Fluid and Electrolyte Imbalances: Causes, Assessment, and Management Part 2
1/50
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
51 Terms
What is Fluid Volume Excess (FVE)?
An abnormally high volume of body fluid leading to congestive heart failure and pulmonary edema.
What are common causes of Fluid Volume Excess?
Insufficient kidney function, liver issues (cirrhosis), and heart pumping issues.
What are the assessment cues for Fluid Volume Excess?
Edema, shortness of breath (SOB), and elevated head of bed (HOB) positioning.
What is pitting edema?
A type of edema where an indentation remains after pressure is applied, graded from +1 to +4.
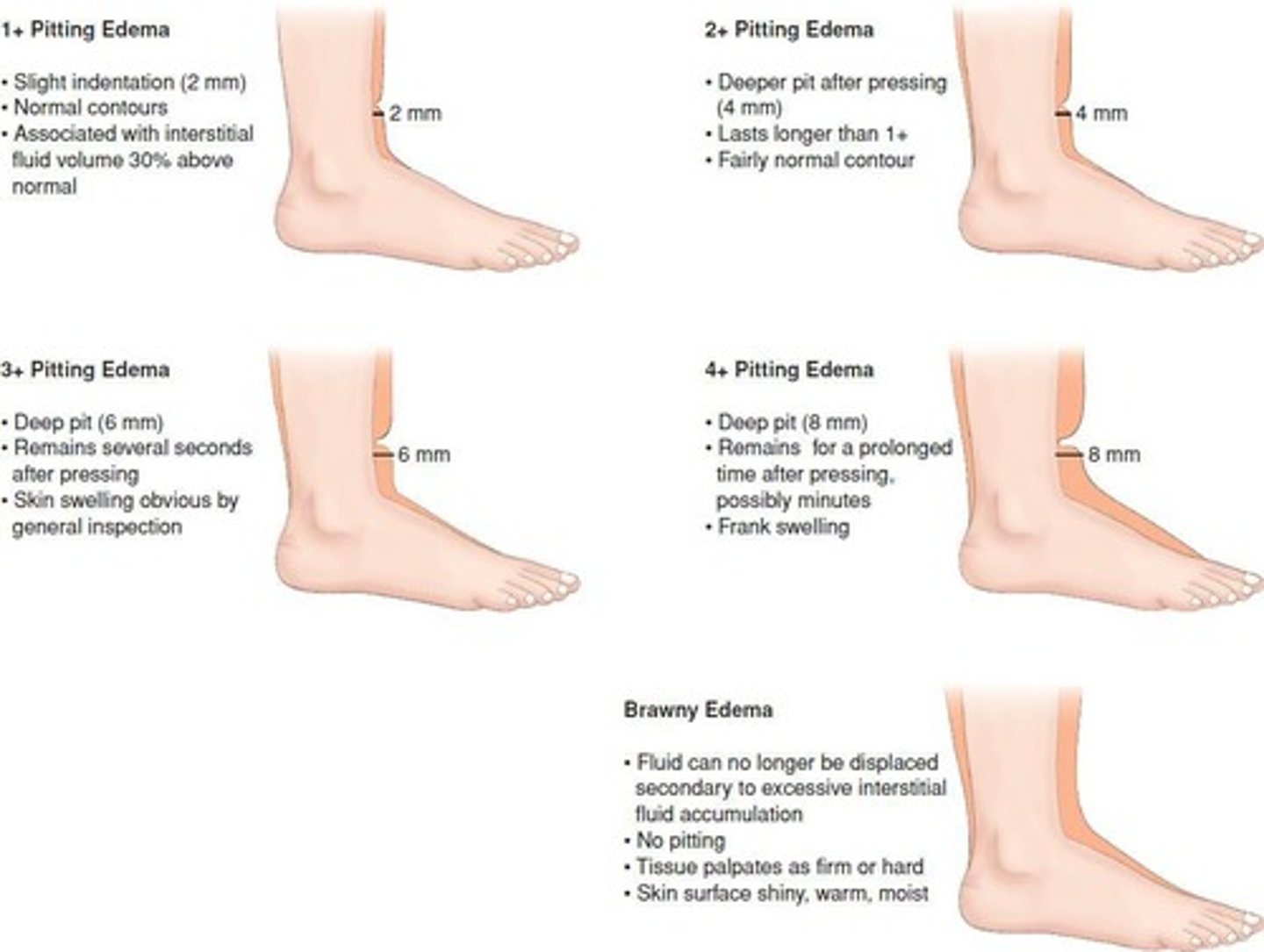
Where is edema most commonly found in patients with Fluid Volume Excess?
Lower extremities, sacral area (in bedridden patients), periorbital area (around eyes), and fingers.
What is the DASH diet?
A dietary approach to stop hypertension, often recommended for patients with Fluid Volume Excess.
What are the vital sign changes associated with Fluid Volume Excess?
Increased blood pressure (BP) and heart rate (HR).
What is the most sensitive indicator of Fluid Volume Excess?
Daily weights.
What laboratory findings indicate Fluid Volume Excess?
Decreased hemoglobin and hematocrit (hemodilution), decreased sodium (dilutional), and decreased BUN.
What are the recommended actions for managing Fluid Volume Excess?
Restrict oral fluids and sodium intake, monitor intake and output (I&O), and administer diuretics as ordered.
What are loop diuretics and their effects?
Diuretics that act on the loop of Henle, causing rapid diuresis and potential hypokalemia.
Give examples of loop diuretics.
Furosemide (Lasix), Bumetanide (Bumex), and Torsemide (Demadex).
What is the role of potassium-sparing diuretics?
They promote sodium excretion while retaining potassium, potentially causing hyperkalemia.
What is hypokalemia and its symptoms?
A condition of low potassium levels, leading to muscle weakness and dysrhythmias.
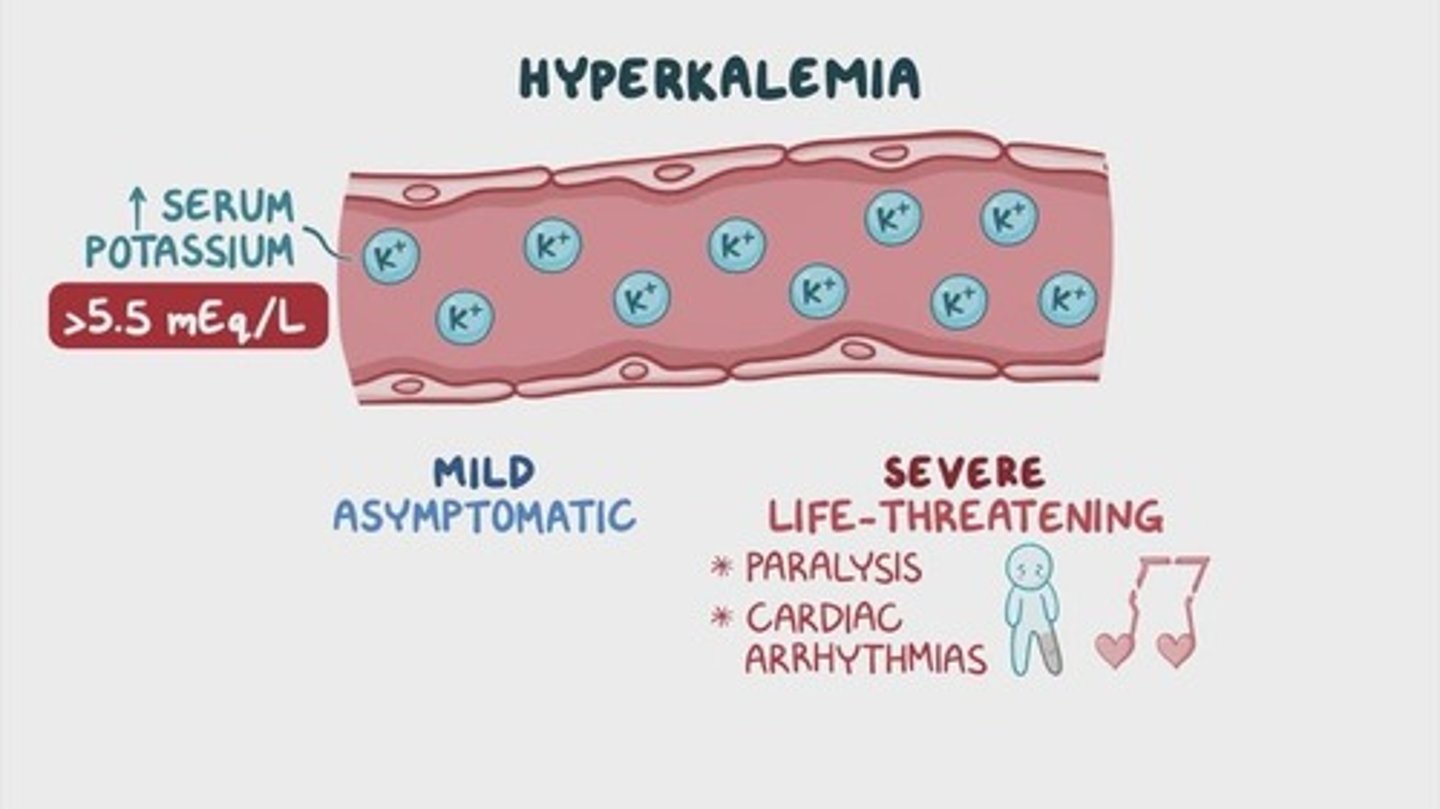
What is hyperkalemia and its potential effects?
A condition of high potassium levels, which can lead to bradycardia and life-threatening dysrhythmias.
What is Fluid Volume Deficit?
An abnormally low volume of body fluid, often resulting from dehydration or hypovolemia.
What are common causes of Fluid Volume Deficit?
Vomiting, diarrhea, hemorrhage, diuretics, and skin trauma.
Who is at risk for Fluid Volume Deficit?
Elderly individuals, NPO or post-operative patients, and those with swallowing difficulties.
What is third spacing in the context of fluid shifts?
Fluid moving from the vascular space into tissues or cavities, often seen in severe burns or pancreatitis.
What are the signs of dehydration?
Hypotension, tachycardia, and narrow pulse pressure.
What patient education should be provided for managing Fluid Volume Excess?
Limit fluid intake as prescribed, follow a low sodium diet, and recognize symptoms like edema and rapid weight gain.
What are common signs of fluid volume deficit in infants and young children?
Altered mental status, decreased level of consciousness, weight loss, dry mucous membranes.
What subjective symptoms indicate fluid volume deficit?
Poor skin turgor, thirst, cool dry skin, weakness, pale skin, fatigue.
What renal symptoms may indicate fluid volume deficit?
Dizziness, oliguria (decreased urine output), muscle cramps, concentrated urine (dark amber).
What objective findings suggest fluid volume deficit?
Increased urine specific gravity, narrow pulse pressure, tachycardia, hypotension, confusion.
What is anuria?
The absence of urine production.
What are the vital signs changes in fluid volume deficit?
Decreased blood pressure and increased heart rate.
What lab findings are expected in fluid volume deficit?
Increased hematocrit (Hct), increased BUN, increased urine specific gravity.
What is the primary action for managing fluid volume deficit?
Encourage oral fluids if able and administer IV fluids as ordered.
What are the functions of sodium (Na⁺) in the body?
Regulates fluid balance, controls blood pressure, essential for nerve impulse conduction.
What is hyponatremia?
A condition where sodium levels are less than 135 mEq/L.
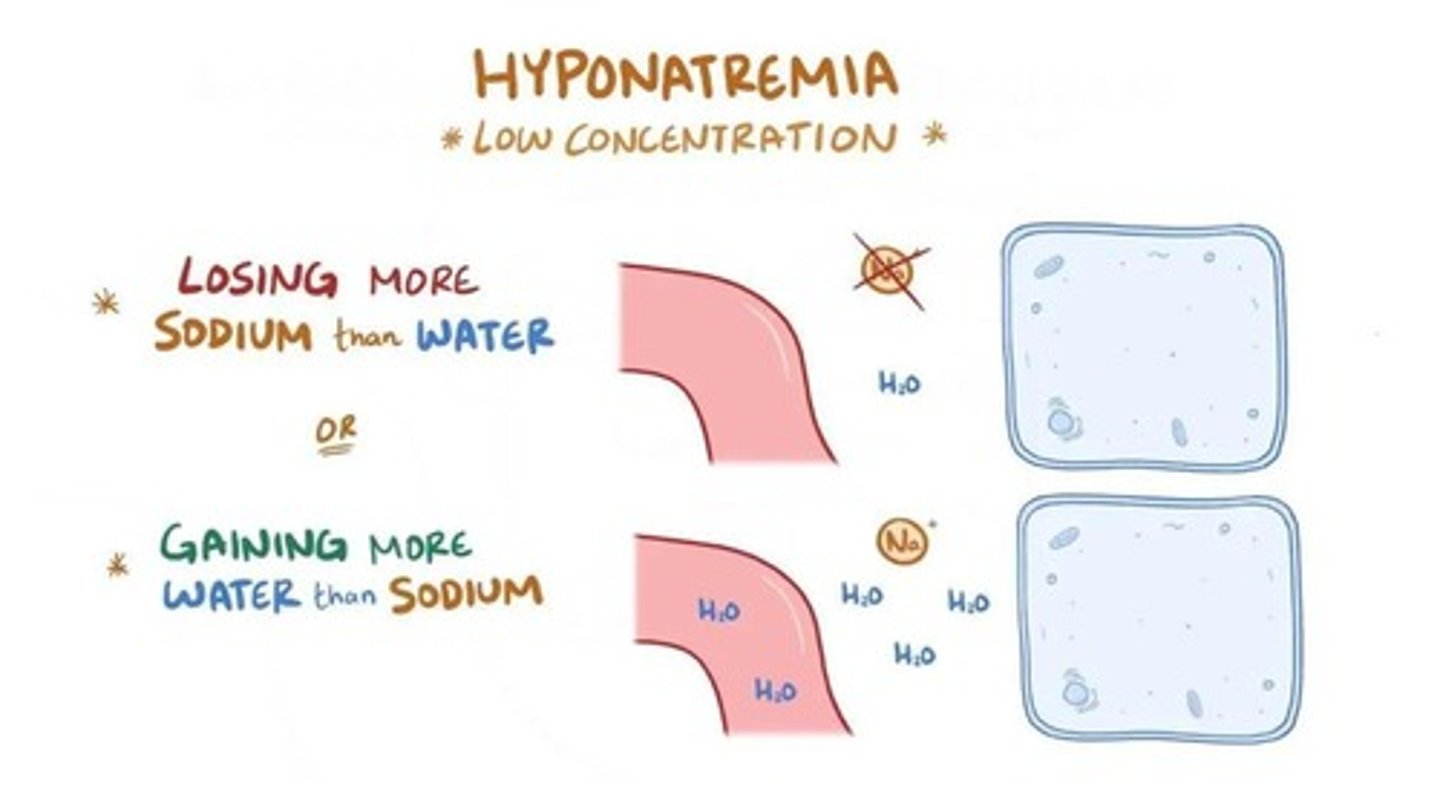
What are the critical levels for hyponatremia?
Critical level is less than 124 mEq/L, which poses a risk for seizures or coma.
What causes hyponatremia?
Sodium loss from diuretics, GI losses, skin losses, or dilution from excess water intake.
What are the clinical manifestations of hyponatremia?
Changes in level of consciousness, muscle weakness, nausea, vomiting.
What is hypernatremia?
A condition where sodium levels are greater than 145 mEq/L.
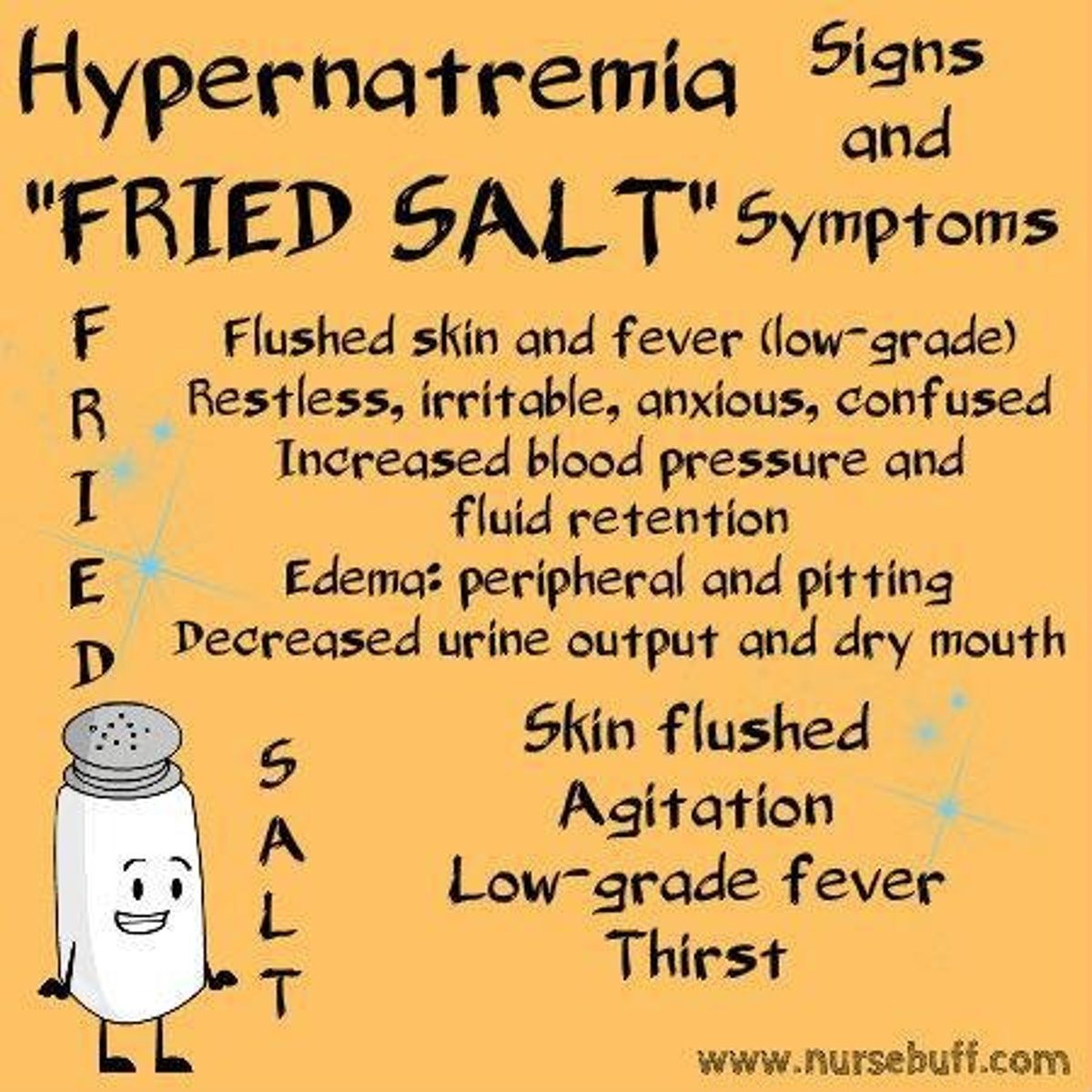
What are the critical levels for hypernatremia?
Critical level is greater than 160 mEq/L, which poses a risk for severe neurologic dysfunction.
What causes hypernatremia?
Water deficit, inadequate water intake, fluid loss, or excess sodium intake.
What are the clinical manifestations of hypernatremia?
Thirst, confusion, weakness, muscle twitching.
What is hypokalemia?
A condition where potassium levels are less than 3.5 mEq/L.
What are the critical levels for hypokalemia?
Critical level is less than 2.5 mEq/L, which poses a risk for life-threatening dysrhythmias.
What are the causes of hypokalemia?
GI losses, excessive sweating, medications like loop diuretics.
What are the clinical manifestations of hypokalemia?
Muscle weakness, leg cramps, dysrhythmias, decreased bowel motility.
What is hyperkalemia?
A condition where potassium levels are greater than 5.0 mEq/L.
What are the critical levels for hyperkalemia?
Critical level is greater than 6.0 mEq/L, which poses a risk for lethal dysrhythmias.
What are the causes of hyperkalemia?
Decreased excretion due to renal failure, increased intake, or shifts out of cells.
What are the clinical manifestations of hyperkalemia?
Cardiac dysrhythmias, muscle weakness, abdominal cramping.
What is the normal range for sodium levels?
135-145 mEq/L.
What is the normal range for potassium levels?
3.5-5.0 mEq/L.
What is the importance of magnesium for potassium absorption?
Magnesium is essential for the absorption of potassium in the body.
What is the recommended daily intake of sodium?
2.3 grams per day.
What are the actions to take for a patient with hyperkalemia?
Stop potassium sources, administer diuretics, and monitor ECG.