exam 3 # 2
1/555
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
556 Terms
Respiratory System provides
for gas exchange between the blood and air.
what is the Upper Respiratory Tract: Head and Neck responsible for
• Filtering out harmful particles in “air”
• Humidifying “air”
• Delivering “air” to the lung
what is the Lower Respiratory Tract: Thorax responsible for
• Gas Exchange
• Prevention of infection
• Clean alveolar surface
what are Ventilatory Mechanics:
Skeletal muscle of diaphragm and intercostal muscles between ribs. Also: abdomenal muscles
does it take energy to inhale or exhale
inhale
What organs facilitate the movement of air to the lung
nose and trachea
how important is of mucus and the mucus membrane to the respiratory system
it is critical
air entry pathway
Nasal Cavity and Conchae-
– Sinus Cavities-
– Oral Cavity: poor airflow efficiency/low resistance
• Pharynx-
• Epiglottis and Glottis-
• Trachea-
• Bronchial Tree-
• Alveolus
Each lung and its lobes sit in what?
pleural cavity under a slight vacuum
what is often mistaken as an airway that can be fatal?
the esophagus
Each lung is surrounded by what?
pleural fluids
Air is distributed into lower respiratory air passages called
bronchi and bronchioles
(that ultimately lead to dead-end alveoli)
what does the Bronchial Tree do?
moves air from large to narrow branching airways
Bronchi have what?
cartilage and smooth muscle- for support
cilia- for cleaning
Nourished by bronchiolar artery
how big are Bronchioles
1mm diameter airways with smooth muscle for
changing diameter to needs
Bronchi in Order from biggest to smallest
Primary B
Secondary B
Tertiary B
leads to Bronchioles
Bronchioles in order from biggest to smallest
Terminal Bronchiole
Respiratory Bronchiole
leads to Alveoli(Gas Exchange)
airflow in lung pathway to alveoli
Primary B
Secondary B
Tertiary B
Terminal Bronchiole
Respiratory Bronchiole
alveoli
what don’t respiratory Bronchiole and alveoli have
cilia or smooth muscle
can the smooth muscle lining Bronchiole constrict
Yes -asthma
what are Alveoli:
clusters of dead end pouches for gas exchange
what is the purpose of Alveolar macrophages
cleaning
what is the purpose of Type II alveolar cells
surfactant
what is the purpose of Type I alveolar cells (simple squamous epithelial)
gas exchange
the conducting zone
area only for airflow not gas exchange
respiratory zone
area gas exchange
characteristics of bronchi and bronchiole
cartilage, yes or no
type of epithelium
blood flow
alveoli, yes or no

how much air can a fully inflated lung contain
5-6 liters
The surface area of the 150 million tiny alveoli in
each lung is about
75 meters
in a single lung, The surface area of the capillaries that sit underneath the alveoli is about
60 meters
the volume of blood in these alveolar capillaries at rest is about
70 ml
the volume of blood in these alveolar capillaries when exercising rigorously is about
200 ml
how fast must blood move through
capillaries
fast
how fast must gas exchange be
fast
how many pleural cavities do you have in your thorax
2
what causes asthma
The smooth muscle lining Bronchiole can constrict
bronchi characteristics
cartilage
>1mm
pseudostratified columnar
blood supply bronchial
no alveoli
Terminal bronchioles
no cartilage
<1mm
cuboidal
bloody supply bronchial
no alveoli
respiratory bronchioles
no cartilage
<1mm
cuboidal
bloody supply pulmonary
alveoli
transit time across the alveoli is______ seconds or less
0.75 secs
Pneumothorax:
a collection of air outside the lung but within the pleural cavity.
(if pleural cavity loses its vacuum, the lung collapses and gas exchange to blood stops)
Why do right and left lung lobes have different sizes
The right lung is shorter, because the liver sits high, tucked under the ribcase, but it is broader than the left.
The left lung is smaller because of the space taken up by the heart
Why do aspirated objects/obstructions affect the right side more often than the left?
it is wider
The respiratory system is rich in
elastin and cartilage
Why is elastin so important for the respiratory system
– It stretches and stretches back!
– Located in lung tissue and thoracic wall
is Inhalation active or passive
active
is exhalation active or passive
passive
Barrel Chest:
sign of loss of elastin
Emphysema/cigarette smoke/ alpha-1-antitrypsin/ all cause
loss of elastin
Hyalin Rings are where
trachea and bronchi of lung
what do Cartilagenous rings do
prop airways open and keep airways from collapsing when you inhale
what do Smooth muscles in airways do
lets you control tune diameter/airflow
what helps prevent airway collapse when you
INSPIRE!
Cartilaginous hyalin rings
what causes the lung to collapse passively
Elastin
what causes Asthma
trachealis and other airway smooth muscle cells constrict in
response to irritants, this increases airway resistance.
Changes in resistance are most pronounced when the what constrict.
bronchioles
Cilia
tiny “hair-like” structures that carry mucus, bacteria, pollen, dust and other potentially harmful material (caught in mucus) up and out
to the glottis.
cilia do not extend into the what
alveolus/terminal bronchiole
cilia can be destroyed by what?
smoke
Lungs move and circulate air to what
maximize alveolar gas exchange
where are acute effects of asthma found
all three Bronchi
how gas exchange happens in Terminal Bronchioles and Respiratory Bronchioles
hardly any
when air isnt in the alveoli, the air sits in what can be called a
“dead space”
what is a “dead space”
significant gas exchange can’t occur here
(These dead spaces should never collapse)
You CAN inhale air and get no gas exchange to the blood because of what
collapsed bronchioles due to asthma
what length are terminal and respiratory bronchioles have
very short lengths that terminate in the blind alveolar sacs.
alveolar sacs are richly supplied
with what?
capillary beds for gas transfer to/from blood.
where does gas exchange with blood occur
Alveoli
where do cartilaginous rings end
Tertiary Bronchi
where is dead space located
above Terminal Bronchiole
how much gas exhcange happen in the Respiratory Bronchiole (Alveolar Ducts):
just a small amount
Describe carbon dioxide and oxygen transfer to/from blood/air
as oxygen in the lungs leaves and goes into the blood, co2 leaves the blood and enters the lungs
Distance from alveolar surface to capillary is a function of..
cells in between and the depth of fluids lining the alveolus
Distance from Alveolus to hemoglobin in a erythrocyte in a Capillary
0.5
what differs from Smoker vs Non-smoker
difference in HEMATOCRIT
How many plasma membranes must oxygen pass through before reaching hemoglobin
5
Gas Diffusion REQUIRES what?
a thin film of water on alveolar surface
Can oxygen or carbon dioxide directly dissolve in water!
a very little amount can
to improve solubility, oxygen is carried by
4 subunits of hemoglobin
to improve solubility, Carbon dioxide is converted to
bicarbonate
Wandering Macrophage (ma)
destroy bacteria and cleans the surface
surfactants and mucus are important for what
air cleaning, optimal gas exchange and lowering internal surface tension.
Alveolar macrophages
specialized monocytes (macrophages) actually leave the blood and patrol the alveolar surface against bacteria and unwanted items.
visceral membrane covers what
lung
parietal membrane covers what
rib cage
Visceral and Parietal Pleural membranes allow what
serosa
Pleural Fluid Function
Friction
Pressure gradient/maintains suction
Pulmonary Cavity:
air space inside airways (bronchi-alveoli)
Inspiration and Expiration require what
pressure gradients
respiratory pressure at rest
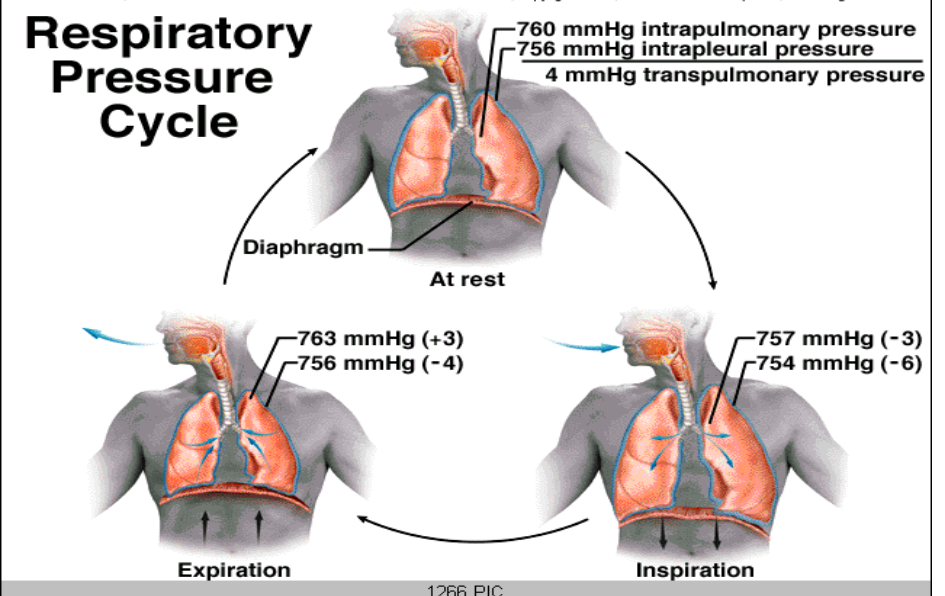
respiratory pressure during inhaltion
volume goes up pressure goes down.
respiratory pressure during exhalation
pressure goes up volume goes down
BOYLE’S GAS LAW
ressure is inversely proportional to volume if temp.
so as pressure goes up volume goes down
and as volume goes up pressure goes down.
1 Atmosphere is equal to:
760
Pressure inside an alveoli
Intrapulmonary Pressure
Pressure inside pleura:
Intrapleural Pressure
Transpulmonary Pressure-
determines if lung inflates (-mmHg) or deflates (+mmHg)
as Transpulmonary Pressure decreases the lungs
inflate
as Transpulmonary Pressure increases the lungs
deflate
Inspiration is caused by
diaphragm contracts and pulls down and/or External intercostal muscles contract
+Volume and - Pressure (↑Vol ↓Press) ....air sucked into lung