SDL 10: Peripheral Vascular Disease and Venous Disorders | Quizlet
1/58
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
Raynoud Phenomenon
-exaggerated vascular response to cold temp or emotional stress
-abnormal transient vasospasm of digital arteries that results in triphasic color changes in the affected region
Hands and Toes
most common location for Raynauds Phenomenon
Raynaud Crisis
-assoc with paresthesia due to sensory nerve ischemia
15-30
age of onset for Primary Raynaud Phenomenon
>40
age of onset for secondary Raynaud Phenomenon
Primary Raynaud Phenomenon
-symmetric attacks
-absence of tissue necrosis, ulceration, or gangrene
-normal nailfold capillaries
-negative test for autoantibodies
-normal ESR
Secondary Raynaud Phenomenon
-occurs in the context of another disease
-Asymmetric attacks
-painful attacks with tissue necrosis or ulceration
-presence of a rheumatic or autoimmune disease
-abnormal nailfold capillaries
-positive test for autoantibodies
-elevated ESR
Nailfold Capillary Microscopy
-assoc with Raynaud Phenomenon
-performed by dropping oil on the periungual area and examining with a microsope
Arteriovenous Anastomoses (AVAs)
Thermoregulation is mainly accomplished by numerous __________________________________, low-resistance conduits that allow shunting of blood from arterioles to venules at high flow rates
Primary Raynaud Phenomenon
-due to vasoconstriction of AVAs, allowing for heatloss on non-hairy skin
-increased activation of cold alpha-2 adrenergic receptors (α2-AR) located on vascular smooth muscle cells of AVAs
Secondary Raynaud Phenomenon
-reflects structural abnormalities in the microcirculatory bed
-endothelial function is compromised
-intimal fibrosis
-reduced levels of vasodilatory mediators and increased levels of vasoconstrictive mediators
Phlebitis
-inflammation within a vein, in absence of thrombus
-typically due to infection
Thrombophlebitis
-venous thrombosis that results from inflammation or infection of the vein
Phlebothrombosis
-venous thrombosis related to hemodynamic and coagulation alterations without an initiating infection or inflammation
Virchow's Triangle
-pathogensis of venous thrombosis
-vessel wall injury
-venous stasis
-hypercoagulability
Hypercoaguable States
-defined as a group of inherited or acquired conditions assoc with a predisposition to venous thrombosis
Phlebothrombosis
-primary intravascular coagulation in a vein that is not inflamed
-cause usually hypercoagulable states and venous stasis
-inflammatory vessel wall alterations are initially absent
Superficial Vein Thrombosis and Deep Vein Thrombosis
most common forms of phlebothrombosis
Superficial Vein Thrombosis
-thrombotic process in a superficial vein such as saphenous vein, and lesser saphenous vein of the lower extremities
Deep Vein Thrombosis
-formation of thrombi in the deep veins of the lower extremities, such as iliac, femoral, popliteal, and tibial veins
Thrombophlebitis
-primary inflammation fo the vessel wall followed by secondary thrombosis
-causes: IV catheters, venipuncture for phlebotomy and IV injections
S. aureus
most common infective organisms assoc with thrombophlebitis
Thrombophlebitis
-very high fever and chills
-swelling of the limb and marked tenderness
-sepsis
-infective endocarditis
Deep Vein Thrombosis
risk factors for ______________________:
-immobilization (longer than 3 days)
-obesity
-cigarette smoking
-oral contraceptives
-pregnancy
-postmenopausal hormone replacement
-surgery
-trauma
-medical conditions (anitphospholipid Ab syndrome and cancer)
Factor V Leiden and Prothrombin Gene Mutations
Although only a minority of pts develop DVT genetically, what mutations are assoc with DVT?
Pulmonary thromboembolism
life threatening complicaiton of DVT
Migratory Thrombophlebitis (Trousseau syndrome)
-recurrent or migratory venous thrombosis that precedes the diagnosis of an occult visceral malignancy or appear concomitantly with the tumor
Migratory Thrombophlebitis (Trousseau syndrome)
most often related to pancreatic, lung, prostate, gastric, colorectal, ovarian, and breast cancer
Cancer procoagulant
a cysteine protease that activates coagulation factor X
Migratory Thrombophlebitis (Trousseau syndrome)
venous thromboses appearing in one site only to disappear and be followed by thromboses in other veins
Superior Vena Cava Syndrome (SVCS)
-partial or complete obstruction of blood flow thru the superior vena cava
Superior Vena Cava Syndrome (SVCS)
-often results form a malignany tumor (esp lung cancer) outside the vessel compressng and invading the vessel wall
-distended veins of the upper part of chest and neck
-swelling of the face, neck, and upper extremities
-puffy eyes
-papilledema
-blurred vision
-altered mental status
-syncope
-stupor
-coma
Inferior Vena Cava Syndrome
-partial or complete obstruction of blood flow through the inferior vena cava
Inferior Vena Cava Syndrome
-causes include luminal thrombosis, extrinsic compression, and complications of IVC filter placement
Inferior Vena Cava Syndrome
-may be asymptomatic, if slow and progressive occlusion allows for development of collateral flow
-edema of lower extremities
-pulmonary thromboembolism
-chest pain and shortness of breath
Varicose Veins
-dilated, lengthened and tortuous subcutaneous veins of the lower extremity characterized by retrograde blood flow
-Great Saphenous Vein
-Lesser Saphenous Vein
-Saphenous Tributaries
varicosities mostly affect which veins?
Varicose Veins
-due to increased venous pressure and impaired reutrn of blood
-chronic venous insufficiency
Primary Varicose Veins
-varicose veins that develop as a result of inherent weakness in the wall of the vein
Secondary Varicose Veins
varicose veins assoc with failure of superficial venous valves in pts with DVT
Primary Varicose Veins
-linked to downregulation of purinergic P2X1 receptors
-results in loss of contractile activity of the venous walls
-congenitally weak vein walls dilate under normal pressures, and secondary valve failure develops
Lymphangitis
-an inflammation of the subcutaneous lymphatic vessels typically in an extremity
-occurs as a result of cutaneous inoculation of pathogenic organisms into the lymphatic vessels thru a skin wound
Streptococcus pyogenes
the leading cause of acute lymphangitis
Sporotrichosis
-a cutaneous mycotic infection caused by a dimorphic funges
-infection that can result after being pricked by a contaminated rose thorn
-assoc with Lymphangitis
Fish Tank Granuloma
-a skin infection caused by mcobacterium marinum
-assoc with Lymphangitis
-organism found in stagnant freshwater and saltwater environments
Lymphatic Filariasis
-transmitted by mosquitoes
-assoc with Lymphangitis
-caused by Wuchereria bancroftii
Elephantiasis
the advanced stage of lymphedema
Lymphangitis
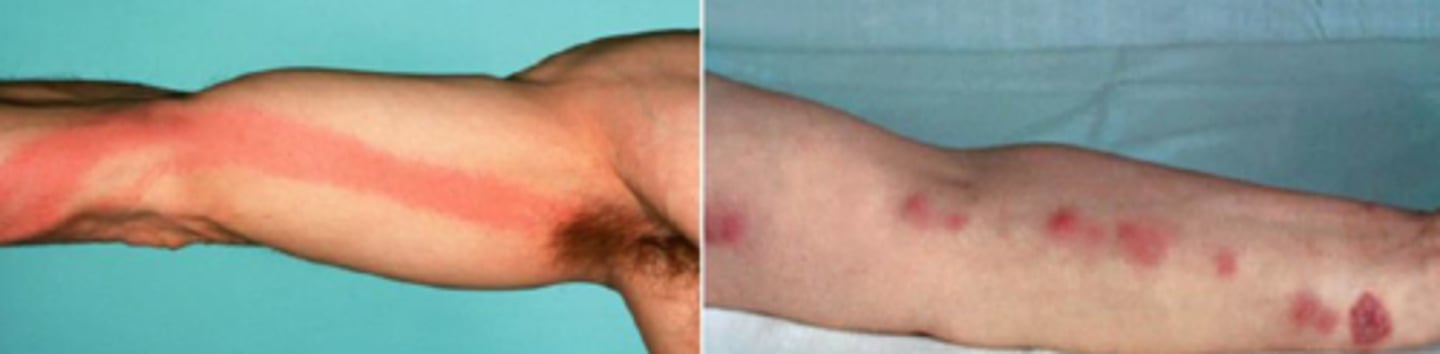
Lymphangitis
-rapid appearance of erythematous streaks proceeding from the site of cutaneous infection toward regional lymph nodes
-tender lymphadenopathy
-sepsis
-nodular lymphangitis
Nodular Lymphangitis
-inflammatory subcutaneous nodules in a linear fashion along the course of the lymphatic channels draining a primary skin infection
Sporothrix schenckii and Mycobacterium marinum
the most common causes of Nodular Lymphangitis
Lymphedema
-swelling caused by excess lymphatic fluid collecting in the body's soft tissues, usually in the arms or legs
Primary
which type of lympedema is infrequent, and seen in children due to inborn error in lymphatic development
Secondary
which lymphedema is an acquired injury to a normally developed lymphatic system
Primary Lymphedema
Milroy Disease is an example of ___________________________
Breast cancer-related lymphedema
-accounts for most cases of secondary lymphedema
-complication of mastectomy in combination with axillary lymph node dissection and is located in the ipsilateral arm
-Damage to the axillary lymphatic system caused by surgery and/or radiotherapy impairs lymph drainage from the arm, resulting in lymphatic fluid accumulation
-Lymph node dissection
-Extensive Skin Resections
-Radiation therapy
-Extreme Obesity
significant risk factors for lymphedema
Lymphedema
-sensation of swelling of heaviness of the affected limb
-pitting edema
-skin becomes dry and firm with decreasing pitting secondary to cutaneous fibrosis and adipose deposition
-brawny induration or a peau d'orange (orange peel) appearance of the overlying skin.
Milroy Disease
-autosomal dominant
-VEGFR3 mutation
-painless, chronic, lower-limb lymphedema found at birth or developing in the early neonatal period
-does not worsen overtime
-reduction in dermal lymphatic vessel density combined with a profound failure of the lymphatic system to absorb interstitial fluid