MICROBIOLOGY UNIT 4 PATRICIA LONGORIA
1/104
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
105 Terms
catalase test
Test that determines whether or not bacteria has "catalase" enzyme.
Coagulase test
a test in which organisms are mixed with plasma on a slide. if the cells clump together, the culture is coagulase positive
skin defenses
keratinized layer, sloughing, low pH, high salt, antimicrobial peptides, sebum from sebaceous glands
keratin
hard protein material found in the epidermis, hair, and nails
sebaceous oil glands
scent glands associated with the hair follicle
integument
the skin together with the hair, nails, and sweat and oil glands
normal biota on healthy skin
streptococcus, staphylococcus
propionibacterium, corynebacterium, pseudomonas, lactobacillus, candida (yeast)
maculopapular rashes
Flat to slightly raised colored bumps on the skin
Rubeola-Measles
measles virus
respiratory droplet transmission
humans are the only living reservoir for this virus
symptoms: sore throat, dry cough, headache, conjunctivitis, lymphadenitis, fever, Kopliks spots
characteristic exanthem (widespread rash, begins on the head to the rest of the body)
defective, dormant measles virus can stay in a person's body and can move toward neurons and invade the brain; can remain years after measles has cleared
Rubeola-Measles virulence factors
syncytium formation, ability to suppress CMI
the virus implants the respiratory mucous and infects the tracheal and bronchial cells. it then travels to the lymphatic system leading to viremia
Rubella
caused by the rubella virus
moderately communicable through respiratory secretions and urine droplets in close living conditions.
has 2 clinical forms
postnatal rubella
caused by rubella virus
rash on the face, spreads to the body
aka: "3 day measles"
joint pain
congenital rubella
fetus is born already infected with rubella
strongly teratogenic: can cross placenta and infect the baby in utero
severe
miscarriage
sequelae: deafness, cardiac abnormalities, mental/ physical retardation
Fifth disease (erythema infectiosum)
human parvovirus B19, a strain of the dog virus "parvo"
mild "slapped-cheek" rash, low fever, fatigue, runny/ stuffy nose
spread through respiratory secretions
very contagious with no treatment, usually mild
the rash of this disease may reoccur for several weeks and may be brought on by any activity that increases body heat
Roseloa (sixth disease)
human herpesvirus 6 (HHV-6)
common in young children/ babies
high fever (105F) seizures
rash, last symptom, after 4th day; only about 30% even develop a rash
pustular rashes
rashes with lesions that contain fluid
smallpox
variola virus
droplet transmission or bedding/ clothing
2 forms: variola minor, variola major
last natural cause in 1977
class A bioterrorism agent: easily disseminated, high mortality rate, incite panic, require preparedness
rash is macular>papular>vesicular>pustular>crusting over
ability to dampen, avoid immune response
variola minor
a form of smallpox; not as severe, less rash, less illness
variola major
a form of smallpox; severe, highly virulent, shock, DIC, sepsis
2 weeks of high fever, malaise, back/ abdominal pain rash with "BB pellet-like" fluid in lesions
chickenpox/ shingles
human herpes virus 3 (HHV-3 aka varicella zoster virus, VZV)
fever, itchy rash vesicles with clear fluid which are contagious until they scab over and fall off
do not give aspirin or else Reye's Syndrome will occur
incubation 10-20 days, lasts 4-7 days
0.1% of chickenpox cases are followed by encephalopathy
transmission: humans are the only natural hosts for HHV-3, if you're exposed, you'' most likely get it; droplet contact, inhalation of aerosolized lesion fluid
ability to fuse cells and become latent in ganglia and re-emerge as shingles (aka: herpes zoster)
MRSA
methicillin-resistant staphylococcus aureus; breaks in the skin by injury/ abrasion
GPC in clusters
catalase (+), coagulase (+)
direct or indirect contact transmission
raised, red, tender, pus, warm to touch, fever
norma flora AND pathogen
common on gym equipment
common norma flora on healthcare workers
impetigo
caused by S. aureus (exfoliative toxin) or S. pyogenes (streptokinase)
superficial bacterial inflammatory skin disease characterized by vesicles, pustules, and crusted-over lesions; honey colored crust, flaky/ peely skin
highly contagious by direct contact and fomites
peak incidence: summer and fall
prevention (good hygiene)
cellulitis
Inflammation of cellular or connective tissue
caused by S. aureus or S. pyogenes (or any bacteria)
fast-spreading infection in the dermis and subcutaneous tissues
common in the immunocompromised
if caused by S. aureus = methicillin resistant (MRSA)
Staphylococcal scalded skin syndrome (SSSS)
S. aureus
dermolytic infection
newborns/ babies
bullous lesions: often appear first around the umbilical cord (in neonates) or in the diaper or axilla area
transmission: when caregivers carry the bacterium from one baby to another
30% of adults are asymptomatic carriers
cutaneous anthrax
B. anthracis GPR endospores, enter skin through cuts/ abrasions
forms eschar (painless and black)
least dangerou anthrax infections
20% fatality rate
class A bioterrorism agent
transmission: direct contact with endospores
fungal infections
transmission: fomites, soil, human contact, animals
mainly caused by 1/3 dermatophytes:
trichophyton, microsporum, epidermophyton
superficial mycoses
fungal infection; malassezia species
cosmetic
dandruff/ skin discoloration
conjunctivitis
pink eye; clear watery exudate "glued shut"
neonates N. gonorrhea or C. trachnomatis
Staph. epidermis, Strep. pyogenes, Strep. pneumoniae, Haemophilus. influenza
prevention: good hygiene
keratitis
more serious eye condition than conjunctivitis; damage to deeper eye tissues, post trauma
80% cases are bacterial
viral (herpes simplex virus HSV1 or 2), protozoan
GI tract defenses
saliva, mucus in the intestinal tract (IgA)
peristalsis
stomach acid
GALT
tonsils
Peyer's patches
Appendix
normal biota of the GI tract
Acintomyces, Lactobacillus, Neisseria, Prevotella, Streptococcus, Treponema, Veillonella, Candida Albicans
oral cavity defenses
Saliva, sIgA, lyzozyme, tonsils, adenoids
accessory organs
salivary glands, gallbladder, liver, pancreas
free of a natural microbiome but can be exposed to microbes when normal barriers in the gut are disrupted by a condition called dysbiosis
dysbiosis
an unhealthy mix of the gut microbiome
normal flora of the gut
Clostridium species, Bacteroides species, Enterobacteriaceae, Escherichia, Lactobacillus
acute diarrhea
3 or more loose stools in a 24 hour period;
treatment: electrolyte therapy
prevention: hand hygiene, follow food safety guidelines, avoid untreated water, cook chicken to int. temp. of 165, follow food safety guidelines
common culprits: salmonella, norovirus, campylobacter, E. coli STEC strains, staphylococcus aureus, clostridium perfringens
salmonella typhi
causes typhoid fever
not common in developed countries
contracted from human feces F/O
resistant to bile
high ID, need 100,000 bacterial cells to get sick
10% human consumption rate
salmonella thypimurium and enteritidis
zoonotic
normal biota of reptiles, chickens, cattle, rodents
resistent to bile
salmonellosis
can be relatively severe with an elevated body temp and septicemia as more prominent features than GI tract disturbance but can also be fairly mild with gastroenteritis, vomiting, diarrhea, and mucosal irritation. blood can appear in the stool.
symptoms spontaneously subside after 2-5 days.
death infrequent unless debilitated
needs electrolyte replacement and ciprofloxacin in severe cases
shigella
GNR, NLF
F/O for infected person, direct contact
low ID
dysentery, fever, intense abdominal pain, vomiting
resembles E. coli
virulence factors:
has enterotoxin that damages the GI tracts (mucosa and villi)
shiga toxin: responsible for more damage to the intestines, systemic effects, neurological damage
invades large intestine villi
enters intestinal mucosa by peyer's patches
can establish chronic carrier that can last several months
transmission: spread epidemically in day care centers, prisons, mental institutions, nursing homes, and military camps
prevention: good hygiene and avoiding contact with infected persons
Shiga toxin-producing E. coli (STEC)
aka: e. coli 0157:H7
acquired shiga toxin from bacteriophage that previously infected S. dystenteriae
bloody diarrhea, fever
transmission: contaminated food. is normal biota in cattle
severe complication: hemolytic uremic syndrome (HUS), kidney failure, blindness, seizure, stroke
hemolytic uremic syndrome (HUS)
Serious condition characterized by red blood cell breakdown and kidney failure; severe hemolytic anemia that can cause kidney damage and failure, neurological symptoms such as blindness, seizure, and stroke, and long-term debilitation
other e. coli that cause diarrhea
enterotoxigenic E. coli
enteroinvasive E. coli
enteropathogenic E. coli
enteroaggresive E. coli
difusely adherent E. coli
campylobacter jejuni
seagull shaped GN bacteria
lives in intestines of poultry, cattle, pigs, sheep, dogs, cats
ingestion of undercooked chicken, contaminated water, feces of pets
watery stool, fever, vomiting, headache, abdominal pain
complication (not permanent): Guillain-Barre syndrime (GBS)
Guillain-Barre Syndrome (GBS)
temporary paralysis caused by an autoimmune attack on peripheral myelin, causing weakness and usually ascending paralysis of the limbs, face and diaphragm
leading cause of acute paralysis in the US
40% of GBS cases are preceded by infection with campylobacter
clostridium difficile
GP endospore-forming rode round in the normal biota of the intestine
antibiotic associated colitis (pseudomembranous colitis)
healthcare associated infection
transmitted from patient to patient
enterotoxin A and B
abdominal pain, leukocytosis, watery diarrhea, vomiting, rapid heart rate, perforation of cecum-death
66% healthcare-associated, 24% did not occur until patient had gone home
vibrio cholerae (cholera)
darting GNR resemble a comma
water/ saline rich areas (Seaports) spread through infected water and food
spread from person to person (F/O) in underdeveloped countries
"rice water" stool
dehydration, blood volume loss
muscle cramps, severe thirst, sunken eyes
electrolyte loss-tachycardia
70% morality rate in untreated children
enterotoxin: cholera toxin: causes intestinal cells to shed large amounts of electrolytes into intestine; 1 liter of water per hour - 50% of patient body weight (severe)
virulence factors:
100,000,000 ID
adhere to junction of duodenum and jejenum, penetrate mucosa barrier w flagella, adhere to microvilli, epithelial cells and multiply
prevention:
proper sewage treatment and water purification
vaccines for travelers (not in US)
rotavirus
primary viral cause of death from diarrhea
F/O route contaminated by food/ water/ fomites
mild and self-limiting diarrhea
watery diarrhea, fever, vomiting, dehydration shock = intestinal mucosa damage
babies without maternal antibodies most affected
50% of all diarrhea cases
norovirus
second more common cause of hospitalization from food-borne illnesses
F/O route via contaminated food/ water
profuse watery diarrhea 3-5 days
mild self-limiting
cruise ship industry affected
3-5 days watery diarrhea, vomiting in early phases, mild fever, make sure to rehydrate
Staphylococcus aureus
food poisoning
on skin of food handler-left unrefrigerated
heat sable can grown in salty/ sugary foods
cramping, nausea, vomiting, diarrhea 24hrs
violent symptoms, short incubation period
bacillus cereus
food poisoning
exotoxin: rice/ pasta = emesis
exotoxin: meats/ veggies = diarrhea
symptoms last 24hrs
common resident on veggies and anything in contact with soil
clostridium perfringens
food poisoning
intestinal protozoan of apicomplexan type that infects a variety of mammals, birds, and reptiles
undercooked beans and meat
avoid by reheating food (heat labile exotoxin)
abdominal pain, nausea, diarrhea 24hrs
urinary tract
has the job of removing substances from the blood, regulating certain body processes, and forming urine and transporting it out of the body
remove metabolic waste from the blood acting as a sophisticated filtration system for the blood
kidneys, ureters, bladder, and the urethra
defense symptoms: flushing action of urine, urine sheds epithelial cells from the lining of the urinary tract
genital system
has reproduction as its major function
aka: the reproduction system
normal biota of the genitourinary tract
lower urethra: has a well-established microbiota
upper urinary tract: has a few types of biota but lower abundance
genirourinary tract defenses
voiding, lyzozyme and lactoferrin, secretory IgA, estrogen
male genitourinary biota
psuedomonas
staphylococcus
anaerobic GN bacteria = uncircumsized
female genitourinary bacteria
lactobacillus, candida albicans (low numbers), gardnerella vaginalis (low numbers)
leptospirosis
a spirochete-caused disease transmitted by contact of broken skin or mucous membranes with contaminated animal urine
vehicle: contaminated soil or water
prevention: avoiding contaminated vehicles
treatment: doxycycline, penicillin G, or ceftriaxone
urinary tract infection (UTI)
result from invasion of the urinary system by bacteria or other microorganisms
cystitis, pyelonephritis, urethritis
symptoms: dysuria, frequent urges to urinate, cloudy urine, back pain, fever
common agents:
95% from normal biota from the GI tract
80% E. coli
Klebsiella pneumoniae
Proteus mirabilis
community-acquired UTIs
transmitted not from person to person, but organ to organ (ex: GI tract to urinary tract) much more common in women than men bc of the short perinatal disease
cystitis
bladder infections
pyelonephritis
kidney infection
urethritis
if the infection is limited to the urethra
vaginitis
inflammation if the vagina: candida albicans overgrowth
broad spectrum antibodies
diabetes
pregnancy
HIV
white curdlike discharge
vaginosis
bacterial in origin with less inflammation: Garnerella vaginalis overgrowth (fish odor) semen
saliva
discharge with fishy smell
group B streptococcus-neonatal disease
no issues for non-pregnant females
associated with preterm delivery
small % blood stream infection, meningitis, or pneumonia
transmission: vertical (passing of an infection or disease from a mother to her child during pregnancy, childbirth, or breastfeeding. This can occur through the placenta, vaginal fluids, or breast milk)
treatment: treat mother with penicillin/ ampicillin
watch for clindamycin-resistant strains as they are a concerning treat category on CDC antibiotic resistant report
prostatitis
inflammation of the prostate gland-caused by GI bacteria
can be acute or chronic
virtually always caused by a bacterial infection
symptoms:
painful urination, frequent urge to urinate, painful ejaculation, difficulty emptying bladder
treatment:
ciprofloaxcin or levofloxacin (antibiotics, muscle relaxers, alpha blockers)
50% men experience in lifetime
STIs that cause discharge
gonorrhea, chlamydia
gonorrhea
caused by Neisseria gonorrhoeae
GN diplococci, kidney/ coffee bean shaped bacteria
pyogenic (pus-forming)
catalase (+)
oxidase (+)
symptoms:
yellow discharge, blood discharge, painful urination, PID, infertility
10% males asymptomatic
50% females asymptomatic
virulence factors:
fimbriae anchor to mucosal epithelial cells
fimbriae can rearrange
IgA protease: can cleavage IgA molecules stationed for protection on mucosal suurfaces
salpingitis
transmission: direct contact (STI), vertical
effects on fetus: eye infections, blindness
salpingitis
inflammation of the fallopian tubes or it may include other parts of the upper reproductive tract (pelvic inflammatory disease (PID)
Chlamydia trachomatis
most common reportable infectious disease in the united states
virulence factors:
grows intracellularly, triggers intense cytokines, greater risk of PID in females
symptoms:
discharge, painful urination
75% infected are asymptomatic
transmission: direction contact (STI), vertical
effects on fetus: eye infections, pneumonia
STIs that cause ulcers
syphilus, congenital syphilus, chancroid, genital herpes
Syphilis
Treponema pallidum
GN spirochete (mainly viewed with dark-field microscopy
virulence:
lipoproteins
hooked up to epithelial cells
penetrates nearby capillaries to spread
primary: painless, hard chancre; 3-6 weeks
secondary: rash, hairloss, bone/ joint pain; 3-6 months
tertiary (non-transmissible): gummas and Argyll-Robertson pupil; 20 years or longer
congenital syphilis
" snuffles" excess profuse nasal discharge
notched barrel teeth in late ______
"hutchinson's teeth"
chancroid
Haemophilus ducryei
painful soft chancre
more common in uncircumcised males
direct contact
rule out other ulcer diseases
avoid contact
genital herpes
HSV 1 and HSV2
80% US pop positive for HSV 1
40% US pop positive for HSV 2
painful tender vesicle with clear fluid
mouth, genitals, breasts, buttocks, thighs, groin
has a strong tendency to become latent
STIs that cause warts
HPV
Human Papillomavirus (HPV)
warts on genitalia, buttocks, groin, thigh, pelvic area
oncovirus-cervial
aslo associated with throat factor
CDC-"nearly all active adults will get HPV at sometime in their lives"
HPV vaccine provides 97% protection against cervical caner and warts
condyloma acuminata: extensivley branching, cauli-flower like masses
has oncogenes as virulence factor
condoms
how to prevent STIs
sexually transmitted, vector borne, fecal-oral route, water/ soil
how are parasites spread?
diagnoses for parasites
O&P test
CBC Blood Smears-high eosinophil count
O&P test
Test for ova and parasites in the stool
CBC Blood Smear
test for high eosinophil count
protozoa
large group of creatures, single-celled, have startling properties when it comes to movement, feeding, and behavior
form and function:
single cells, contain all major eukaryotic organelles
pseudopods: false feet; how they move through fluids, flagella, or cilia
lack cell wall, so theyre flexible
trophozoites
what protozoa are called when theyre in the motile feeding stage
requires ample food and moisture. to remain active
cyst
dormant resting stage when environment become unfavorable for growth and feeding; rounds into sphere, and ectoplasm secretes a thick cuticle around the cell membrane; resistant ti heat, drying, and chemicals and can survive adverse periods, breaks when. theres moisture and nutrients
protozoa life cycle
single-celled organisms
free-living
parasitic
prophozomites
cyst
5 protozoal parasitic infections
trichomonas vaginalis
leishmania species
giardia lamblia
entamoeba histolytica
plasmodium
trichomonas vaginalis
does not survive long outside host body
trichomoniasis (STI):
most common non-viral sexually transmitted disease males
mostly carriers females
mostly symptomatic
causes itchy burning genitals, green white frothy discharge
no cyst form
chronic infection may lead to infertility
Leishmania species
bite with sandfly infected with Leishmania parasite causes leishmaniasis
cutaneous (pictured) = L. tropica
Mucocutaneous = L. brasiliensis
System fatality 100% untreated
Giardia lamblia
Giardiasis
intestines of beavers, cattle, cayote, cats, human carriers (beaver fever)
contaminated food/ water, fomites
greasy foul-smelling diarrhea, flatulence, abd. pain
entamoeba histolytica
amebiasis
food/ water contaminated with feces
1/10th pop asymptomatic carriers loose stool, cramping, stomach pain
hemorrhage, perforation, appendicitis, extra-intestinal infection (amoebic hapatitis)
Plasmodium
transmitted by female anopheles mosquitos
most infections close to the equator
symptoms: malaise, fatigue, body aches, chills, fever, sweating in 48-to-72 hour intervals
over 200 species:
P. malariae
P. vivax
P. knowlesi
P. ovale
P. falciparum (most deadly)
complications from plasmodium infections:
hemolytic anemia
Enlargement/ rupture of organs (spleen, liver, kidneys)
Cerebral Malaria
diagnosis and treatment:
CBC Blood smear-thin and thick smears
Medication quinine, chloroquine, Artemisinin
helminths
Nematodes (roundworms)
Cestodes (tapeworms)
Trematodes (flukes)
helminths life cycle
Sexual reproduction
Hermaphrodite (tapeworms, flukes)
Fertilized egg, larvae, adult worm
intermediate host: host in which larval development occurs
definitive host: final host where adulthood and mating occurs
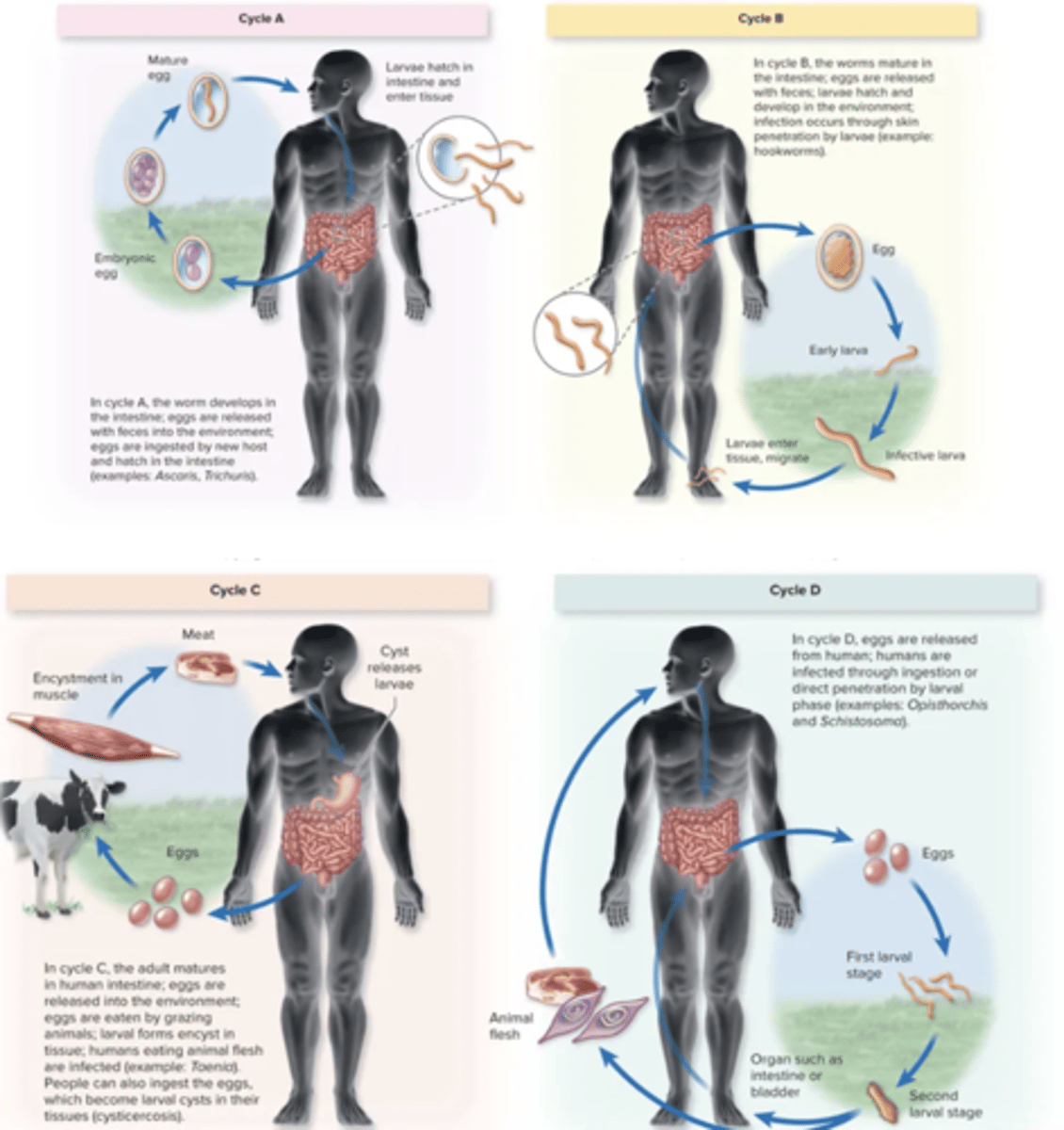
parasitic nematodes
enterobius vermicularis, trichuris trichuria
Enterobius vermicularis
"pin worms"
infects large intestine. female enterobius vermicularis mature in 1 month and mates deposits eggs into anus
causes anal itchiness, restlessness, loss of appetite, weight loss
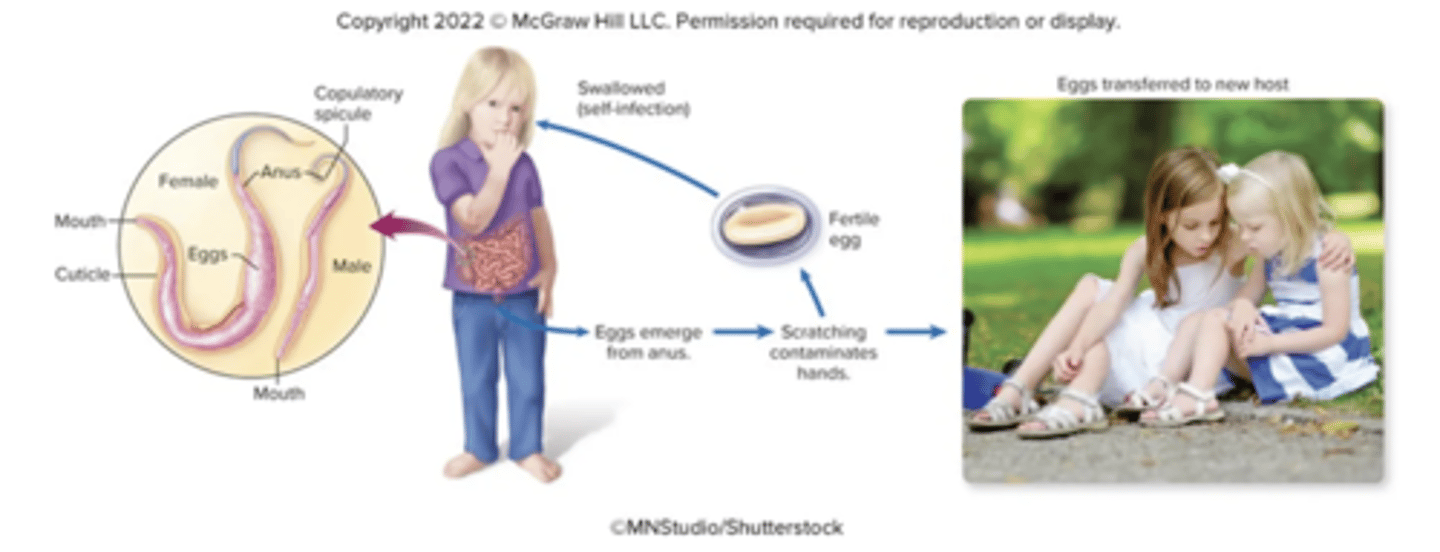
trichuris trichuria
"whip worm"
contaminated first or feces with eggs
hemorrhage of bowls, dysentery, loss of muscle tone, rectal prolapse
parasitic cestodes
Diphyllobothrium latum, Taenia solium