psychotherapy exam 4
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
95 Terms
Murphy Journal Club 3: Background
Metaanalyses demonstrate small but significant association between alliance and symptom reduction in CBT for depression
20% rate of dropout in psychotherapy for depression
Dropout associated with alliance
1 study in CBT for depression+meds
No studies of client expectations of alliance
How does the therapeutic alliance affect other areas of therapy like dropout?
No studies looking at high expectations of alliance (what client predicts/imagines what the relationship between client and therapist is going to be like)
Study aims
Compare change in symptoms prior to dropout between those who did/didn’t drop out
Examine client and therapist reported early alliance as predictors of dropout
Methods: participants
n=126 clients CBT for depression
60% female
83% white
85% completed some college
Mean age ~32
Primary major depressive disorder; stable med dose (34%) - could not have serious disorder like bipolar, substance dependence
N = 5 therapists
Advanced graduate students
2 women, 3 men
Methods: treatment
Up to 16 weeks
CBT for depression
Dropout
Stated intent to discontinue
No show 4 weeks
Methods: measures
Working alliance inventory-short
Therapist and I collaborate on setting goals for my therapy, etc.
Beck depression inventory
Results: dropout
17% dropout (robust)
Mean dropout session ~6
Lower symptom reduction predicted dropout risk
Those who dropped out had higher depression symptoms at last session than those who did not dropout
Results: Alliance
Client rated alliance predicted dropout risk over and above baseline depression and medication status
No significant prediction by therapist reported or client predicted alliance
No significant association between dropout and demographic factors, or medication status
Transtheoretical model of change: 5 core constructs
Decisional balance
Self-efficacy
Temptation
Stages of change
Processes of change
Decisional balance
individual's relative weight of pros vs. cons of changing
Self-efficacy
situation-specific confidence in ability to cope with high-risk situations without relapsing
Temptation
intensity of urge to engage in the behavior
Transtheoretical model of change
How someone progresses through stages of change
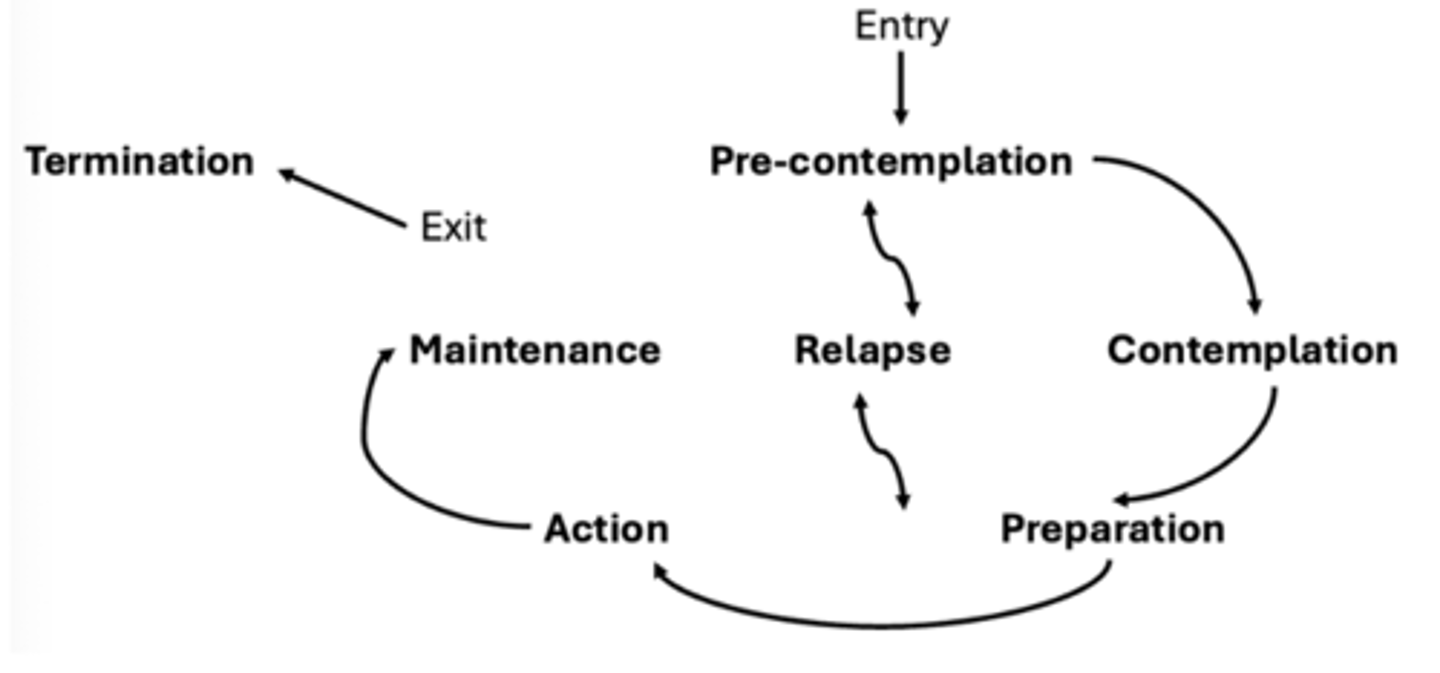
Stages
pre-contemplation
contemplation
preparation
action
maintenance
relapse
termination
Pre-contemplation
Not intending to take action in the foreseeable future (usually measured: at least next 6 months)
May be uninformed or underinformed about consequences of behavior
Or may have tried to change in the past and be demoralized
Avoid reading, thinking, talking about problematic behavior
Not ready for action-based therapy
Contemplation
Intending to change in next 6 months (some time in the foreseeable future)
Increased awareness of benefits of change
But also very aware of costs of change
Decisional balance -> ambivalence
Can get stuck in this stage
Not ready for action-oriented therapy
Preparation
Intending to take action in immediate future (the next month)
Typically have made some meaningful step towards change in the past year
Have a plan of action, but not acting yet
Ideal targets for action-oriented therapy
Action
Have made specific, overt change in past 6 months
Must meet criterion agreed upon by physicians/scientists to be sufficient to reduce health risks
Criterion depends on the behavior
Maintenance
Working to prevent relapse
Need to apply change processes less
Less temptation, more self-efficacy
Relapse
Regress to an earlier stage
Relapse is common
Typically return to contemplation or preparation
Not necessarily back to pre-contemplation
Termination
Not temptation, total self-efficacy
As if the unhealthy behavior never happened
Will not relapse regardless of context
<20% of smokers reach termination
More realistic goal may be sustained maintenance
Distributions of smokers by stage
Looking at current smokers (not in action/maintenance/termination)
Most people remain stuck in the early stages & not ready for action
- Most are in precontemplation and contemplation, fewer are in preparation
Treatments are going to be more effective if matched with stages people are actually in
Processes of change
overt and covert behaviors that people use to progress through the stages of change
Processes of change - 4 ways
Consciousness raising: increased awareness of causes, consequences, cures
- precontemplation stage
Self re-evaluation: assess self-image with and without the behavior
- contemplation
Stimulus control: remove cues for behavior, add prompts for healthy alternatives
- action
Contingency management: reinforce positive health behaviors
- action
Motivational interviewing - goal
Goal: reduce or eliminate substance use or other health-risk behaviors through expressing empathy and eliciting clients’ reasons for and commitment to changing
Informed by humanism, Carl Rogers person-centered therapy
Suited for clients in the precontemplation and contemplation stages
Four core assumptions of motivational interviewing
1. Ambivalence about substance use and change is normal and is an important motivational barrier to substance use behavior change
2. Ambivalence can be resolved by exploring the client's intrinsic motivations and values
3. Your alliance with the client is a collaborative partnership to which you each bring important expertise
4. An empathic, supportive counseling style provides conditions under which change can occur
Core skills in MI: OARS
Asking open questions
Affirming
Reflective listening
Summarizing
Asking open questions
Open questions are questions that invite clients to reflect before answering and encourage them to elaborate
Encourage clients to tell their story
Help therapist understand client's point of view
Facilitate dialogue
form: "Tell me about..."
Affirming
Therapist expresses genuine positive regard for client
Promotes client self-efficacy
Convey message of “I see you, what you say matters, and I want to understand what you think and feel”
Emphasize client strengths, successes, and efforts to change
You vs. I framing
Reflective listening
Key component to expressing empathy
Make a mental hypothesis about the underlying meaning or feeling of client statements and then reflect that back your best guess
Establishes trust and invites clients to explore their own perceptions, values, and feelings
Encourages a nonjudgmental, collaborative relationship
Follow open questions with at least one or more reflective listening response before asking another question
Summarizing
Form of reflective listening that distills the essence of several client statements and reflects them back
Select statements that have meaning for the client and present them in summary the gives a fuller picture of client’s experience
Ways of summarizing
Collecting: create a narrative of a series of related client statements
Linking: link back to an earlier client statement
Transitional: wraps up a conversation or task to propel the change process
Ambivalence: summarize sustain and change talk during 1 session
Recapitulation: summarize change talk from many sessions
Sustain talk and change talk
Sustain talk: client statements that support not changing
Change talk: client statements that support changing
Goal: evoke change talk and minimize evoking or reinforcing sustain talk
Change talk: DARN-CAT
Desire to change
Ability to change
Reasons to change
Need to change
Commitment
Activation
Taking steps
Evoking change talk
Eliciting importance of change
Exploring extremes
Looking back
Looking forward
Minimizing sustain talk
Simple reflections
Amplified reflections
Double-sided reflections
Agreements with a twist
Reframing
Emphasis on autonomy
Developing discrepancy
Identify how behavior conflicts with client's values and goals
Recognition of discrepancy -> increased motivation to change
Therapist must convey acceptance, compassion, affirmation
The Columbo approach
MI Efficacy
Meta-analysis on adolescents with substance-use
Small effect size for post-treatment & follow-up
Most have only 1 session of MI
With larger doses of MI, we might have more substantial effect sizes
Summary

Pain
An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage
acute vs. chronic
Acute pain vs. Chronic pain
Acute
Less than three months
Is a symptom
Identified cause; body’s response to injury
Diminishes with healing and responds to treatment
Chronic
More than three months
Is a condition
May develop after incident; may have known or unknown cause
Persists beyond expected healing time and/or despite treatment
Pain categories
Nociceptive pain
Musculoskeletal
Described as aching or deep
Neuropathic pain
Peripheral or central nerves
Described as burning, shooting, electric
Headache pain
Felt in forehead, eyes, neck
Describe as a tight band, pounding, throbbing, dull
Development of pain theories
René Descartes (17th century): mind cannot influence the body
Specificity Theory of Pain (1894): sensory receptors are directly responsible for pain
Gate Control Theory (1965): pain signals project from pain location and are gated by the brain
Neuromatrix Model of Pain (1976): pain is an interaction between initial pattern of nerve impulses (neuromatrix) and sensory experiences and learning (neuroplasticity)
Biopsychosocial Model
Build on the Gate Control Theory and the Neuromatrix Model of Pain
The individual experience of pain is influenced by physiological, psychological and social factors
Pain is physical signals sent by the nervous system; Suffering and pain behaviors are affected by individual differences
Psychological factors
Pain cognitions
Catastrophizing
Subcategory of pain cognition
Hurt vs. harm
Negative affect
Answer-seeking
Pain self-efficacy
Behavioral factors
Passive coping
Guarding
resting/underactivity
Active coping
Exercise
Overactivity
Social factors
Solicitous others
Punishing others
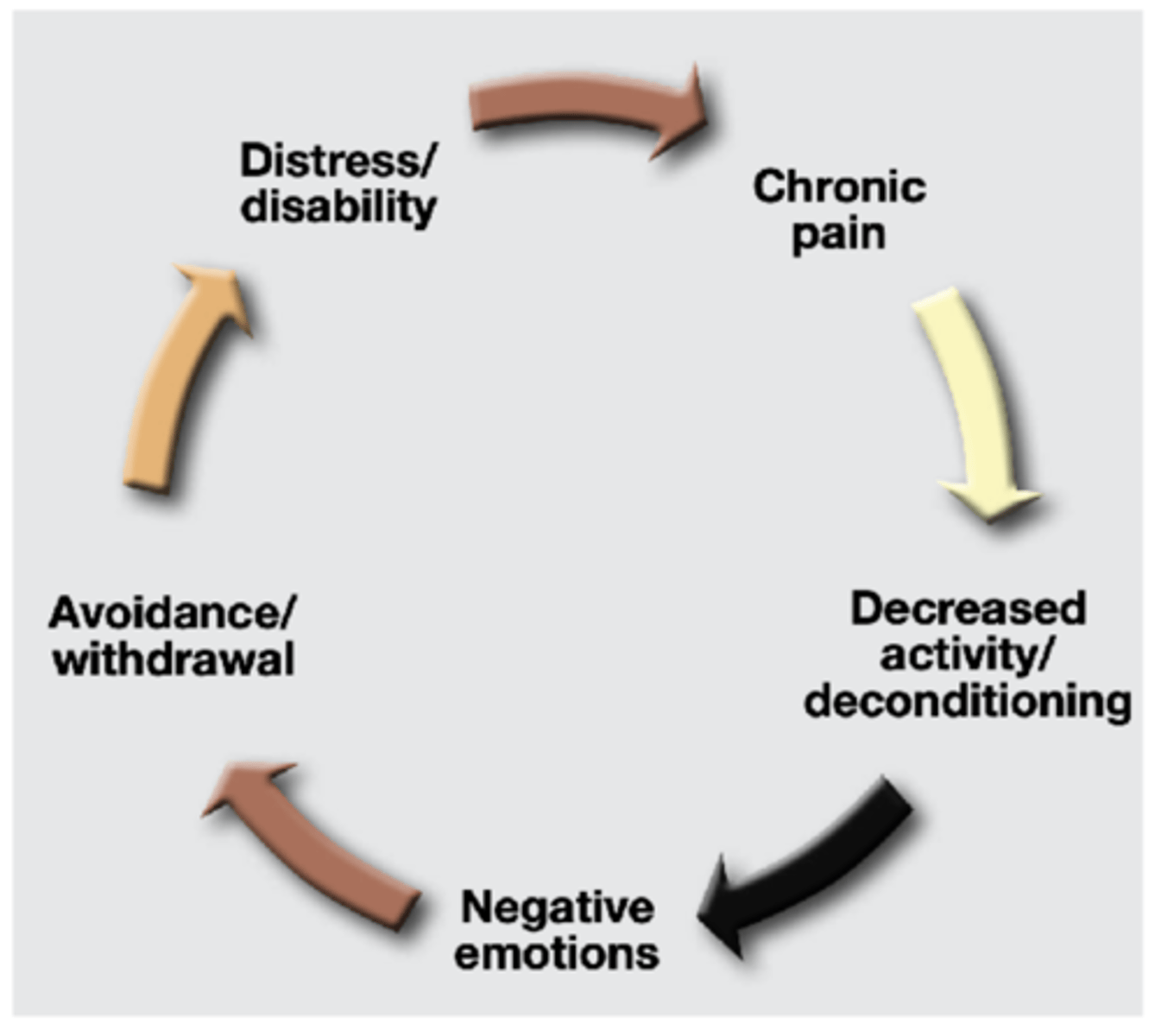
Chronic pain cycle
Experience of chronic pain
Decreased activity/deconditioning
Negative emotions
Avoidance/withdrawal
Distress/disability
Experience of chronic pain
CBT-CP model
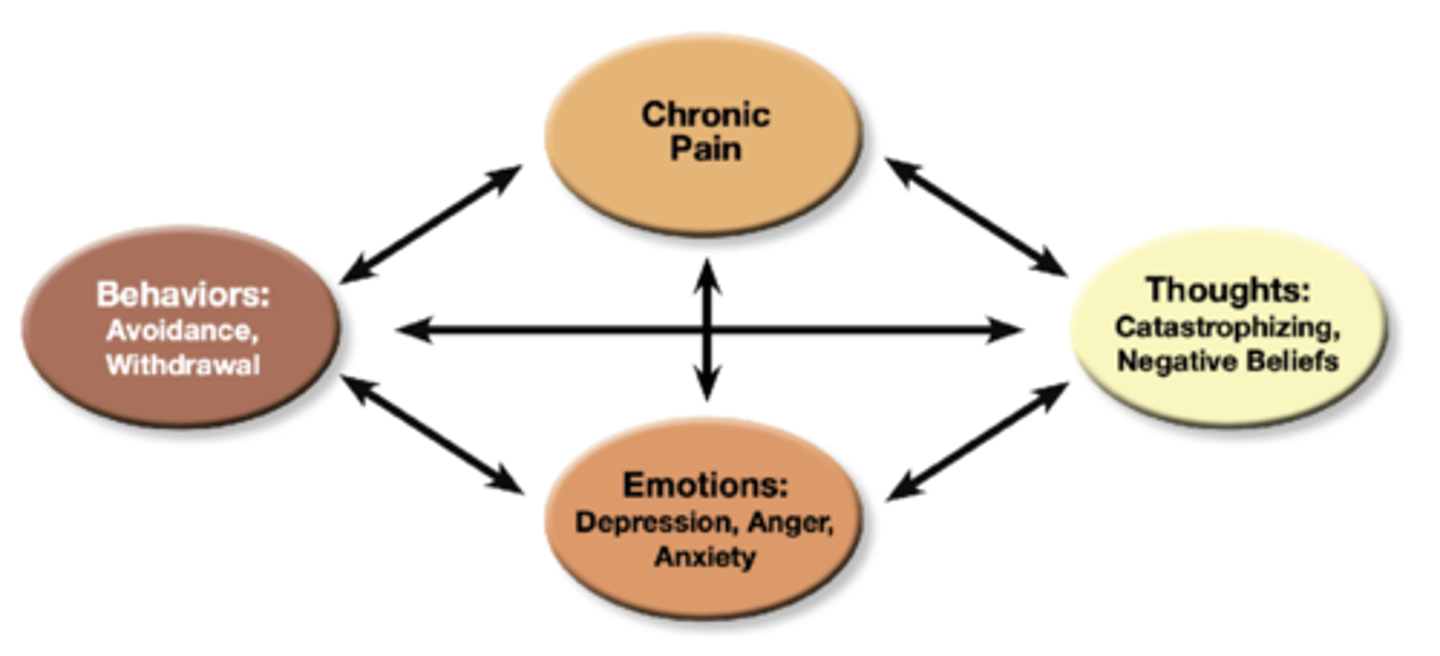
Goals of CBT-CP
Reduce negative impact of pain on daily life
Improve physical and emotional functioning
Increase effective coping skills for pain management
Reduce pain intensity
Components of CBT-CP
Exercise & pacing
Relaxation training
Behavioral activation
Cognitive restructuring
Sleep health
Exercise
Goal: increase activity levels to increase physical health
“Motion is lotion”: the more you move, the easier to move
PCP (medical provider)-approved walking program or other low impact exercise
Difficult for clients to accept that movement will make pain better
Emphasize movement is foundation for healthy body, walking is safe, and plan will be gradual
Set goal to walk 5 days/week with increasing duration
Cannot be accomplished through existing activities
Pacing
Engage in moderate, safe level of activity regularly
Time is guide
Break activity into segments with rest between
Helps to maintain a consistent activity level, improve mood through effectively accomplishing tasks
Relaxation training
Chronic pain is a physical and psychological stressor
Creates additional wear and tear on the body
Physical tension and emotional distress increase pain-related stress
Use relaxation skills to activate parasympathetic nervous system to counter stress response
Repeated practice -> skill to manage stress
Relaxation training techniques
Deep breathing
Guided imagery
Progressive muscle relaxation
Behavioral activation
Those with chronic pain tend to have decreased their engagement in pleasurable, meaningful activities
Decreases quality of life, increases negative mood
Benefits of engaging in pleasurable activities
- Positive distraction from pain
- Improved mood and self-esteem
- Increased socialization
- Enhanced attention, concentration ability
- Enhanced sense of purpose and direction
Cognitive restructuring
Catastrophizing
Should statements
All or none thinking
Overgeneralization
Jumping to conclusions
Emotional reasoning
Disqualifying the positive
Sleep
Sleep -> pain
Not getting enough sleep: can increase the feeling of pain & disrupt the restorative process
Negative consequences in mood & attention that also modulates sleep
Pain -> sleep
Pain can impact sleep
Pain-related factors that influence sleep
Pain medications
bedding/pillows
Daytime bed use
Substance use
Low daytime activity
Stimulus control
Only go to bed when sleepy
Use bed only for sleep and sex
If unable to sleep after 20 minutes, get out of bed and return only when sleepy
Wake up at the same time every day
Do not nap
Efficacy of CBT-CP
For lower-back pain, evaluate pain & disability
Immediately after treatment: small-medium effect size on disability & pain
Pain follow-up: effect size becomes smaller over time
Disability follow-up: also drops over time, rebound at 12 months
The effects tend to be statistically significant but small
Summary

Sleep continuity: sleep metric
Sleep duration: total amount of time from sleep onset to sleep offset
Sleep onset latency (SOL): amount of time to fall asleep
Wake after sleep onset (WASO): amount of time spent awake from sleep onset to sleep offset
Sleep quality: subjective perception of quality of sleep
Sleep efficiency: sleep duration/time in bed (%)
Healthy: 85%-90% or higher
Sleep stages
Non-rapid eye movement (NREM)
3 stages: stage 1, 2, 3
Progress from lighter to deeper sleep
Rapid eye movement (REM)
Characterized by rapid eye movements, muscle paralysis, and mixed frequency EEG activity
- Prevent us from acting out on our dreams
- EEG activity: similar to an awake brain
Two process model of sleep regulation
The homeostatic sleep drive
As you stay awake, the drive accumulates
The accumulating pressure for sleep drives for sleepiness
During sleep, the pressure decreases
The circadian drive for arousal
24-hour clock in our body, one of the output is circadian wakefulness
Sending the highest alerting signals during mid-day, dropping off at biological night
Most likely to fall asleep when pressure for sleep is high and circadian alerting signal is low
Most likely to wake up when pressure for sleep is low and circadian alerting signal goes up
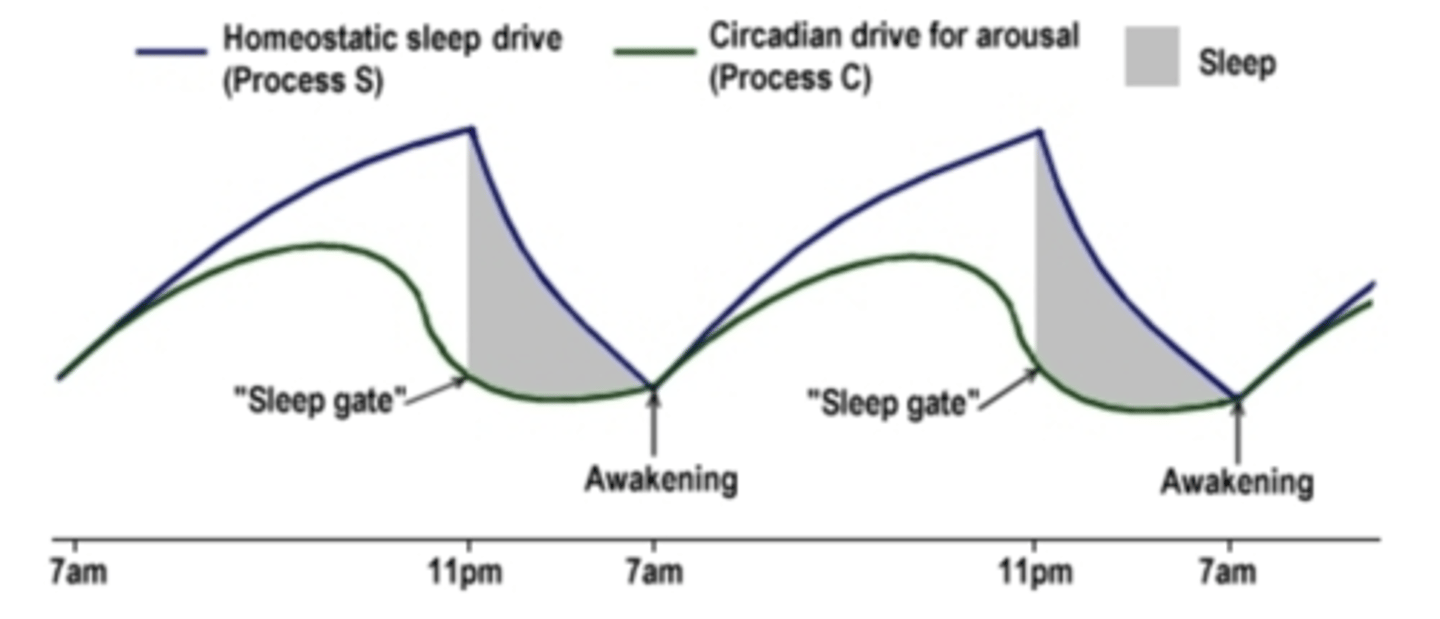
Circadian rhythms
Describe 24-hour rhythms and multiple processes that keep us in sync with the light/dark cycle
Allow us to anticipate changes in our environment rather than respond passively
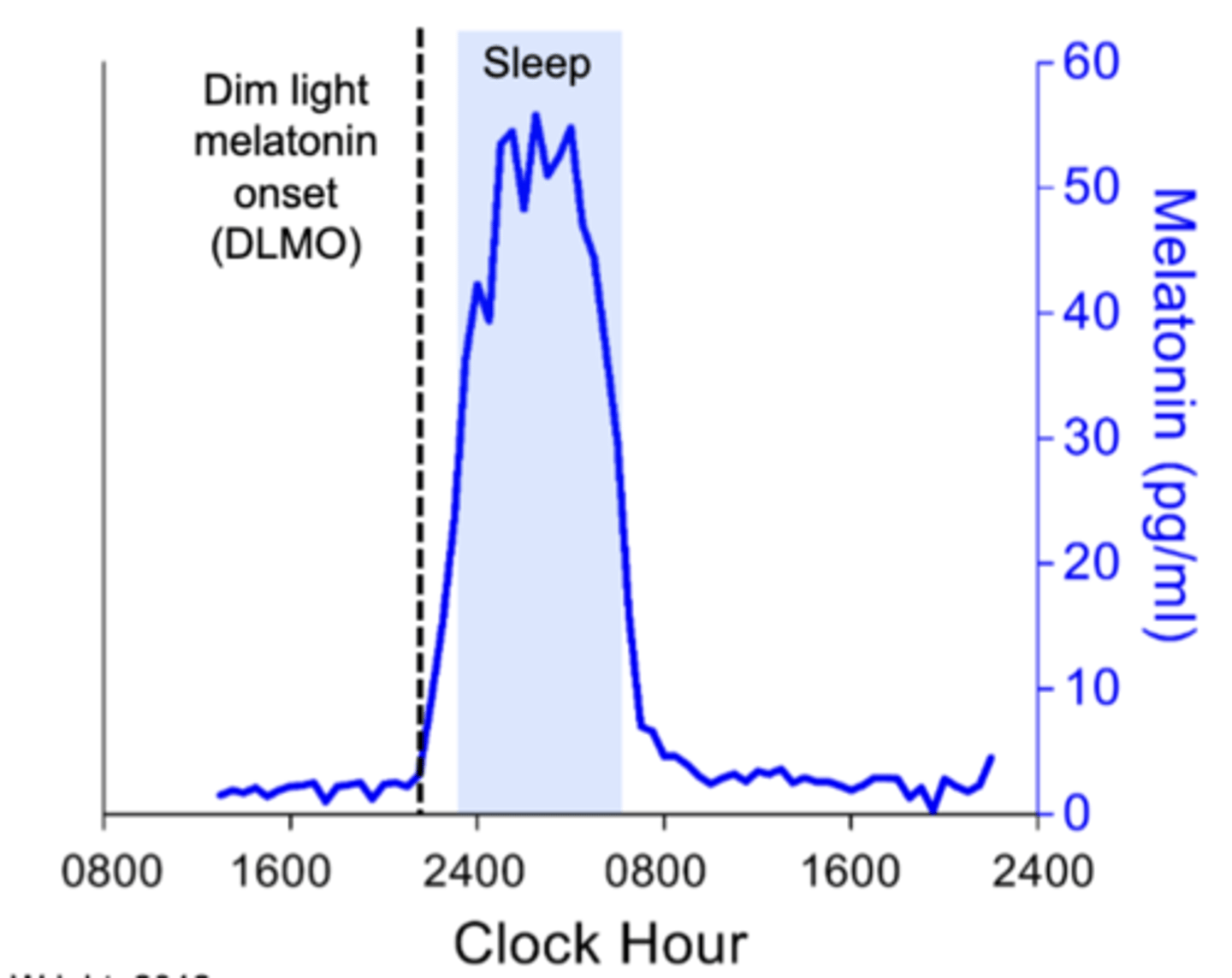
the circadian rhythm of melatonin: Low during daytime, have a peak over night
To measure circadian rhythm: measure the time we see the steep rise of melatonin levels
Cognitive Behavior Therapy for Insomnia (CBTI)
Behavioral treatment designed to treat chronic insomnia (unable to fall asleep, stay asleep, wake up too early)
Behavioral model of insomnia
Y-axis: insomnia severity
Threshold: when insomnia symptoms become clinically significant
Premorbid: no insomnia symptoms
Acute: meaningful insomnia symptoms
Early: engage in perpetuating factors
Chronic: precipitating factor goes away, perpetuating behaviors maintaining the insomnia in the long-run
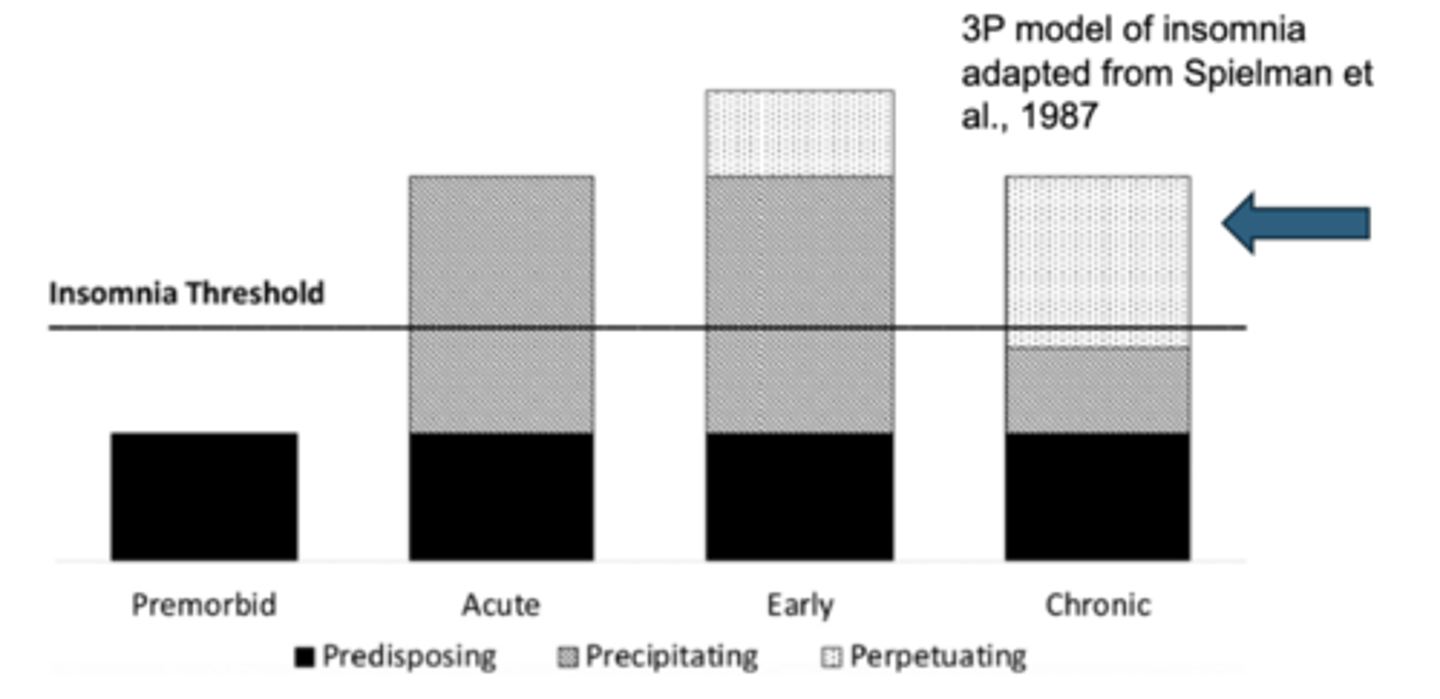
3P model of insomnia
Predisposing: risk factors, things make you more vulnerable to insomnia but don’t cause insomnia on their own
- Genetic risk, medical conditions, mental disorders
Precipitating: stressor in the short-run
- Stressful life event (positive or negative)
- Most people experience in their lives
Perpetuating: behaviors that maintain insomnia over time
- Try to compensate for the sleep loss or to get more sleep
- Spending excessive time awake in bed, going to bed earlier, doing things in bed other than sleep or sex (try to catch sleep)
The problem with perpetuating factors
Mismatch between time in bed and sleep duration
Stimulus dyscontrol
Conditioned arousal
3 core components of CBTI
Stimulus control
Sleep restriction
Sleep hygiene
Stimulus control: playing the odds
Odds 1 in 2: sleep/sex
Odds 1 in 6: sleep/sex/read/eat/worry/work
Complex conditioning history: stimulus paired with many responses
Low probability the stimulus will yield a single given response (sleep)
Stimulus control
Aims to limit amount of time spent in bed/bedroom awake
Instructions:
- Go to bed only when sleepy
- Avoid any behavior in the bed or bedroom other than sleep and sexual activity
- Leave the bedroom if awake more than 15 minutes
- Return to bed only when sleepy
Goal: reduce stimulus dyscontrol; create new conditioning history (bed-sleep instead of bed-awake)
Sleep restriction
Limit sleep opportunity to current sleep duration
Sleep prescription
- Set fixed wake time based on patients weekday needs
- Set bedtime based on average sleep duration
Goals
- Reduced mismatch between time in bed and time asleep
- Increase sleep pressure -> more consolidated sleep
Weekly upward titration by 15 minutes if >90% sleep efficiency
Sleep hygiene
good habits related to sleep
Aims to address problematic sleep-related behaviors/environment
Not effective monotherapy
Example sleep hygiene instructions
- Exercise regularly
- Make sure you bedroom is at a comfortable temperature
- Don’t watch the clock
Optional components
Cognitive therapy
Reduce preoccupation with or anxiety about insomnia
Relaxation/mindfulness
Reduce physiological arousal in the pre-sleep period
Light therapy
Reduce circadian phase delay/advance
CBTI efficacy
Recommended as first-line treatment for insomnia by American College of Physicians
Reduces sleep onset latency and wake after sleep onset by ~50%
60-80% have a therapeutic response to treatment
Improvements stable up to 24 months
Small acute increases in sleep duration but ~1hr increase over long-term follow up
CBTI vs. hypnotics: efficacy
Similarly effective in short-term
CBTI treatment responses maintained up to 24 months
- Long-term: more enduring benefits
Gains from medications diminish after medication cessation
- Hypnotics: more side-effects, tolerance problems
CBTI + hypnotics
adults with insomnia randomly assigned to CBTI alone or CBTI + hypnotics
Conclusion: the combined group has a faster response to treatment compared to CBTI alone, but both groups end up in the same place
Light Therapy
Light has multiple effects: circadian and training effects (directs our circadian clock), but also non-circadian regions of the brain (arousal effect), and mood-related areas of the brain (mood-promoting effect independent of the circadian effect)
time of light exposure
The time at which we receive light exposure affects its impact on circadian clock
Bright light in the morning + dim light in the evening: shift circadian clock earlier
Dim light in the morning + bright light in the evening: shift circadian clock later
The same principle used in light therapy: increase in bright light morning exposure
Light therapy delivery options
Historically: delivered through light boxes: high-intensity lighting
10,000 lux = outdoor natural daylight, 30min-1hr each morning after wake up to receive treatment
Limitation: have to sit in front of the box: burdensome
Recent alternative: wearable light therapy glasses
Benefits: less burden, can continue morning routine
Downsides: much dimmer intensity of light compared to the box (400-500 lux, bright indoor lighting)
Light therapy in seasonal depression
Compared patients with seasonal depression to healthy controls
Baseline: one week of fixed sleep schedule
Two light therapy conditions: bright light 6-8am or 7-9pm
Measure depression symptoms & circadian rhythm using melatonin onset
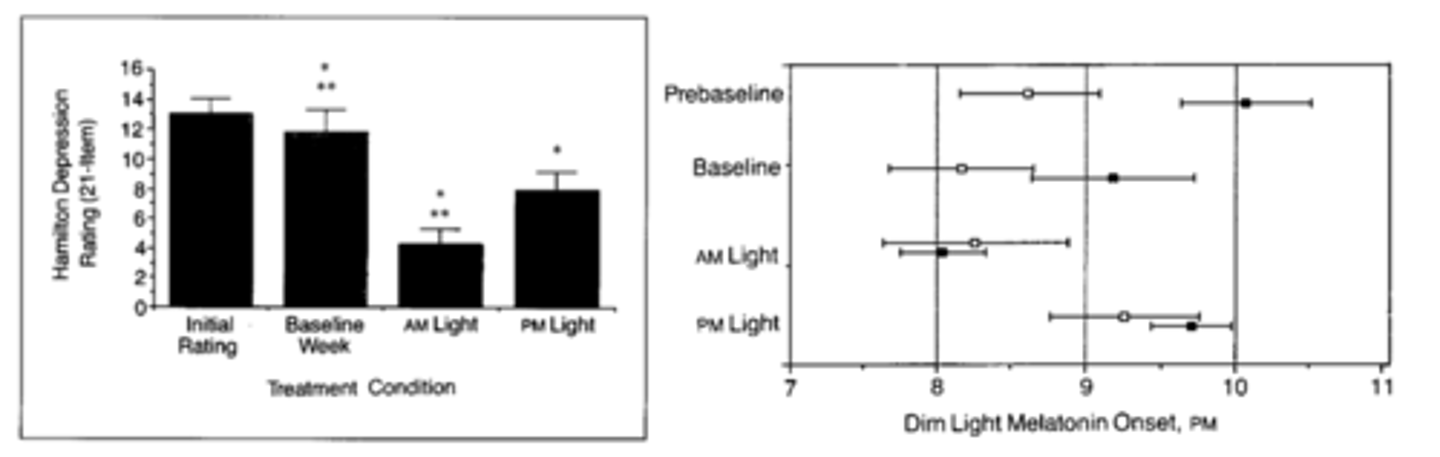
Compared to baseline week, depression symptoms decreased in both conditions, largest in morning condition compared to evening condition
Patients with seasonal depression have a significant delay pre baseline
In baseline: an advance just by stabilizing the sleep schedule
Morning light condition: further circadian phase advance
Evening light condition: circadian phase moved later
Conclusion: two effects of lights (circadian + mood impact)
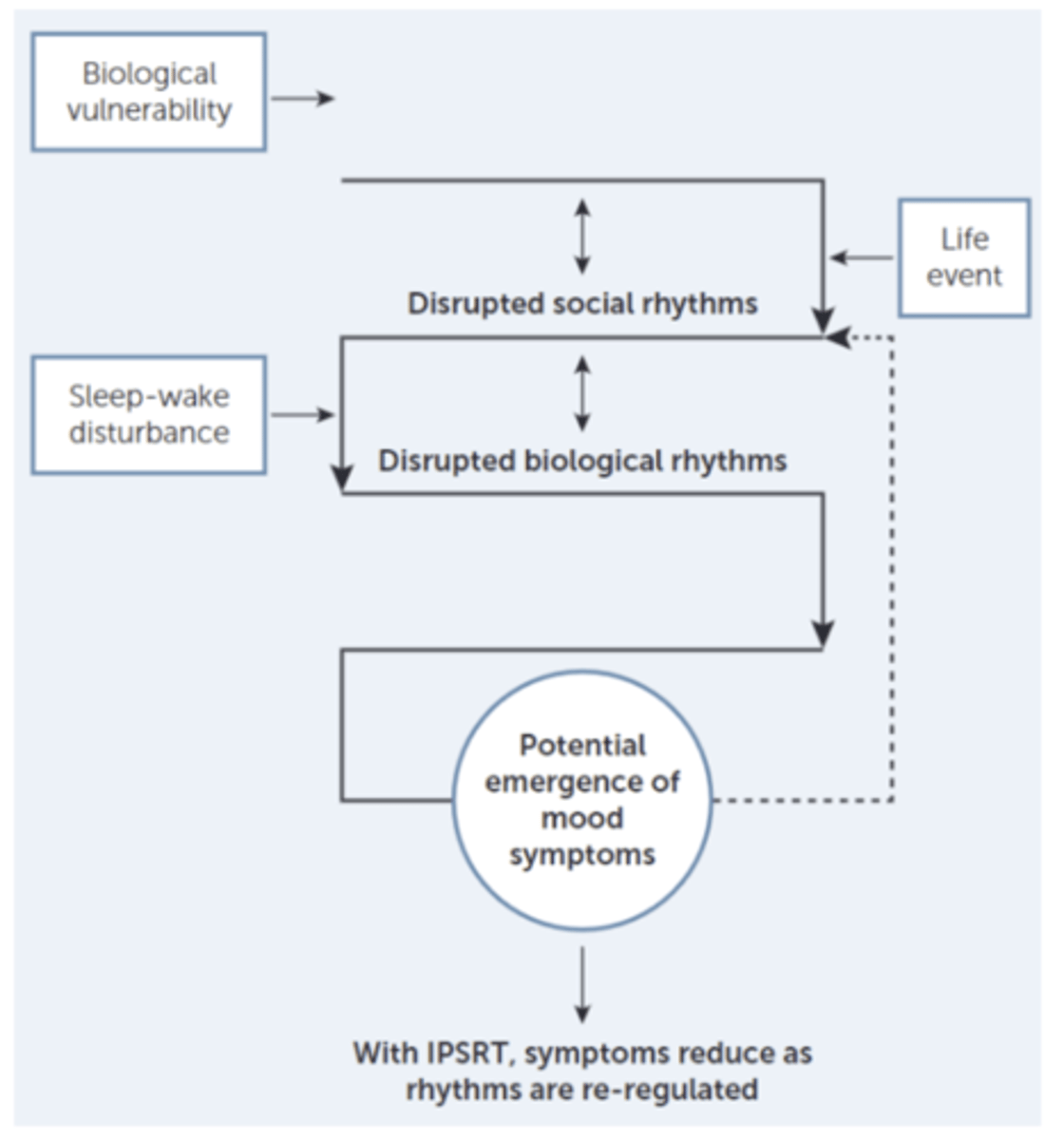
Interpersonal and social rhythm therapy (IPSRT)
Developed for bipolar disorders
What are the intervening mechanisms of stressful life events precipitating mood episodes?
Social time cues: interacting with people, eating, etc.
Stressful life events disrupt social time cues (context about time), which impact circadian rhythms, and result in disruption in biological rhythms, which in turn precipitate a mood episode
Interpersonal and social rhythm therapy (IPSRT) component
Interpersonal psychotherapy +
Social rhythm therapy: stabilize social time cues, which in turn stabilizes biological rhythms
Have clients track their social rhythm through social rhythm measure (SRM-5)
Help them construct a daily schedule to stabilize social time cues

IPSRT Efficacy
Efficacious for improving bipolar disorders
BP vs. TAU
T0: baseline; T1: 3-month into treatment; T2: 3-month follow up
A significant reduction in manic symptoms for IPSRT compared to TAU
Increase the amount of time into the next mood episode
Improved regularity of social rhythms
Association between increase social rhythm regularity & reduced likelihood of mood episode recurrence
The role of sleep and circadian medicine in traditional psychotherapy
Sleep disturbance and mental health
Across disorders, medium to large effects for decreased sleep continuity, small to medium to decreased sleep depth, small to medium to increased REM pressure compared to healthy controls
Takeaway: broad association between worse sleep and mental health conditions
Delayed sleep timing associated with blunted response to psychotherapy for OCD
Worse sleep reduces treatment responses for psychotherapies
Later sleep timing (suggesting rhythm delay) is associated to lower response to ERP for OCD
Bedtime at baseline: divided into non-delayed and delayed group
delayed: less reduction in symptoms, more non-responders
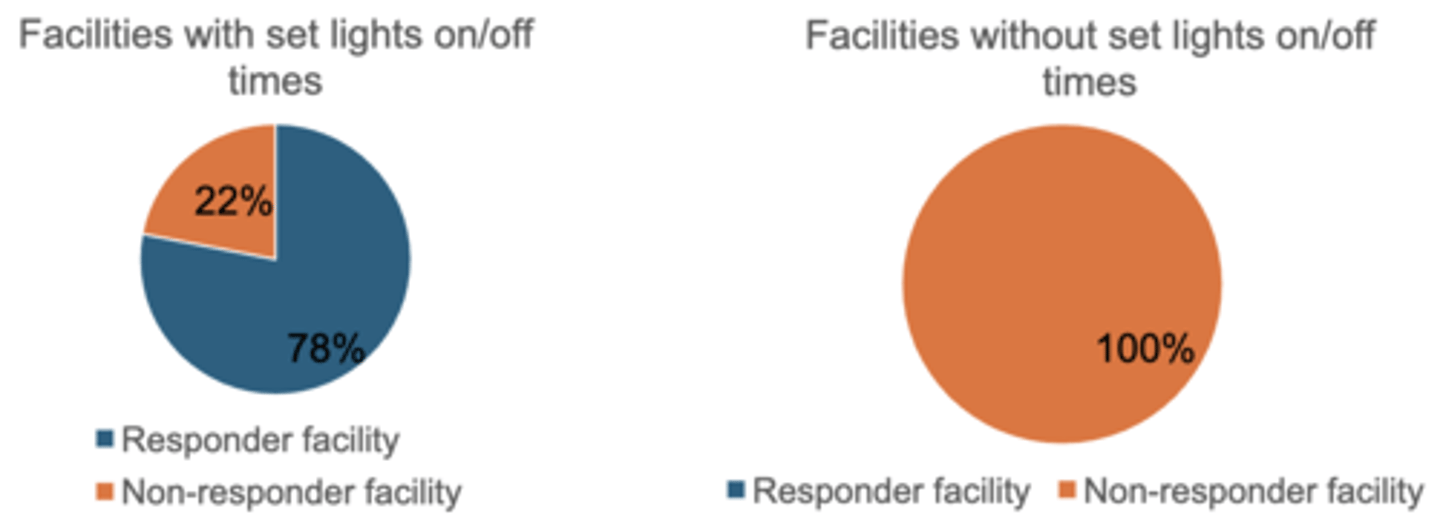
Consistent lighting schedules associated with treatment response in residential OCD treatment facilities
Residential facilities for OCD categorize by the average symptom scores of their patients at discharge
Responder facility: the average patient responds to treatment
Non-responder facility: the average patient doesn't respond to treatment
A fixed lighting schedule can have impact on treatment outcomes
Multiple symptoms of psychopathology decrease following CBTI in adolescents
Adolescents with insomnia treated with CBTI (GT)/CBTI over Internet (IT)/waitlist
Both GT and IT significantly decreased mood symptoms that are maintained after 12-month follow-up
Both GT and IT significantly improvements in sleep efficiency
Only treated for insomnia but have improvement on other symptoms
Depression and anxiety decrease following CBTI in pregnant women
Pregnant women with insomnia treated with digital CBTI or TAU
Depression and anxiety decrease from pre to post insomnia treatment and were maintained after 12-month post-treatment follow-up
Suicide ideation decreases following CBTI
Treated with CBTI or control
CBTI reported lower rate of SI at post-treatment and 1-yr follow-up
CBTI enhances PTSD treatment
Treated with CBTI first and then CPT (treatment for PTSD) or control first + CBT
After CBTI/control & after CPT, CBTI has significantly lower depression and PTSD symptoms
Only targeting sleep has significant positive benefits for individual depression and PTSD symptoms
Adding CBTI onto psychotherapy for PTSD improves treatment outcomes
CBTI prevents incidence of depression
Patients treated with CBTI followed over time
Those who were treated with CBTI were less likely to be depressed in the future compared to control
Can leverage CBTI to prevent new depression onset in the future
Summary
