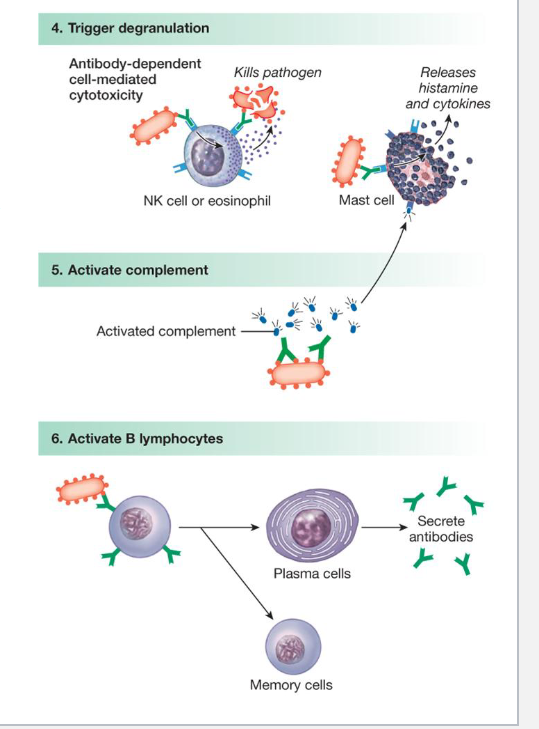
Antibodies can also activate complement proteins
which can create membrane attack complexes
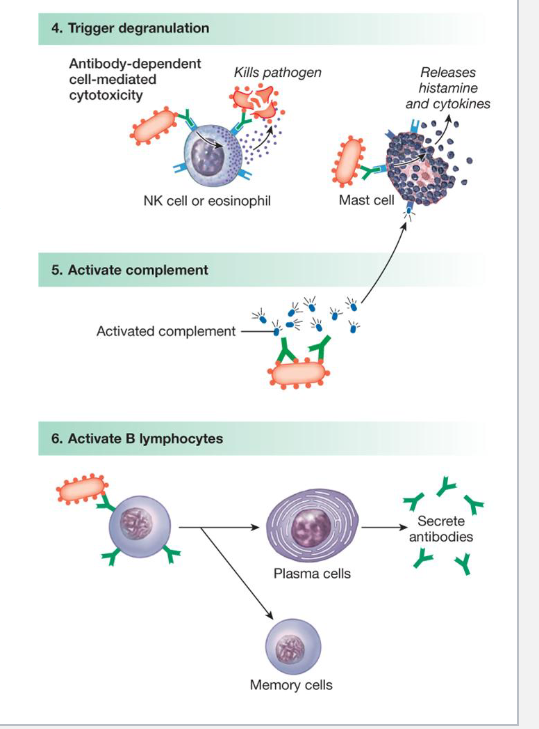
Antibodies attached to B-cells, when triggered by foreign antigens, cause those B-cells to become either ….
plasma cells or memory B-cells
T lymphocytes provide cell mediated immunity
Designed to destroy pathogen-infected cells
this is the primary way viruses are destroyed
→ remember, they must enter cells to reproduce
Any bacteria that enter cells are also targeted
Infected cells display foreign antigens on their MHC class I platforms
→ Killer T-cells seek out, bind to, and destroy these infected
Killer T-cells (aka cytotoxic T cell)
Attack infected cells
→ bind to MHC class I-antigen complex
Killer T-cels destroy infected cell similarly to the Natural Killer Cells mentioned earlier
Secrete perforins
→ form pores in infected cell’s membrane
Secrete granzymes
→ destroy cell’s DNA
→ stimulate apoptosis
Helper T cells
Interact w/ antigen-presenting cells
→ bind to their MHC class II-antigen complexes
Helper T cells become activated
Do not directly attack infected cells
Bind to and stimulate B-cells to reproduce and differentiate
Secrete cytokines to enhance immune response
→ Interferon-gamma
→ colony-stimulating factors
→ interleukins
Interferon-gamma
Activate macrophages
Colony-stimulating factors
Enhance leukocyte production
Interleukins (ex: IL-2)
Activate killer T-cells
Enhance mast cell and eosinophil function
Activate plasma cells to produce antibodies
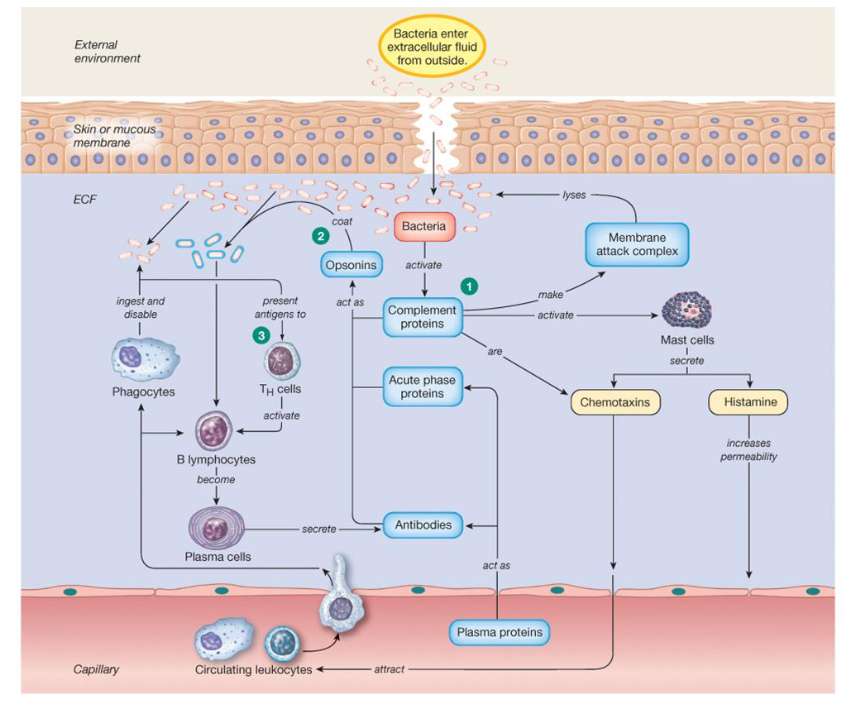
Defenses against bacteria
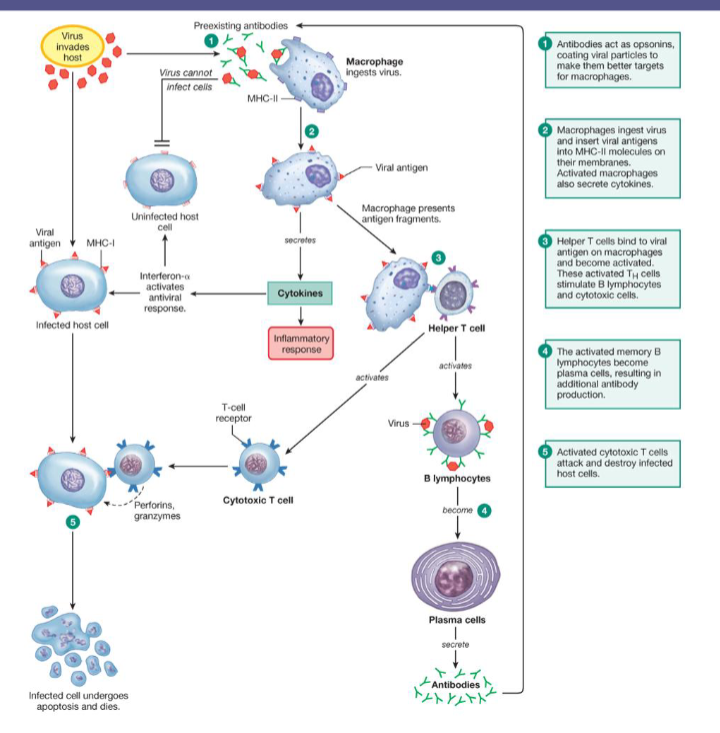
Defenses against viruses

Killer T-cells
B lymphocyte
Immunoglobulins
Opsonization
Killer T cells
Bradykinin