Bio 222 Week 5: Transporting Materials in Animals - Plant Energy + Nutrients
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
Although in a closed circulatory system blood never leaves the vessels, fluids containing material carried by the blood exit from a(n) capillary (vessel type). This happens at the artery (vessel type) end of that vessel and fluids enter the blood from interstitial fluid at the opposite end. When fluid is exiting from the blood differences in pressure potential between the blood and interstitial fluid is greater than differences in osmotic potential between blood and interstitial fluid. Although blood pressure decreases within these vessels, the difference in osmotic potential doesn't change; and the osmotic potential of the blood is always lower (more negative).
The purpose of our circulatory system is transport of goodies and waste. But these distributions, the passage of material to and from the blood, take place only through vessels we call capillaries . These vessels have the smallest diameter of any vessel type. This is advantageous because it improves the rate of gas exchange between the blood and intersitital fluid, which is driven by diffusion . The sum of the area of these vessels is the largest of any vessel type. The sum area of these vessels ensures that the velocity of blood travel through these vessels is (high, low,unchanging) low when compared to travel through other vessels.
True or False:
An increase in the average diameter of arterioles would decrease blood pressure
True
True or False:
An increase in blood viscosity would decrease blood pressure
False
Under what circumstances would you expect to find AOX1 activity?
In the evening
Why do female cycads make their cones hot later than do male cycads?
to attract only pollen bearing beetles
Osmotic potential is always negative, but the difference in osmotic potential between the blood and surrounding interstitial fluid is positive. Which osmotic potential is less than (more negative than) the other?
The osmotic potential of the blood is lower than that of the IF
The TRPA1 channel found in snakes and weevils opens in response to ...
heat
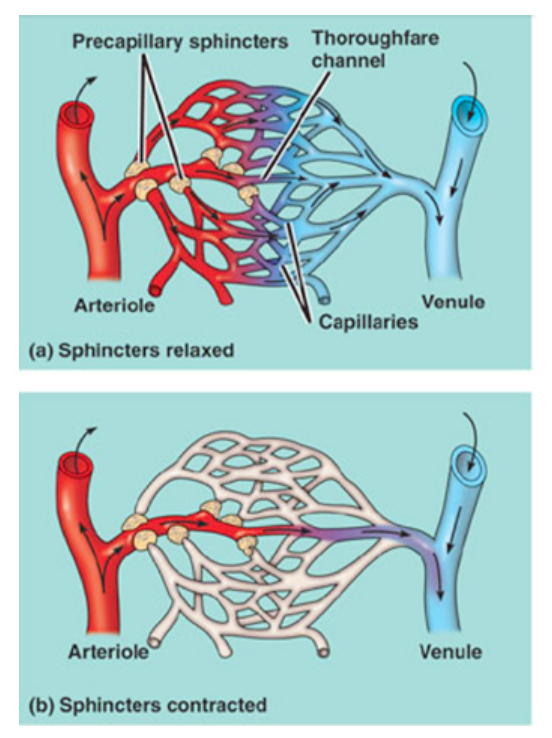
Blood has the same flow rate throughout all the vessels. However, the amount of blood delivered to any location (i.e. the distribution) can change with the demand of the tissues around the delivery sites (w/vessel size).
If you the reduce number of blood target sites, you can increase flow to the remaining sites more easily. An example of this is reducing blood flow to the digestive system and skin when you get an adrenaline rush. However, local signals overwhelm the global signal, so during exercise our flow rate increases and our vessel resistance decreases because the local signals are extensive.
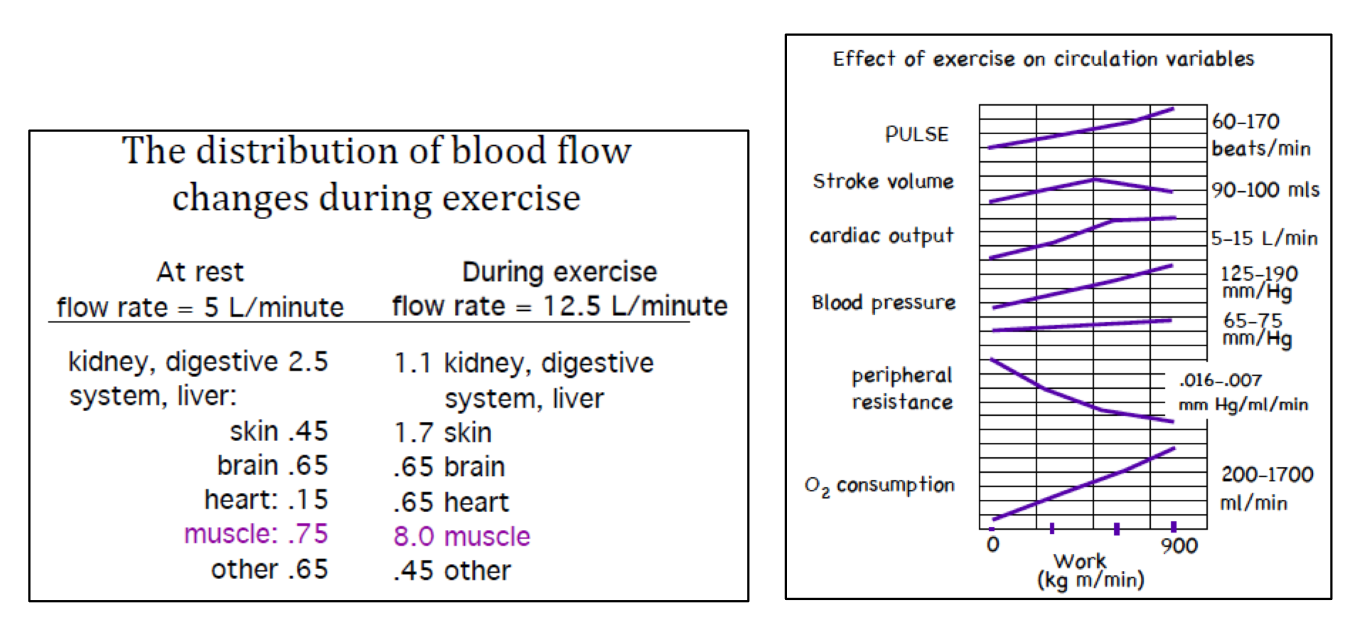
Graphs/data regarding how the distribution of blood flow changes during exercise.
(Note: It is possible to change flow rate by changing heart output or resistance. Complicating the big picture is that flow does not need to increase across the entire body for every given action. Flow may be increased in the muscles, while being decreased in the digestive system)
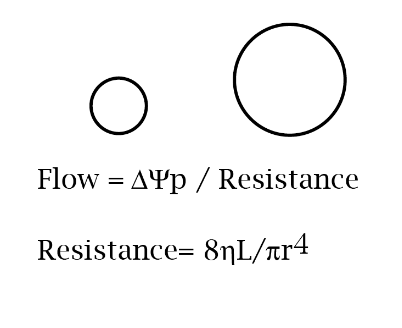
Flow = ∆Ψp / Resistance
Resistance= 8hL/πr4
8hL/π can be considered the same as viscosity.
Therefore, the most simplified equation would be: Resistance = 1/vessel radius4
Knowing this, if somehow the pressure drop along a vessel were held constant while the radius of the vessel doubled, by how much would the rate of flow change?
The rate of flow would increase by 16x because 24 = 16
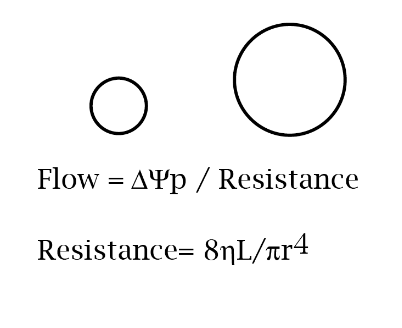
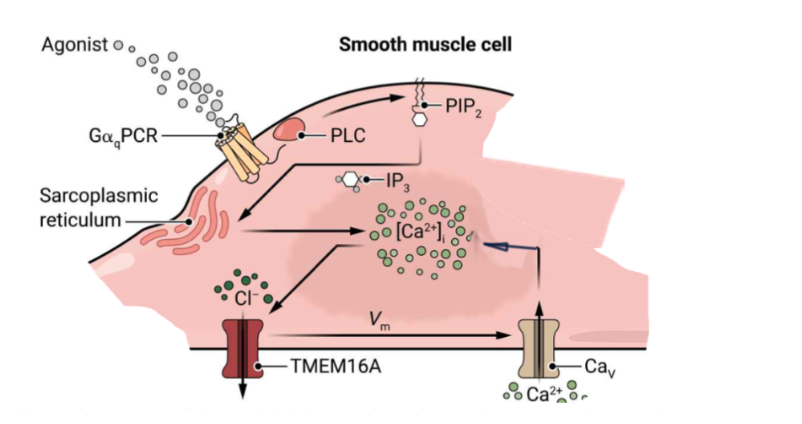
WILL BE ON EXAM!!!
Smooth muscle cells respond to an agonist to Noradrenaline by release of Ca++ from organelles into the cytoplasm. This causes a depolarization, allowing the muscle to contract (vasoconstriction). In this smooth muscle cell type associated with some arteries, depolarization and calcium entry create a positive feedback loop (AKA calcium entering opens TMEM16A chloride channels, so chloride leaves and depolarizes the membrane causing calcium to enter).
Essentially:
smooth muscle cell depolarization → contraction → reduced lumen cross sectional area
WILL BE ON EXAM!!!
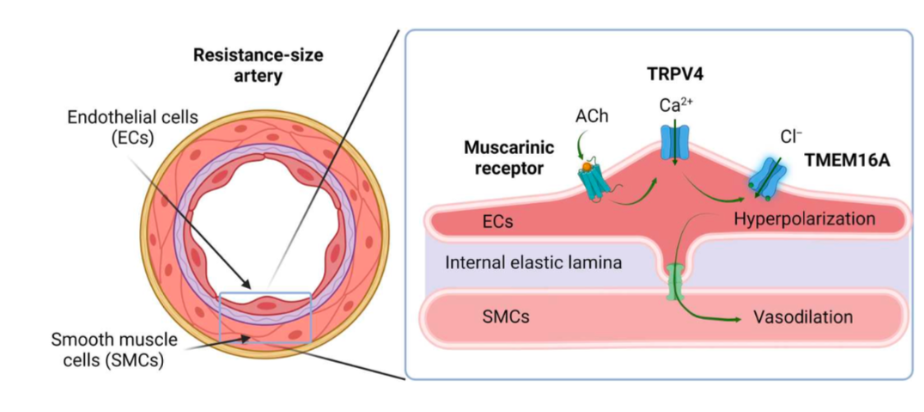
Vasodilation is accomplished when arteriole endothelial cells respond to signals (Ach in this diagram) through a receptor initiated cascade that includes the opening of Ca++ and Cl- channels, which generate the hyperpolarization of these cells. This hyperpolarization is transmitted to smooth muscle cells via gap junctions that can transmit charge directly between cells, and that this leads to relaxation of those cells and enlargement of the vessel lumen.
Essentially:
smooth muscle cell hyperpolarization → relaxation → increased lumen cross sectional area
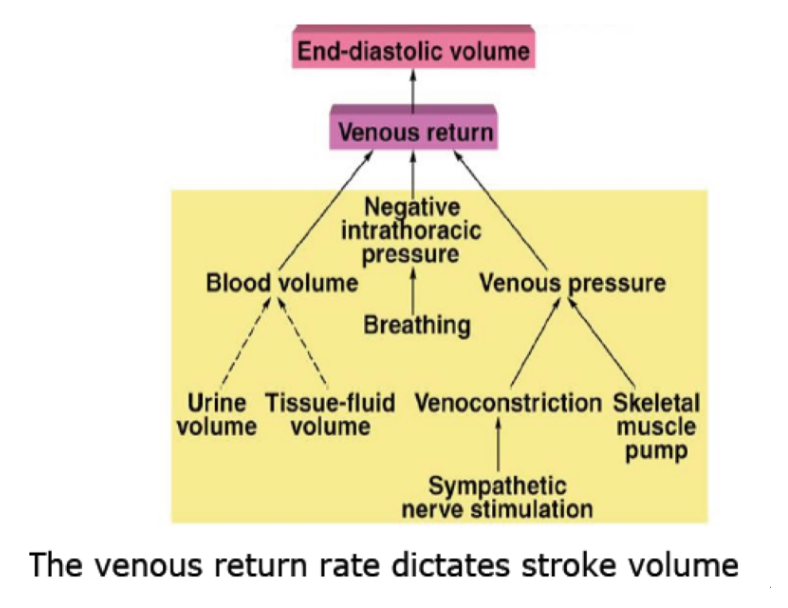
Changing heart output:
Stroke volume and rate increase together. More blood gets returned to the heart and the heart works more efficiently when work increases within reasonable loads.
(^Venous return rate dictates stroke volume)
Pulse rate is the primary mechanism by which nervous system regulates BP.
Flow rate is limited by the ability of blood to return and fully re-fill the ventricle. Because this becomes less efficient at higher pulse rates, there is a maximal heart rate at above which output actually decreases.
Pulse x stroke volume = cardiac output (flow rate)
In the heart, electrical activity spreads through the atrium from the sinoatrial (SA) node. Once it arrives at the atrioventricular (AV) node, fibers there carry the electrical signal to the opposite end of the heart so that the direction of contraction moves blood to the exits of the ventricles. The flow of electrical events generates a domino effect of cellular contractions that generates the directional contractions that move blood efficiently towards the exits.
Blood enters atria, then is pumped into ventricles which then pump blood to the body and lungs.
SA NODE = PACEMAKER!
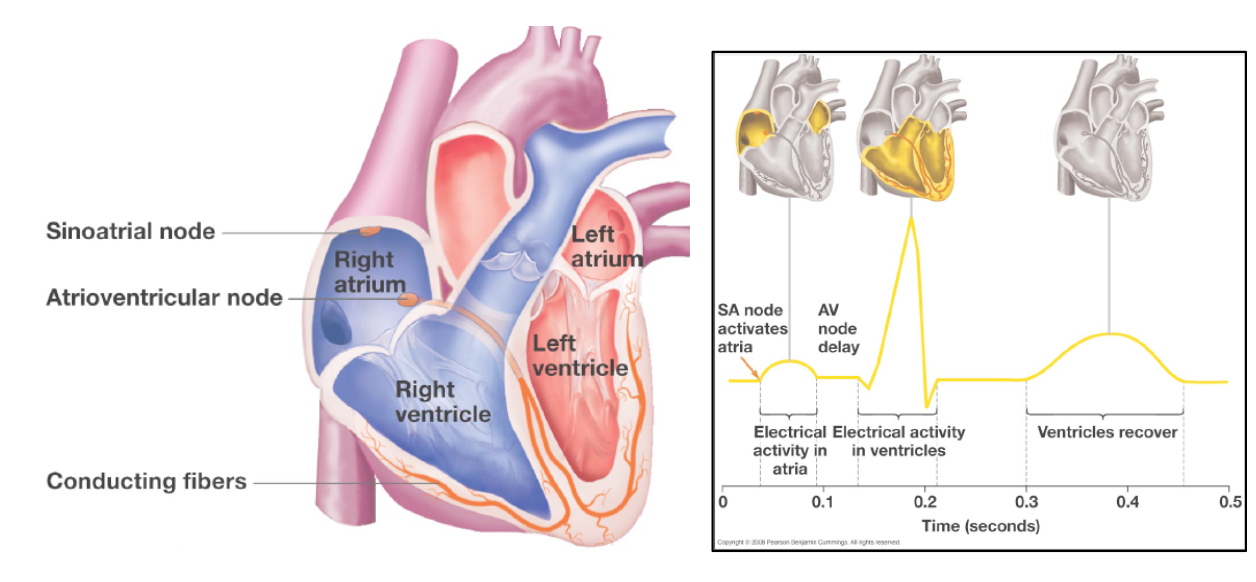
Pacemaker Cells…
Control electrical activity of the heart.
Are auto-rhythmic. They set the heart beat rate (pulse) due to the the fact that they have the fastest endogenous rate for membrane depolarization (called action potentials), which trigger contractions.
Action potentials = cell contractions.
Are so tightly connected that an action potential in a cell of this type (the sinoatrial node (SAN)) leads to the depolarization of the cells neighboring it, setting off a cascade that leads the entire heart to contract.
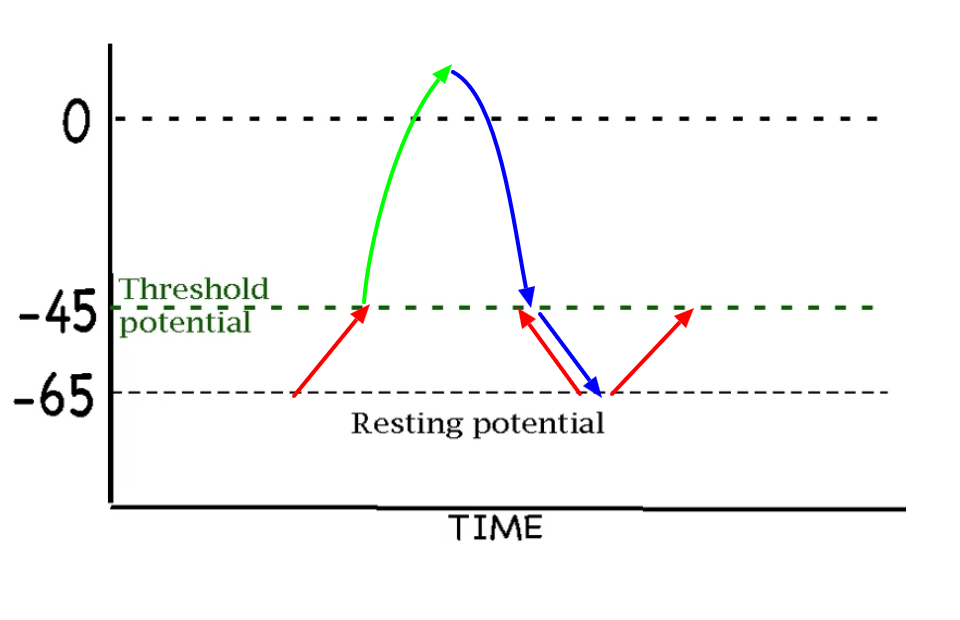
What is going on in a pacemaker cell during each of these colors?
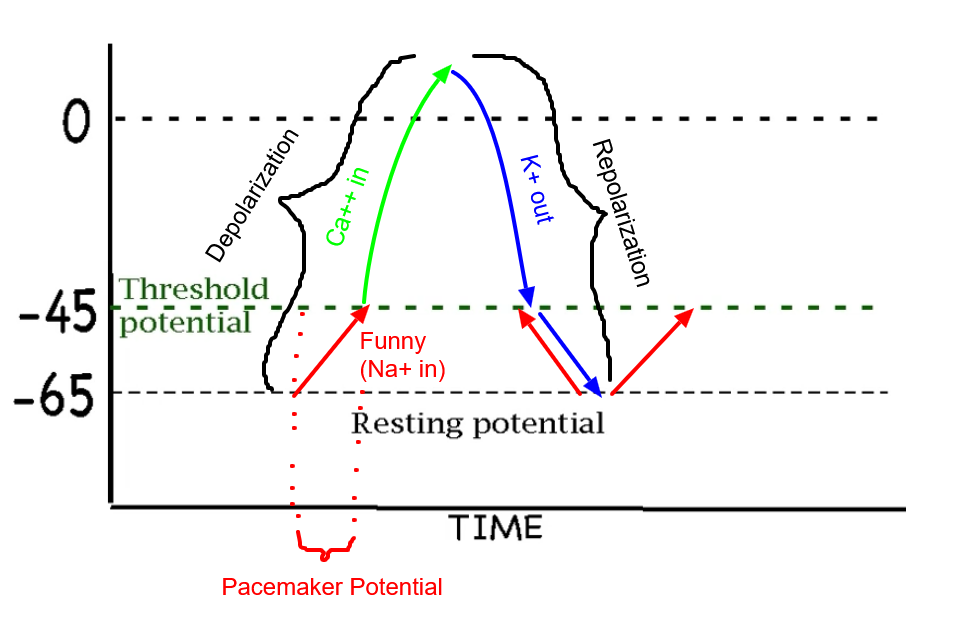
What drives Na+ through the membrane during the pacemaker potential?
Charge and concentration.
This is because Na+ is going into the cell through funny channels, meaning that since this is in a typical animal cell the membrane potential would be negative and thus it would want to go in towards that charge.
Knowing this (“Banana in the ocean”) we can also say that there would be more sodium concentrated outside, meaning that it would want to go in with concentration as well.
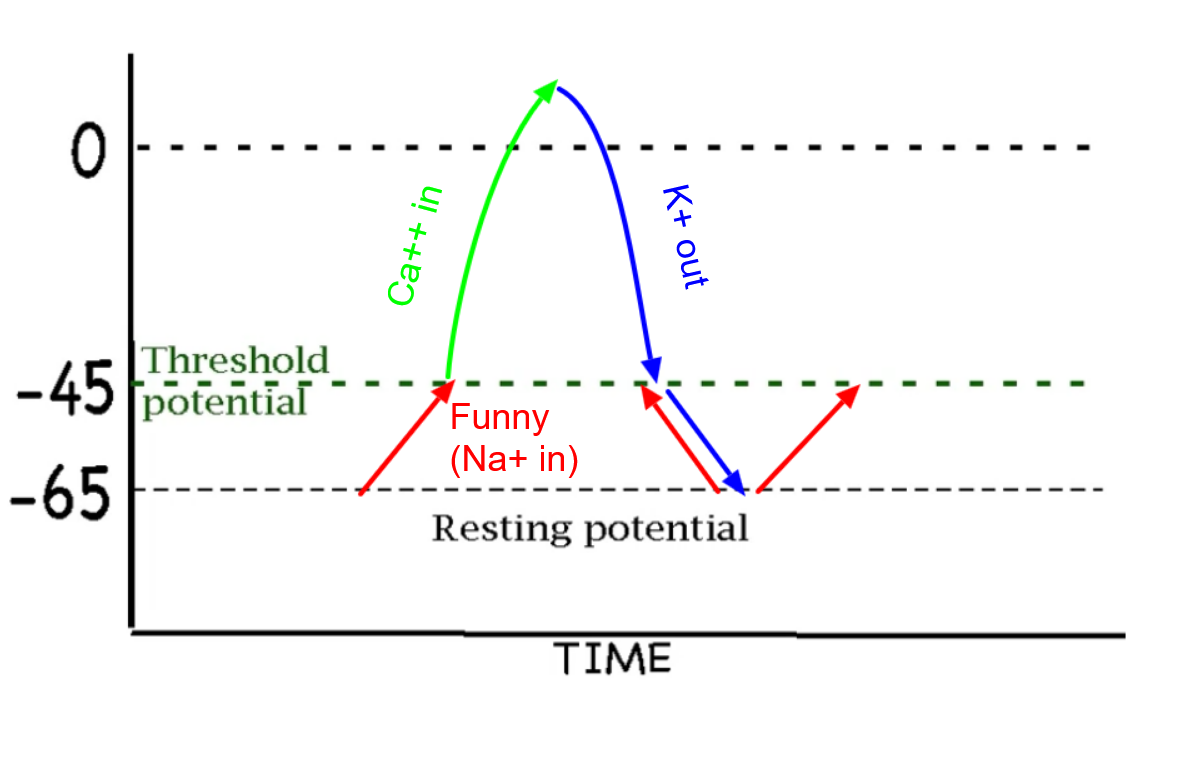
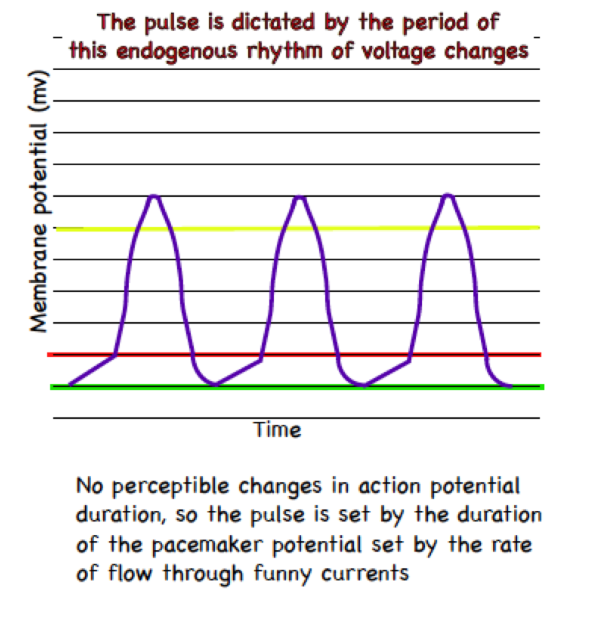
To calculate the pulse you would need values…
On just the x axis.
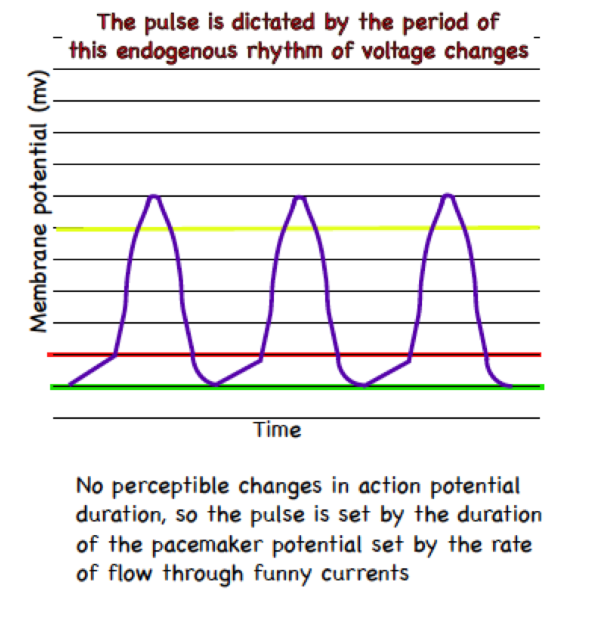
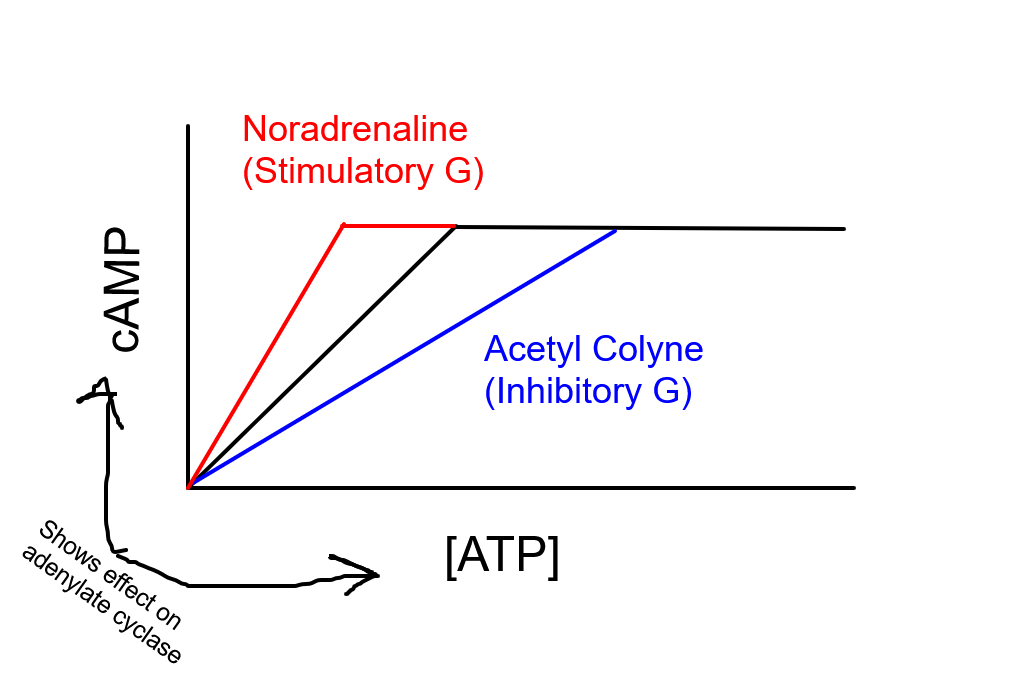
Regulation of pacemaker cells (controlling cardiac output)
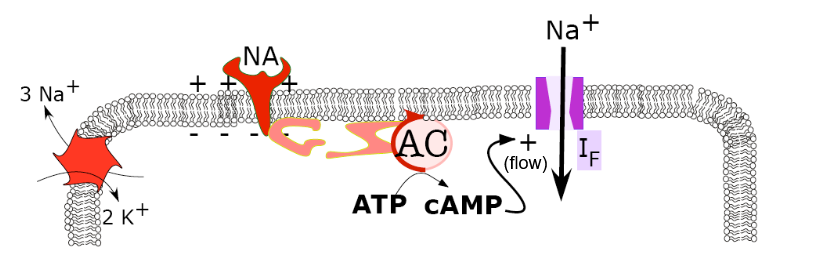
Pacemaker cells when noradrenaline (NA) is involved:
NA binds to the appropriate receptor, speeding up adenylate cyclase (AC) using a stimulatory G-protein.
This increases cAMP, which increases the flow of sodium through funny channels (doesn’t open it!!! Funny channels open below -45 mv)
This increases the slope of pacemaker potentials, leading to more action potentials over time and a faster heartbeat.
(Notice: cAMP increases funny channel flow directly, without PKA participation. So it turns out that a PKA inhibitor does not decrease the effectiveness of funny channel regulation of pulse.)
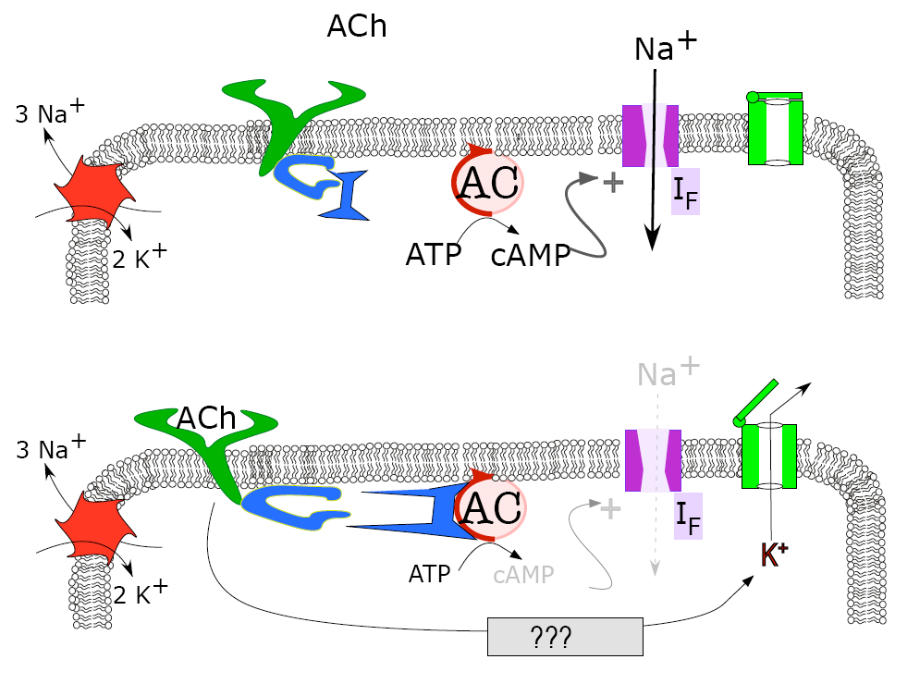
Pacemaker cells when acetylcholine (Ach) is involved:
Ach binds to the appropriate receptor, slowing down adenylate cyclase (AC) using an inhibitory G-protein.
This decreases cAMP, which decreases the flow of sodium through funny channels
Ach also opens K+ out channels, which are ligand gated
This K+ efflux decreases the slope of pacemaker potentials, leading to less action potentials over time and a slowerheartbeat.
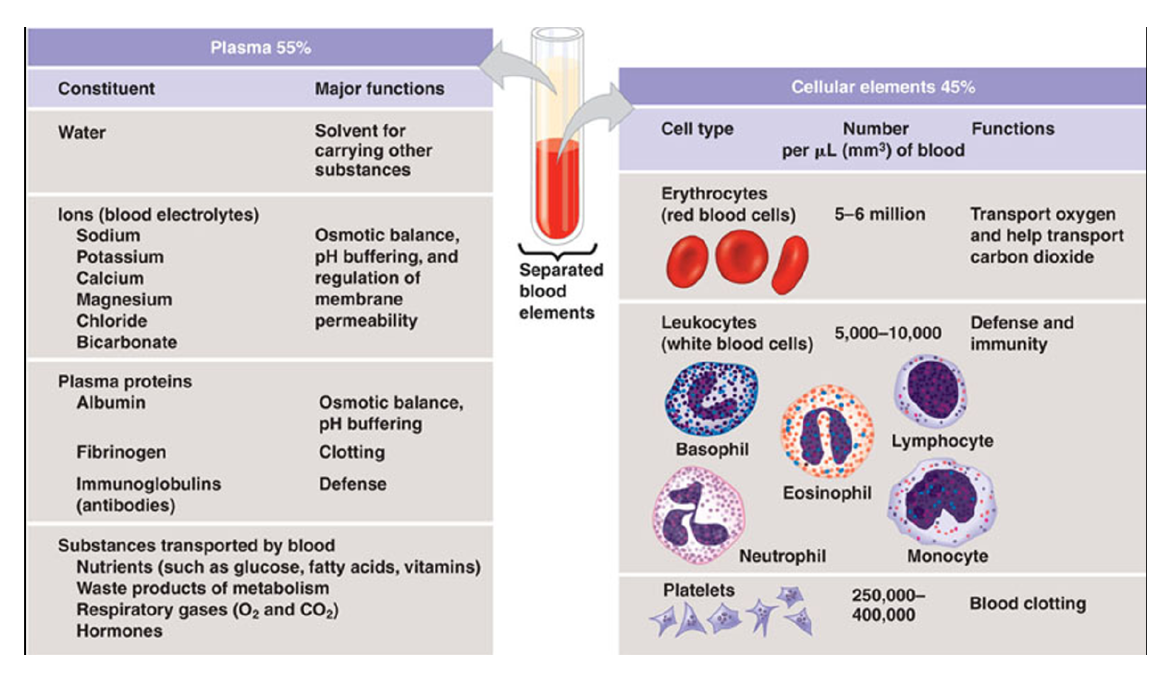
Blood is made up of 55% plasma and 45% cellular elements.
Plasma:
Water and ions
Plasma proteins - many functions, some will come up later in this class.
Most don’t pass from capillaries. Plasma is instrumental in keeping the osmotic potential of the blood lower than that of the interstitial fluid.
Delivery materials
Important materials and wastes, ions, fuel (sugar and fat), messages (hormones) etc.
Helps move heat.
Cellular components
Red blood cells
Have a flattened and concave shape that allows them to fold to easily fit through things and gives them a high SA/V ratio
White blood cells
Immune system (not covered in BI212)
5 white blood cell types present in numbers around 1/1000th the number of RBCs.
Platelets
Cell fragments involved in Hemostasis (clotting).
Plasma is the liquid portion of the blood in which clotting has been prevented by an anticoagulant. Serum is the liquid that remains if clotting is allowed to occur.
Funny channels are voltage gated cation channels that remain open when membrane potential is below (more negative) threshold potential. While open these channels generate the pacemaker potential that brings the membrane potential from resting potential to threshold potential.
A Post-Doc at the University of Maine studying metabolic thermogenesis engineered a bacterial version of adenylate cyclase (bPAC) into a line of mice cells that is directly activated by blue light. If we engineered the construct into mice pacemaker we would expect mice pulse to increase and we would expect a decrease in the pacemaker potential duration when blue light is provided due to changes in flow through funny channels.
Acetylcholine…
Does not open or close funny channels, but reduces flow through them. It also leads to the opening of ligand gated K+ channels
Fluid begins to enter the blood only after the blood is 50% of the way through the vessel. The blood pressure at this location is 7 Kpa greater than the pressure of the surrounding interstitial fluid. The interstitial fluid has an osmotic potential of -7 Kpa. What is the osmotic potential of the blood?
Δ7 = -7 + Ψo Blood
Ψo Blood = -14
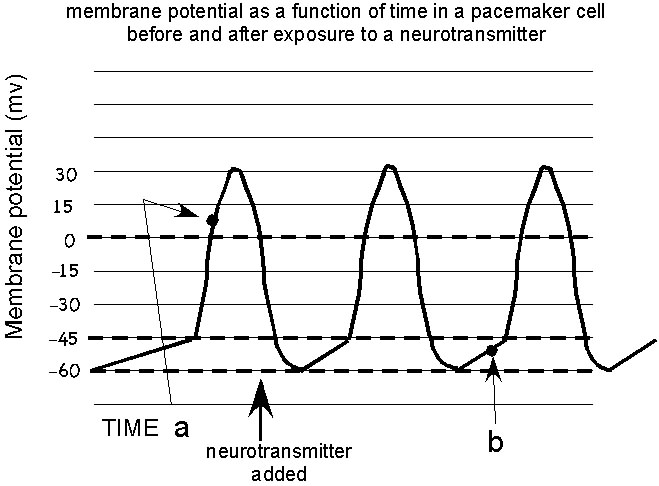
At time a:
The funny channels are closed. The voltage gated Ca++ channels are open. The voltage gated K+ channels are closed.
At time b:
The funny channels are open. The voltage gated Ca++ and channels are closed. The voltage gated K+ channels are closed .
Voltage below threshold opens funny channels. Voltage above threshold opens channels that participate in the action potential.
Concentration drives ions through the open channels at time a.
Charge and concentration drives ions through the open channels at time b.
Chloride exiting a smooth muscle cell of an arteriole would depolarize that cell if moving with a sufficient flow rate. Ca++ entering a cell would depolarize this cell, but it doesn't enter at a rate that moves membrane potential to a measurable extent.
Chloride exiting a smooth muscle arterial cell leads to a decrease in vessel diameter. This would tend to decrease flow through that vessel.
On a more global scale, if flow rate is maintained but the arterioles get a general signal that leads to a change in vessel diameter, the blood pressure in that organism will change in the direction opposite the change in vessel radius.