VETT 201 Lecture Final Exam
1/277
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
278 Terms
What is the definition of hemostasis?
Stopping bleeding
Are hemostasis and coagulation the same thing?
No
What is coagulation?
Blood changing from liquid to gel
What does hemostasis require interactions between?
Platelets, coagulation factors, fibrinolytic factors, blood vessels, etc.
Who is involved in primary hemostasis?
Platelets and von Willebrand factor
What is primary hemostasis?
von Willebrand factor captures platelets
When do primary and secondary hemostasis occur?
In the case of endothelial injury
Where do primary and secondary hemostasis occur?
At the site of injury
What is the goal of primary hemostasis?
To form a platelet plug
What is platelet activation influenced by?
Thrombin
What is secondary hemostasis also known as?
Coagulation
Who is invovled in secondary hemostasis?
Platelets, coagulation factors, fibroblasts, etc.
What is secondary hemostasis?
Extrinsic/intrinsic coagulation cascades form cross-linked fibrin
What is the goal of secondary hemostasis?
Stabilize the platelet plug made from primary hemostasis to stop hemorrhage
What is thrombin?
An enzyme in blood plasma that causes the clotting of blood by converting fibrinogen to fibrin
What initiates the extrinsic coagulation cascade?
Tissue factor produced by fibroblasts
What activates the intrinsic coagulation cascade?
Thrombin
What enzyme cleaves fibrinogen to fibrin?
Thrombin
What does the coagulation cascade result in?
Formation of fibrin clot over injury
What is the coagulation cascade initiated by?
The extrinsic pathway
What is the coagulation cascade amplified by?
Intrinsic and common pathways
Who is involved in fibrinolysis?
Endothelial cells, plasminogen, plasmin
What is fibrinolysis?
Plasmin degrades cross-linked fibrin
When does fibrinolysis occur?
It is initiated in endothelial injury but inhibited by thrombin
Where does fibrinolysis occur?
On the surface of cells and the fibrin clot
What is the goal of fibrinolysis?
To dissolve the fibrin clot
What is the lifespan of platelets in dogs?
5-7 days
What is the normal range of platelets in dogs?
200,000-900,000/μL
What is the normal range of platelets in cats?
300,000-700,000/μL
What is thrombopoietin produced by?
Hepatocytes, liver endothelial cells, renal tubular epithelial cells, bone marrow stromal cells
What is thrombopoietin degraded by?
Circulating platelets
What is thrombopoiesis?
Formation of thrombocytes (platelets)
How is a manual platelet estimate performed?
Oil immersion field on stained blood smear, count platelets in 10 fields and average, then multiple by 15,000 platelets/μL
What do non-activated platelets look like?
Vary by species; round, oval, or elongated with clear to pale blue cytoplasm, may contain small pink to purple granules
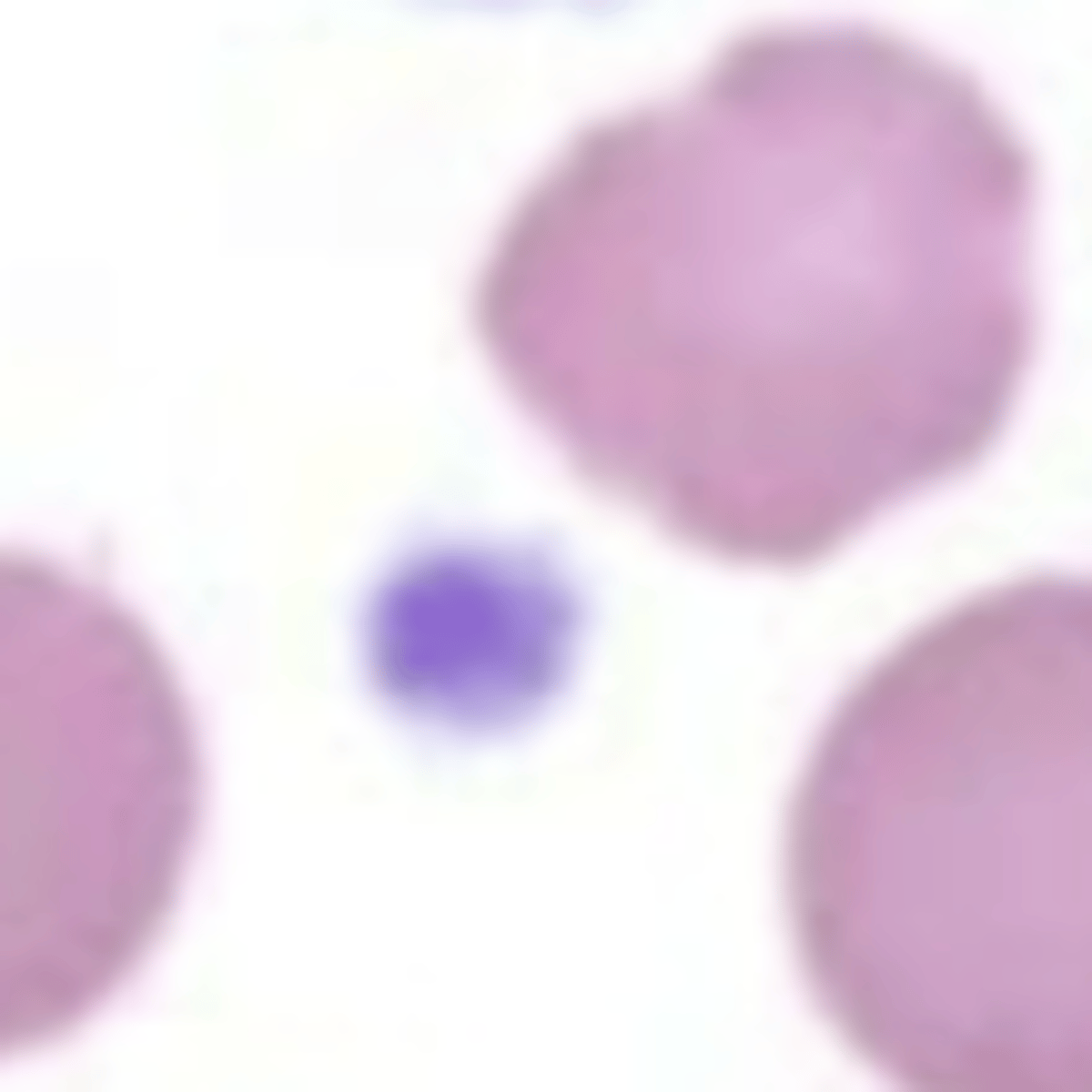
What do activated platelets look like?
Platelets with dendritic processes
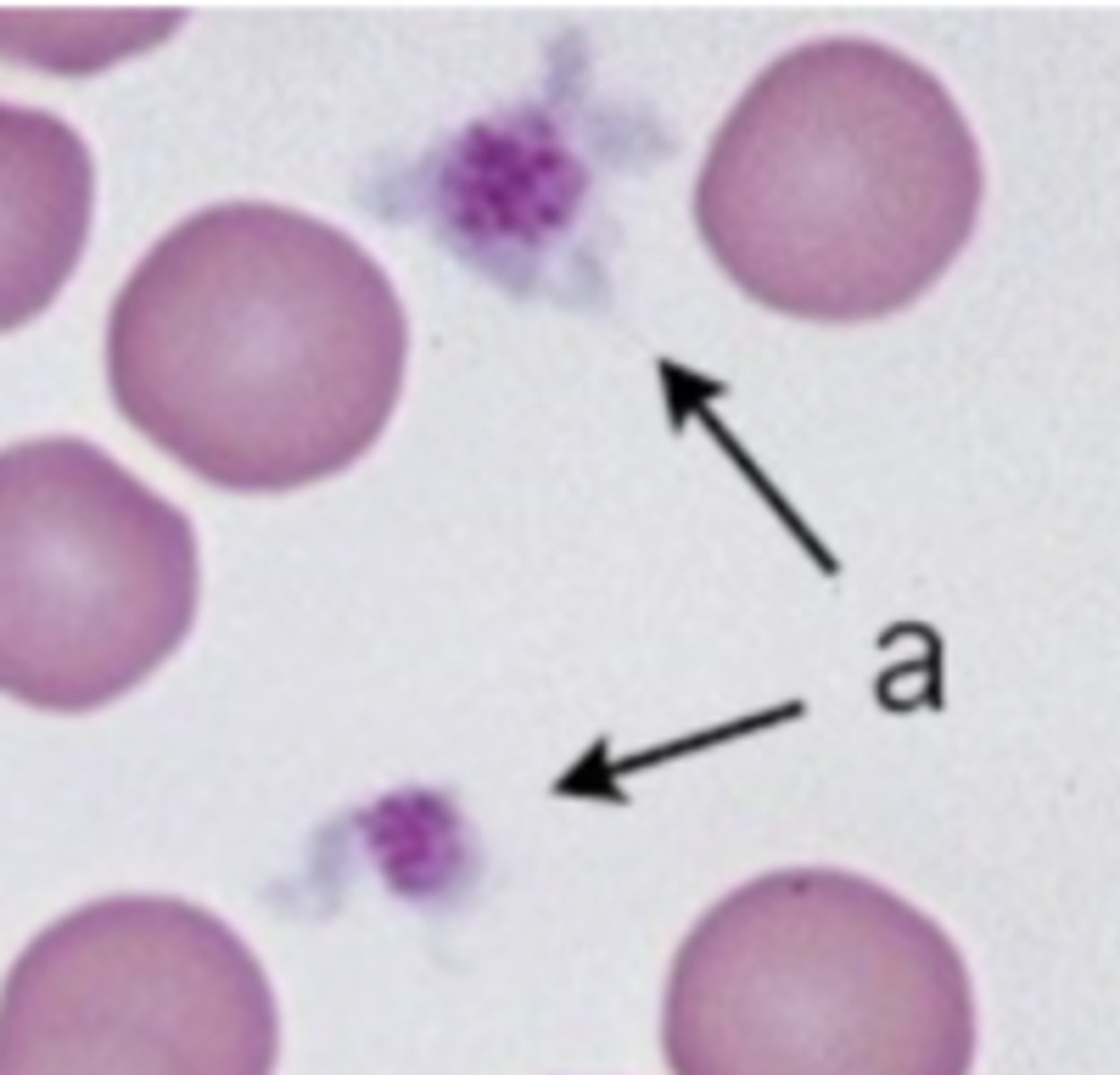
What are the two quantitative platelets disorders?
Thrombocytosis and thrombocytopenia
What can cause thrombocytosis?
Corticosteroids, inflammatory disease processes, neoplasia, iron deficiency anemia, drugs (vincristine, epinephrine, norepinephrine)
What can cause thrombocytopenia due to decreased production of platelets?
Canine distemper, neoplasia, chemotherapy, Ehrlichia canis, inherited macrothrombocytopenia, breed-related (greyhounds, akitas)
What can cause thrombocytopenia due to increased use of platelets?
Trauma, anticoagulant rodenticide toxicosis, DIC, severe sepsis
What can cause thrombocytopenia due to increased destruction of platelets?
Immune-mediated disease, neoplasia, Anaplasma platys, Ehrlichia spp., methimazole, sulfonamides
What can cause thrombocytopenia due to sequestration of platelets?
Splenomegaly, endotoxemia
What are the inherited thrombopathias?
Canine thrombopathia (abnormal platelet function) and Glanzmann thrombasthenia (weak platelets)
What breeds are predisposed to canine thrombopathia?
Basset hounds, Spitz breeds
What are the clinical signs of canine thrombopathia?
Chronic mucosal bleeds, petechiae and aural hematomas
Prolonged hemorrhage during estrus, shedding of deciduous teeth, and trauma/surgery
What is Glanzmann thromboasthenia?
Autosomal recessive disorder in otterhounds, great pyrenees, and quarter horse fillies
Improper platelet aggregation leading to prolonged bleeding times, hematomas at venipuncture/injury sites
What are the clinical signs of thrombocytopenia?
Petechiae, ecchymoses, mucosal bleeding, epistaxis, hematemesis, melena, hyphema, hematuria, prolonged bleeding times after surgery/injury
What is hyphema?
Collection of blood in the anterior chamber of the eye
What breeds are predisposed to inherited macrothrombocytopenia?
Cavalier King Charles spaniels, Norfolk terriers, Cairn terriers, labs, poodles
What is macrothrombocytopenia?
Low platelet count with abnormally large platelets that is usually asymptomatic with normal platelet function (large platelet size makes up for low platelet count)
What is the most common inherited bleeding disorder in dogs?
von Willebrand disease
What is the most common type of von Willebrand disease and what breeds does it affect?
Type 1; low concentration of von Willebrand factor that has variable severity
Doberman pinschers, Pembroke Welsh corgis, German shepherds
What is type 2 von Willebrand disease and what breeds does it affect?
Abnormal structure of von Willebrand factor that leads to moderate-severe signs; German short/wirehaired pointers
What is type 3 von Willebrand disease and what breeds does it affect?
von Willebrand factor is completely absent and leads to severe signs; found in the familial trees of Chesapeake Bay retrievers and Scottish terriers, and sporadically in blue heelers, Cocker spaniels, and labs
What are the clinical signs of von Willebrand disease?
Asymptomatic
Spontaneous bleeds of mucous membranes, gingiva, epistaxis, hematuria
Excessive bleeding after trauma/surgery/teething
How is von Willebrand disease treated?
Cryoprecipitate, fresh frozen plasma, fresh whole blood
Desmopressin acetate for type 1 (releases von Willebrand factor from endothelium)
What process of hemostasis is mainly affected in animals with von Willebrand disease?
Phase 1; primary hemostasis (mainly platelet adhesion)
How soon after blood collection should chemical measurments be performed?
Within one hour
What anticoagulant is found inside purple top tubes?
Na or K EDTA
What tube type should be used for CBCs and blood smears of mammals?
Purple top (EDTA)
Is it okay to use a purple top tube for chemical assays?
No
What type of anticoagulant is found in green top tubes?
(Na or Li heparin)
What tube type should be used for chemical assays?
Green top
Why should green top tubes not be used for mammalian CBCs and blood smears?
Causes clumping of WBCs and platelets, and interferes with staining of WBCs
What anticoagulant is found in blue top tubes?
Na or Li citrate
What tube type should be used for coagulation panels?
Blue top
What tube type should be used for collecting blood for blood transfusion?
Blue top
Why should blue top tubes not be used for CBCs?
Too much dilution
What are tiger/yellow top tubes?
Tubes containing silicone gel separators for separation of serum
Do red top tubes contain any additive?
No; allows blood to clot
What is blood plasma?
The fluid, cell-free portion of whole blood that has been treated with anticoagulants
What percentage of blood plasma is water?
90%
What constituents make up blood plasma?
Proteins, carbohydrates, vitamins, hormones, enzymes, lipids, waste products, antibodies
What is blood serum?
Blood plasma with fibrinogen removed, obtained from spinning down whole blood after coagulation in serum separator tubes
What constituents are found in higher amounts in blood serum versus blood plasma?
Lactate dehydrogenase, potassium, phosphate (all released from cells during the clotting process)
What constituents are found in higher amounts in blood plasma versus blood serum?
Protein (globulin; fibrinogen)
Is hemolysis most often due to pathology or artifact?
Artifact
What are the possible artifact causes of hemolysis?
Excessive suction, mixed too vigorously, forced through needle when transferring, frozen whole blood
How does hemolysis change sample values?
Elevated potassium, phosphorus, and enzyme levels
Interferes with lipase activity and bilirubin determinations
How should frozen whole blood be mixed after thawing?
Gentle inversions
What values can be affected by non-fasted blood samples?
Elevated blood glucose and phosphorous, postprandial lipemia, lowered renal values due to transient increase in GFR after eating
How do impedance analyzers work?
The cells impede/block the flow of current as they pass, the analyzer can determine values based on how much it was blocked. Can detect cell size and volume
What are histograms?
Helps us determine if our counts are accurute
How do laser flow cytometers work?
Focused laser beams evaluate size and density of solids; different cells scatter light differently based on granules, nuclei, shape, and volume
What are spectrophotometers?
Automated chemistry analyzers that work by measuring light transmitted by a substance
What are colorimeters?
Automated chemistry analyzers that work by using a filter to select a wavelength
What are reflectometers?
Automated chemistry analyzers that detect light reflected off a substance rather than transmitted light
What are end-point assays?
Tells of a value based on when a reaction reached a stable end point
What are kinetic assays?
Each specific enzyme catalyzes the reaction of a specific substrate and produces a specific product; measures rate of formations of the product
What are most photometric analysis procedures?
End-point assays
What is acid-base balance?
A steady state of pH
What is the normal blood pH range?
7.35-7.45
How are acidosis and alkalosis categorized?
By cause (respiratory vs. metabolic)
What is acidemia?
Abnormally low blood pH
What is acidosis?
Abnormally low pH of body tissues (increased H+ ions)
What is alkalosis?
Abnormally high pH of body tissues (decreased H+ ions)
What is alkalemia?
Abnormally high blood pH
What do normal metabolic processes continually generate?
Acids
Why are buffers needed?
Normal metabolic processes continually generate acids, buffers are needed to maintain normal pH of 7.4
What body systems is blood pH regulated by?
Renal and respiratory
What is the most prevalent buffer in the body?
Bicarbonate (HCO3)