Lecture 11, 12, 13
1/31
Earn XP
Description and Tags
T cell subsets
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
32 Terms
why do we need different T cell subsets
diverse type of pathogens
different target sites
different target cells
cell types are classified based on
cytokines that induce differentiation
transcription factors that control gene expression
cytokines produced by the cells
cytokine production by T cells controls (helps) other cells of the immune response
overall T cell response diagram
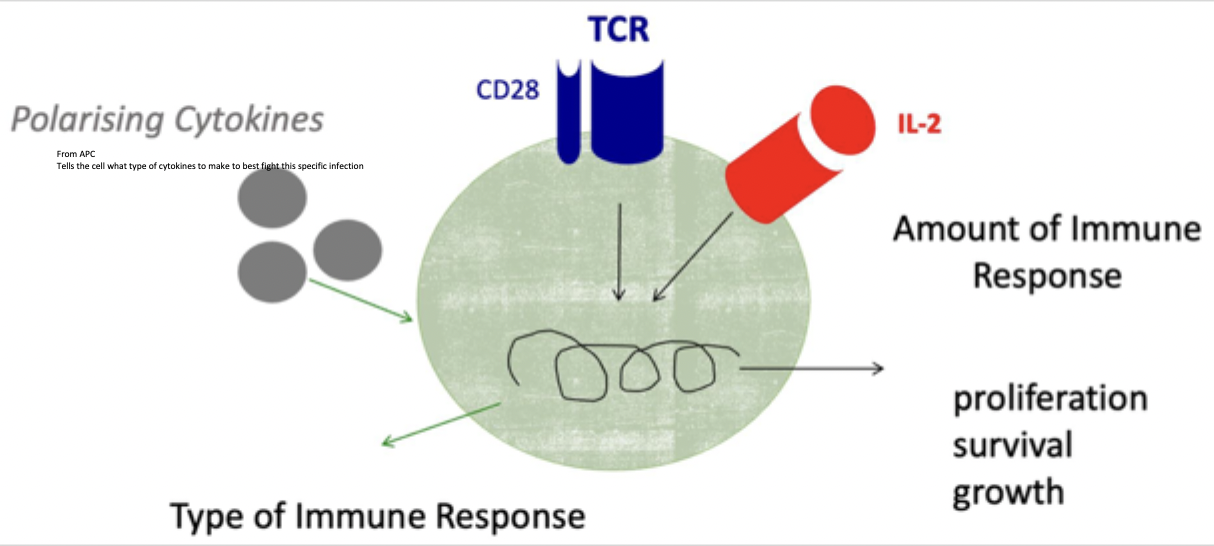
important T cell subsets (223)
Th1 - intracellular pathogens, APC produced IL-12, T cell produces interferon gamma
Th2 - parasite, APC prodiuces IL-4, T cell stimulated to produce IL-5
Th17 - pathogen actvates APC, stimulated to produce IL-23, T cell stimulated to produce IL-17
JAK-STAT signalling
binding of cytokine to receptor = receptor dimerises
this brings receptor associated JAKs in close
JAKs phosphorylate each other on tyrosine residues
activated JAKs phosphorylate receptor
receptor phosphorylation creates binding sites for STATs
STATs bind, get phosphorylated by JAKs, then dissociate
STATs dimerise and translocate to nucleus
Th1 cells activation
IL-12 binds IL-12R and STAT4 dimerises
this causes production of interferon gamma and Tbet transcription factor
Th1 cells positive feedback
Tbet causes transcription of more interferon gamma, more Tbet and IL-12R
IFNgamma causes
increased expression of TLRs on APCs
increased MHC expression
increased chemokine secretion
increased macrophage activation
increased phagocytosis
produced by Th1 cells
Th1 cells overall diagram
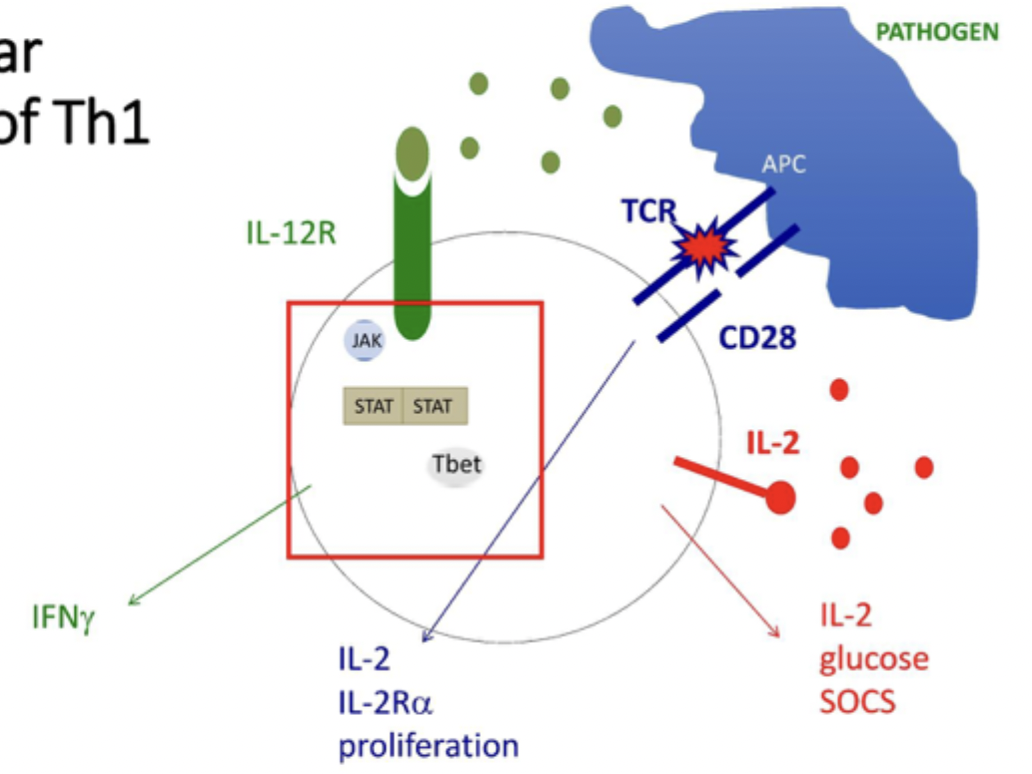
Th2 overall diagram
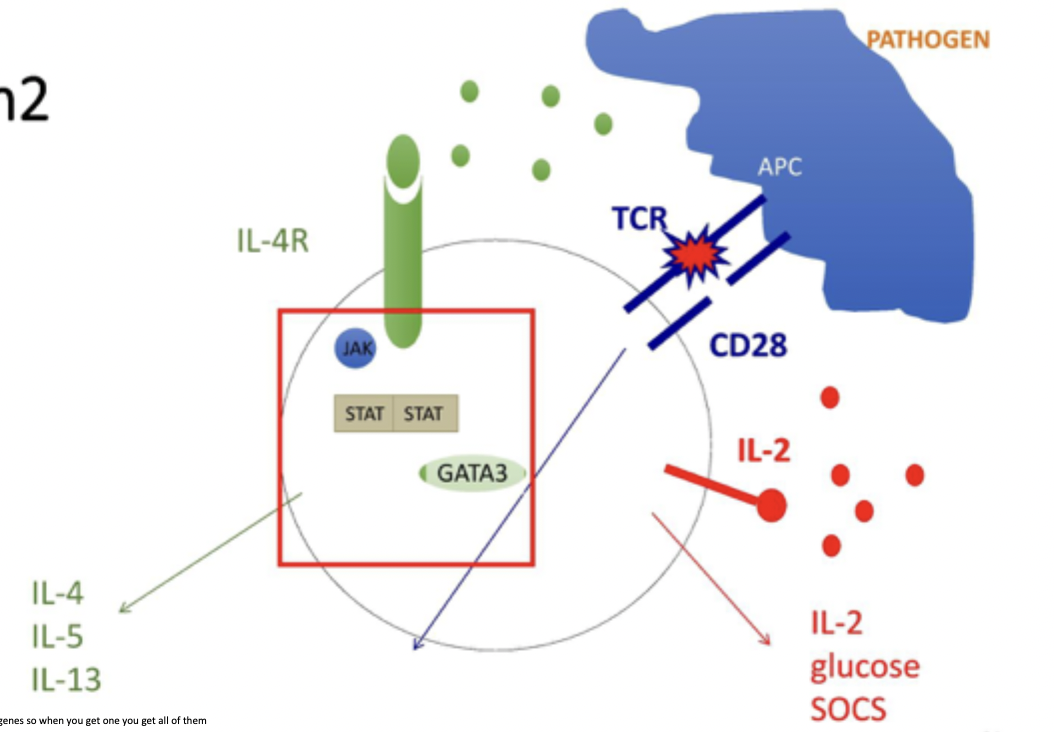
Th2 cells stimulation
IL-4 binds receptor and causes STAT6 to dimerise
causes production of IL-4, IL-5 and IL-13 as well as GATA3 transcription factor
Th2 cells positive feedback
GATA3 causes feedback - get more IL-4,4,13 and GATA3 for more transcription and activation of this pathway
IL-4
activates B cells
enhances IgG and IgE production
inhibits activated macrophages
suppress proinflammatory mediators (IL-1 and TNF)
produced by Th2 cells
Th2 cells and antibody
IL-4 stimulates B cells to make IgE
IL-5 activates mast cells and basophils
IL-13 stimulates mucus production to try and rid the body of the dead parasite
also associated with atopy and allergy
Th17 cells overall diagram
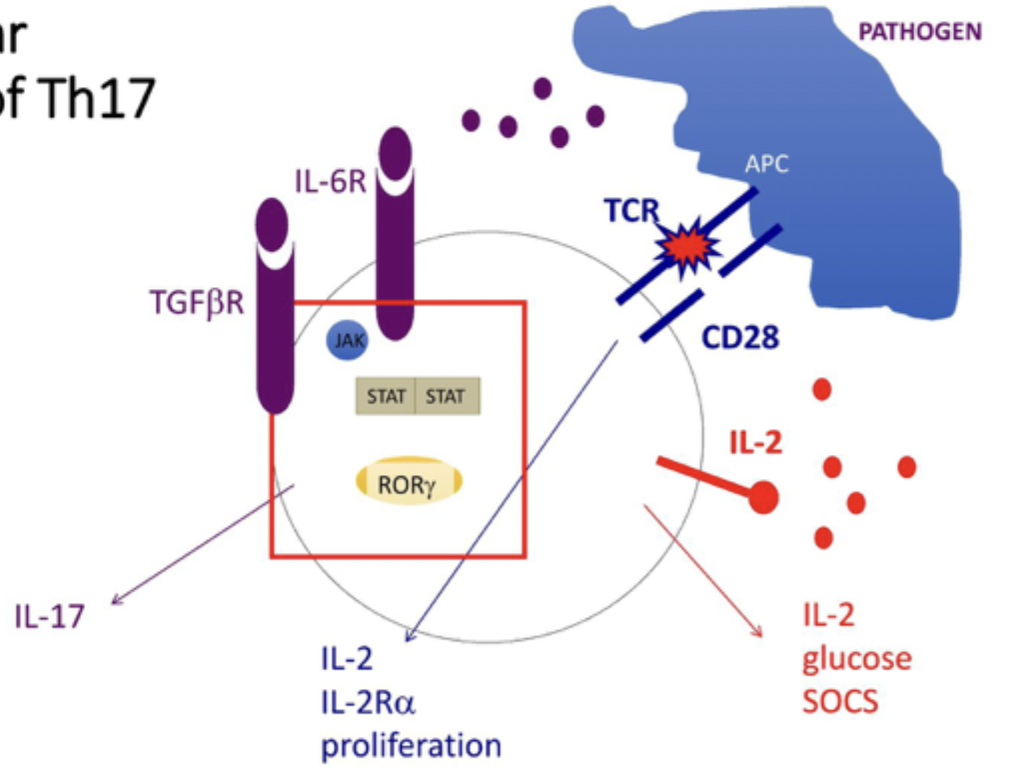
Th17 step 1
through IL6 binding receptor which causes STAT3 to dimerise and TGFbeta binding its receptor as well
causes production of IL-17, IL-21 and its receptor as well as RORgamma transcription factor
Th17 step 2
IL-21 binding its receptor also causes STAT3 to dimerise which causes transcription of IL-17, IL-21 and IL-23 and IL23R
also IL-22 which helps to repair epithelial cells
Th17 cells step 3
IL23 binds its receptor also causin STAT3 to dimerise and produces IL-17 for stability and maintanence
IL-17
promotes recruitment of neutrophils
activates innate immune cells
enhances B cell functions
induces pro-inflammatory cytokines
can promote production of IL-10 to reduce inflammation
produced by Th17 cells
cytokines produced by IL-17 cells
IL-17 - recruits neutrophils and promotes inflammation
IL-22 - stimulate epithelial cells to produce anti-microbial peptides
IL-23 - promotes maintenance of Th17 phenotype
also associated with chronic inflammatory diseases such as MS and IBD
why Th17 cells more complicated
these cells are highly regulated because they have such toxic effects on the body so have to be sure it is needed before activating this pathway
other types of T cell subsets
Th9, Th22, Tfh cells
Th9 cells
transcription factor PU.1
polarised by IL-4 and TGFb, close to Th2 cells
produce IL-9
roles in parasite response, inflammation
Th22 cells
transcription factor AHR
polarised by IL-6 and TNF, close to Th17 cells
produce IL-22
epithelial repair and barrier function
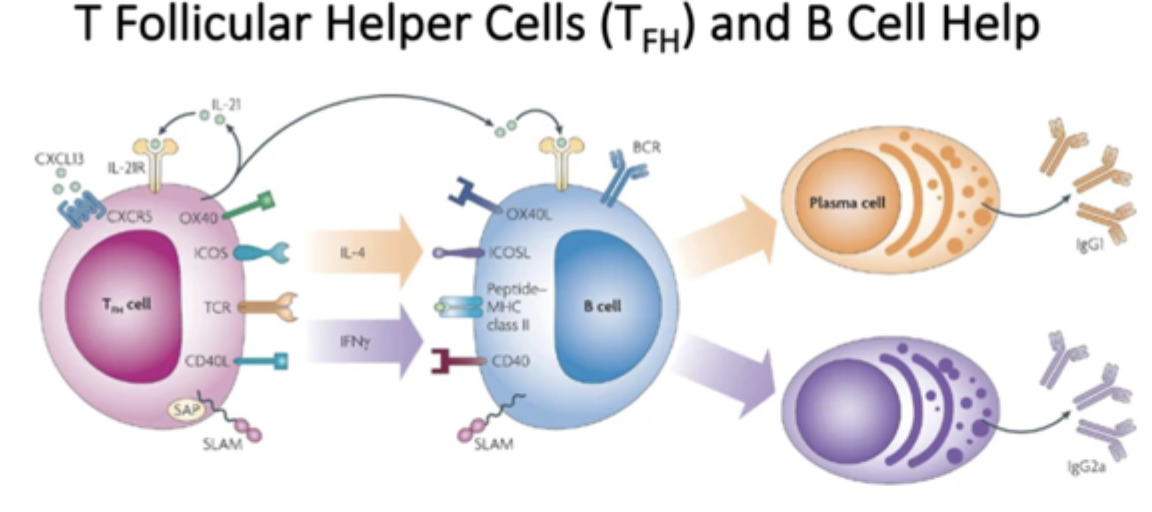
Tfh cells
transcription factor Bcl-6
polairsed by Il-6 and IL-21
produce lots of cytokines, germinal centre - support antibody class switching
Tfh and B cell diagram
defining T cell subsets - transcription factors
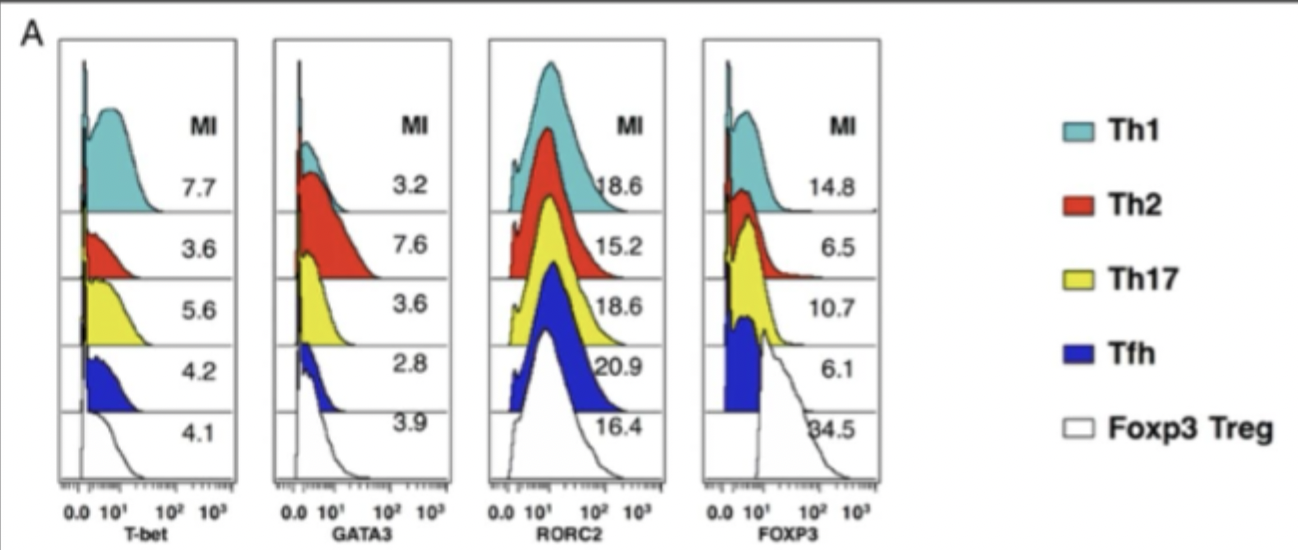
Not super clear cut - where one is expressing something and nothing else is - lots of expression between the different types of cells
Have to think about how you would define what you think is a Th1 cell, Th2 cell etc
Makes sense that these are a bit blurred in an immune response as you need lots of different cells to be doing different things and the response is also changing
T cell subset overlap
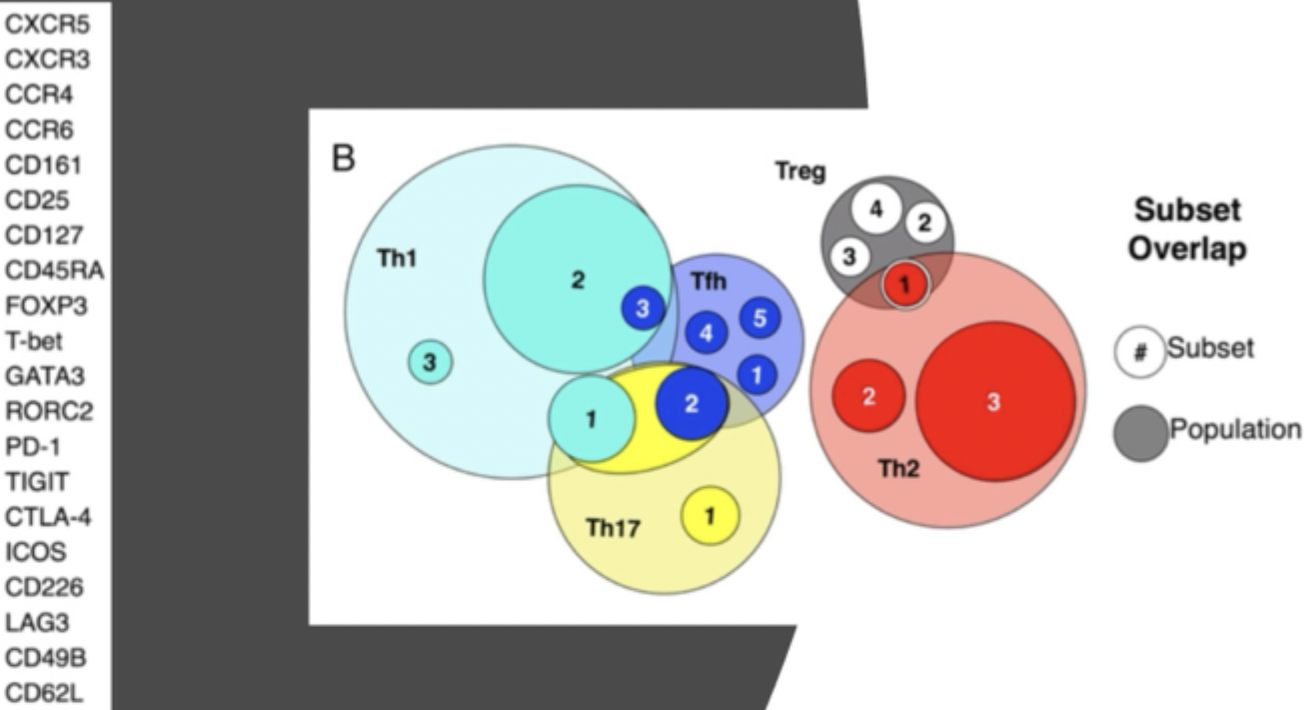
Not looking at what is being produced
Get clusters of cells with similar expression and can class these into subsets
Tfh do lots so lots of overlap
Th2 and Tregs quite separate
If you only look at one thing they look different, but when you start looking at lots of different things you see they have similar things expressed
regulatory T cells overview
immune responses to pathogens cause damage
need to control the scope and size of the immune response
autoreactive cells escape regulation in development - need to control autoimmune responses
types of Tregs
thymic Tregs come from the thymus and are already a Treg
induced Tregs develop from niave T cells in the periphery in response to antigen activation and cytokine signals
Tregs are a type of T cell subset
T cells in thymus can differentiate into
CD8 cells
CD4 cells
CD4 reg
Tregs and CD24