all of NURS216A/B
1/747
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
748 Terms
Medical use for Cannabis-- schedule
Schedule 1
High dose iron-- schedule
Schedule II
meds that contain Cough Syrup stuff (bc contains Codiene) & Cannabis for funzies --- schedule
Schedule III
Tylenol -- schedule
Unscheduled
Schedule I
MUST have PRESCRIPTION & drug must be provided by a pharmacist
- All Prescription drugs
- Drugs w no potential for abuse OR Narcotics('drugs W potential for abuse'= addictive)
- Controlled drugs (also r drugs that has potential for abuse)
- ex. Medical use for Cannabis
Schedule II
- available ONLY from a PHARMACIST('pharmacist rx('prescription')')
- retained in an area w NO public access
ex. High dose iron
Schedule III
- available via open access in a PHARMACY or PHARMACY AREA ('OTC')
- these drugs r Closed & off limits when the pharmacy closes
- *might be addictive if taken in BIG amounts
ex. meds that contain Cough Syrup stuff (bc it contains codiene), cannabis for funzies
Unscheduled
can be sold in any store w/o professional supervision (ex. Any convience store)
- ex. Tylenol
~25%
___ of PR('rectal') drug goes through 1st pass metabolism
Parental roa
'injectable'. ex. SC, IV roa
Enteral roa
'goes through GI sys'
<500 dalton
small. drug goes systemic
AC
'Before Meals'
PC
'After Meals'
QD
'Once Daily'
BID
'Twice Daily'
TID
'Three Times Daily'
QID
'Four Times Daily'
QHS
'At Bedtime'
QAM
'Every Morning'
QPM
'Every Evening'
QOD
'Every Other Day'
QH
'Once Every Hour'
Q2H
'Every 2 Hours'
Q3H
'Every 3 Hours'
PRN
'As Needed'
NPO
'Nothing By Mouth'
SC/SQ
'Subcutaneous'
Liver
25% blood flow at rest
Kidney & Muscles
20% blood flow at rest
Brain
18% blood flow at rest
Skin
7% blood flow at rest
Bone marrow & Heart
5% blood flow at rest
NARROW TI MEDS
- Digoxin (Lanoxin)
- Warfarin (Coumadin)
- Phenytoin (Dilantin)
- Tacrolimus (Prograf, Astagraf)
99% PPB drug
Warfarin (Coumadin)
Amoxicillin
drug class: Penicillin
travel UNCHANGED
- tx: Otitis Media
- roa: PO
- **combined w b-lactamase inhibitors (IF bac is resistant to 'this')
Grapefruit juice
Inhibits CYP3A4 (=> causes the enzyme to metabolize Lovastatin slower = slower Excretion of drug) => drug stays in body for longer => increased reduction of cholesterol)
Zero order elimination kinetic drugs
- Phenytoin (Dilantin)
- Ethanol ('alcohol')
- Aspirin ('ASA')
20mg/dL/hr
Clearance rate of Alcohol
CrCl calculation formula
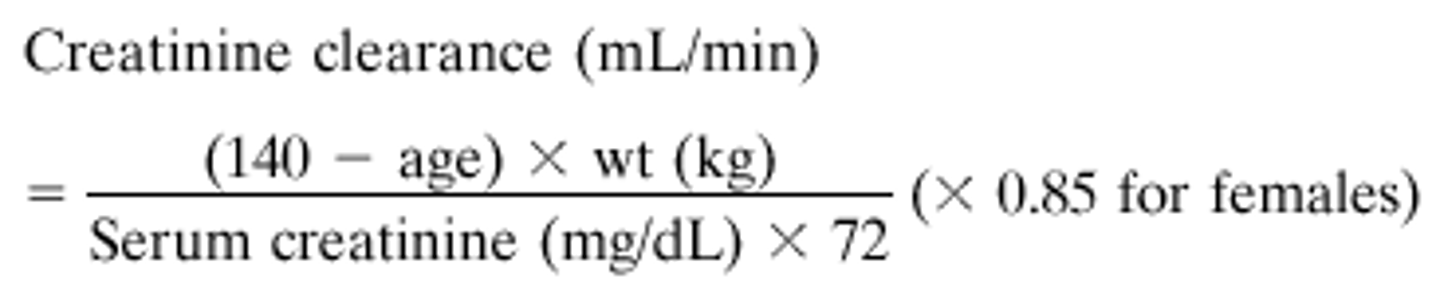
normal Glomerular Filtration Rate
>59ml/min
4 x t ½
90% of the drug has cleared => u can administer more drug to the patient now
adenosine
enodgenous. Binds to receptor => makes u sleepy
- Caffeine binds to the same receptor as 'this' & causes an OPPOSITE effect(make u more alert) ('caffine is an INVERSE AGONIST')
Most common Toxicities
- ASA (Aspirin)
- Acetaminophen (Tylenol)
- Opioids (ex. Oxycodone, Fentanyl)
- Benzodiazepines (ex. Alprazolam (Xanax), Valium (Diazepam))
- Alcohol (ETOH)
- THC
- Cocaine
- +medication errors
ASA toxidromes
- Confusion
- Tachycardia
- Tachypnea
- Hyperthermia
- Diaphoresis
- Vomiting
Acetaminophen toxidromes
- Abdominal pain
- Loss of appetite
- Nausea/Vomiting
- Diaphoresis
- Somnolence
Opioids toxidromes
- Bradypnes/Apnea
- Bradycardia
- Somnolence/Coma
- Pupils CONSTRICTED
Cocaine toxidromes
- Agitation, tremors
- Tachycardia
- Tachypnea
- Hyperthermia
- Diaphoresis
- Pupils DILATED
Cannabis toxidromes
- Tachycardia
- Hypertension
- Seizures
- Nausea/Vomiting
- Acute psychosis
- Agitation; Coma
Activated Charcoal
tx via 'Adsorption'
- ENTERAL administration
- binds the drug to surface carbons => stops drug from getting absorbed => gets eliminated via Stool
- DOESNT work if u took the o.d drug a long time ago, since it prob already got absorbed into body
- tx drugs for": Tylenol, ASA, Benzodiazepines O.D
**doesnt work for alcohol overdose
Naloxone (Narcan)
tx drug for Opioid O.D
- ROA: intranasal, IV, IM, Subcutaneous
- onset: 2-4 min; duration of action: 45min
- ANTAGONIZES opioids from binding at mu & kappa receptors
Flumazenil
tx drug for Benzodiazepine O.D
- ROA: IV
- Flumazenil ANTAGONIZES GABA receptors
'n-acetylcysteine' (NAC)
tx drug for Tylenol O.D
- is a Glutathione enzyme presursor (=> enhnaces phase II metabolism)
*tylenol O.D (>4hrs): liver enzyme ('Glutathione') is depleted => casues low phase II metabolism => causes accumulation of hepatotoxic NAPB (product of phase I M)
Metadoxine
tx drug for ETOH intoxication
- ROA: IV
- induces('increases') alcohol dehydrogenase
**ETOH intoxication: causes depledted 'alcohol dehydrogenase'
Sodium Bicarbonate
tx drug for ASA O.D
- 'this' is BASIC (high pH) => IONIZES acidic substance(ex. ASA)
**acidic drug like acidic env (:. If in basic env, its molecular characteristic gets altered => increased Elimination)
**urine is naturally slightly acidic
Acetaminophen tx
tx Pain at CNS lvl
- Non-opioid centurally acting agents
- *NOT addictive
Opioids tx
tx Pain at CNS lvl
- centurally acting analgesics
*ADDCTIVE
NSAIDs tx
tx Pain at Peripheral lvl
- NON-Steroidal
*NOT addictive
Glucocorticoids (aka. Steroids, Coricoids) tx
tx Pain at Peripheral lvl
- Steroidal
Acetaminophen (Tylenol)
ANTIPYRECTIC, *NOT anti-inflammatory tho!
- CENTRALLY acting analgesic
- Administration: PO, q4h; pediatric: per kg
- HIGHEST efficacy for tx fever (bc 'this' is centurally acting: stimulates Hypothalamus => H causes peripheral Vasodilation => cooling)
- commonly used in Synergy tx (combining w other drugs)
Opioids
aka. Narcotics
- agonists for these CNS receptors: Mu, Kappa, Delta
- 'this' binding to receptor causes: increased Histamine & Dopamine release; Decreased Substance P & Glutamate (s&s: itchiness, addictive, slowed down & sleepy)
- mimics 'Endogenous opioid peptides'
Endogenous opioid peptides
r endogenous inhibitory neurotransmitters ("neuromodulators")
- includes: Endorphins, Enkephalins, Dynorphins
- released from: Hypothalamus, Limbic sys, Reticular formation
- all follows the DESCENDING ('efferent') pathway (=> then they bind to a receptor(meant for: opioids, serotonin, or norepinepherine) => inhibits release of Substance P (@where 1st && 2nd order neuron synapse w eachother))
Endogenous opioid peptides drugs
- Endorphins
- Enkephalins
- Dynorphins
High efficacy opioid:
- Fentanyl
- Hydromorphone (Dilaudid)
- Meperidine (Demerol)
- Morphine
- Methadone (Metadol)
Moderate efficacy opioid:
- Hydrocodone
- Oxycodone (OxyNeo)
- Oxycontin
- Tramadol (Ultram)
- Codeine
- combo drugs: Percocet, Percodan, Vicodin, Tramacet
Percocet
a Moderate efficacy opioid
- oxycodone + acteaminophen
Percodan
a Moderate efficacy opioid
- oxycodone + ASA
Vicodin
a Moderate efficacy opioid
- hydrocodone + acetaminophen
Tramacet
a Moderate efficacy opioid
- tramadol + acetaminophen
Codeine
a moderate efficacy opioid
- a prodrug (:. NO for kids (bc metabolism is too volatile('unpredictable'))
Tylenol #1
8mg codeine, 300mg acetaminophen, 15mg caffine
Tylenol #2
15mg codeine, 300mg acetaminophen, 15mg caffine
Tylenol #3
30mg codeine, 300mg acetaminophen, 15mg caffine
Tylenol #4
60mg codeine, 300mg acetaminophen, 15mg caffine
Non selective NSAIDs drugs
- Acetylsalicylic acid (ASA. aka. Aspirin) (has Enteric coasted ASA (ECASA))
- Ibuprofen (Advil, Mortin)
- Diclofenac (Voltaren)
- Naproxen (Aleve, Naprosyn)
- Ketorolac (Toradol)
- Indomethacin
Indomethacin
a Non selective NSAIDs
- 20x ASA POTENCY!!
- Prescription ONLY
Selective NSAIDs drugs
- Celecoxib (Celebrex)
Celecoxib (Celebrex)
a Selective NSAIDs (inhibits COX-2 ONLY)
- NOT 1st line tx
- Rx only
- rlly potent & has rlly bad s.e
COX-1
cause platelet aggregation
- 'this' activates Arachidonic acid into Prostaglandin
COX-2
cause pain & inflammation
- 'this' activates Arachidonic acid into Prostaglandin
if pain <4/10
=> NON-OPIOID medications
- PO
- probably ex. NSAIDS, Tylenol; synergy
if pain 4-6/10
=> OPIOIDS; combo meds
- PO
- synergy
if pain >6/10
=> HIGHER potency OPIOIDS
- PARENTERAL (ex. IV, SC...etc)
- consider PCA ('patinet controlled analgesia'): always given parenteral (usually IV); allows patient to choose when to receive med by themself
- synergy
Glucocorticoids
a STEROID drug
- Local or Systemic
- stimulates gluconeogenesis ('makes glucose')
- stimulates protein degradation (:. Too much cortisol => musc weakness)
- facilitates lipolysis (=> mobilizses stored energy)
- tx: Local, Chronic inflammation, Systemic disease, Chronic disease, (+ anaphylaxis)
Glucocorticoid drugs
- Prednisone
- Prenisolone
- Methylprednisolone
- Dexamethasone
- Hydrocortisone
- Cortisone
Dexamethasone
a glucocorticoid
- given for systemic inflammation d/t AUTOIMMUNE stuff (ex. IBD, Lupus, Rheumatoid Arthritis)
- give: PO, low dose, daily
- given as adjunct tx
Allergic Rhinitis tx
- Fluticasone (Flonase)
- Mometasone (Nasonex)
- Budesonide (Rhinocort)
Asthma maintenance drugs
- Budesonide (Pulmicort)
- Beclomethasome (Qvar)
- Fluticasone (Flovent)
diff types of Controller drug for asthma
- Glucocorticoids
- Leukotriene modifiers
- Mast cell stabilizers
Asthma rescue drugs
- Beta 2 Adrenergic Agonists (aka. "SABA")
- Antichholinergics
- Epinepherine
Beta 2 Adrenergic Agonists
aka. SABA
- a Asthma rescue tx
- binds to B2 receptor of SNS (=> B2 is located in LUNG :. BROCHODILATION)
Beta 2 Adrenergic Agonists drugs
- Salbutamol (ventolin, albuterol)
Antichholinergics
- a Asthma rescue tx
- inhibits PNS
Antichholinergics drugs
- Ipatropium (Atrovent)
1st generation Antihisamines drugs
- Diphenhydramine (Benadryl, Allerdryl)
- Chlorpherinamine (an ingredient in ex. Benylin)
2nd generation Antihistamines drugs
- Fexofenadine (Allegra)
- Loratadine (Claritin)
- Cetrizine (Reactin)
- Desloratadine (Aerius)
Cetrizine (reactin)
a 2nd generation Antihistamines
- fast melt tabs
- Onset: 10-20mins
- Duration: 24hrs
Prodromal stage
1/5 course of infection
- Initial s&s show: ex. Malaise, mild fever, headache, myalgia('musc pain')
- Generic in nature ('general s&s') :. hard to differentiate if bac or virus or wtv is causing the sickness
Convalescent period
1/5 course of infection
- pathogen DECREASING in numbers
- Progressive host repair of damages
Cell wall synthesis inhibitors drugs
- Penicillins
- Cephalosporins
- Carbapenems
- Bacitaracin
- Vancomycin
- Polymyxin B