Local Anesthesia
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
How do you distinguish aminoamides from aminoesters?
Aminoamides have two I’s in their name (e.g., lidocaine, bupivacaine); aminoesters have one I (e.g., procaine, benzocaine).
What is the mechanism of action of local anesthetics?
Bind + blocking intracellular portion of voltage‑gated Na⁺ channels → decrease rate of depolarization → prevent reaching threshold.


Which form of local anesthetic crosses the nerve membrane?
Uncharged base (lipophilic).


Which form of local anesthetic binds the Na⁺ channel?
Charged, protonated quaternary amine (hydrophilic), and cant cross the cellula rmembrane


How many nodes of Ranvier must be blocked to stop conduction?
At least three nodes.


What determines onset of action of a local anesthetic?
Proximity of pKa to physiologic pH (closer pKa → more uncharged base → faster onset).


Why do infected tissues cause poor block quality?
Low pH(acidity) increases ionized form → less membrane penetration → slow onset and poor block.


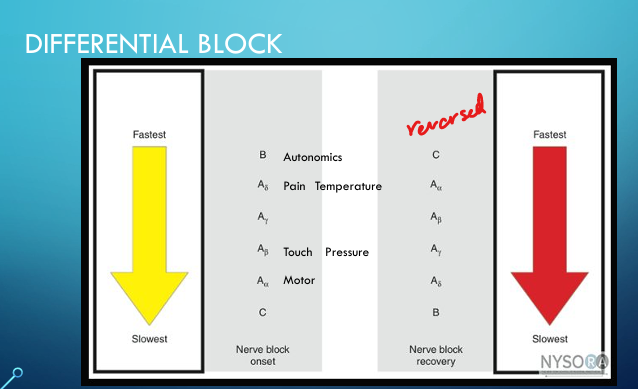
What is differential block?
Autonomic fibers blocked first → pain/temp → touch/pressure → motor last. Reverse order back for recovery

How are aminoesters metabolized? Inhibited by?
Hydrolysis via Plasma esterases. Inhibited by deficiency of plasma cholinesterase activity


How are aminoamides metabolized? Inhibited by?
Hepatic microsomal enzymes (CYP). Inhibited by decreased hepatic blood flow, cirrhosis, liver dysfunction»2 I’s so theyll need heavy duty breakdown by liver


Most local anesthetics are vasodilators (increase systemic absorption because of more blood flow) except ____ a vasoconstrictor?
Cocaine.
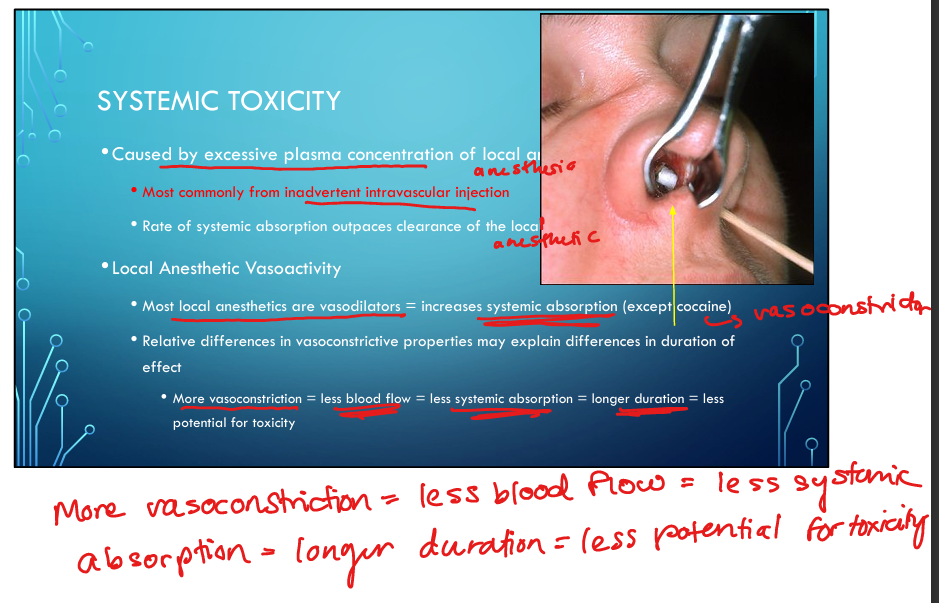

Why does adding epinephrine prolong duration?
It is a Vasoconstrictor which reduces systemic absorption(by decreasing blood flow) → more drug remains at nerve
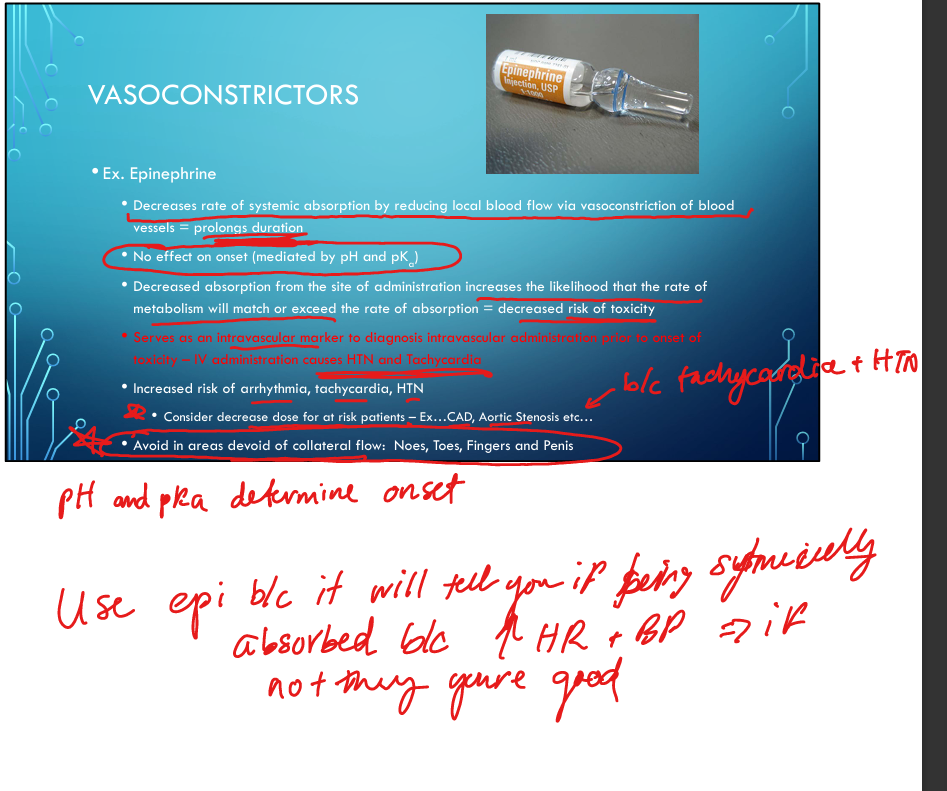

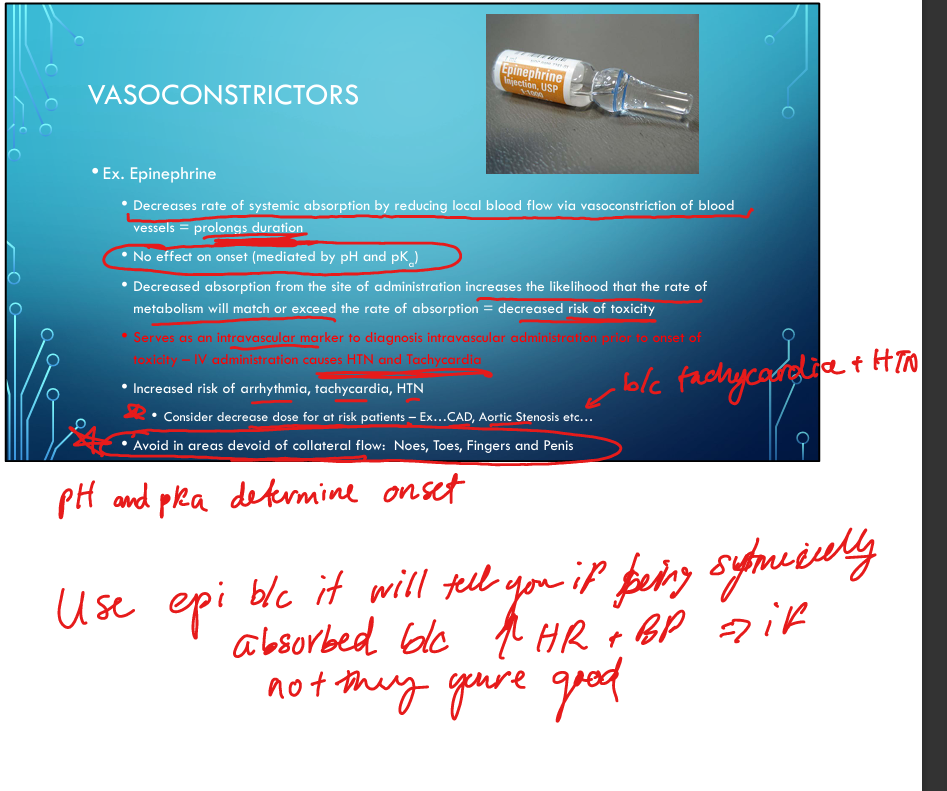
What areas should epinephrine be avoided in?
“No nose, toes, fingers, penis” — areas with poor collateral circulation.

Rank injection sites by systemic absorption (highest to lowest).
Intercostal > caudal > epidural > brachial plexus > femoral/sciatic. (ICE=BS)


What is LAST?
Local Anesthetic Systemic Toxicity due to high plasma concentration.


Early CNS symptoms of LAST?
Circumoral numbness, tinnitus, metallic taste, agitation, restlessness, slurred speech


Late CNS symptoms of LAST?
Seizures → CNS depression → coma.


Cardiac effects of LAST?
Hypotension, PR prolongation(heart block), QRS widening (ventricular arrhythmias), cardiac arrest.


Which drug is more cardiotoxic: lidocaine or bupivacaine?
Bupivacaine (much more cardiotoxic).


What is the treatment for Local Anesthesia Systemic Toxicity (LAST)?
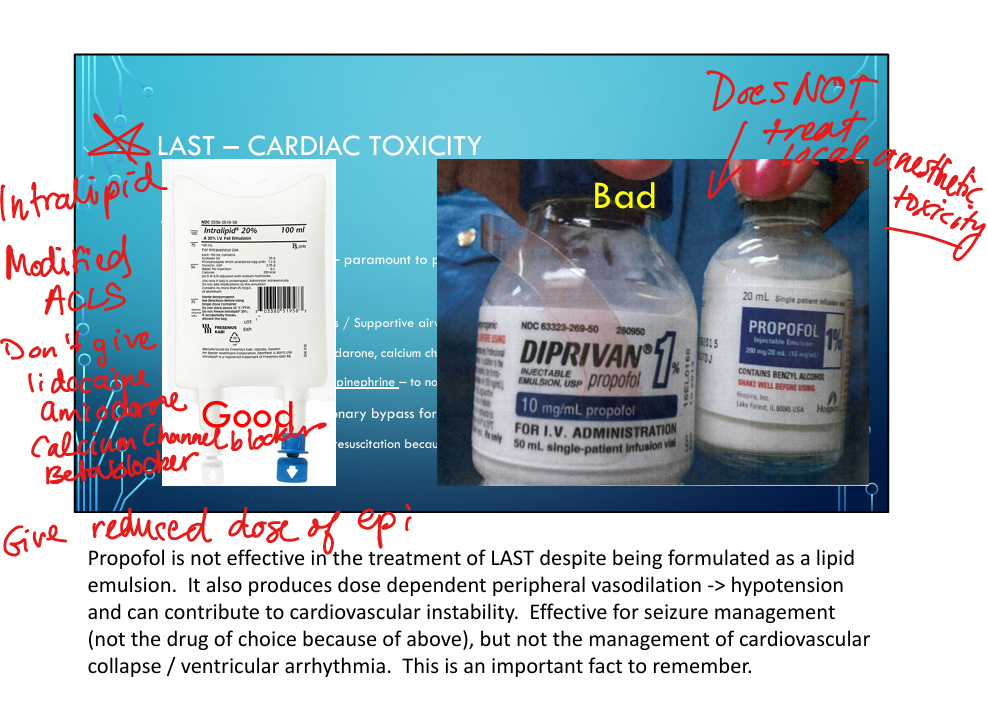
Stop local anesthetic, airway/ventilation, Intralipid 20%, modified ACLS(only give epi because you dont want to vasodilate and produce hypotension anymore), benzodiazepines for seizures,



Why is propofol NOT used to treat LAST?
Despite being a lipid emulsion, it causes vasodilation and worsens hypotension; not effective for cardiac toxicity.

What is the mechanism of intralipid therapy?
“Lipid sink” — binds lipophilic drug and reduces free plasma concentration. Used for Local Anesthetic Systemic Toxicity


What drugs should be avoided during LAST resuscitation?
Lidocaine, amiodarone, calcium channel blockers, beta blockers(all will vasodilate and decrease BP)


What dose of epinephrine is used during LAST?
Reduced dose: ≤1 mcg/kg.


What is the toxic dose of lidocaine without epinephrine?
300 mg (~4.5 mg/kg).


What is the toxic dose of lidocaine with epinephrine?
500 mg (~7 mg/kg).


What is the toxic dose of bupivacaine without epinephrine?
175 mg (~2.5 mg/kg).


What is the toxic dose of bupivacaine with epinephrine?
225 mg (~3 mg/kg).


Are toxic doses additive between agents?
Yes — giving 50% of one drug’s toxic dose means only 50% of another can be given.


Which local anesthetics are long‑acting?
Bupivacaine, ropivacaine.


Which local anesthetics are intermediate‑acting?
Lidocaine, mepivacaine.


Why does systemic absorption shorten duration of action?
Once absorbed into circulation, drug cannot reach nerve.


What is the effect of acidosis on toxicity?
Acidosis increases free drug concentration → worsens toxicity.


How does bicarbonate affect local anesthetic onset?
Increases uncharged base fraction → faster onset.

