biol 230 unit 4 + comprehensive final
1/160
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
161 Terms
hypersensitivity
immune response above normal, overreaction
allergen
antigens that trigger a Th2 response
exposure: skin contact, injection, ingestion, inhalation
type I - anaphylactic reaction
immediate, IgE antibodies
localized anaphylaxis
hay fever, hives.
restricted to area.
systemic anaphylaxis
anaphylactic shock, complete reaction, life threatening
mediator in anaphylactic reactions
crosslinking of allergens to IgE
use of allergy shots in desensitization
inject allergen in increasing concentration over time.
desensitize by switching IgE to IgG production, tricking immune system into blocking allergic response.
type II - cytotoxic reaction
intermediate, antibody.
blood typing!
transfusion reactions
when wrong blood type is transfused and classical compliment is triggered due to differing antibodies.
type III - immune complexes
intermediate, antibody mediated.
neutrophils phagocytose smaller antibody-antigen immune complex trapped in blood vessels damaging tissues.
post-streptococcal glomerulonephritis relating to type III
inflammatory disease damaging kidney tissues after a bacterial infection
type IV - cell-mediated hypersensitivity reaction
delayed, cell mediated.
TH1, Tc response
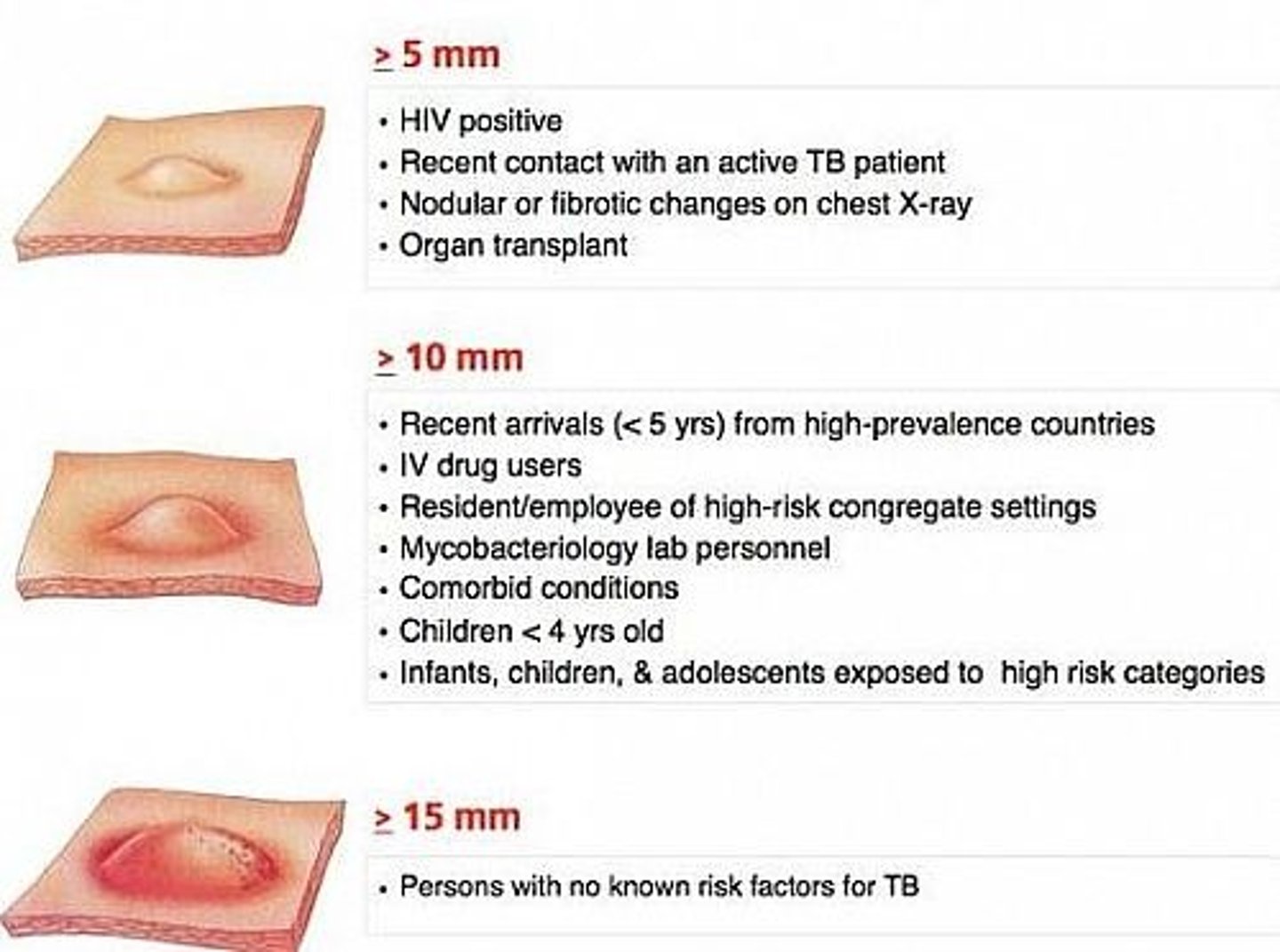
type IV in TB mantoux test
when exposed to TB -> Th1 response. mantoux tests for Tc by injecting TB protein.
positive mantoux test
- signs and symptoms
- exposure to TB, no symptoms
- vaccinated with BCG
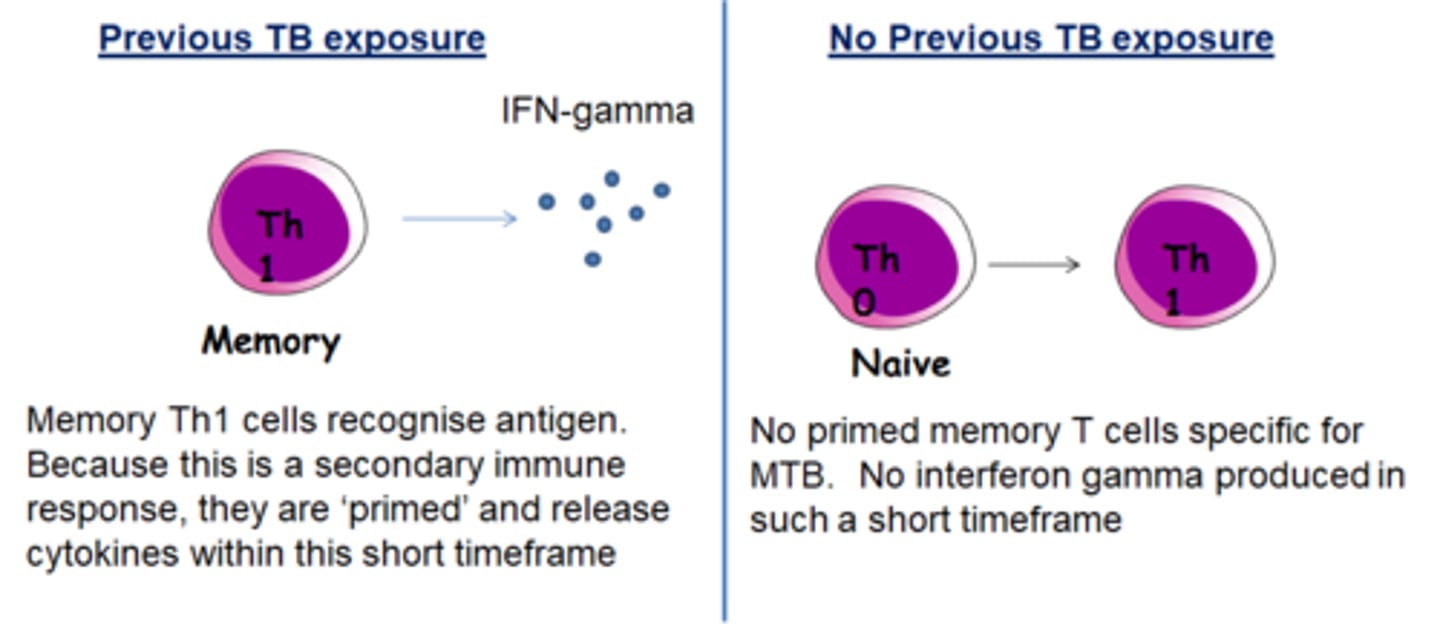
IGRA (interferon gamma release assay)
blood test separates vaccine and exposed groups.
TB antigen added to blood, interferon released if Tc activated by mantoux test
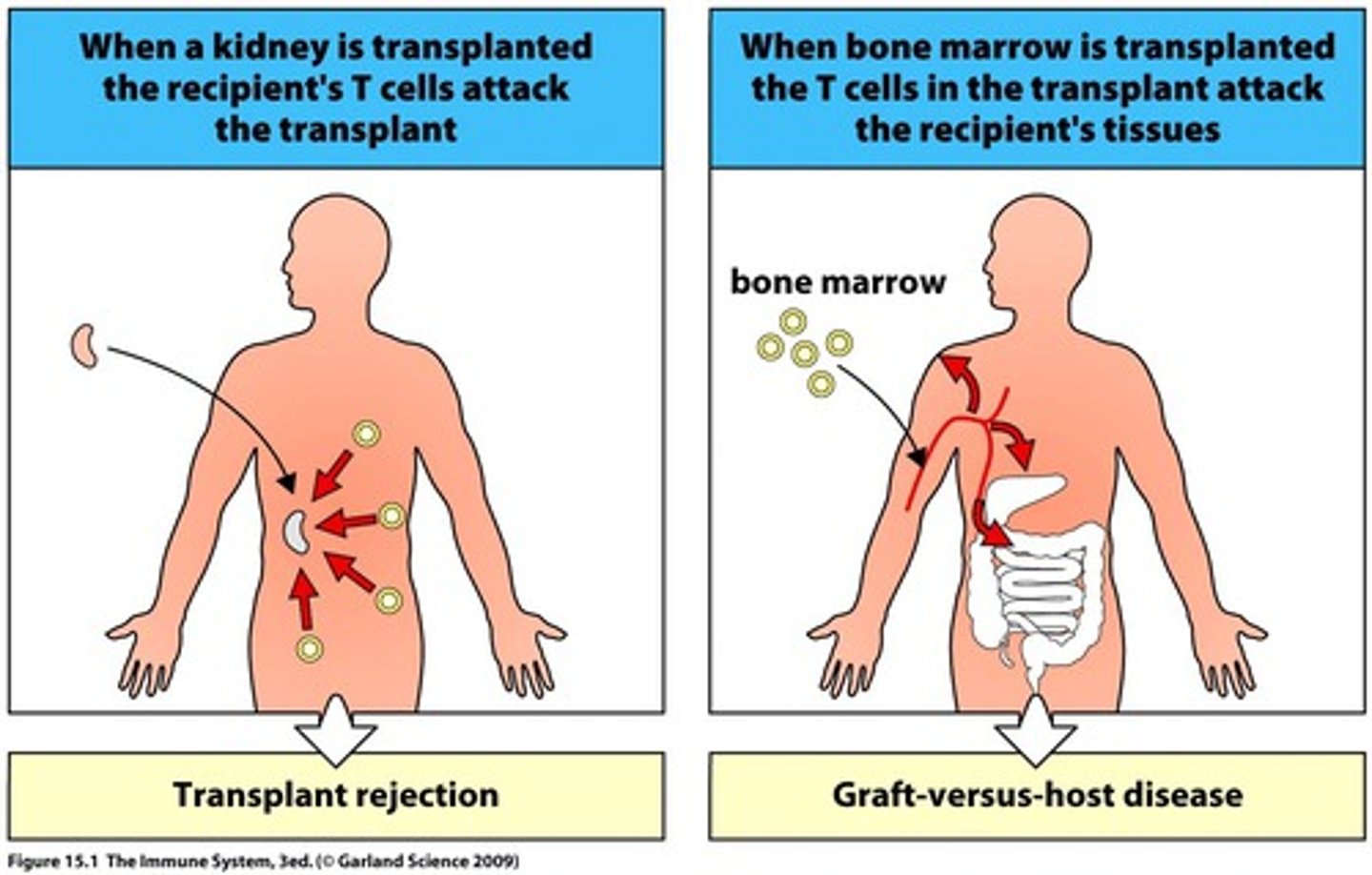
graft rejection
IV reaction due to foreign antibodies creating Tc response
auto immune disease
immune system attacks self
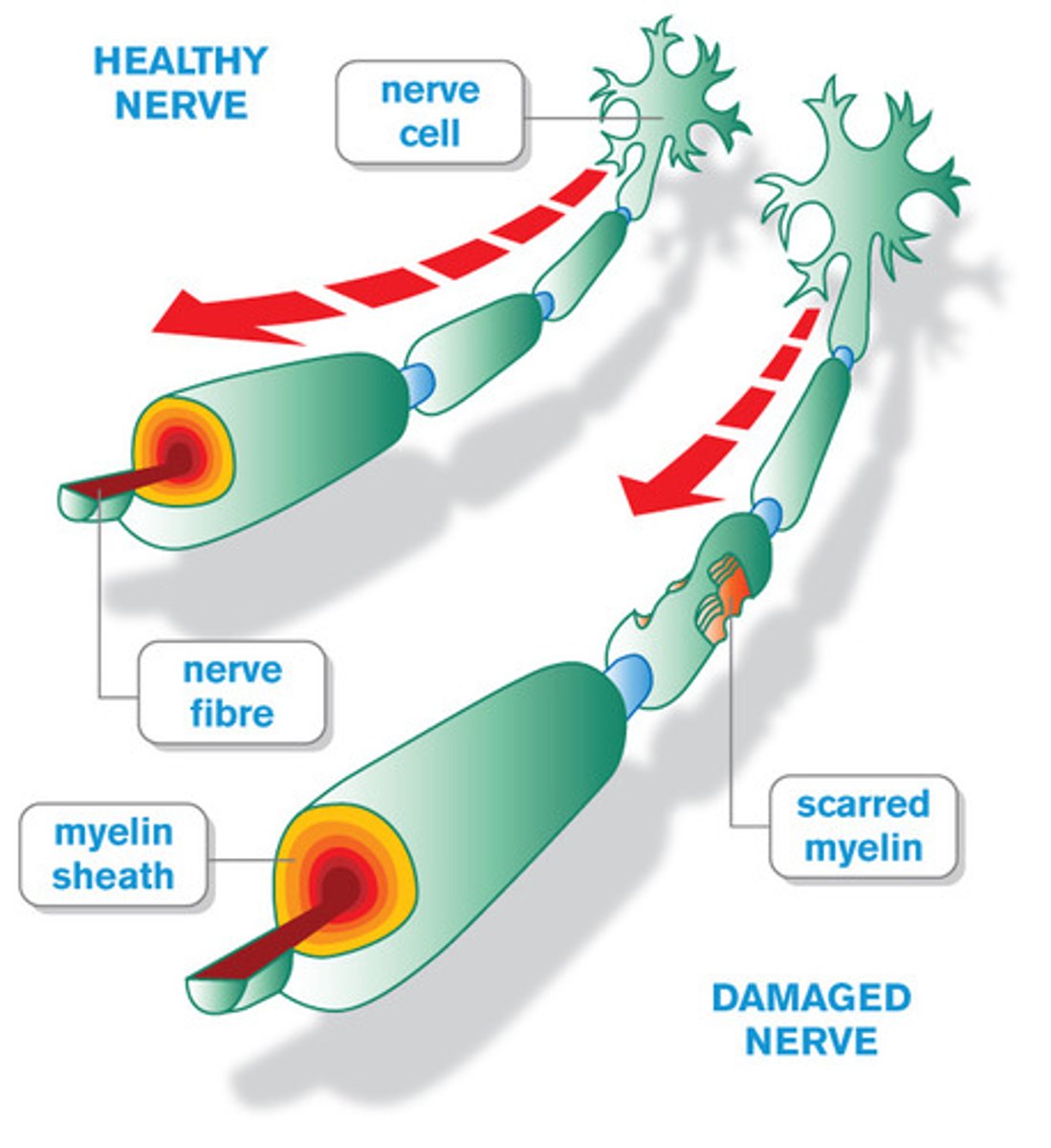
multiple sclerosis
type IV reaction.
caused by mono infection when CD8 is desensitized, transmigration into brain where myelin sheath is attacked. immune response to self.
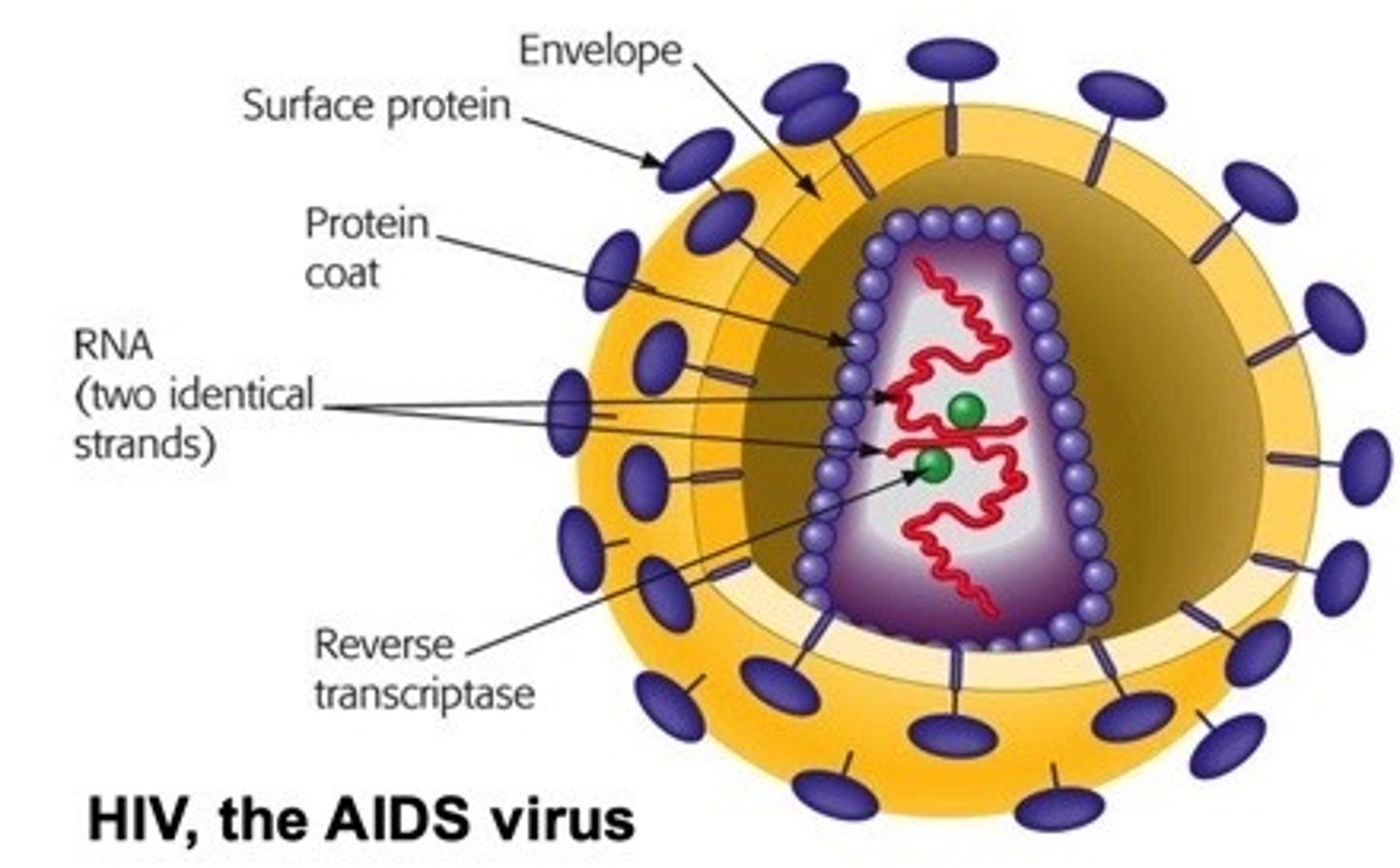
HIV/AIDS
single stranded RNA, enveloped, retrovirus
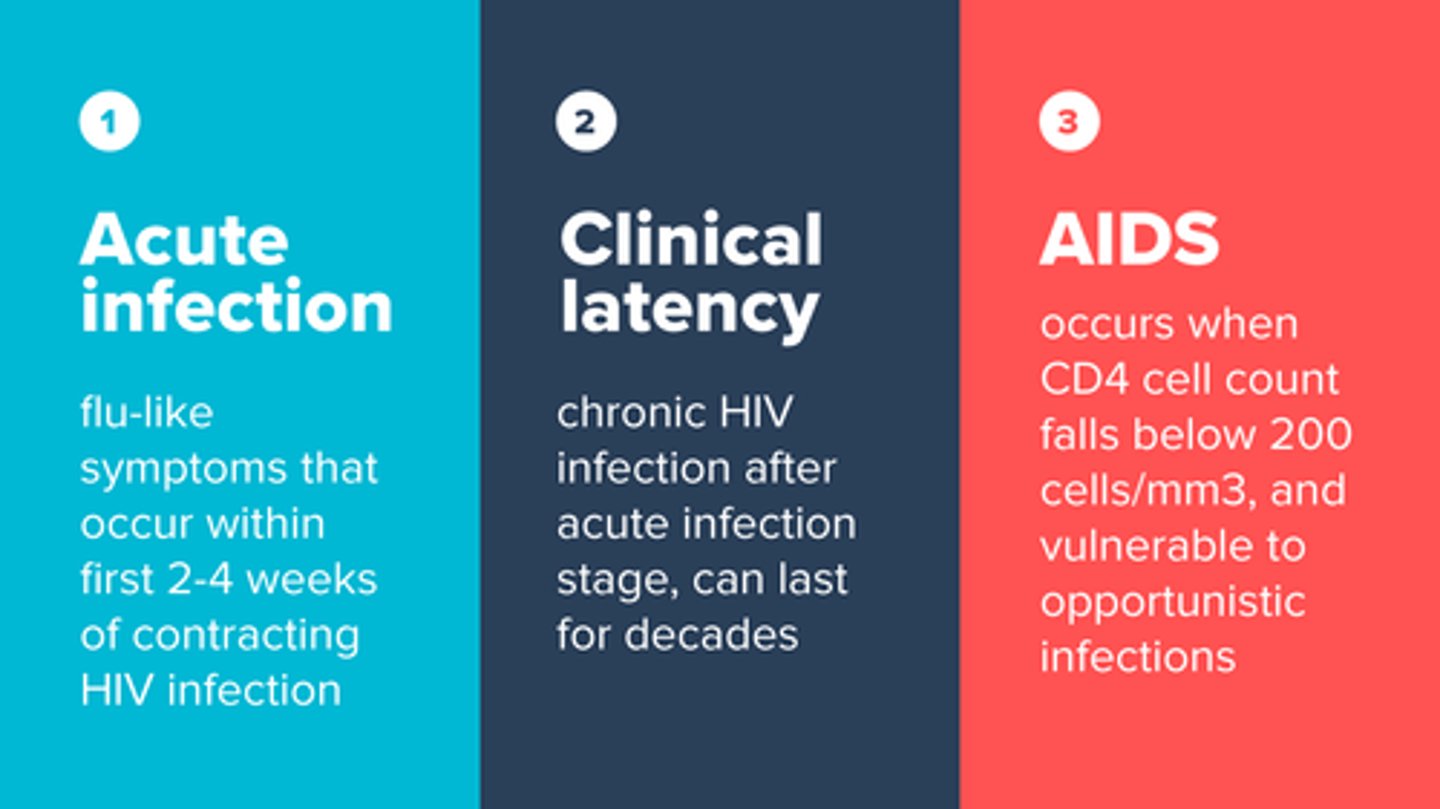
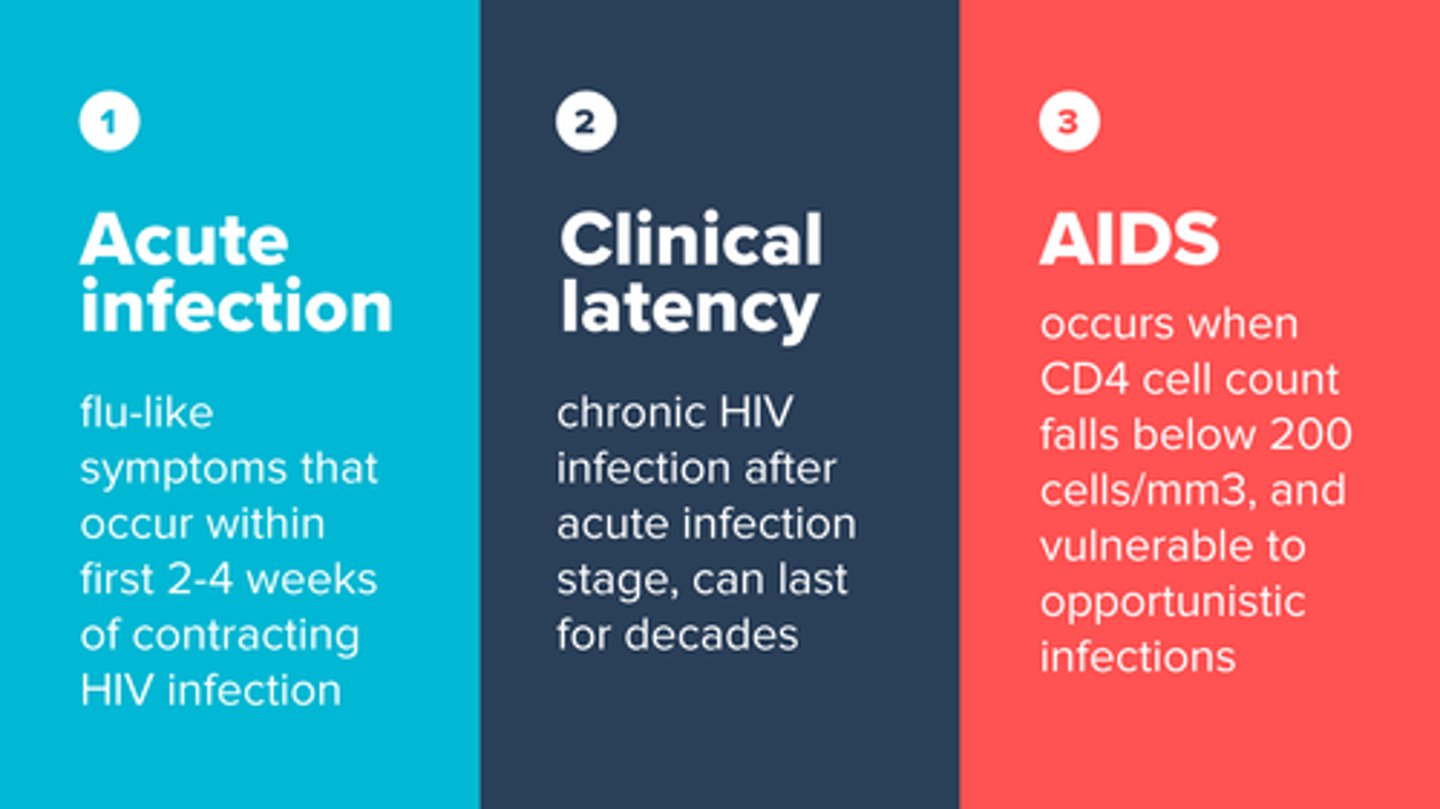
seroconversion
change in serologic tests from negative to positive due to development of antibodies post-exposure
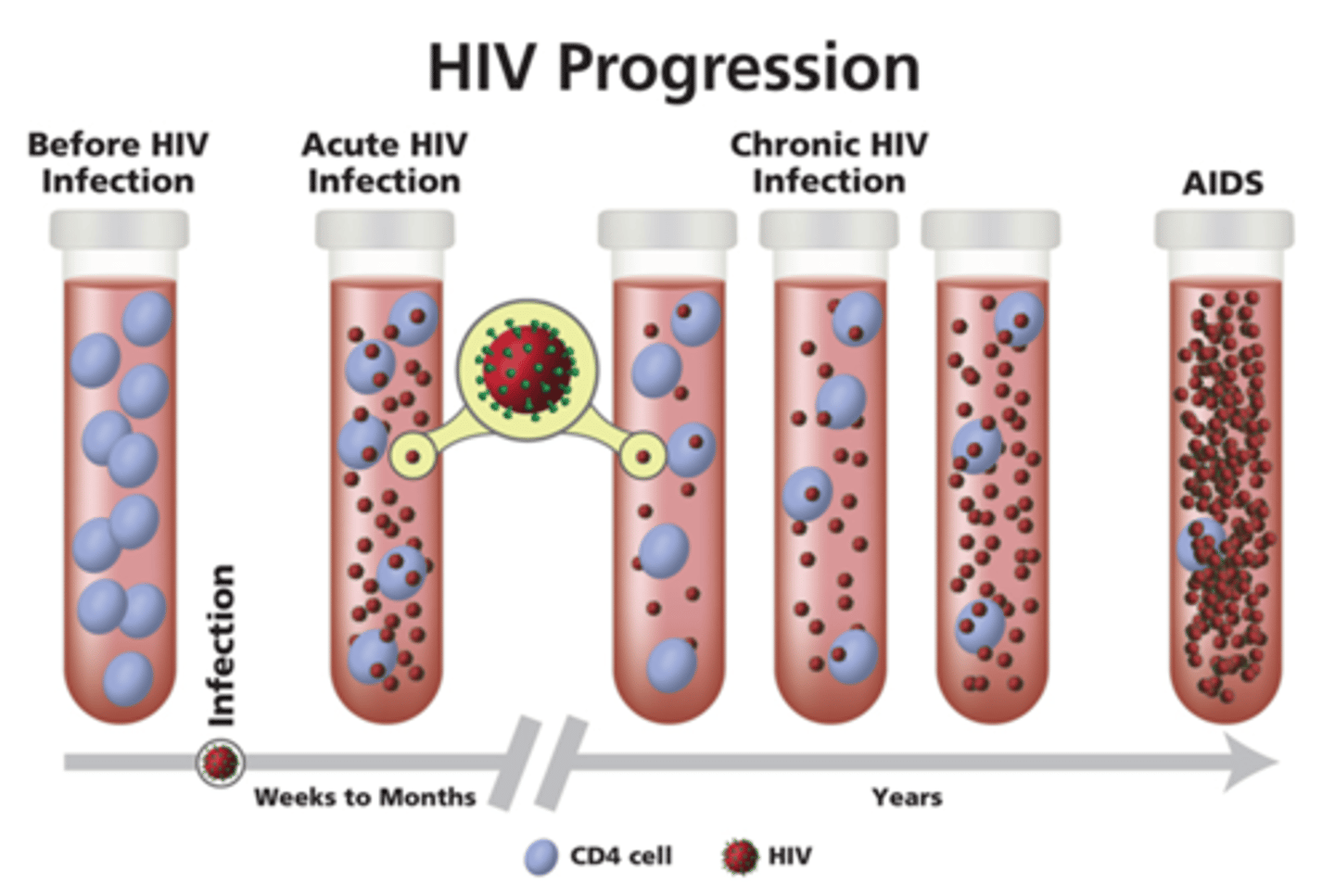
clinical AIDS
CD4+ count 20% below normal, venerable to opportunistic infections like kaposi sarcoma.
HIV latent state
HIV integrates into CD4 Th. after reverse transcription it never leaves & remains as reservoir
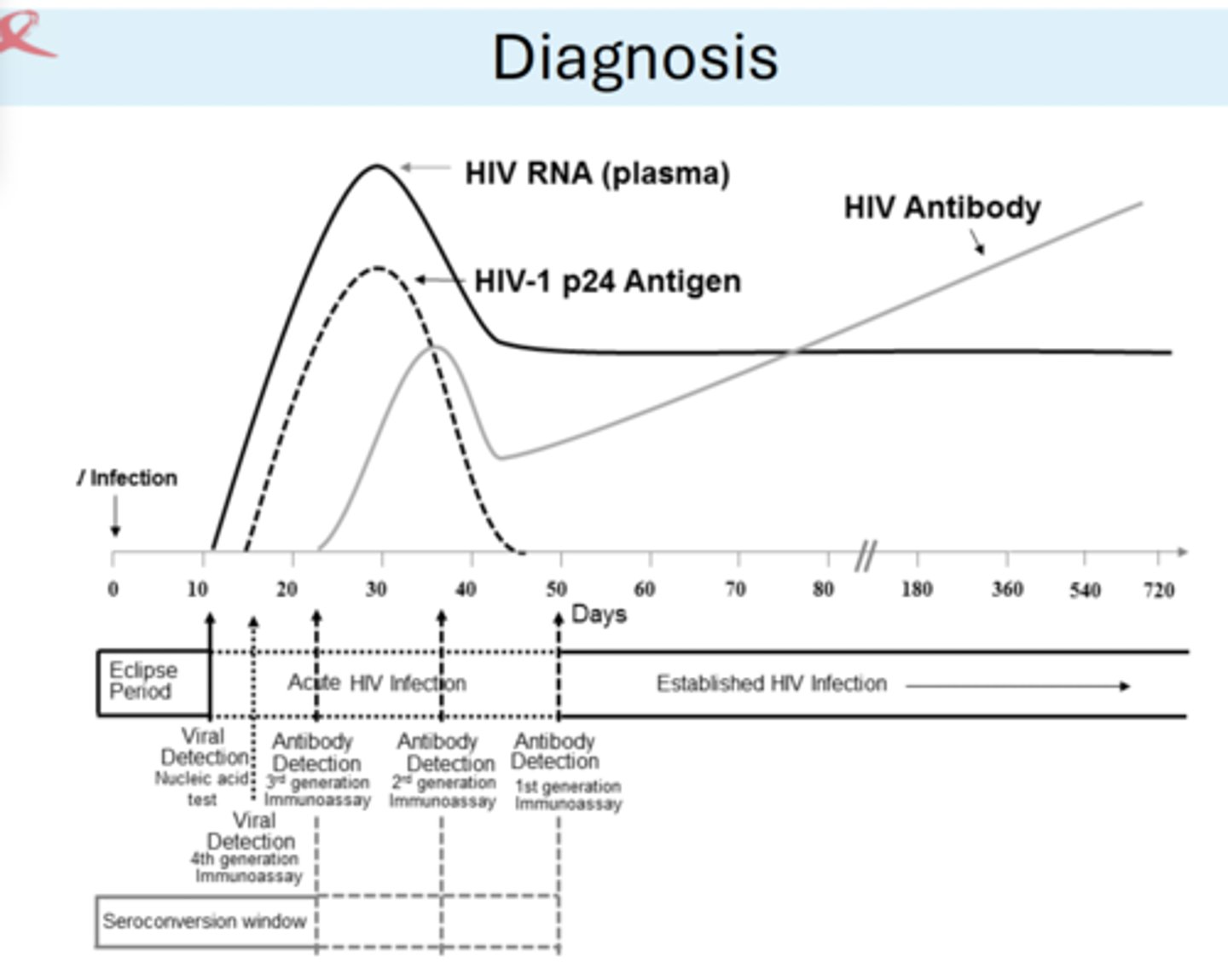
HIV testing
10 day period after exposure cannot be tested.
earliest: RNA test
45 days: western blot for presence of antibodies.
antigen/antibody tests most sensitive!
HIV portals of entry
direct contact/mucus membranes of genitals.
fomite (needles) with contaminated blood.
vaccine
suspension of all or part of microorganism to trigger active immune response
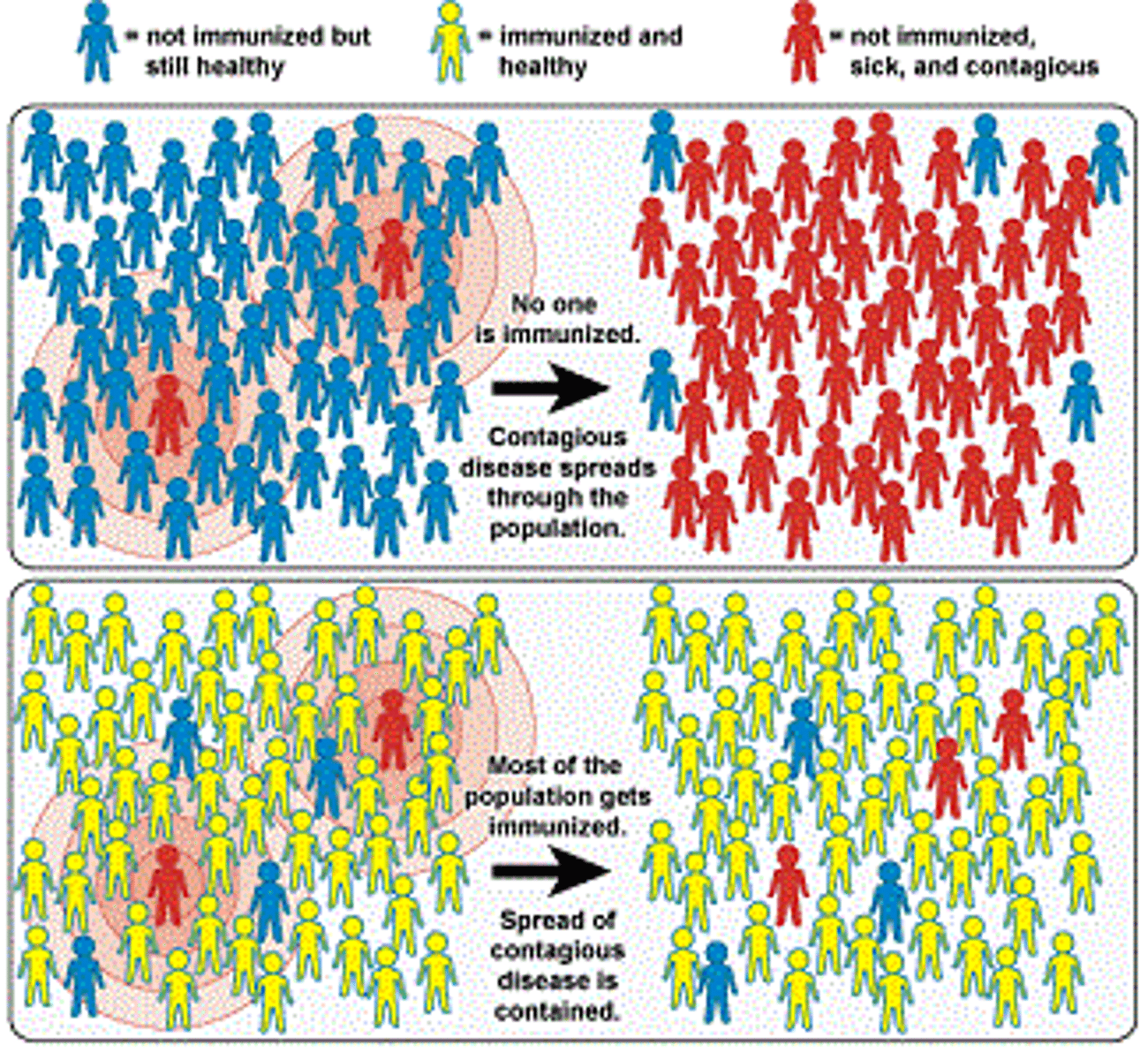
herd immunity
majority of population is resistant to antigen and pathogen cannot spread
attenuated vaccine
weakened whole bacteria/virus.
greater immune response, more effective but not as safe.
can revert to being virulent.
inactivated vaccine
"dead" bacteria incapable of infection but intact antigens still trigger immune response.
not always effective but very safe.
poliovirus
replicates in intestines. can cause paralysis if gets to spinal cord by blood.
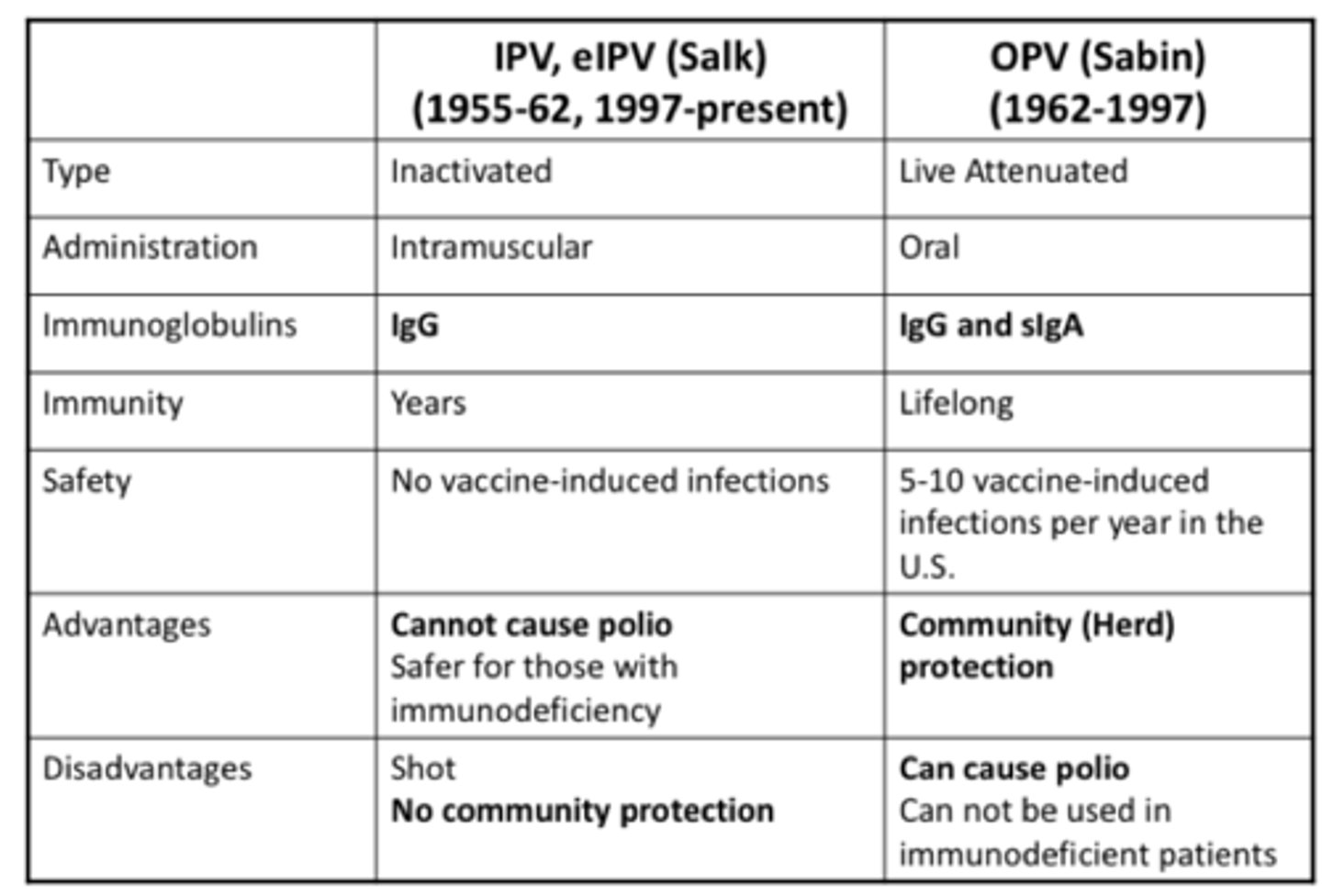
salk vaccine
inactivated shot.
IgG stops paralysis but no IgA gut immunity to prevent replication.
sabin vaccine
attenuated oral.
IgA gut immunity stops replication and transmission.
use of salk versus sabin
salk used in polio free countries due to low risk if reverted.
sabin used in polio endemic countries where immunity needs to be easily distributed.
toxoid vaccines
exotoxin of pathogen inactivated

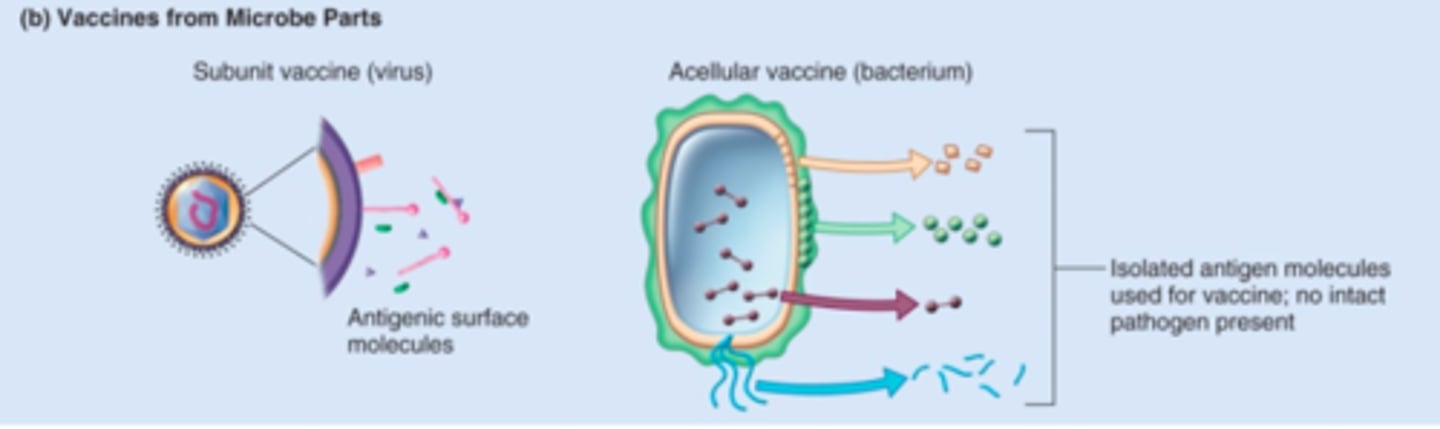
disrupted cell/acellular vaccines
most antigenic parts of a microorganism, not whole, used to stimulate immune response
recombinant vaccines
DNA for antigenic proteins put into yeast, purified, and only antigenic protein is ued in vaccine
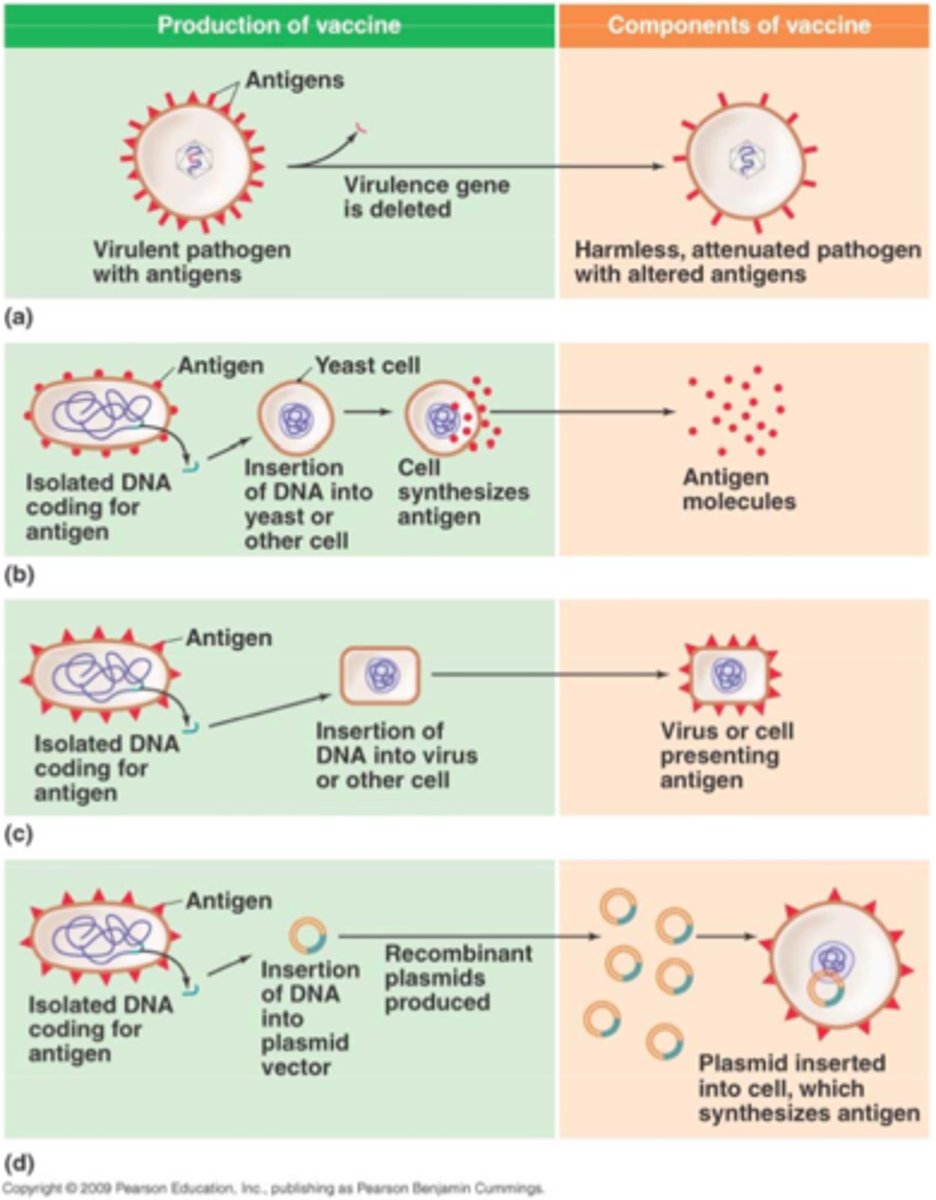
antibody-sandwich (direct)
FC region of antibody attached to bottom of well, patient sample added and antigen binds. enzyme linked antibody binds to patient antigen. when substrate added, color change concludes positive for antigen.
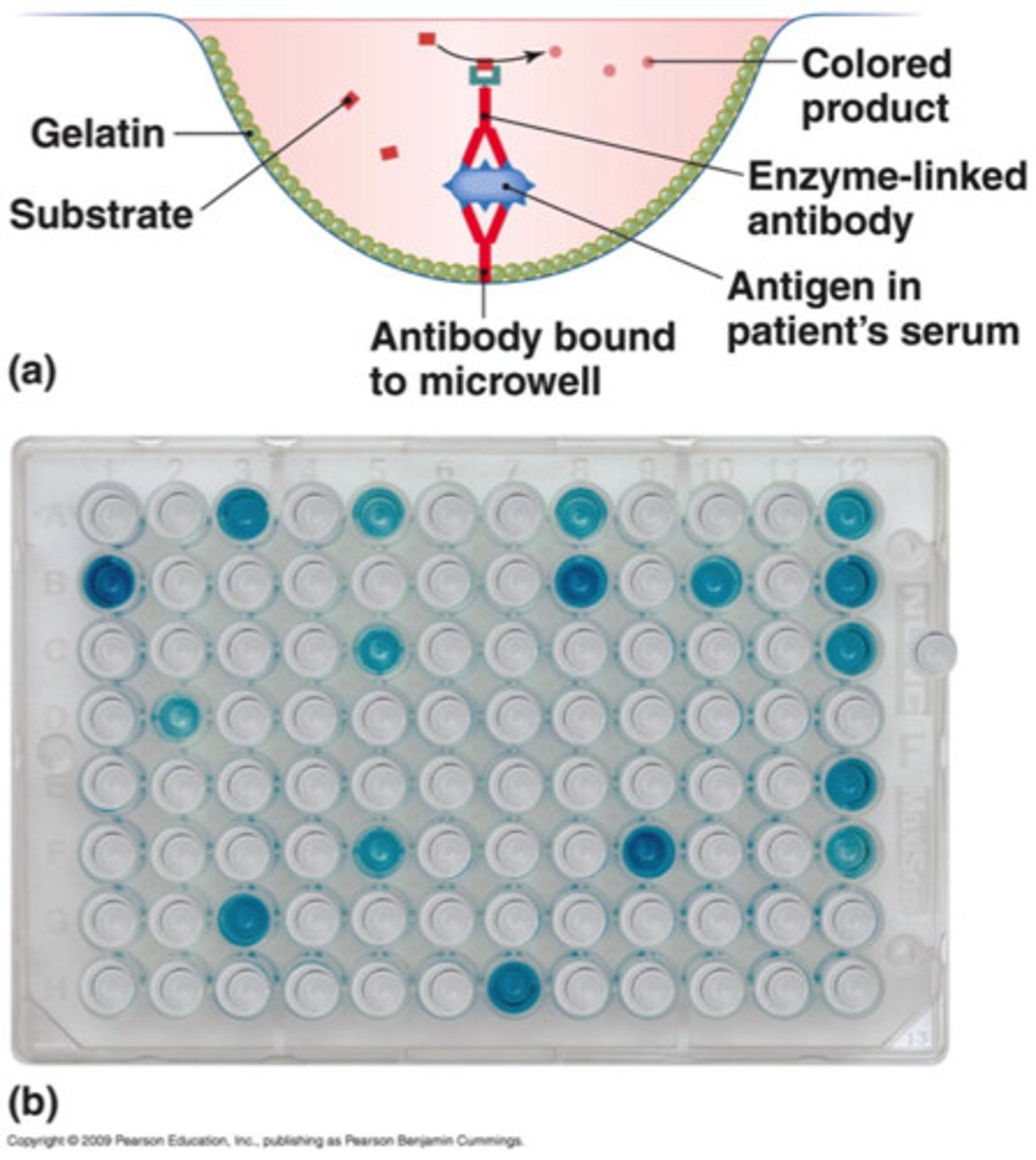
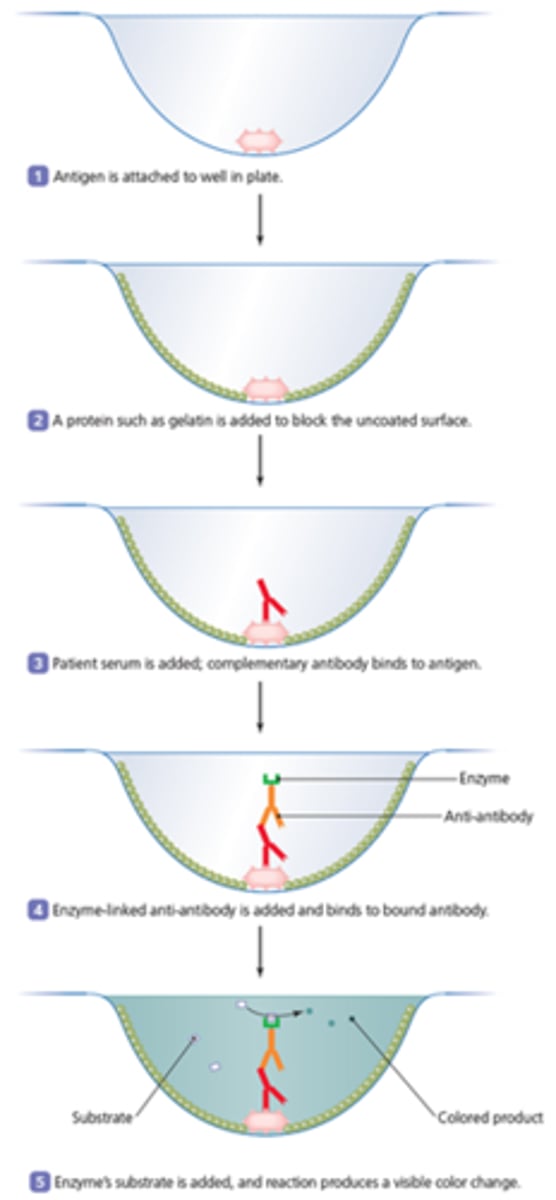
indirect ELISAs
(enzyme-linked immunosorbent assay)
antigen attached to well. patient sample added for antibody to bind to antigen. enzyme linked antibody added to bind to patient antibody. color change concludes positive for antibody
sterilization
eradicate all microbial life

disinfection
eradicate all vegetative pathogens, not spores

antisepsis
eradicate vegetative pathogens on skin
degerming
scrubbing to remove microbes on skin
bacteriostatic
stopping bacterial growth
bactericidal
killing bacteria
asepsis
absence of pathogens

sepsis
presence of pathogens
boiling
disinfecting.
gets rid of some but not all microbes
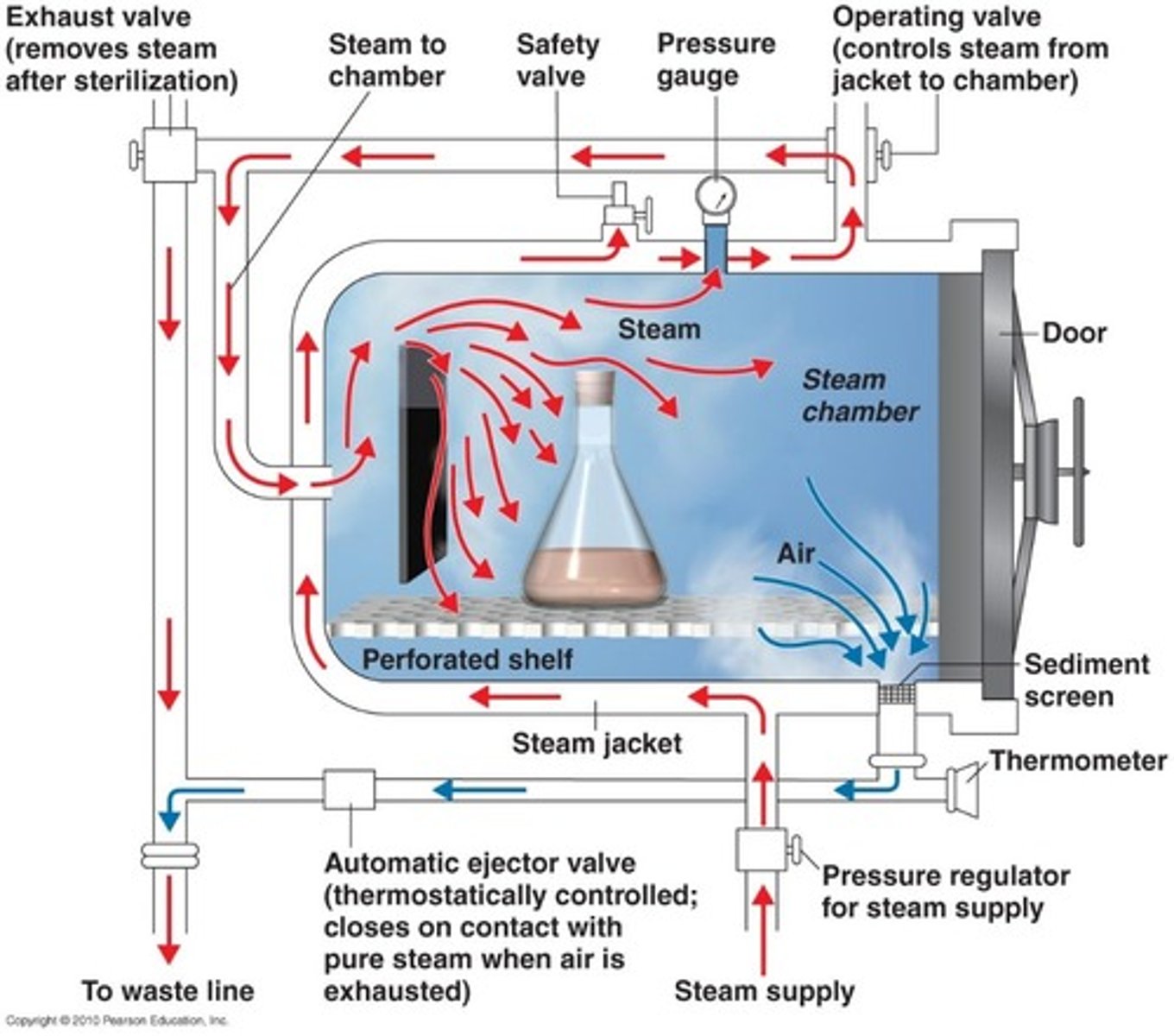
autoclaving
sterilizing.
steam and pressure at high temps to kill all
thermal death point
lowest temp where all organisms killed in 10 min
thermal death time
shortest time all microbes are killed at a given temperature
pasteurization
moist heat treatment of milk to remove pathogens.
not sterilizing.
types of pasteurization
historic: originally used for wine.
high temperature, short time (flash).
ultra high temperature.
filtration
removes bacteria, not cidal or static
low temperatures
-80 C freezer, static. stops growth by stopping division
osmotic pressure
salt! static, stops division by plasmolysis (shrinking of call wall)
desiccation
static. drying fruit.
radiation
cidal.
UV disinfecting, gamma sterilizing
phenols, bisphenols, and phenolic
denature proteins, disrupt membranes.
harsh on skin, bac can develop resistance.

alcohols
denature proteins, disrupt cell membranes.
halogens
denature proteins.
Br, Cl, F, I
oxidizing agent
H2O2 denature proteins.
disinfectant and antiseptic.
surfactants
disrupt cell membrane.
removal of pathogens.
soaps degerm
heavy metals
denature proteins.
silver & arsenic
aldehydes
crosslinking between protein and DNA causes all movement to stop in cell.
can be sterilizing.
gaseous agents
sterilize by crosslinking proteins and nucleic acids.
ethylene oxide
tincture
disinfectant dissolved in OH increases effectiveness
factors effect disinfectants
temperature, surface, number of microorganisms
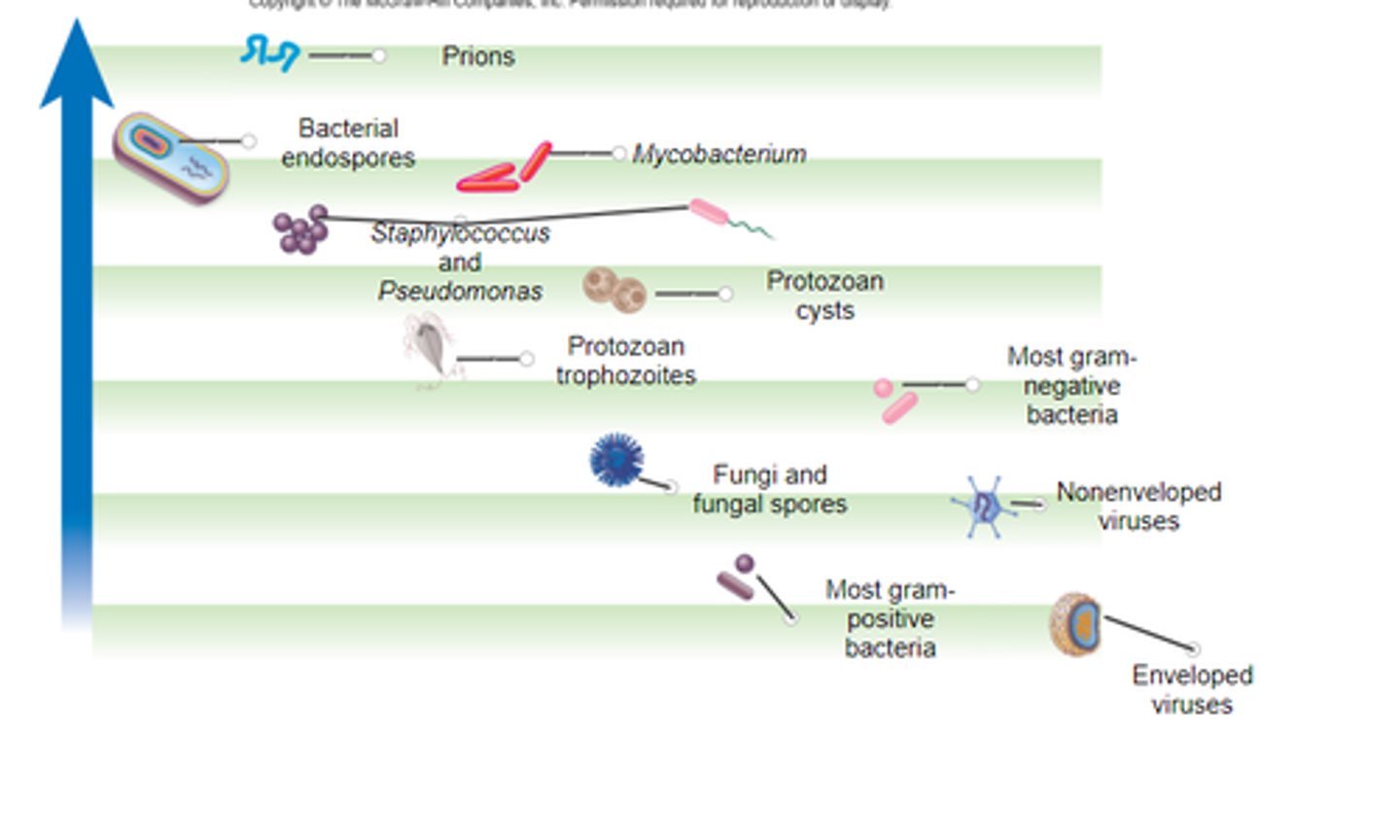
microbial structures from most resistant to least
endospores
mycobacterium
protozoan cysts
vegetative protozoa
gram neg bac
fungi
non enveloped viruses
gram pos bac
enveloped viruses
antibiotic
one organism inhibits another organism's growth
spectrum of microbial activity
number of different pathogens present
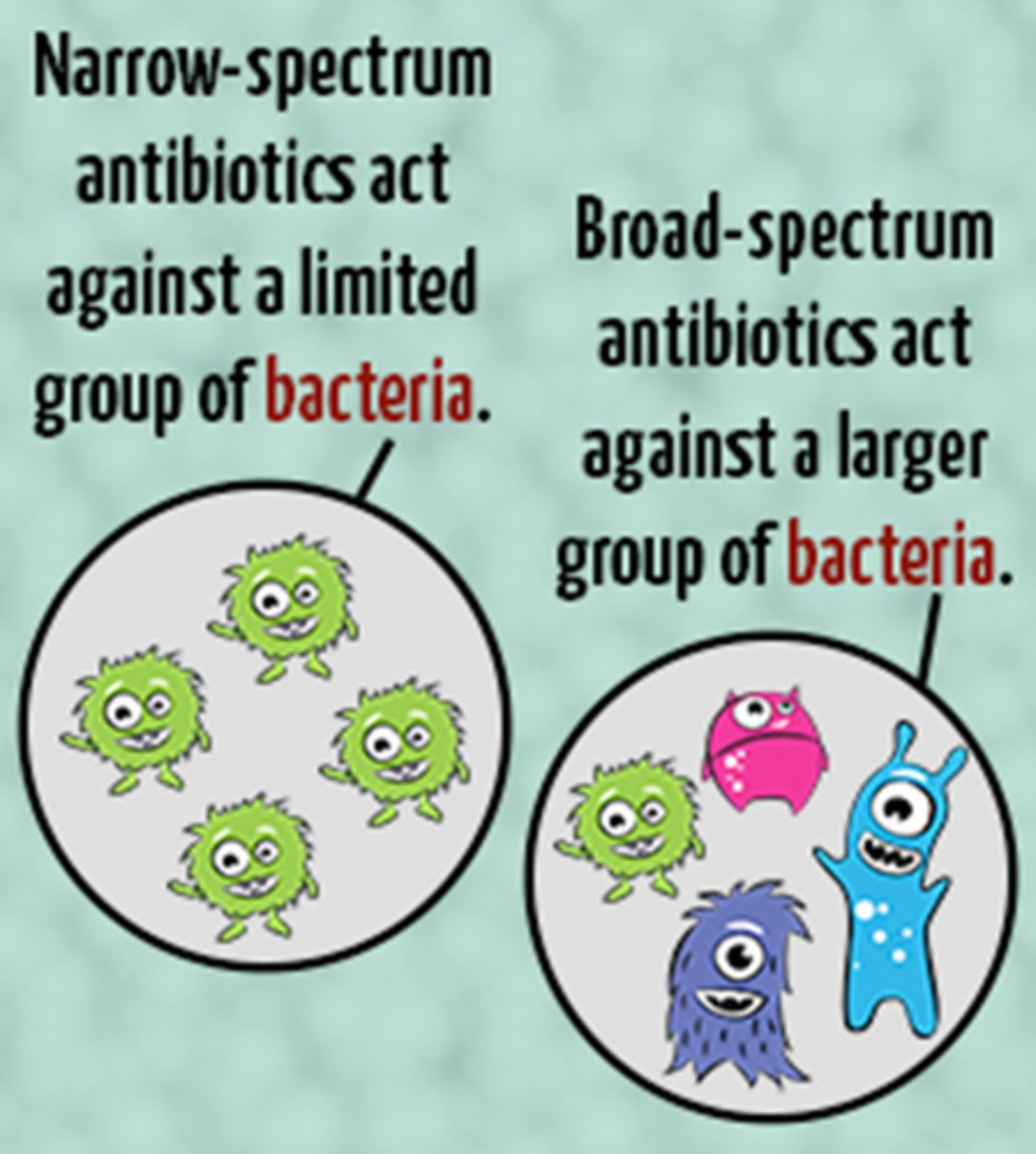
broad-spectrum antibiotics
activity against several different types of pathogens
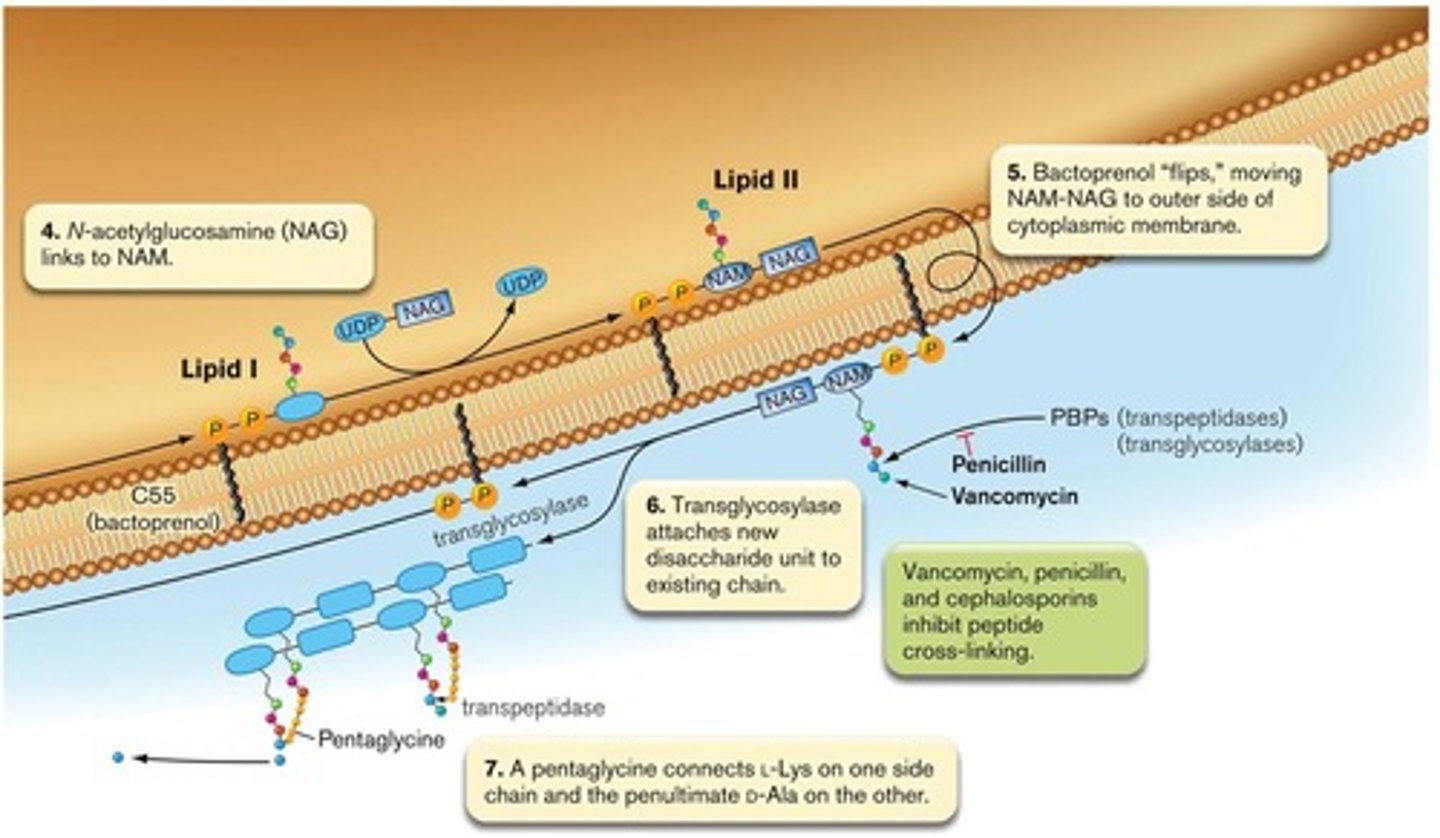
inhibitors of cell wall synthesis
penicillin blocks cross links in peptidoglycan
inhibitors of protein synthesis
erythromycin binds to 50s subunit and blocks A site so no new tRNA can enter
(human ribosomes slightly larger and can block binding)
inhibitors of nucleic acid synthesis
ciprofloxacin targets enzyme to inhibit DNA replication
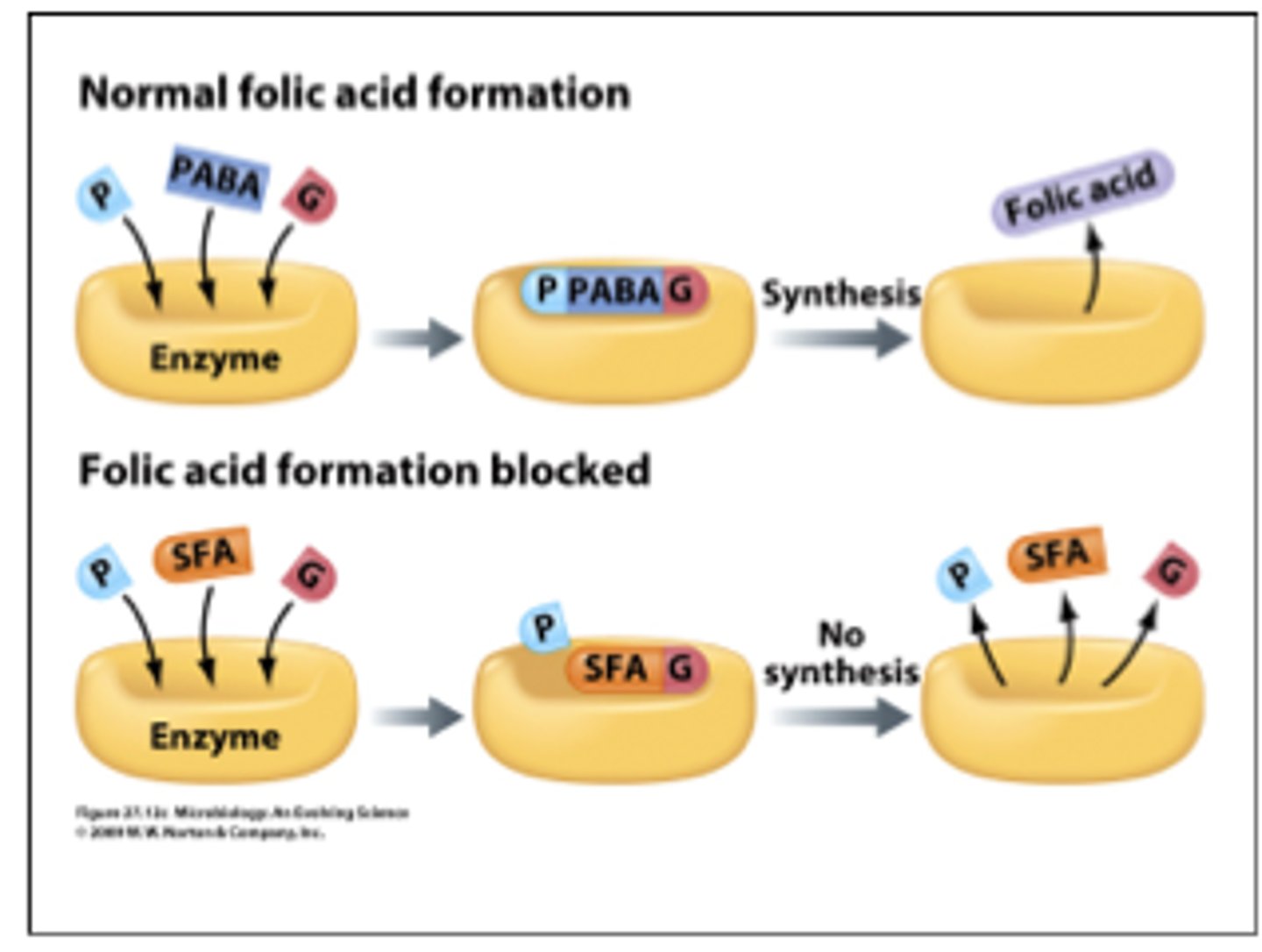
inhibitors of metabolic synthesis
sulfa drugs inhibit folic acid production so no nucleotides are produced.
competitive inhibitor blocking enzyme from binding
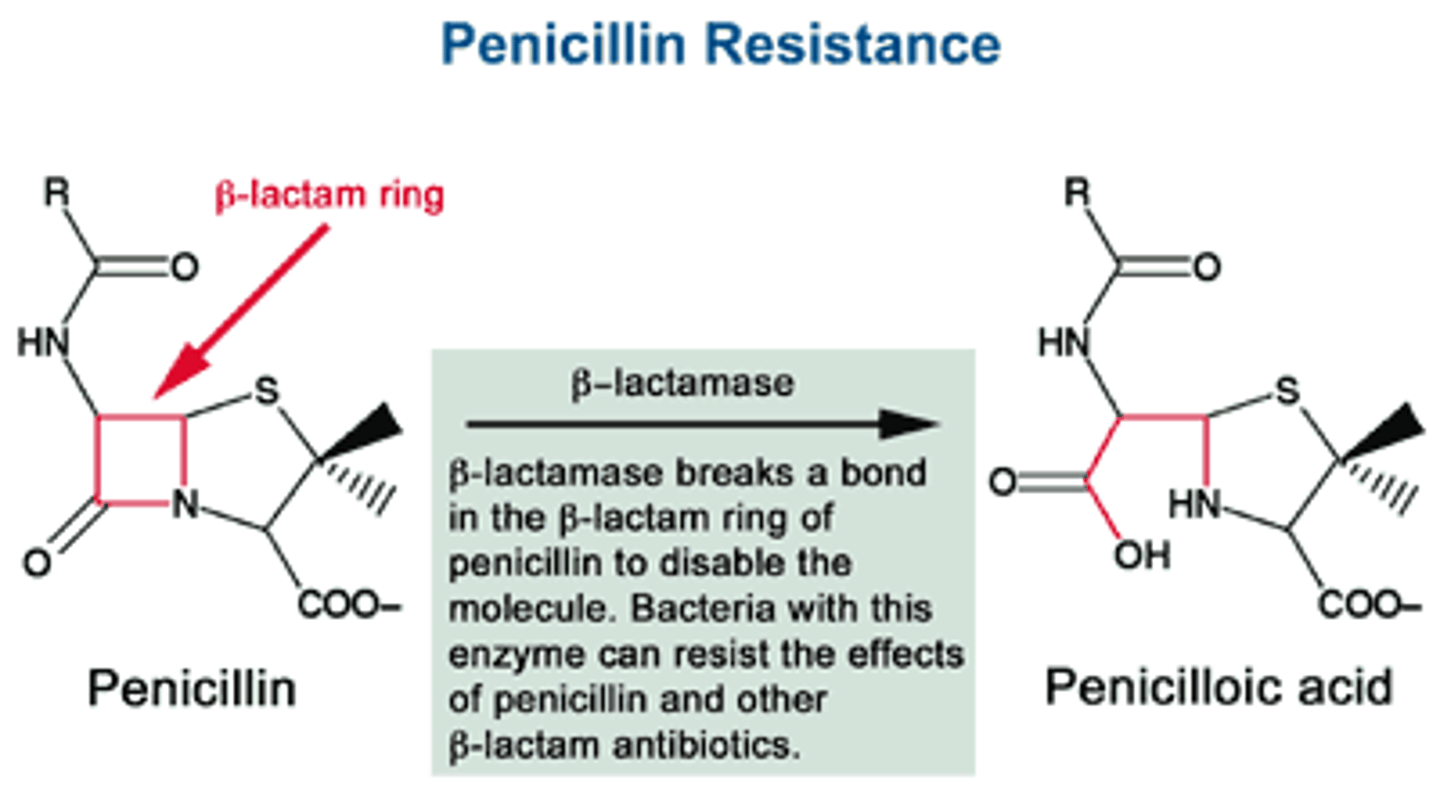
clavulanic acid in augmentin
inhibits penicillinase by irreversibly inactivating beta-lactamase which allows for penicillin resistance
drug inactivation
bac produce enzyme to block antibiotics
decreased permeability
microorganism blocks drug from entering cell
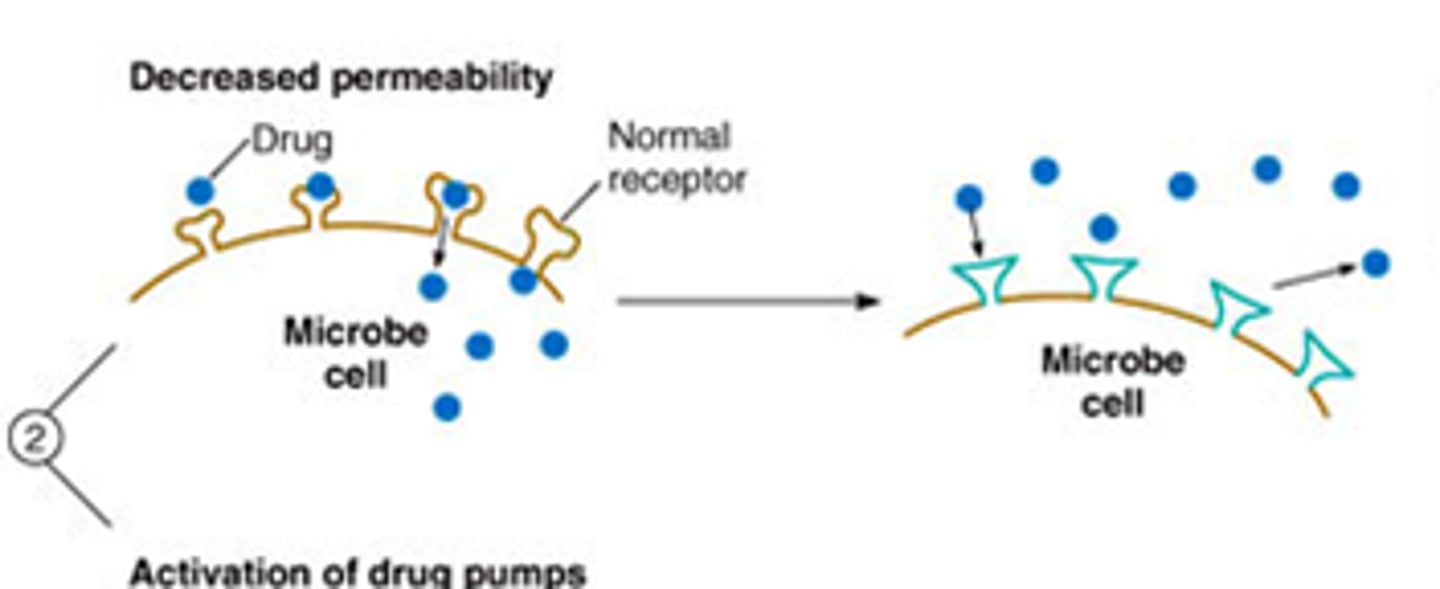
activation of drug pumps
protein structures on membrane pump drugs out of bacteria
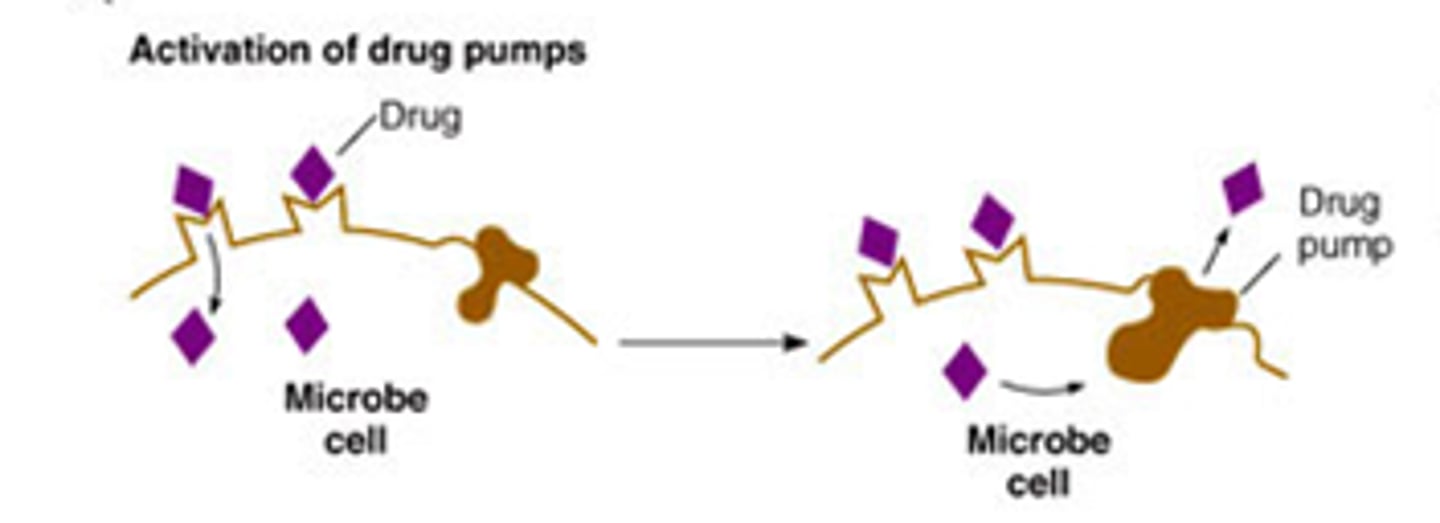
alteration of binding site
change in sequence of the 50s subunit so drug cannot bind
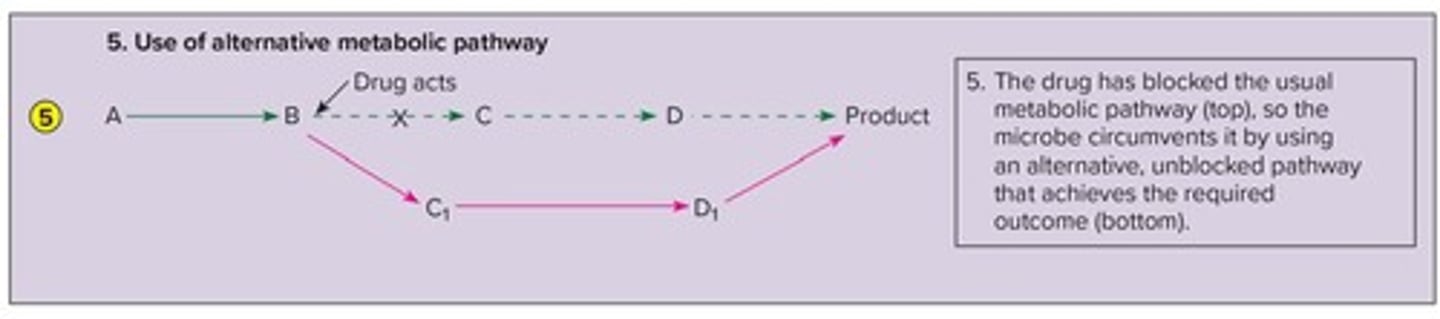
alternative metabolic pathway
bacteria get enzymes to go around antibodies using a different synthesis pathway.
mutations caused by gene transfer!
effectiveness of antimicrobials
kirby-bauer: disc on lawn
minimal inhibitory concentration: how much needed to inhibit bac
ketoconazole
antifungal.
blocks production of membrane ergosterol
metronidazole
breaks up DNA in anaerobic protozoa and bac.
vaginal infections!
quinine derivatives
treebark! used against plasmodium (malaria) by inhibiting formation of digestive vacuole.
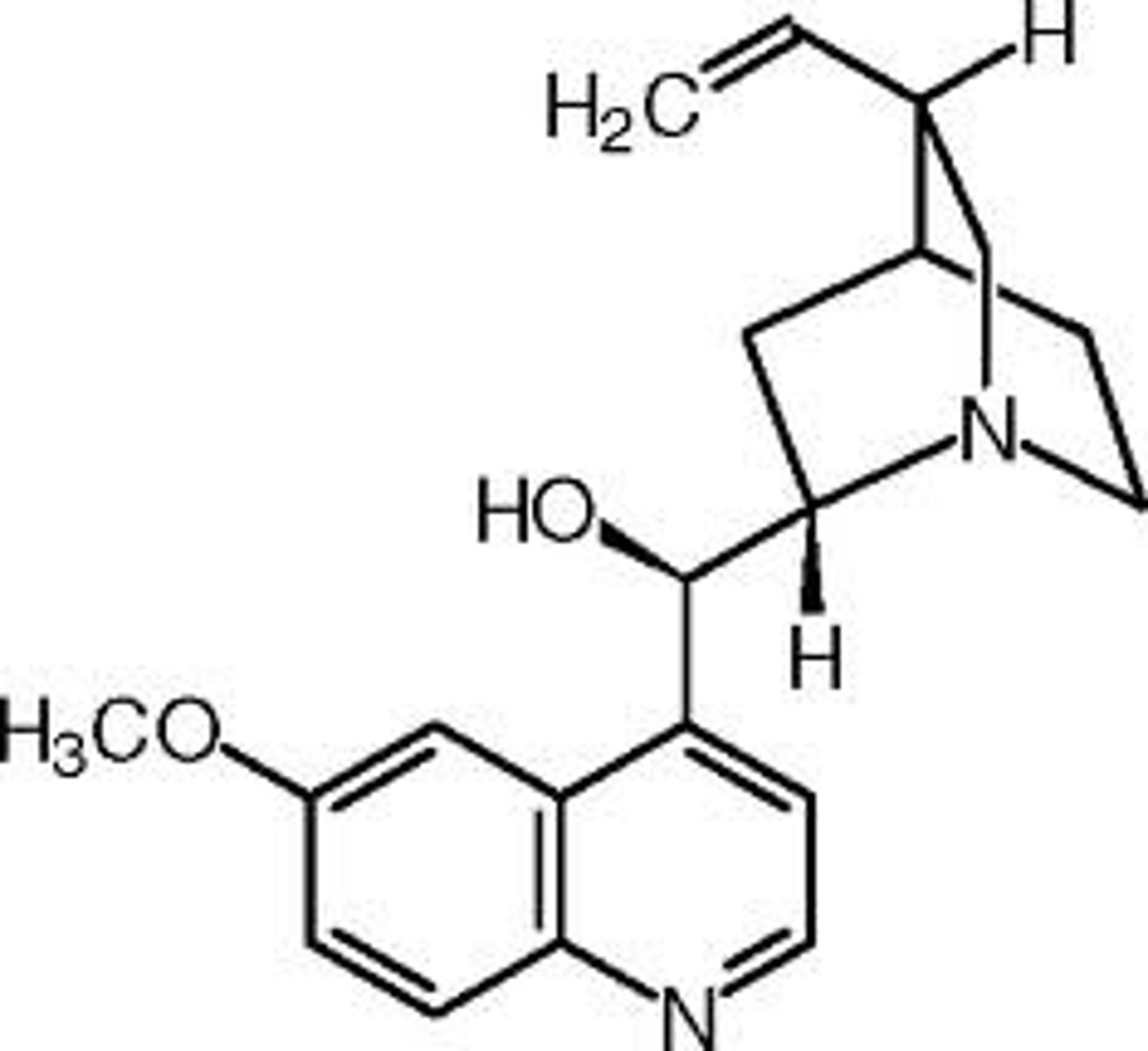
artemisinin
chinese wormwood used against plasmodium, free radicals caused by the cleavage of bonds oxidizes cells
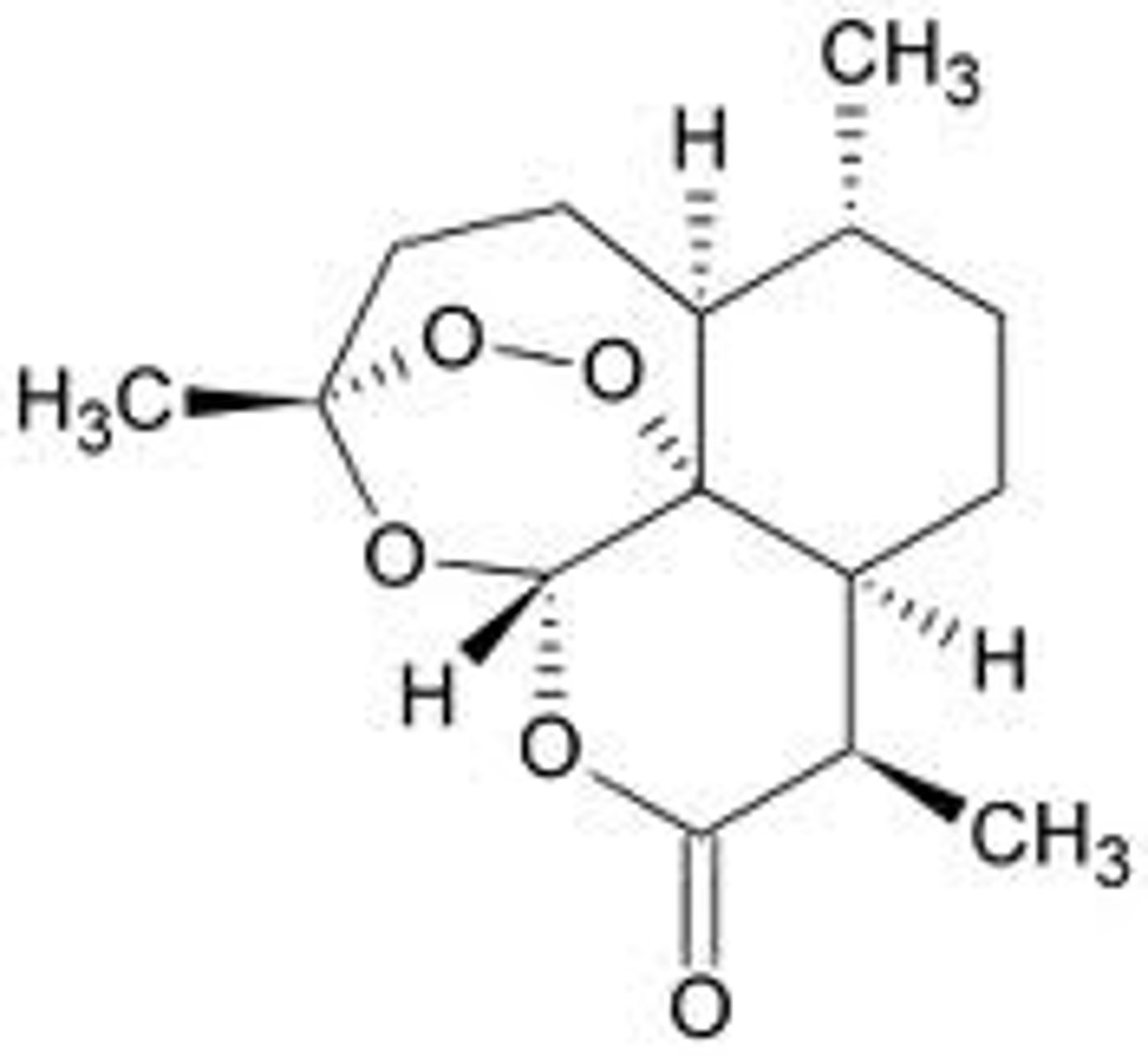
arsenicals
melarsoprol used against early stage african sleeping sickness (Trypanosoma brucei) by inhibiting enzymes
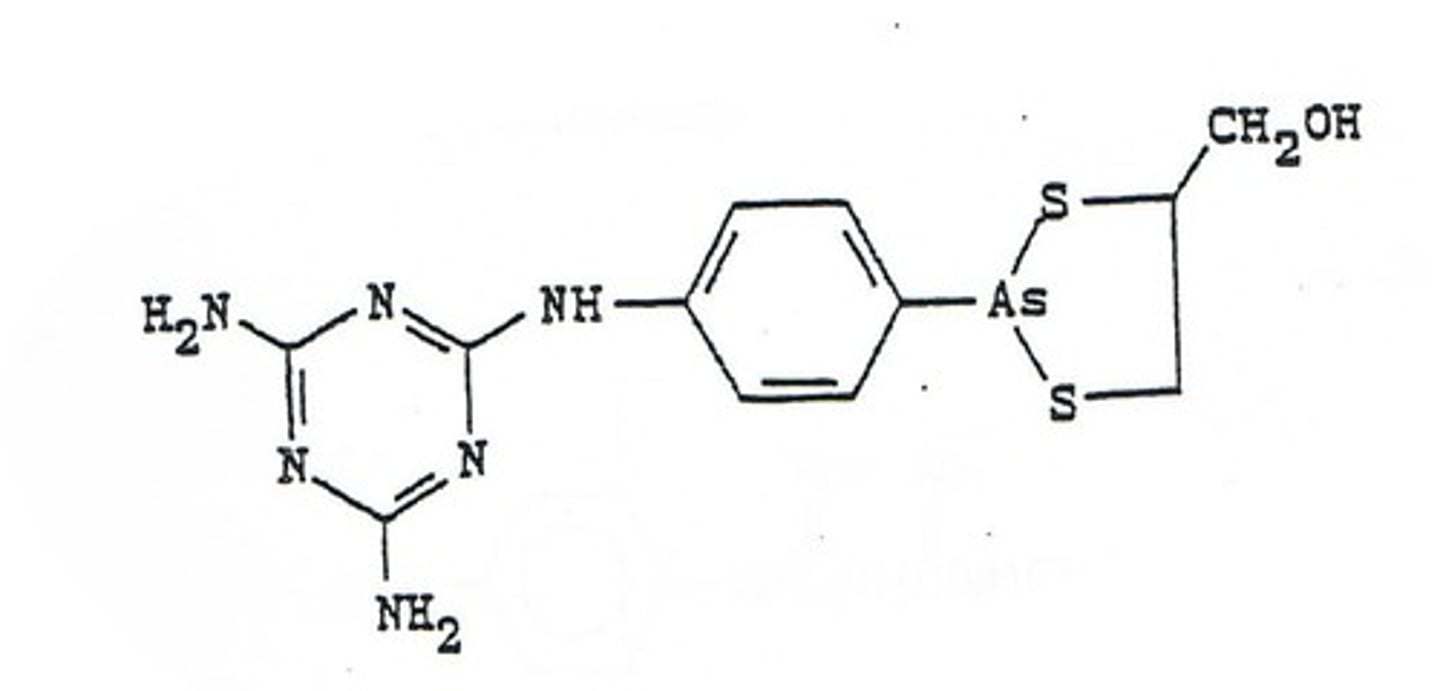
eflornithine
used against late stage Trypanosoma brucei by competitive inhibition
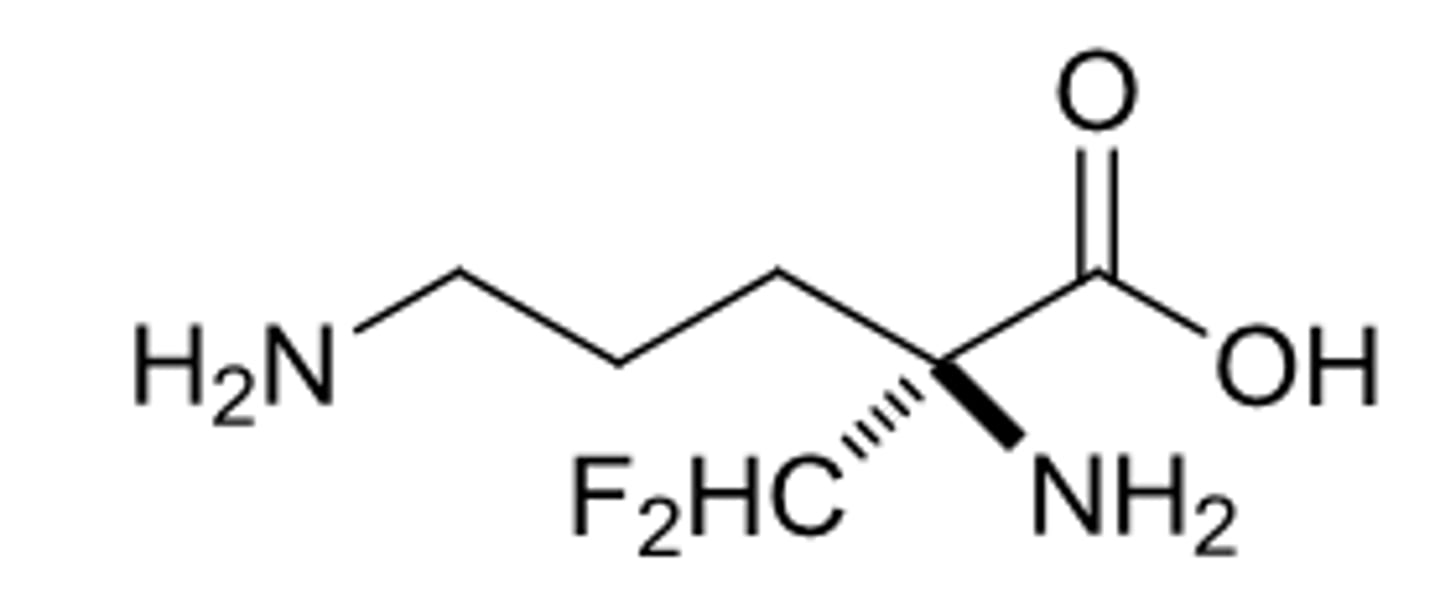
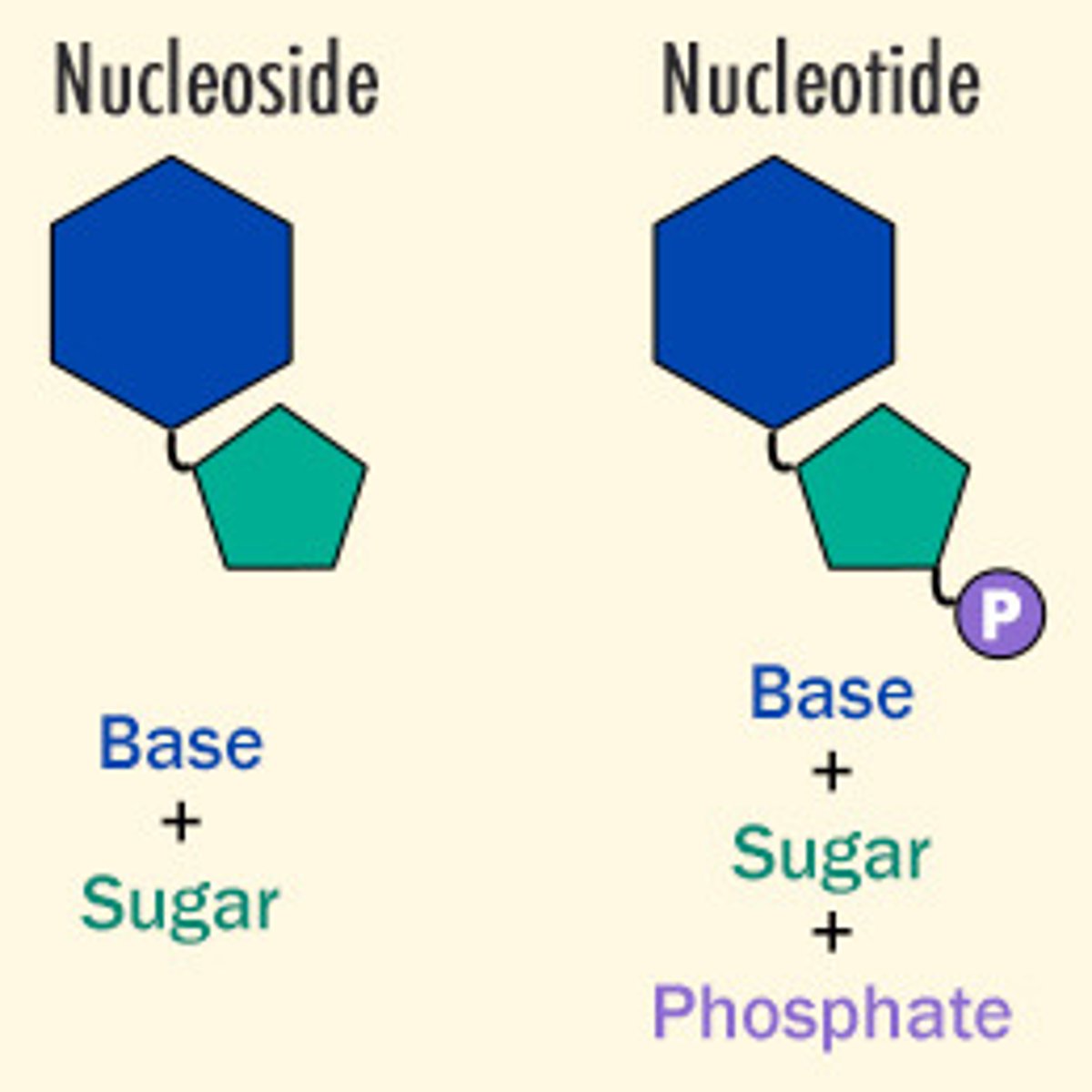
nucleoside
nucleotide lacking a phosphate group
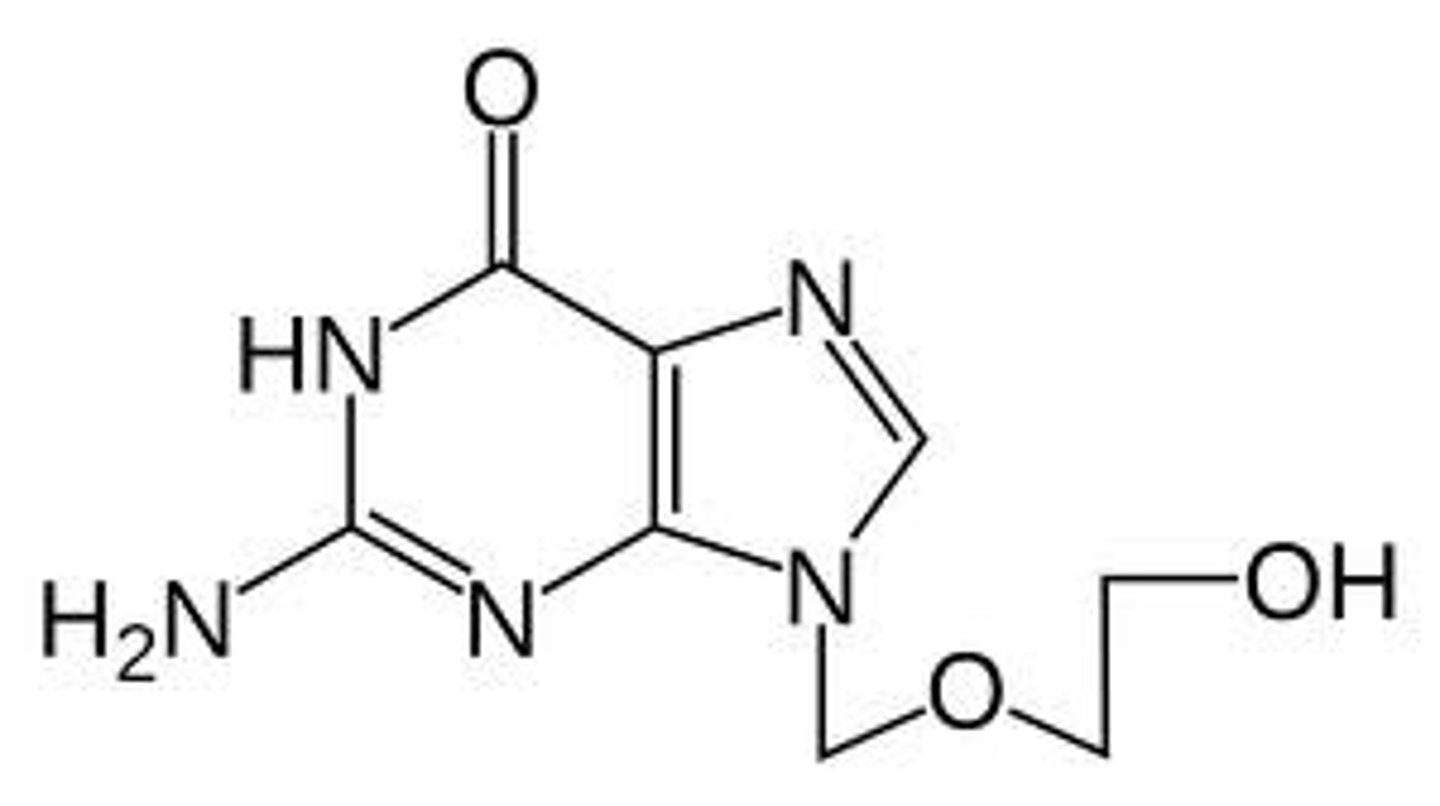
acyclovir
nucleoside analog looks like guanine. picked up by herpes and blocks replication
AZT (zidovudine)
analog against HIV looks like thymine to block reverse transcription
crixivan (indinavir)
protease (HIV enzyme) inhibitor.
GAG POL precursor protein inhibited from cleaving into proteins.
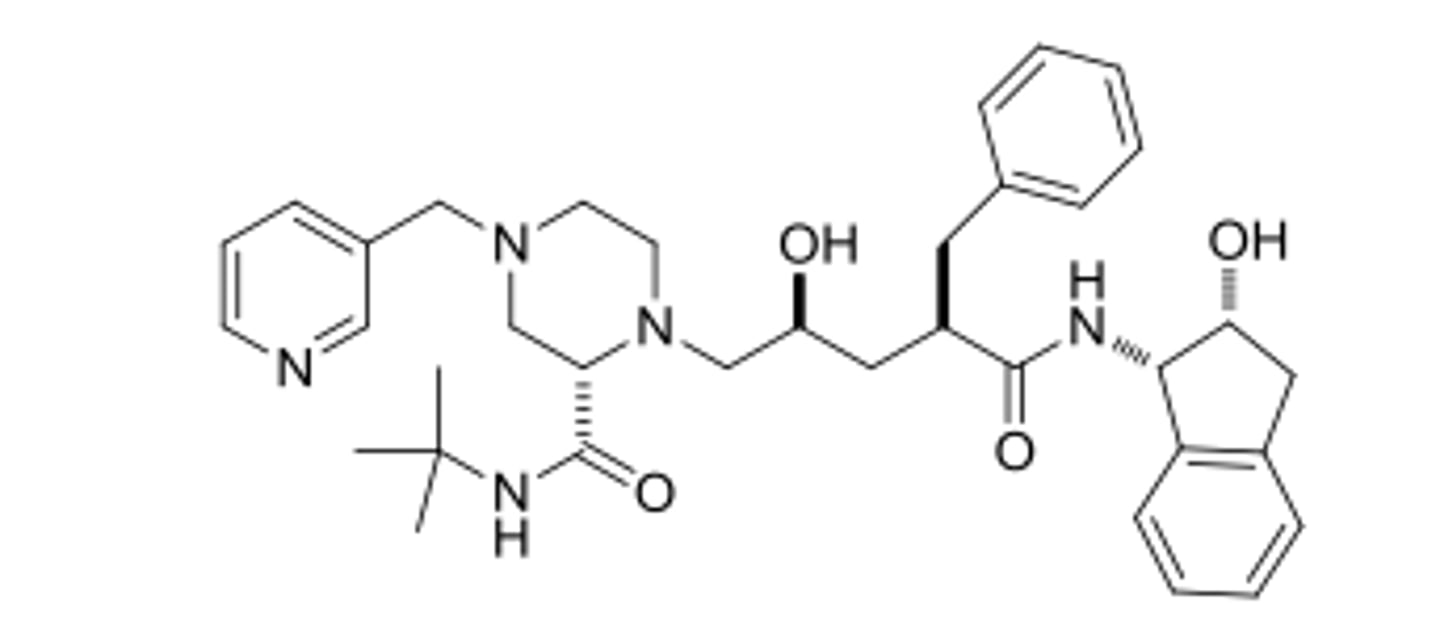
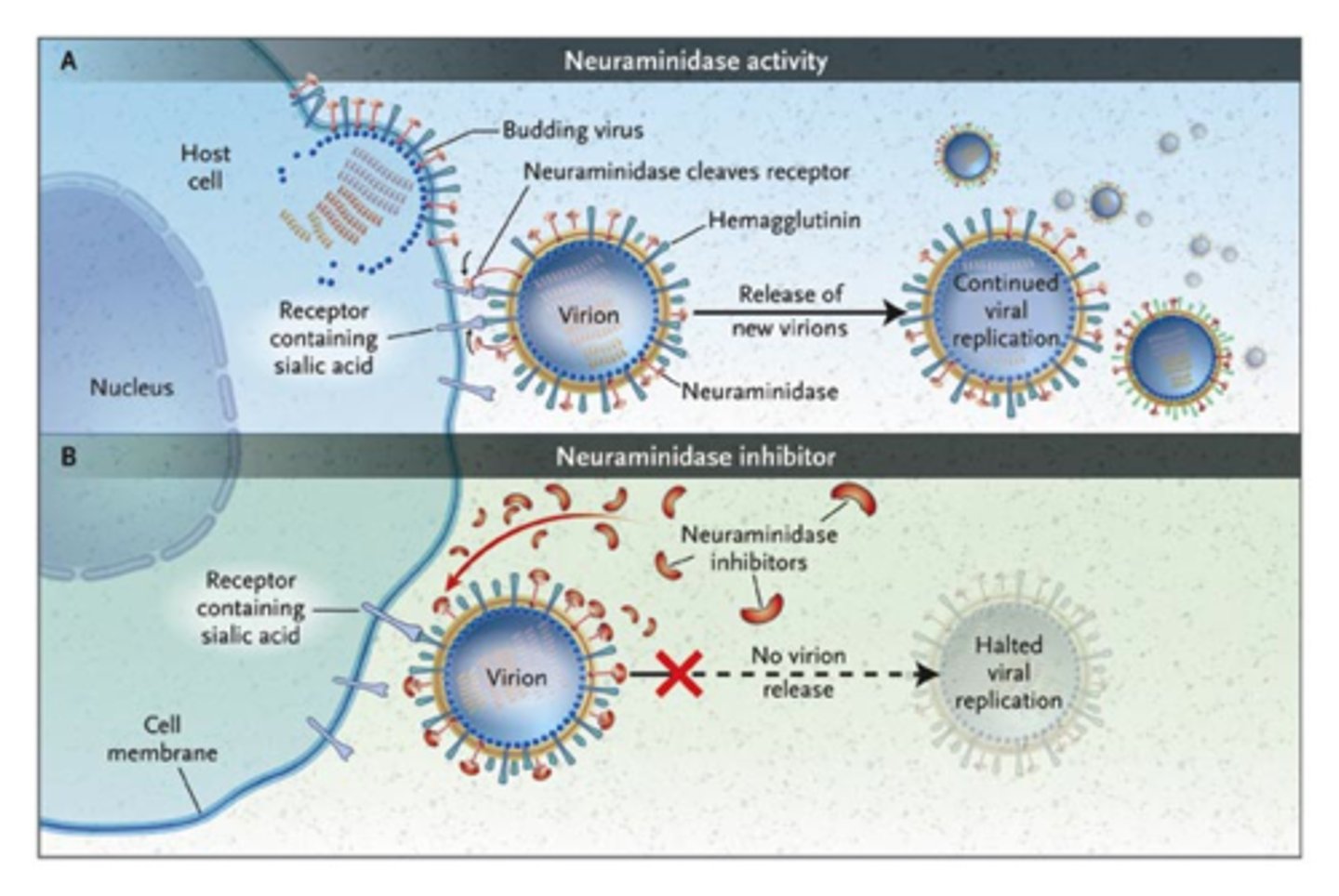
oseltamivir (tamiflu)
inhibits neuraminidase enzyme activity in influenza A by blocking release of virus after replication
antibiotic resistance contibution
not necessary, incorrect dosage, usage in animal feed
Bacillus anthracis
boil bacteria, endospore former, gram negative
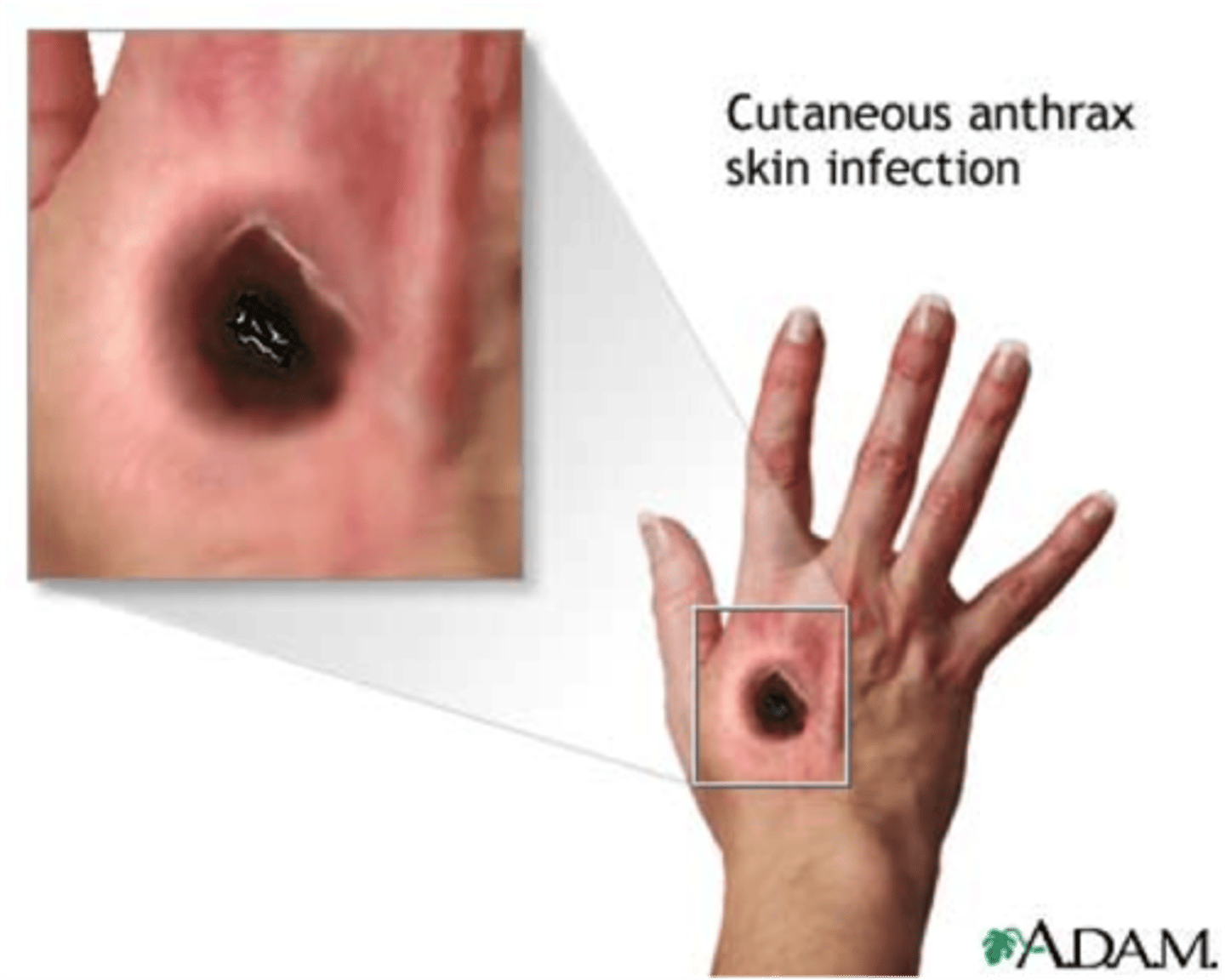
cutaneous anthrax
skin lesions from handling animal skins.
not typically deadly
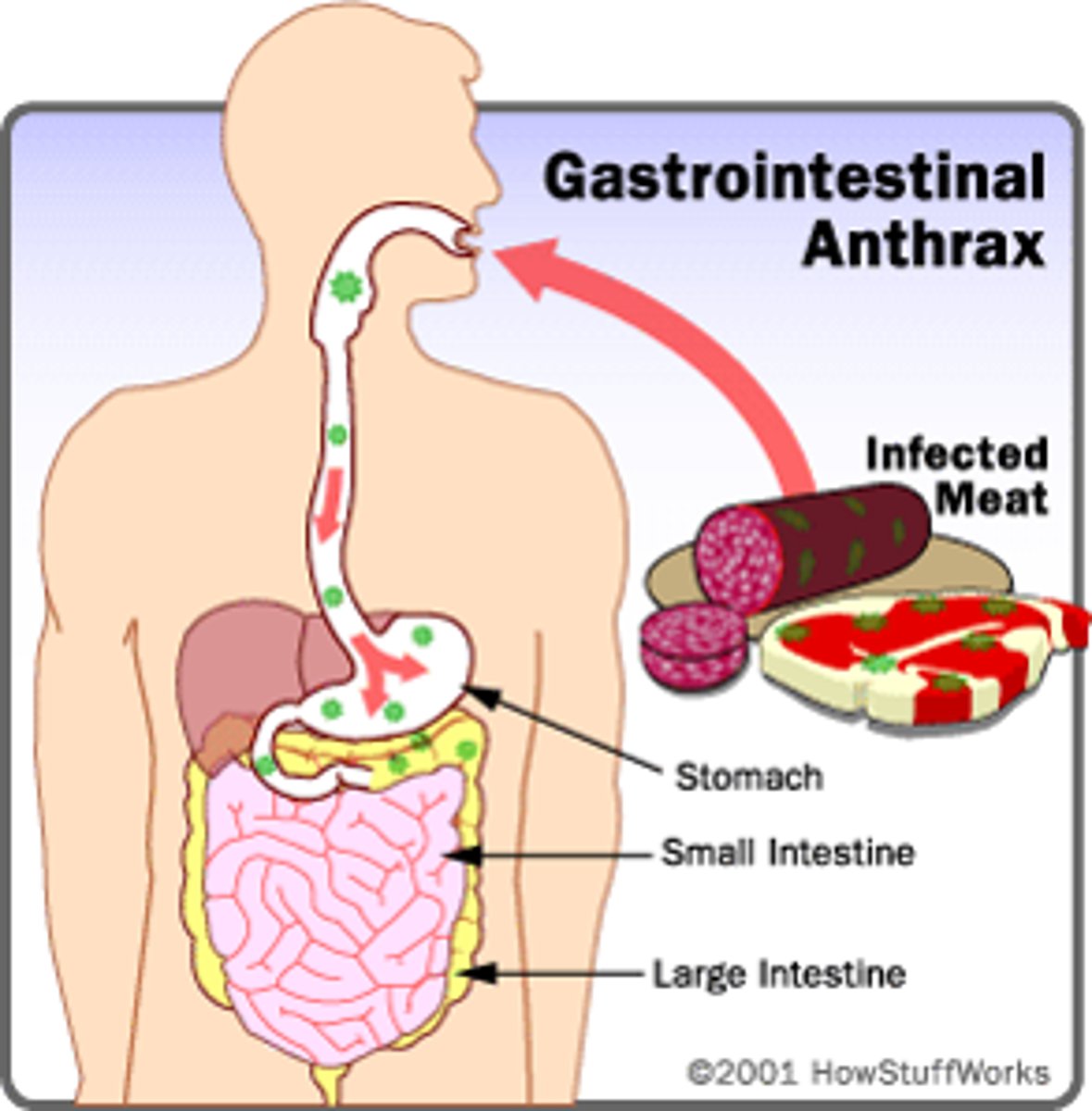
gastrointestinal anthrax
consumption of infected meat.
fatal, uncommon
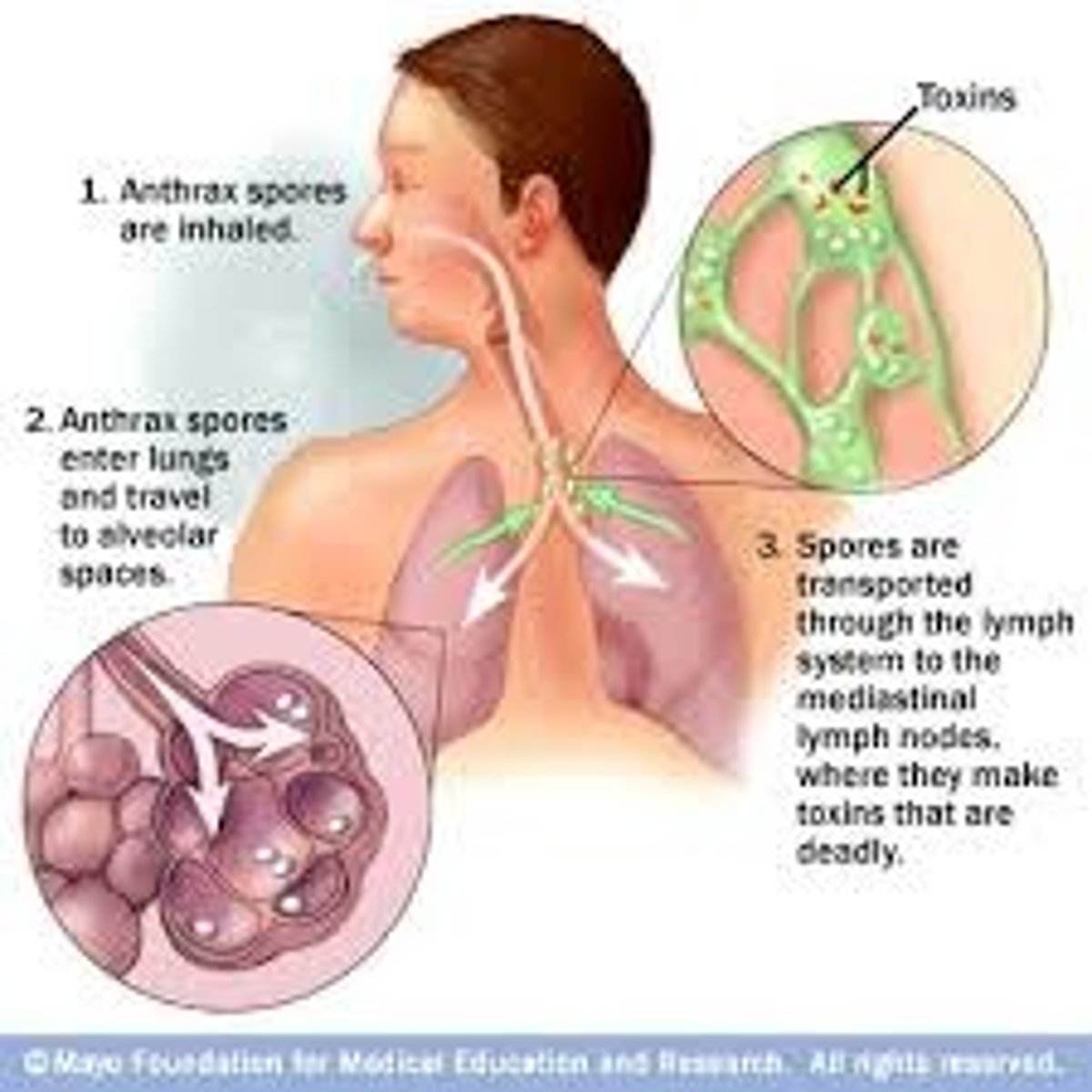
inhalation anthrax
breathing in spores.
fatal if not treated due to spores germinating in alveoli and producing cytoxins
advantages of anthrax
not communicable, antibiotics and vaccine available
disadvantages to anthrax
easily aerosolized, fatal if not treated, cost of clean up
cytotoxin in anthrax progression
first symptoms similar to flu, once cytotoxin is produced drastic decline leads to fatality and inability of treatment