ID ch 34 antimicrobial agents
1/15
Earn XP
Description and Tags
class on march 31st, up to slide 24
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
specificity def + formula
how well does my new test identify infected individuals, vertically down, how many are positive in both gold standard and new test / total positive by gold standard
what is usually used as a gold standard for TB tests
liquid culture
specificity def + formula
how well does my new test identify uninfected individuals, vertically down, how many are negative in both gold standard and new test / total negative by gold standard
PPV long, expl + formula
Positive Predictive Value: if the test is positive, what is the likelihood that the patient is indeed infected; positive from both gold standard and new test / total positive from new test
NPV long, expl + formula
negative predictive value, if the test is negative, what is the likelihood that the patient is indeed uninfected; negative from both gold standard and new test / total negative from new test
prevalence formula
amount infected / whole population
what can you learn from the same test but in a new cohort
prevalence in population really can impact PPV - if prevalence is smaller, tests become less accurate
4 main antimicrobials
antibacterials, antivirals, antifungals, antiparasitics
3 main mechanisms of antimicrobial resistance
altered target site, altered uptake/efflux, drug inactivation
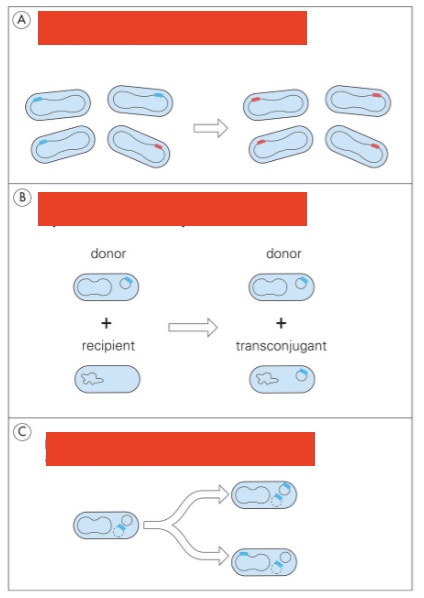
3 main mechanisms of antimicrobial resistance spreading
Horizontal gene transfer:
chromosome mediated resistance: mutant selection, plasmid-mediated resistance: spread of resistance plasmid, plasmid-mediated resistance on a transposon: spread of resistance gene
antibiotics: what is it, what does it do, where does it go (route of administration!!) - general, just what would be possible answers of these questions
chemical structure (natural or synthetic product), target site/mechanism of action, absorption/distribution/metabolism/excretion of the drug in the body of the host
antibiotics: when is it used, what are the limitations to its use, how much does it cost- general, just what would be possible answers of these questions
spectrum of activity and important clinical uses, toxicity to the human host- lack of toxicity (ie resistance of bacteria), great variation between agents- cost is a huge limiting factor in resource poor settings
target sites for attack for antibiotics (5)
cell wall synthesis, protein synthesis, nucleic acid synthesis, metabolic pathways, cell membrane function
target sites for attack for antibiotics: cell wall synthesis, 3 stages +descr
extracellular stage: translocation of the monomer across the membrane, polymerization and cross-linking to extend the peptidoglycan network
membrane associated stage: attachment of precursors to the lipid carrier C55 and formation of the peptidoglycan monomer
cytoplasmic stage: synthesis of UDP-NAG and UDP-NAM recursors
what cell wall synthesis process can we interfere with specifically (4)
adding cycloserine to interfere with adding of alanines, can prevent dephosphorylation of phospholipid carrier with a bacitracin (C55 lipid), can have a glycopeptide sit on the alanine residues not allowing them to be incorporated, beta lactams which bind to and inhibit enzymes which catalyse the pentaglycine cross-links
stages of cell wall synthesis and when each type of antibacterial can work
cytoplasm (synthesis of cell wall precursors): cycloserine
cytoplasmic membrane (synthesis of new cell wall subunit attached to lipid carrier): glycopeptide, bacitracin
cell wall (attachment of new wall unit to growing peptidoglycan): beta lactams