Approach to Group Lamb Health
1/36
Earn XP
Description and Tags
M.18, W.3, L.1
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
Clinical disease is often a symptom of ?
symptom of underlying management or nutrition issues
List the steps of a case investigation
Take a history
Examine environment, housing, nutrition
Live lamb clinical exams
Ewe clinical exams
Lamb post mortems
Additional testing
Preventative actions
List important sheep specific questions to ask when taking a history
AGE of affected lambs
timing of lambing & breeding
management at lambing time
colostrum
breed of animals affected
any treatments
List IMPORTANT data to look at when investigating losses
Number of ewes bred
Scanning results
Number of lambs weaned
Number of lambs sold or kept for breeding
Other:
number of lambs born alive/dead
number of lambs turned out at __ days
number of lambs ‘marked’ or wormed
List issues that can occur Pre-partum and Peri-partum during lambing
Pre-Partum
maternal disease
maternal death
abortion
severe maternal starvation
Peri-Partum
dystocia
abortive agents
membranes over nose
List issues that can occur from neonatal to 3 weeks during lambing
Starvation:
mastitis of ewe
lack of milk
lack of vigor
rejection by ewe
Neonatal infection
congenital disease
Hypothermia
List issues that can occur Pre-weaning during lambing
Nematodirosis
Coccidiosis
Parasitic gastroenteritis
Pulpy kidney
Ruminal acidosis
List issues that can occur Post-weaning during lambing
Parasitic Gastroenteritis
Pneumonia
Septicemia
Ruminal acidosis
Pulpy kidney disease
List one issue that occurs during pre-weaning and post-weaning
Trace element deficiencies
List risk factors for neonatal deaths
low:
birthweight
serum immunoglobulin
ewe body condition
high litter size
being born late in season
inexperienced/young mothers
male lambs
List general ways to prevent lamb losses
ewe nutrition
good
hygiene
lighting
compact lambing
adequate labor
shelter outdoors
bushes, trees, pallets secured upright
vaccinations
stocking rates
appropriate genetics
List prevention of lamb losses at lamb level
COLOSTRUM = GOLD
Navel dipping
dipping better than spraying
good hygiene
regular checks
full abdomen, BAR, navel
Quickly
Target: within 2 hours
Quantity
50 ml/kg in first feed
2-300ml/kg in first 24 hrs
Quality
IgG levels
fat content
checking:
viscosity, color, colostrometer, Brix refractometer
List types of colostrum replacers
Fresh from another ewe
Frozen from other ewes
DO NOT MICROWAVE
Cow colostrum
need 30% more volume (lower fat and IgG content)
pool from 4 cows
vaccinate against Clostridial disease
risk of Johnes disease and TB transmission
Powdered colostrum
why should you not microwave frozen colostrum replacement?
denatures antibodies
List reasons why orphan lambs are high risk
poor colostrum provision
nutrition very artificial
Red gut
define red gut
fatal disease
occurs when rapid fermentation of feed causes SI to become unstable —> torsion of intestines
sudden death, abdominal bloat, dark red intestines
List ways to prevent red gut in orphan lambs
ensure fiber intake
milk at room temp after 7 days
continual milk supply or frequent small feeds
wean early
List simple steps of lamb PMEs
Check outside (nose, toes, tail, navel)
Remove skin (chest and abdomen)
Open abdomen
Open chest
Why should aborted lambs not get a PME
zoonotic agents!!
List other types of testing for a lamb mortality case investigation
Lamb Colostrum Intake
serum total protein
IgG direct measures
GGT (indicates intake not IgG absorption)
Parasitology
Ewe:
dietary analysis
metabolic profiles
List preventative measures to apply after a lamb mortality
Vx
maternal nutrition
colostrum management
hygiene
navel treatment
individual lamb treatments:
glucose, warming box, Abs
List conditions you’ll see on a farm causing lamb mortality
Starvation / hypothermia
watery mouth
neonatal diarrhea
neonatal bacteremias
Orf
congential conditions
umbilical prolapse
cow colostrum anemia
Describe starvation and hypothermia (how lambs appear, temperature, underlying causes, brown fat reserves purpose)
lambs curled up (maybe away from dam)
T < 39°C, empty abdomen
Underlying causes
mismothering
maternal mastitis
birth trauma / joint ill
Brown fat reserves
depend on maternal nutrition
last approx 5 hrs
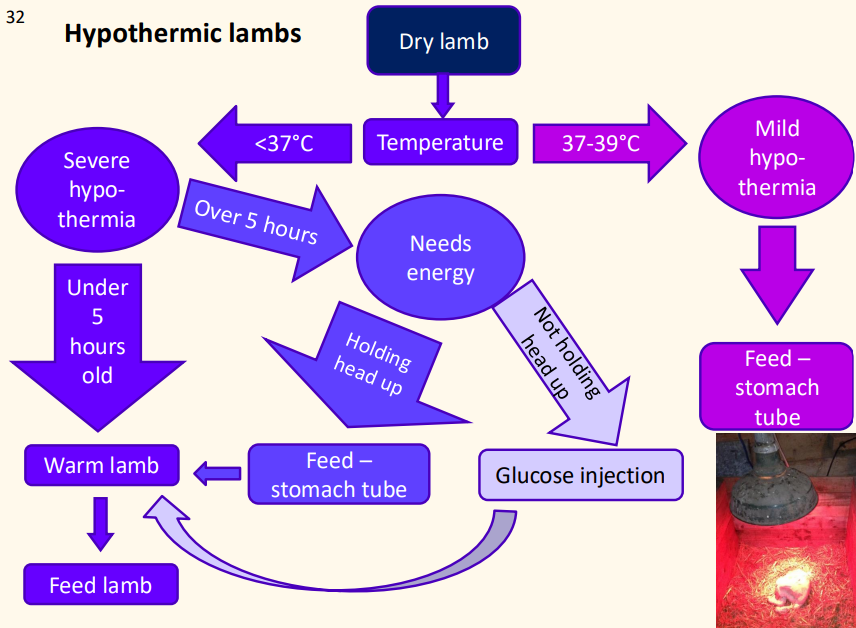
Describe how to give a glucose injection
New needle – 19 guage, 1 inch
New syringe (50ml)
Mix into one syringe
4ml/kg 50% glucose
20ml - 5kg lamb
6ml/kg hot boiled water
30ml - 5kg lamb
Mark the spot with antibiotic spray
1 inch behind and ½ inch to side of navel
Insert needle, pointing it toward the tail-head
Describe watery mouth (other names for it, what age lambs it affects, when it occurs during lambing, what it causes)
Rattle Belly or Slavers
1-3 day old lambs
towards end of lambing
failure of passive transfer of immunity
decrease colostrum
slow GIT motility + high abomasal pH
enterotoxemia, e.g. E. coli
List early and later signs of watery mouth
Early Signs
cold wet mouth
reluctance to suck
dull
Later signs
salivation
distended abdomen w/ gas + fluid
recumbency
diarrhea or constipation
List Dx and Tx of Watery Mouth
Dx
typical clinical signs
PME suggestive
Tx
fluids, 50 ml every 3 hours w/ glucose
NSAIDs
warmth (keep w/ ewe if possible)
Abs
List causes of neonatal diarrhea
E.coli K99
Cryptosporidiosis
Salmonellosis
Rotavirus
Lamb dysentery
Coccidiosis
Describe Lamb Dysentery (type, 2 forms, Dx, Tx, and prevention)
Clostridium perfringens type B
2 Forms
young lambs (1-3 days old)
sudden death
PME hemorrhagic enteritis - jejunum
Older lambs (up to 3 wks)
abdominal pain
hemorrhagic diarrhea
death
Dx
Toxins B and E in intestinal contents
PME
Tx
symptomatic
most need PTS
Prevention
vaccination (ewes pre-lambing)
Colostrum
Describe Enterotoxigenic E.coli (ETEC) (what age it affects, symptom, Tx, Prevention)
<48 hrs old
secretory diarrhea
Tx
prompt fluid therapy
Abs
NSAIDs
Prevention
hygiene, colostrum, isolate sick lambs
Describe Cryptosporidium parvum (zoonotic?, what age it affects, symptom, recovery time, Tx, Prevention)
Zoonotic
< 3 wks old
profuse watery diarrhea
may recover in 5-7 days or die of dehydration
Tx
fluid therapy
Halofuginone (Halocur)
not licensed
Prevention
hygiene (difficult to kill)
Describe Salmonellosis (zoonotic?, strains, symptoms
zoonotic
Salmonella typhimurium or S. Dublin
Profuse diarrhea
rapid death
Tx
fluid therapy (intense)
Abs
NSAIDs
Opportunistic infections
immunosuppressed
high environmental contamination
E.coli, Mannheimia hemolytica, Pasteurella multocida
Navel ill
Septic polyarthritis
Spinal abscess
Meningitis
Pneumonia
Liver abscesses
Septicemia
Navel Ill
umbilicus
Meningitis, Septic polyarthritis, Septicemia
mouth
upper resp. tract
umbilicus
Spinal abscess
all of the above
infected tail ring
Mild
slight swelling
± serosanginous to purulent discharge
Severe
depression
± pyrexia
failure to suckle
painful, warm swelling ± discharge
Can lead to
hepatic necrobacillosis
peritonitis
meningitis
cystitis
Tx
systemic antibiotic:
penicillin, amoxicillin ± clavulanic acid
fluorfenicol
long course, min 7 days, ideally 10-14 days
NSAID
Prevention