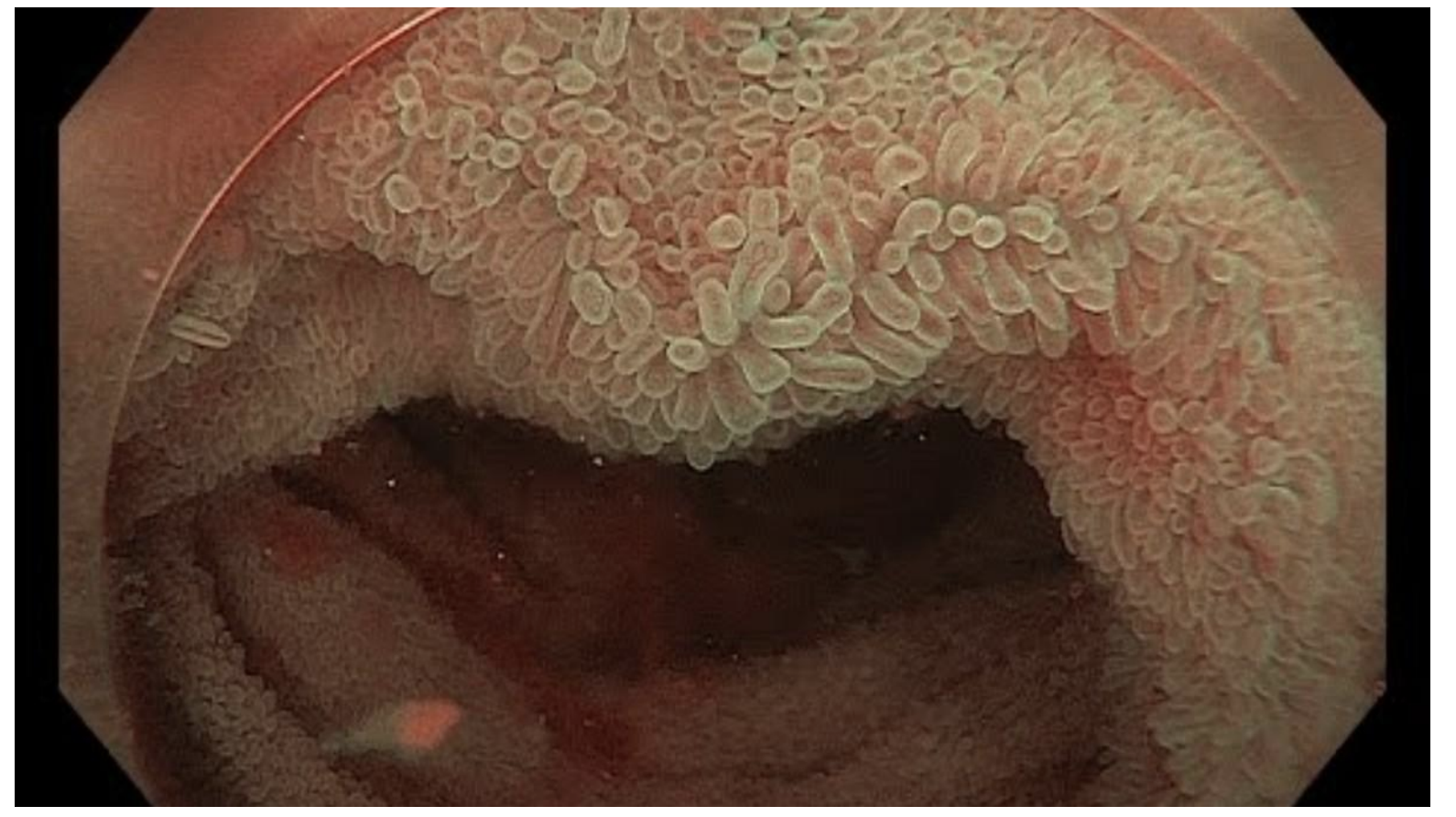
Digestive System
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
Intro
-how long
-accessory organs
-where is the lumen technically
-digestion
-30 feet in cadavers; shorter in living body due to muscle tone
-Accessory organs: not part of digestive tract but secrete substances into it; ex=pancreas, liver
-Lumen is technically outside the body (*some things never absorbed; imp barrier bc don’t want gut bacteria to mix)
-Digestion: breaking down food into simpler chemicals that can be absorbed/utilized by the body (*ex: protein → AA)
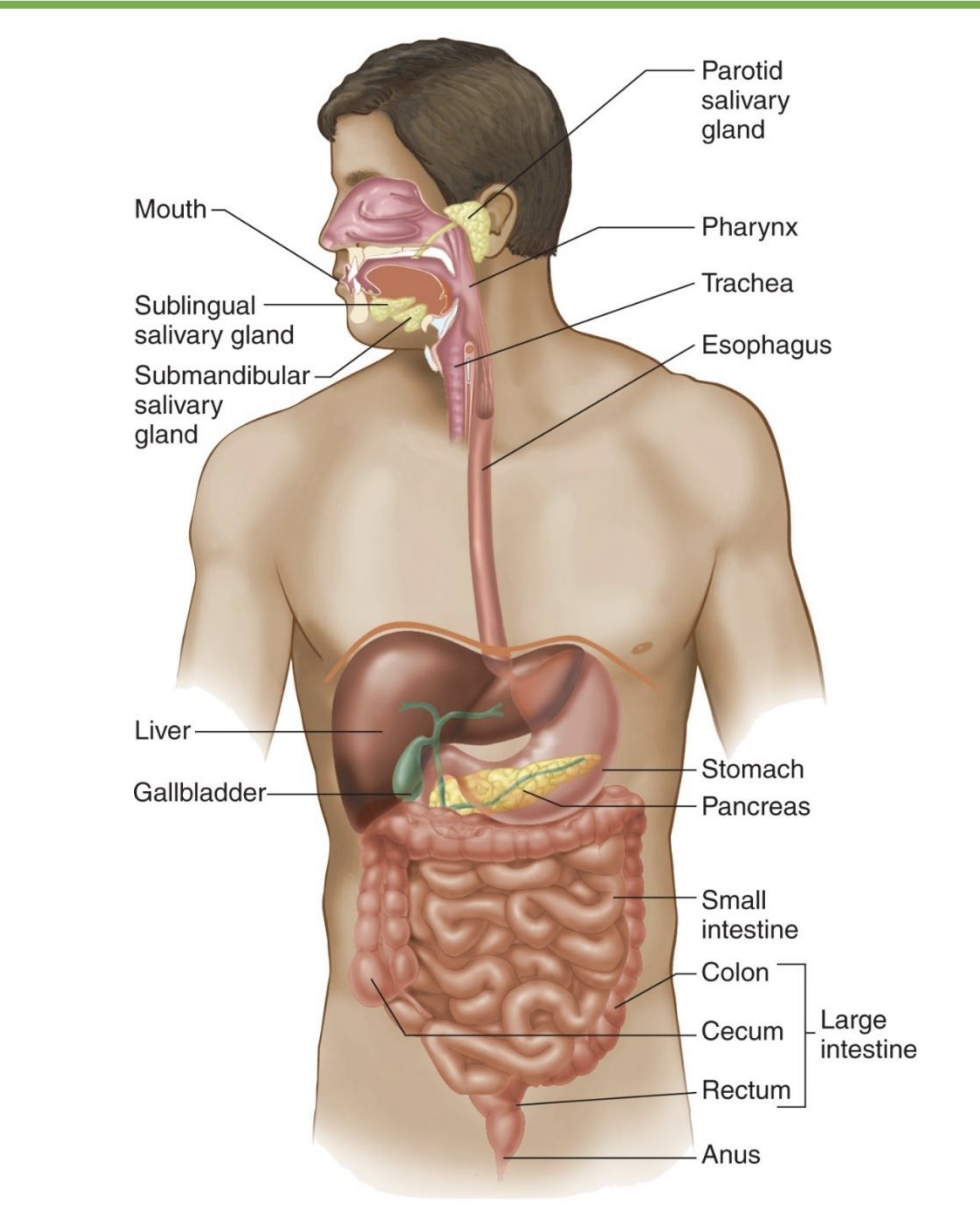
secretion vs absorption
-secretion: blood → lumen
-absorption: lumen → blood
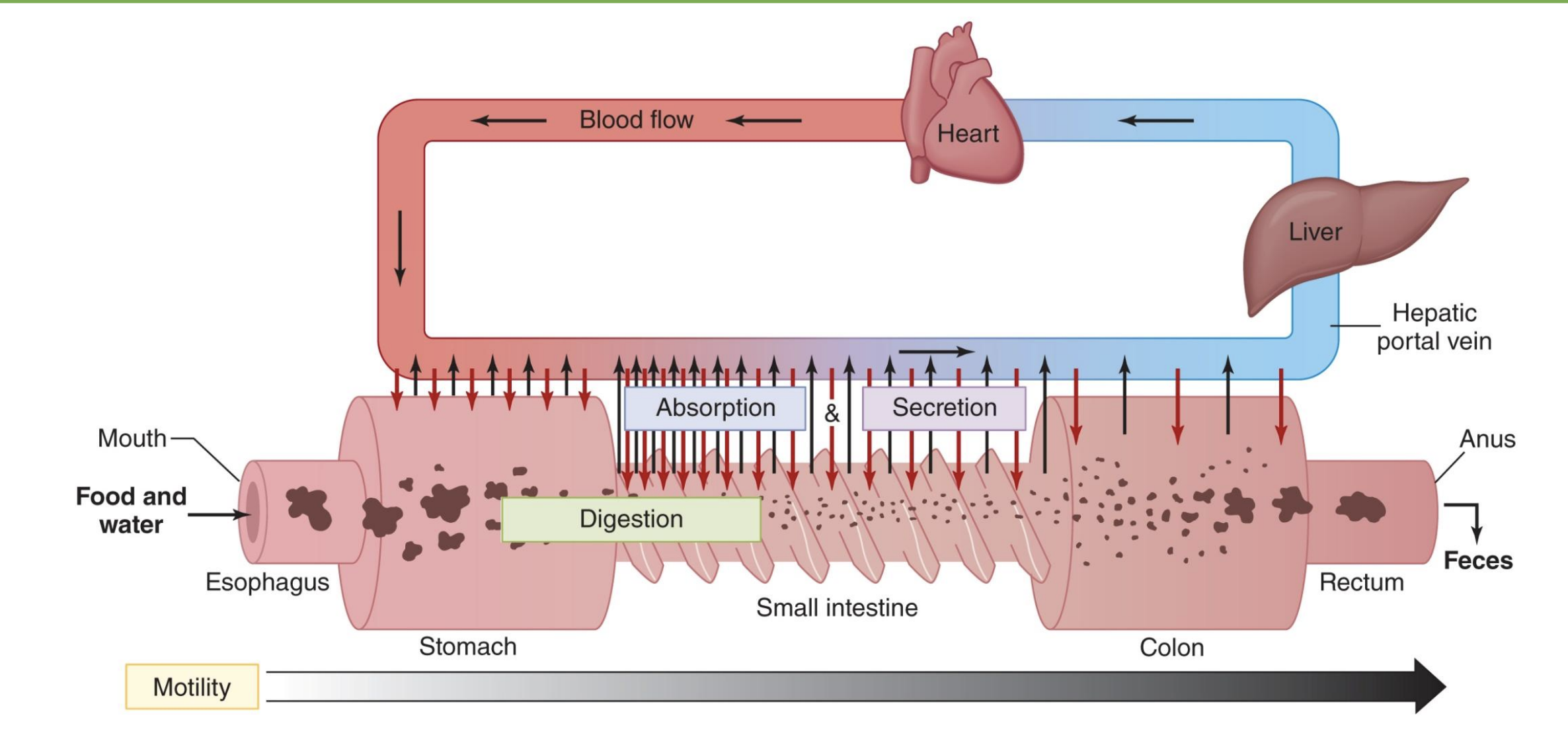
where does most digestion happen?
small intestine (first half)
-mouth: mechanical break down and saliva
-stomach: holding take, some digestion with HCl and pepsin
-SI: most digestion in first half, bile and pancreatic secretions, most useful things absorbed by end of SI
-LI: some absorption, water and electrolytes
*liver: main organ of nutrient balance
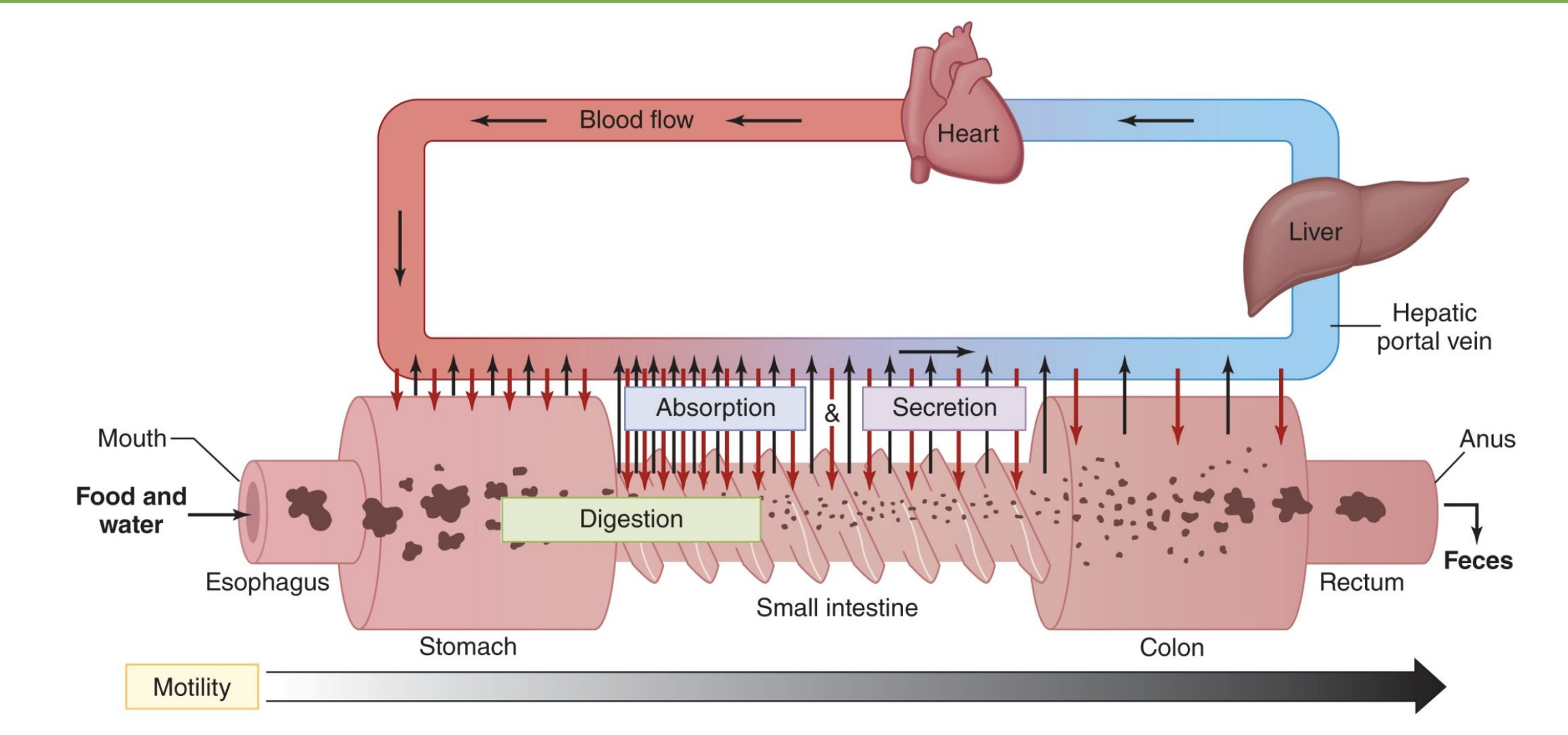
average secretions
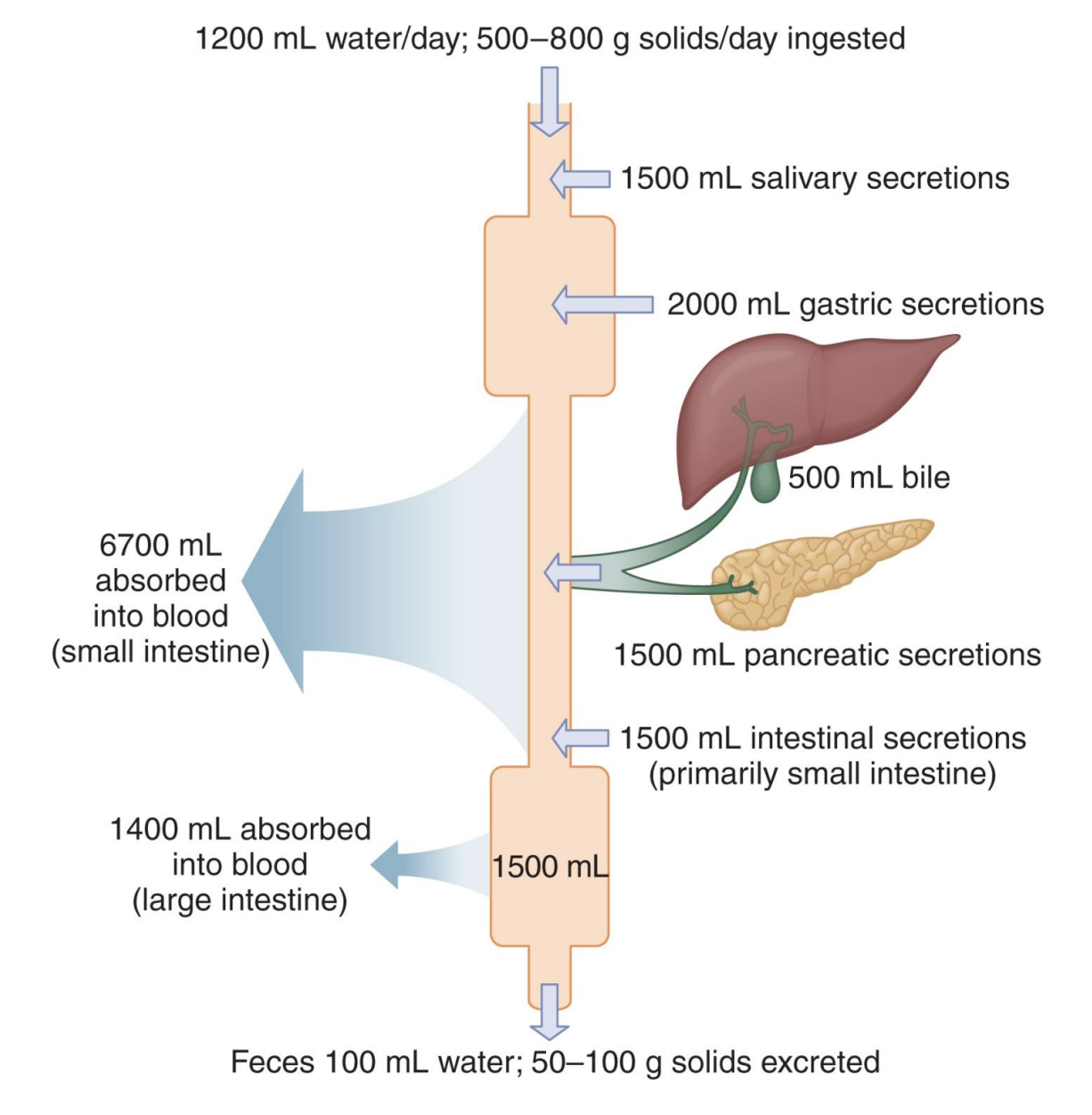
Average amounts of solids and fluid ingested, secreted, absorbed, and excreted from the gastrointestinal tract daily; most reabsorbed
-salivary secretions: in mouth
-gastric secretions: gastrin, pepsin
-pancreatic secretions
-LI: recovers a lot of water not reabsorbed earlier
-only 100mL water lost
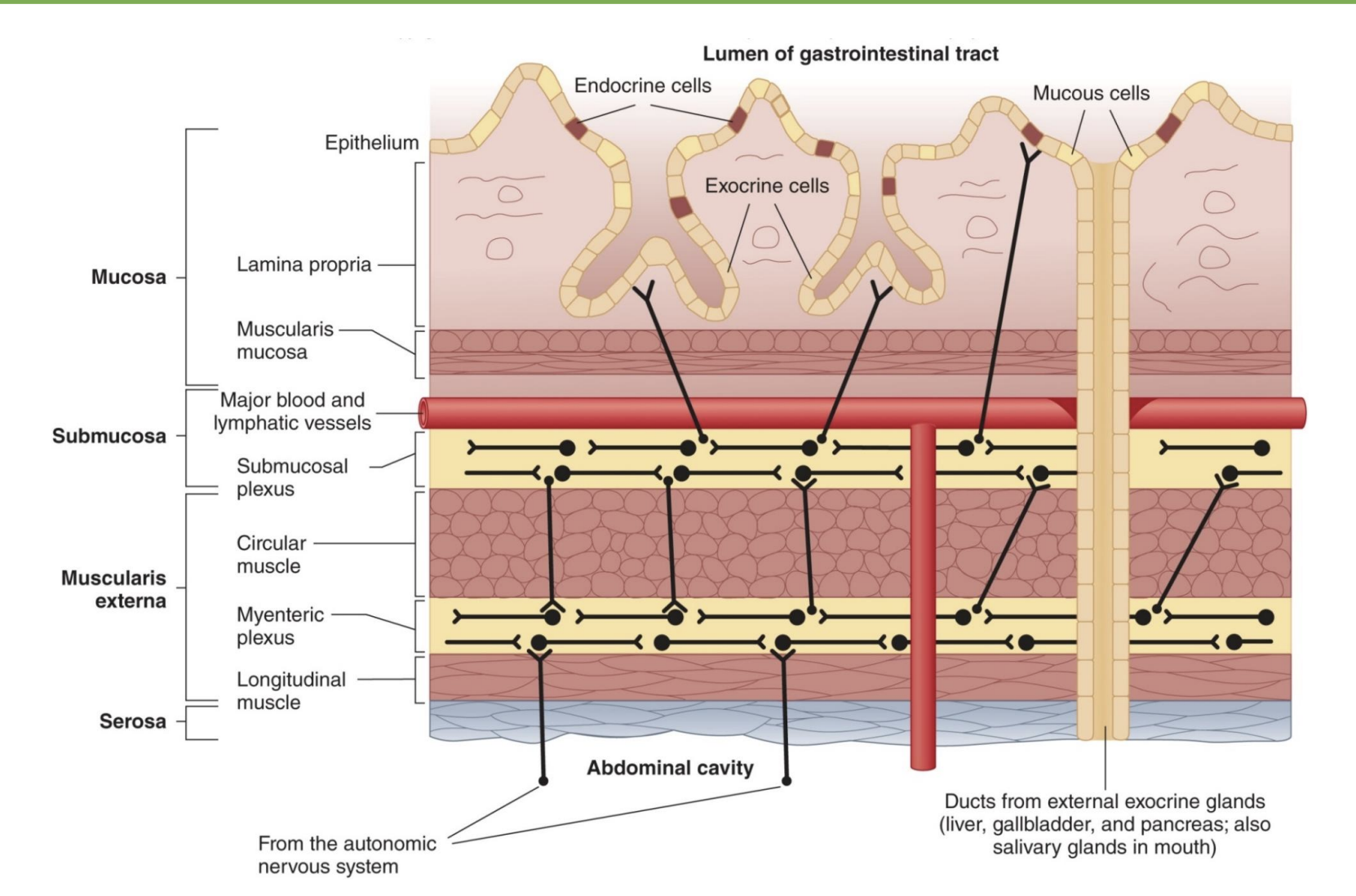
Structure of the Gastrointestinal Tract Wall
same throughout GI, but customized to dif organs; outer → inner…
Serosa
-connective tissue, separates and encloses
Muscularis externa
-Myenteric plexus: in between muscle layers and nerve that coordinates contraction
-usually 2 layers of muscle (stomach=3); contract together to create peristalsis
longitudinal: schrunch up and shorten
circular: ring, narrow diameter to break up content
Submucosa
-Submucosal plexus: nervous tissue, controls secretion from mucosal cells
-majority blood and lympathic vessels
Mucosa
-in contact with digestive contents; ex=esophagus
-Muscularis mucosa: anchor point, resistance and strength
-lamina propria
-small vessels
-epithelium: single-layer absorb important things, more layers if mechanical
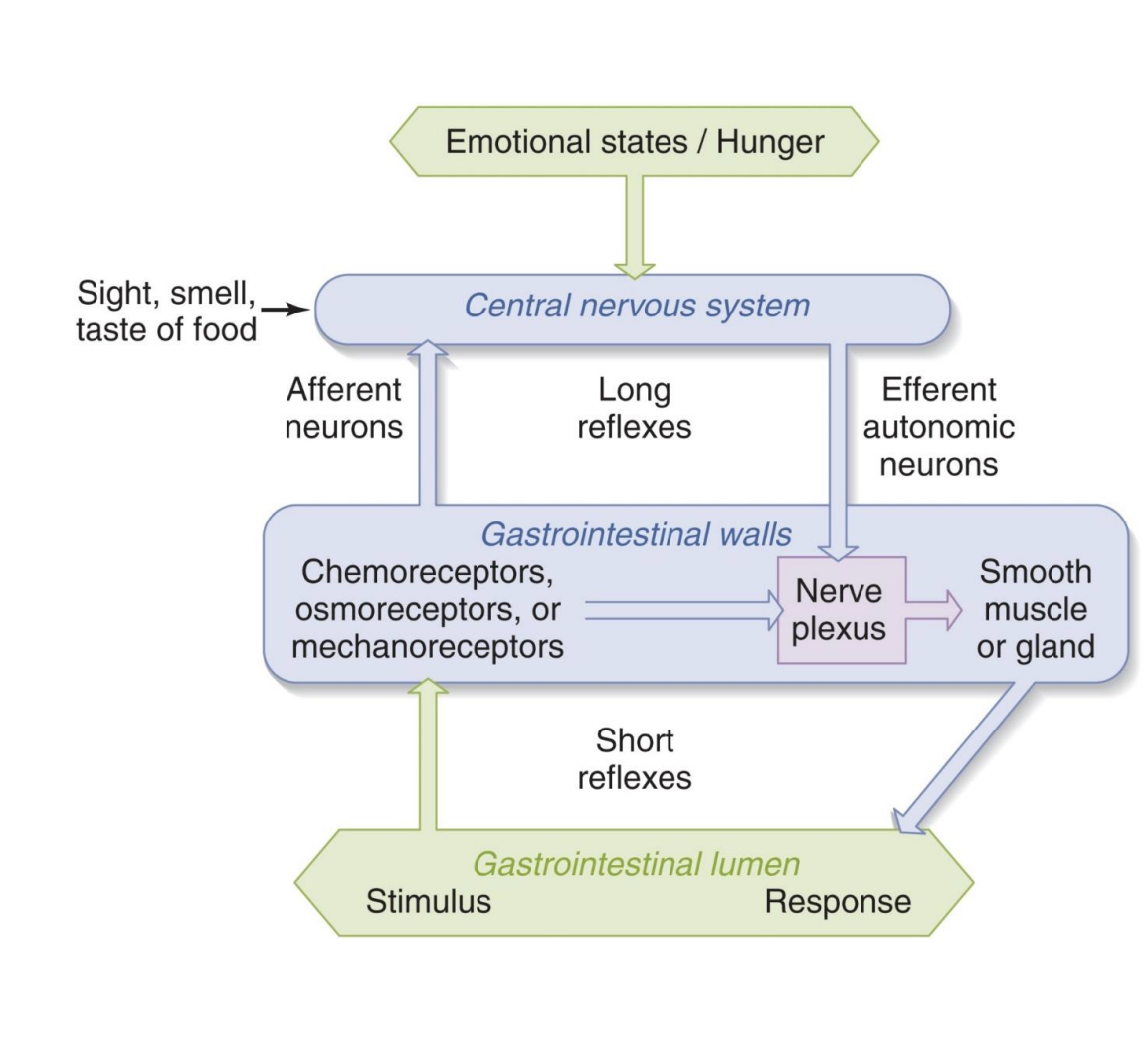
receptors if GI tract + plexuses
Receptors in GI tract can sense:
-Acidity
-Nutrient concentrations
-Distension
Plexuses
-Myenteric plexus neurons: generally stimulate muscle contraction
-Submucosal plexus neurons: generally stimulate glands
*stim=emotional states/hunger; long reflexes=use ANS PSNS; short reflexes=don’t need brain
chewing + saliva
-Chewing: breaks apart food; increases surface area that can be acted upon by acid and digestive enzymes (*mechanical)
Saliva:
-Contains amylase which begins the digestion of starch (*complex carb; most in SI)
-Dissolves food which allows for taste (*tastebuds work in aq envionrment)
-Helps to form a bolus that can be swallowed
*more hydrated so easier to move food bolus
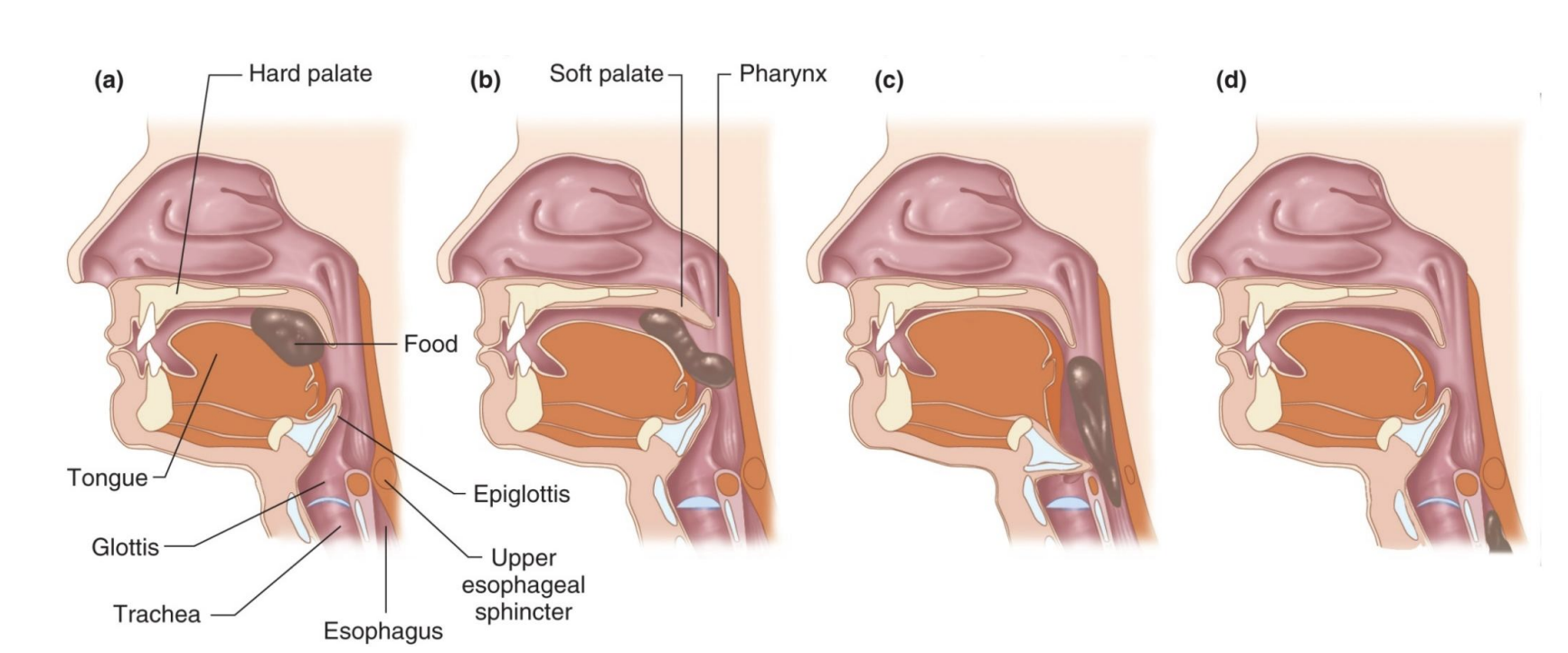
upper and lower esophageal sphincters
-Upper: prevents air from entering esophagus (*bc negative pressure in chest; after trachea)
-Lower: prevents stomach contents from entering esophagus; decline in this function is gastroesophageal reflux
-Swallowing causes relaxation of sphincters
-Peristaltic waves propel food toward stomach – swallowing works even upside down or in zero gravity
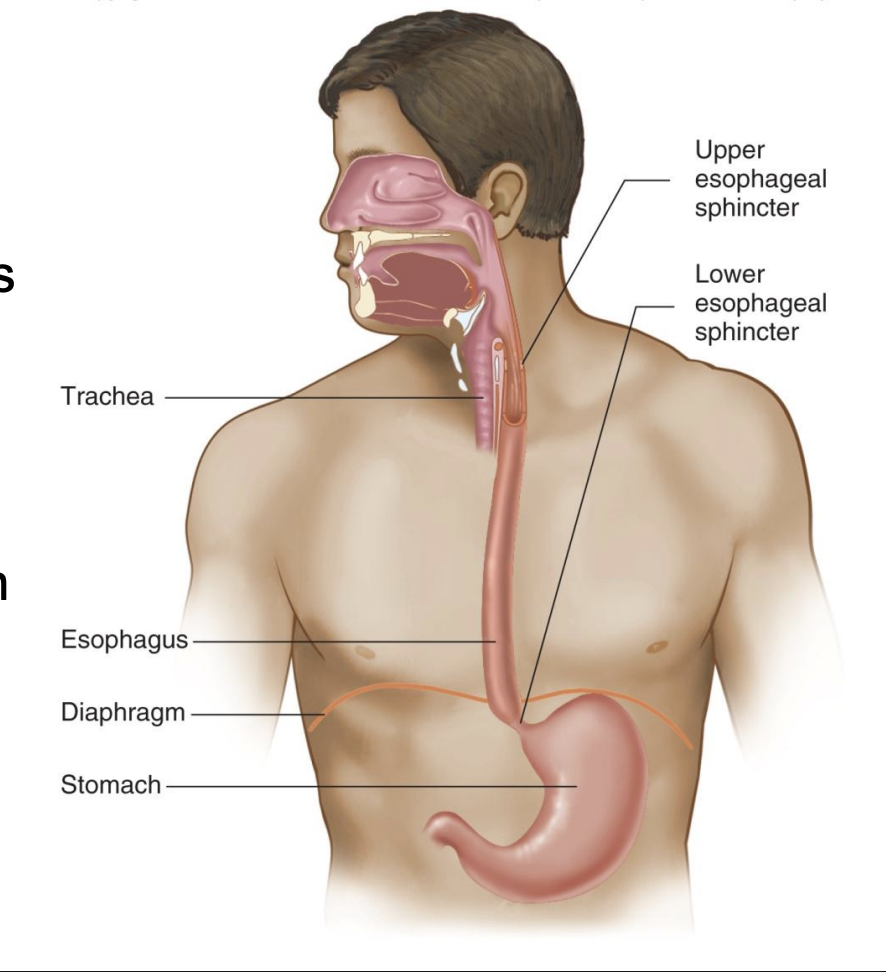
stomach
-High acidity denatures proteins, which makes enzyme sites accessible (*pH ~1-2 bc high HCl)
-Also kills most bacteria
-Stomach is lined with mucus for protection (*bc high acid)
-Peristaltic waves mix and break up food
-Not much absorption: digestion is only beginning to occur; also large volume relative to surface area (*mainly holding and mixing tank)
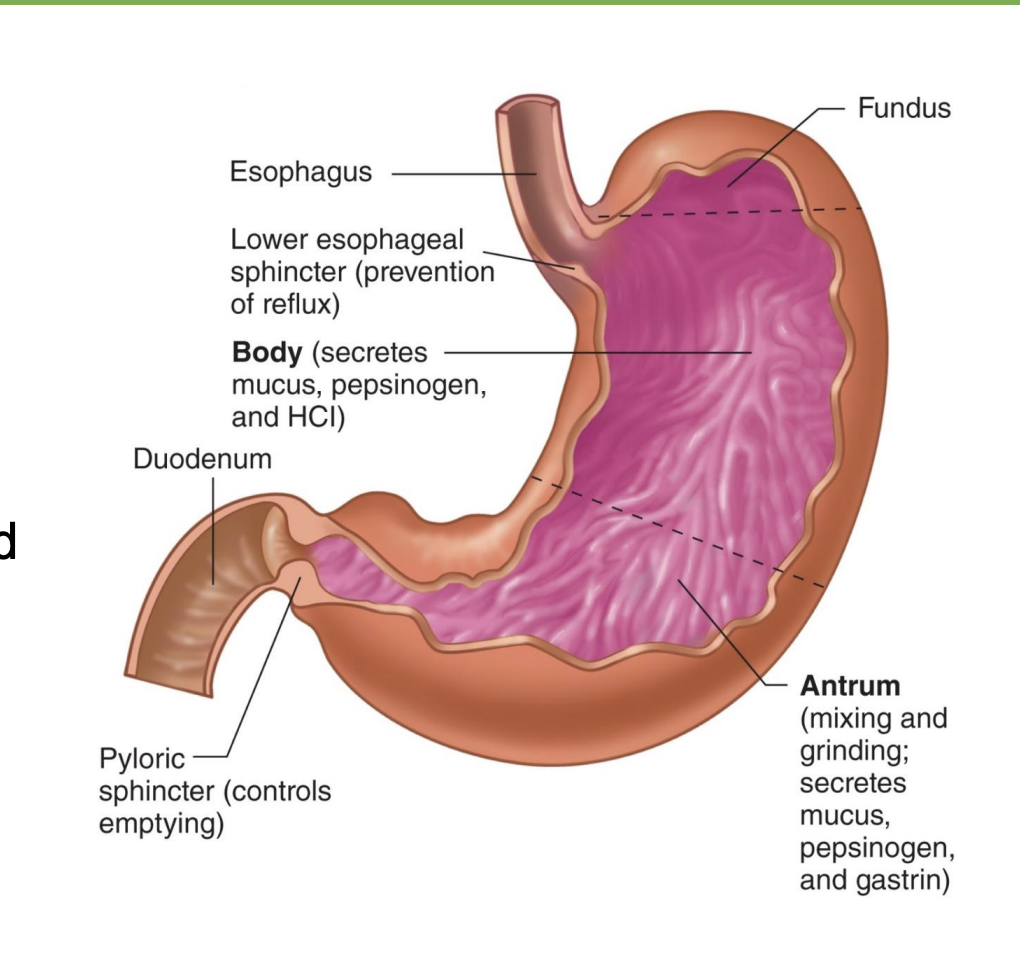
gastric glands cell types
-Parietal cells:
Secrete hydrochloric acid (HCl)
Secrete intrinsic factor that is used for Vitamin B12 absorption
-Chief cells: secrete pepsinogen, precursor form of pepsin (digests proteins)
-G cells: produce gastrin, a hormone (*switch on majors stomach processes)
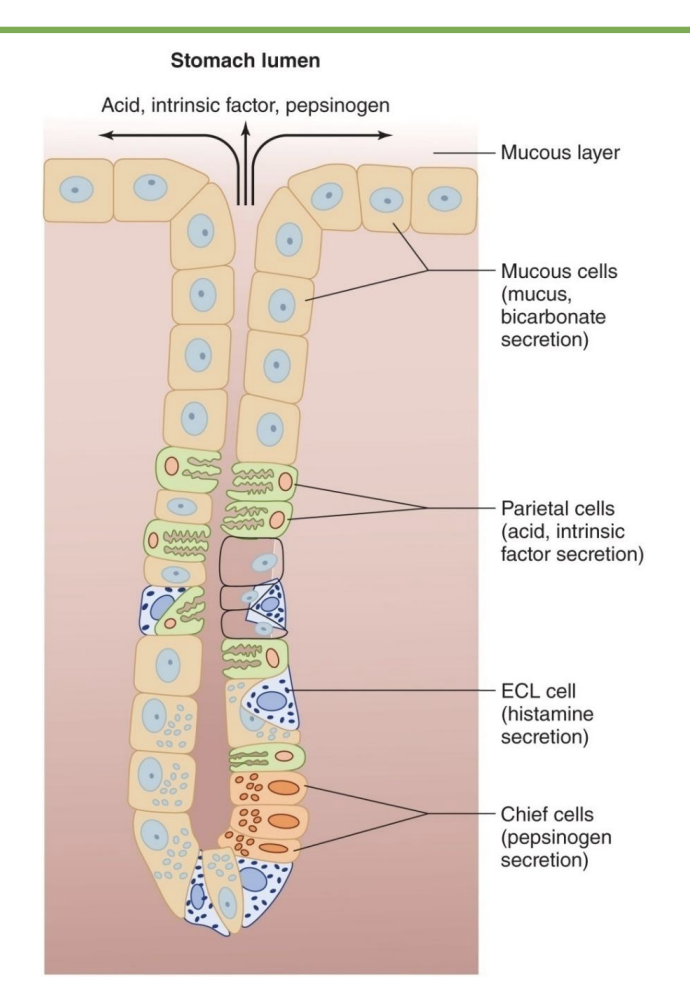
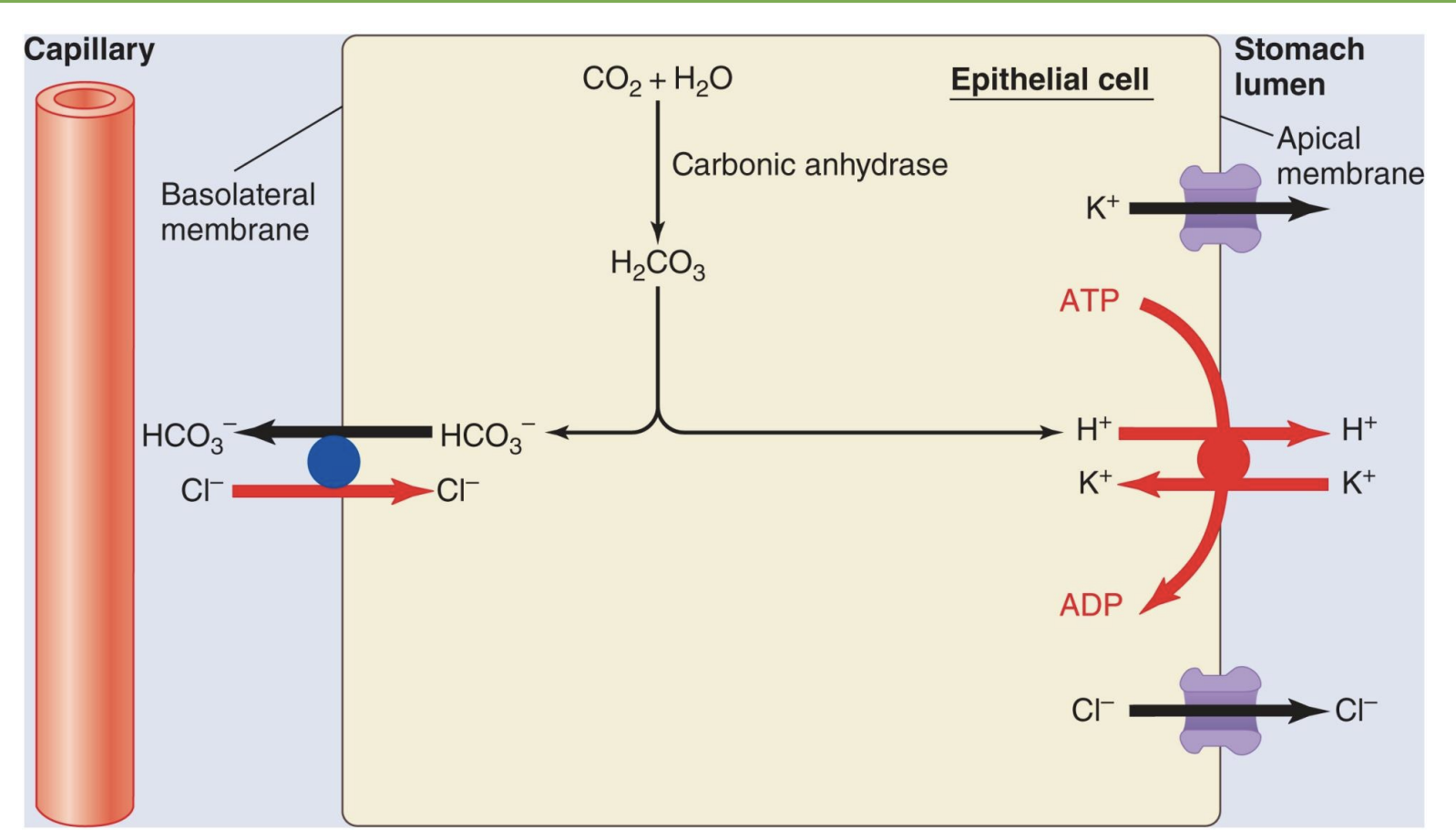
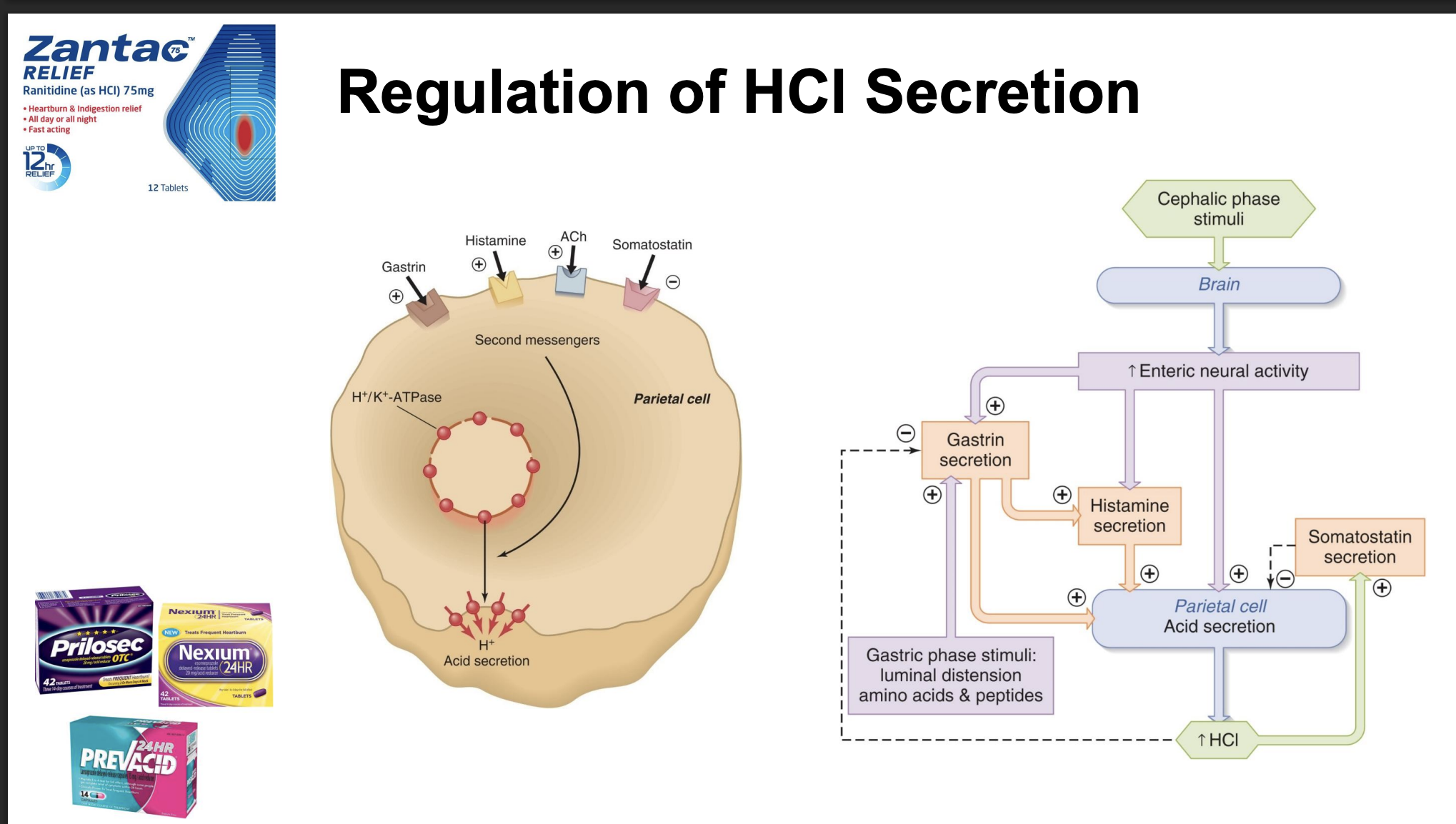
secretion of HCL by parietal cells
*takes energy so use “proton pump”; “proton pump inhibitor” drugs slow down stomach acid secretion
*if vomit a lot, lose acid and increase HCO3- ratio so get alkalosis
*HCO3- out
regulation of HCl secretion
-brain or local reflexes
-stimulus=think about food; increase acid production rate when eating a meal
-gastrin, histamine, ACh: increase acid secretion (common drug to block histamine, not as powerful at decreasing acid secretion as proton pump blocker)
-block H+ acid secretion if proton pump inhibitor
-gastric phase stimuli: food in stomach, local reflex increases H+ secretion and gastrin
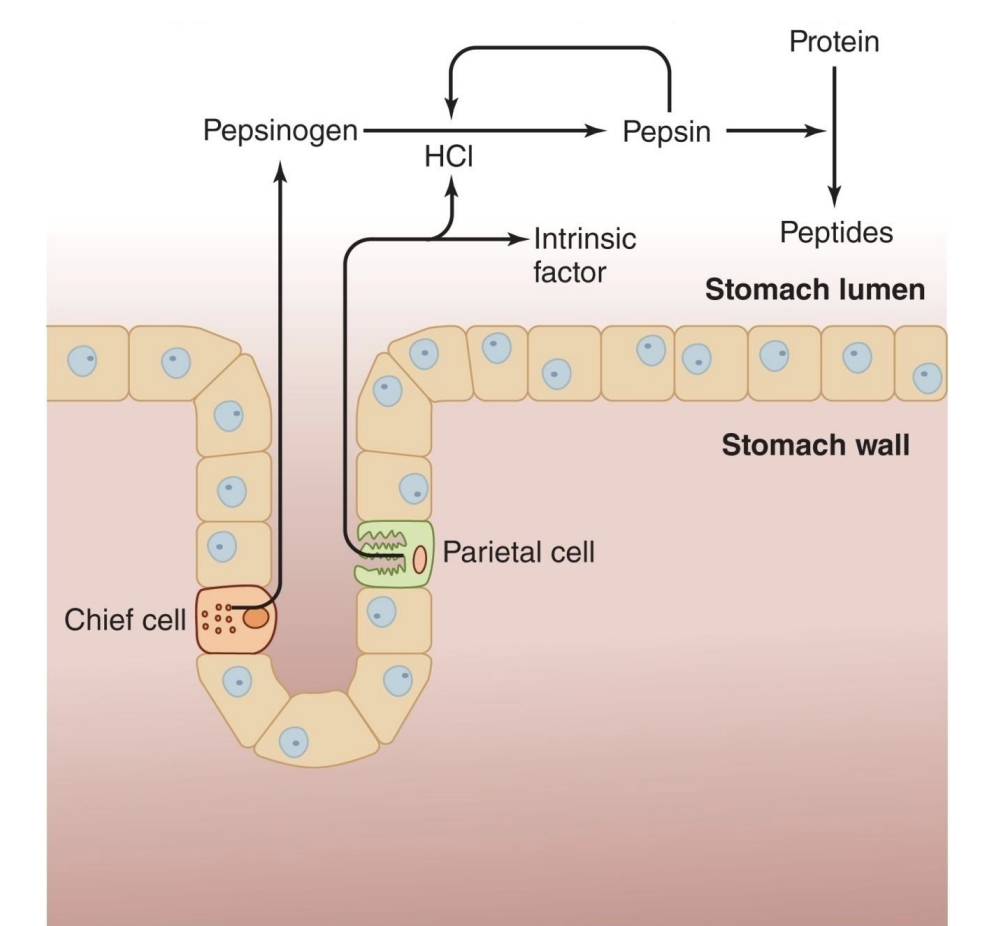
pepsin secretion
-first step of protein digestion, NOT AA but into smaller peptides
-pepsinogen → pepsin; protective so make sure left cell before activate, bc not specific
-chief cell; activate with HCl
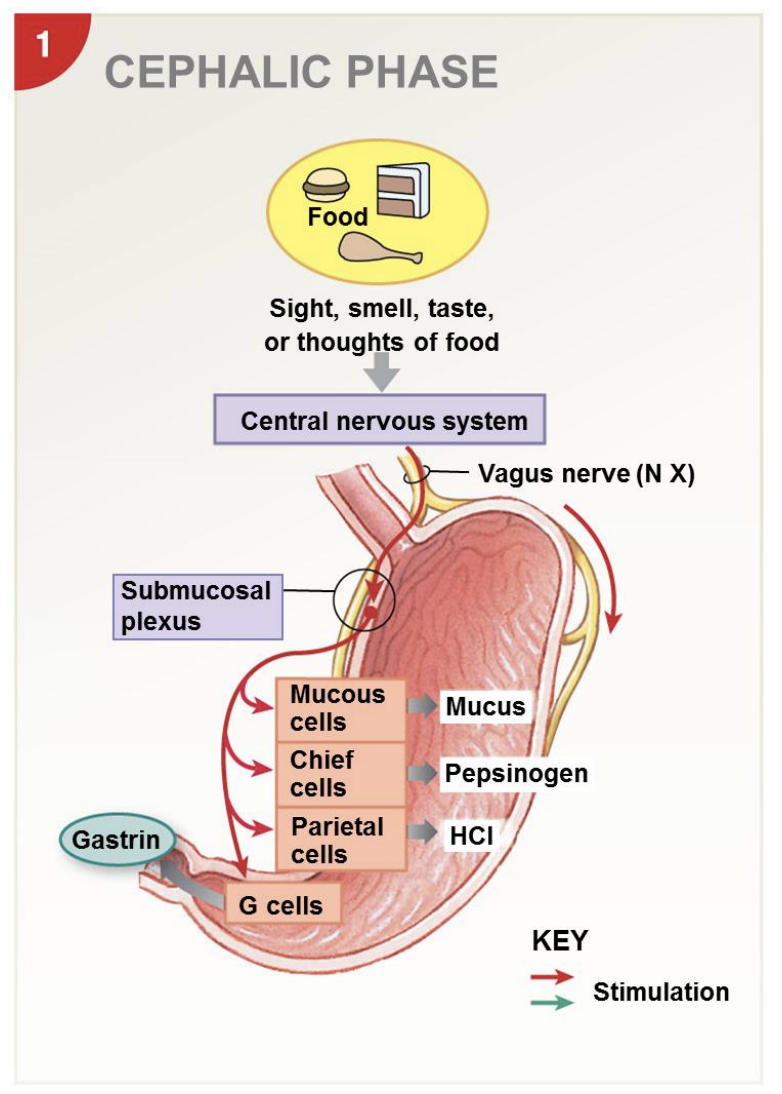
3 stages of stomach digestion: cephalic phase
-controlled and activated by brain; “cephalic”=head; signals from brain
-sight, smell, taste, or thoughts of food
-vagus nerve (CN X)
-get stomach ready for digestion: increase mucus so protected, increase pepsinogen, increase HCl
-gastrin reinforces
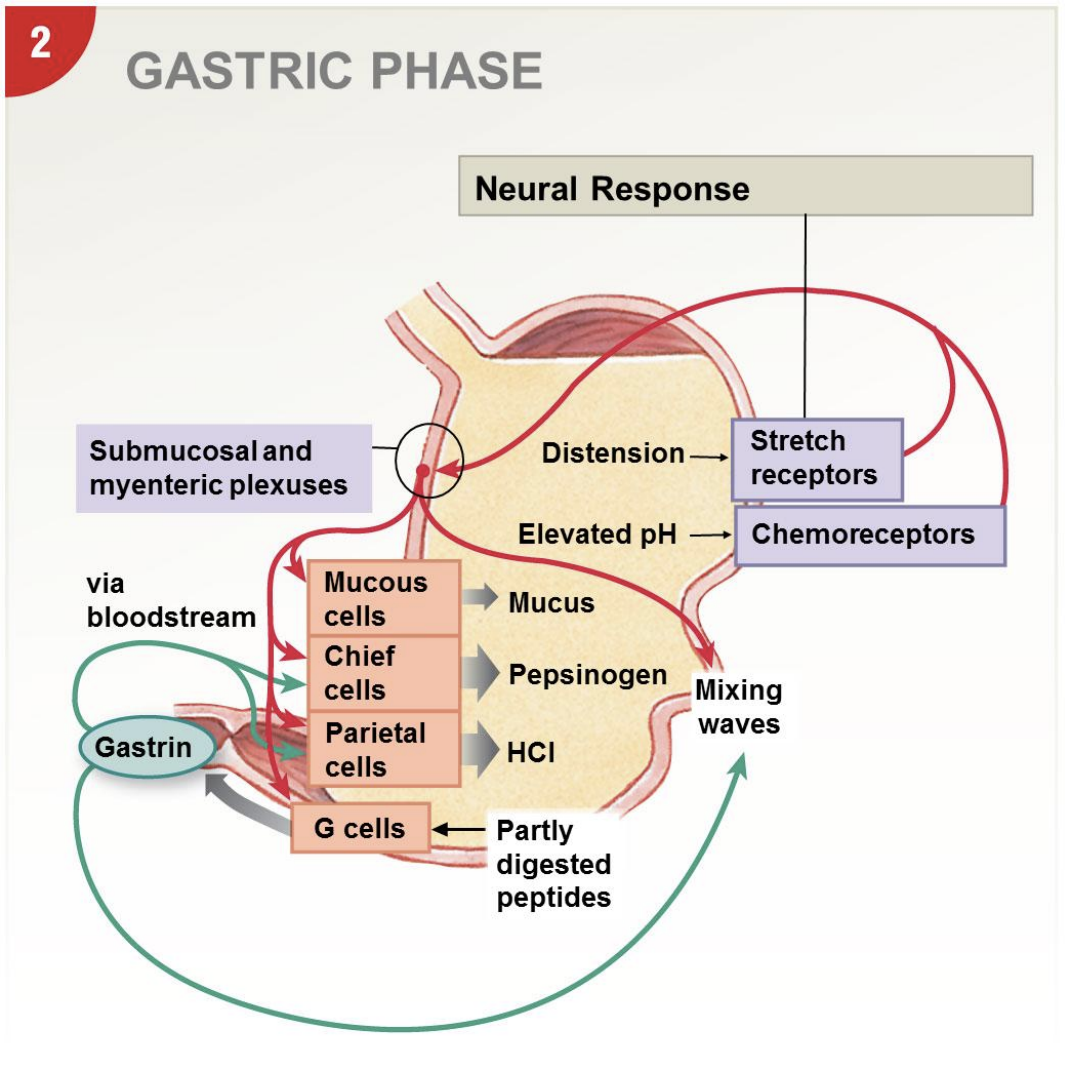
3 stages of stomach digestion: gastric phase
-mainly local reflexes
-stretch receptors, chemoreceptors (detect higher pH, signal production more acid) → stimulate plexuses
-muscle layers contract and create mixing waves; stomach 3 layers, transverse layer further enhance mixing and provide structural support as stretch
3 stages of stomach digestion: intestinal phase
-negative feedback SI to stomach (inhibit upstream); create chyme
-CCK=cholecystokinin: need to shift focus to digestion and signal satiety; brain, pancreas, liver
-hormones inhibit acid, enzymes, and peristalsis
-GIP cause insulin secretion
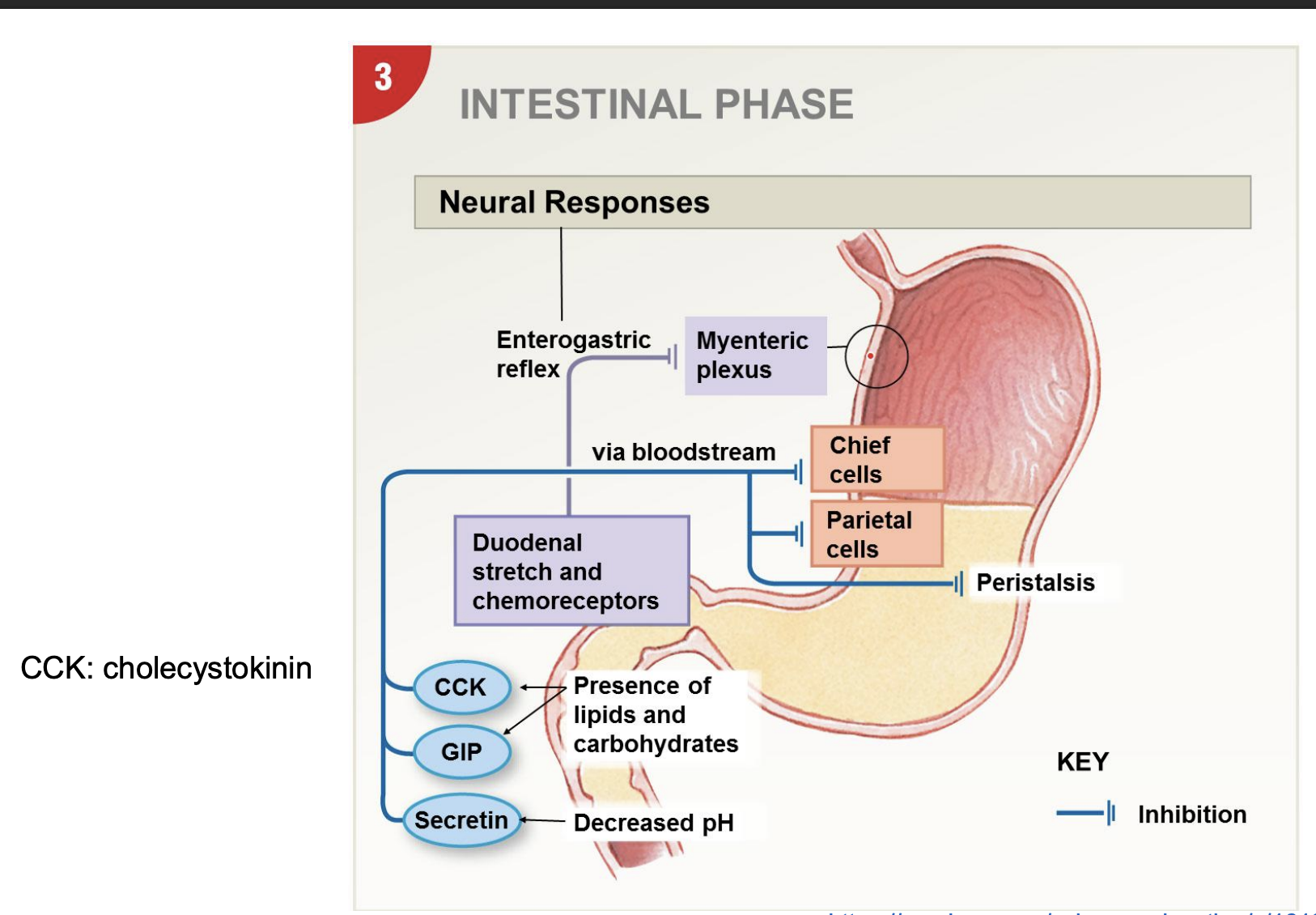
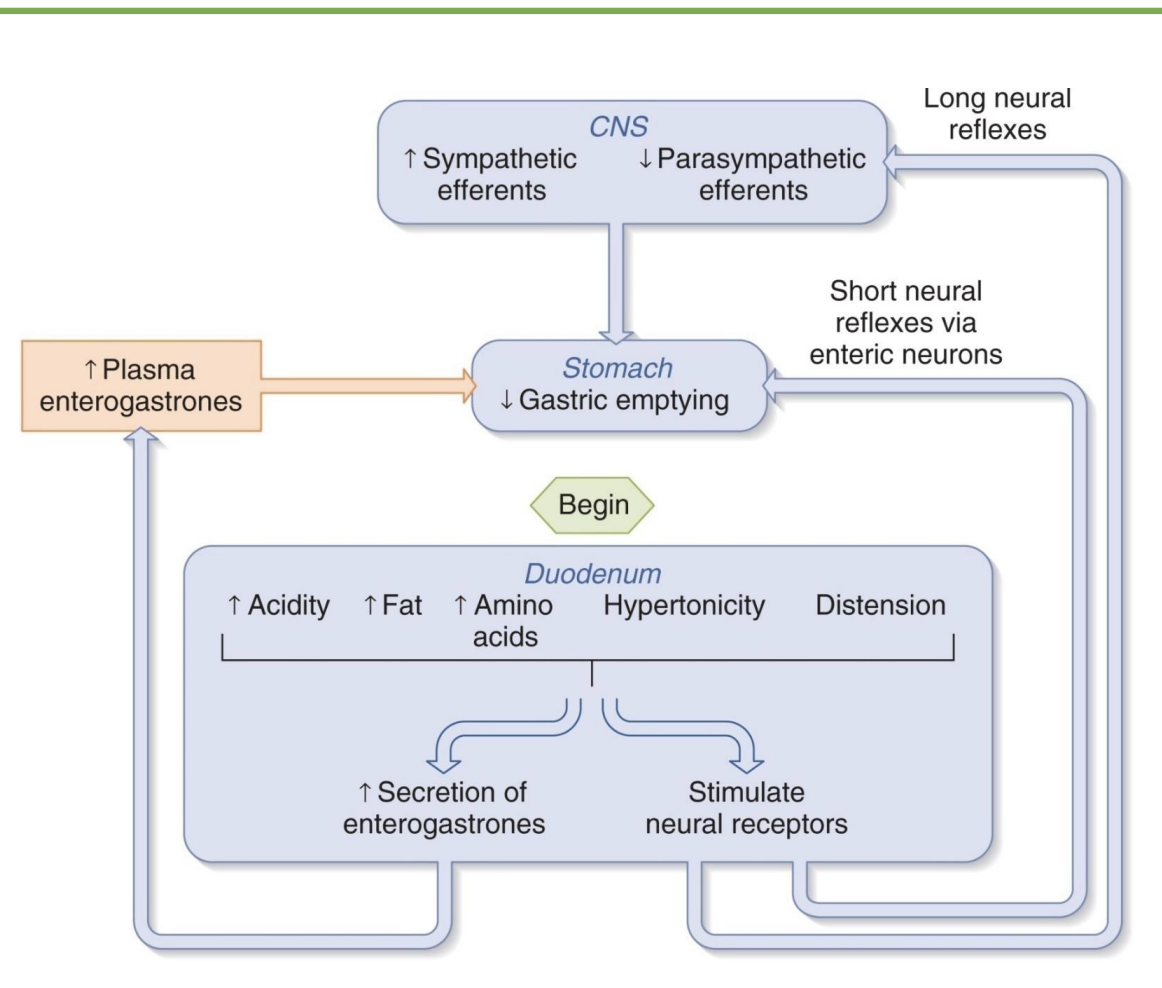
regulation of gastric emptying
-slow down stomach to tell brain full
-enterogastrones: intestinal hormones that signal stomach and intestine
small intestine segments
-Duodenum: first ~25cm (*mix chyme from stomach, bile from liver, and pancreatic secretions)
-Jejunum: longest segment, majority of absorption
-Ileum: third segment, normally most absorption completed by this point
*all 3 designed to be efficient and capture most nutrients
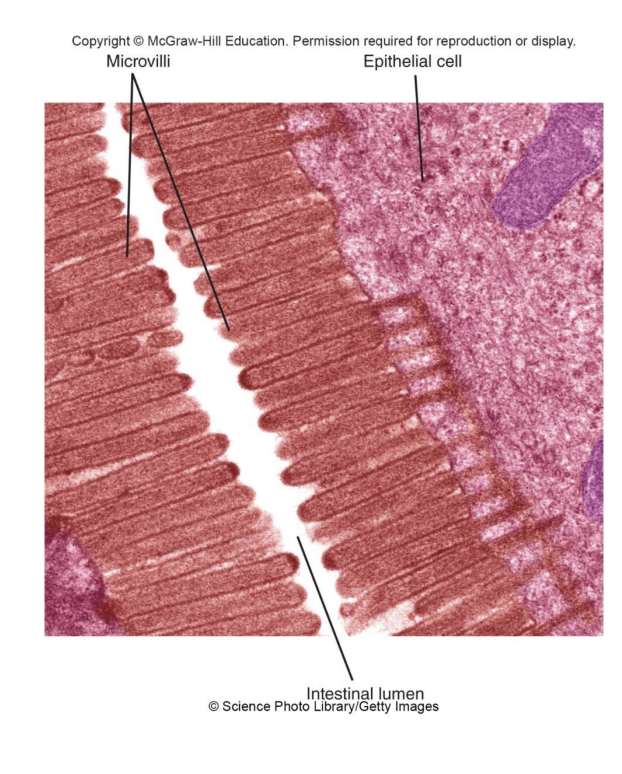
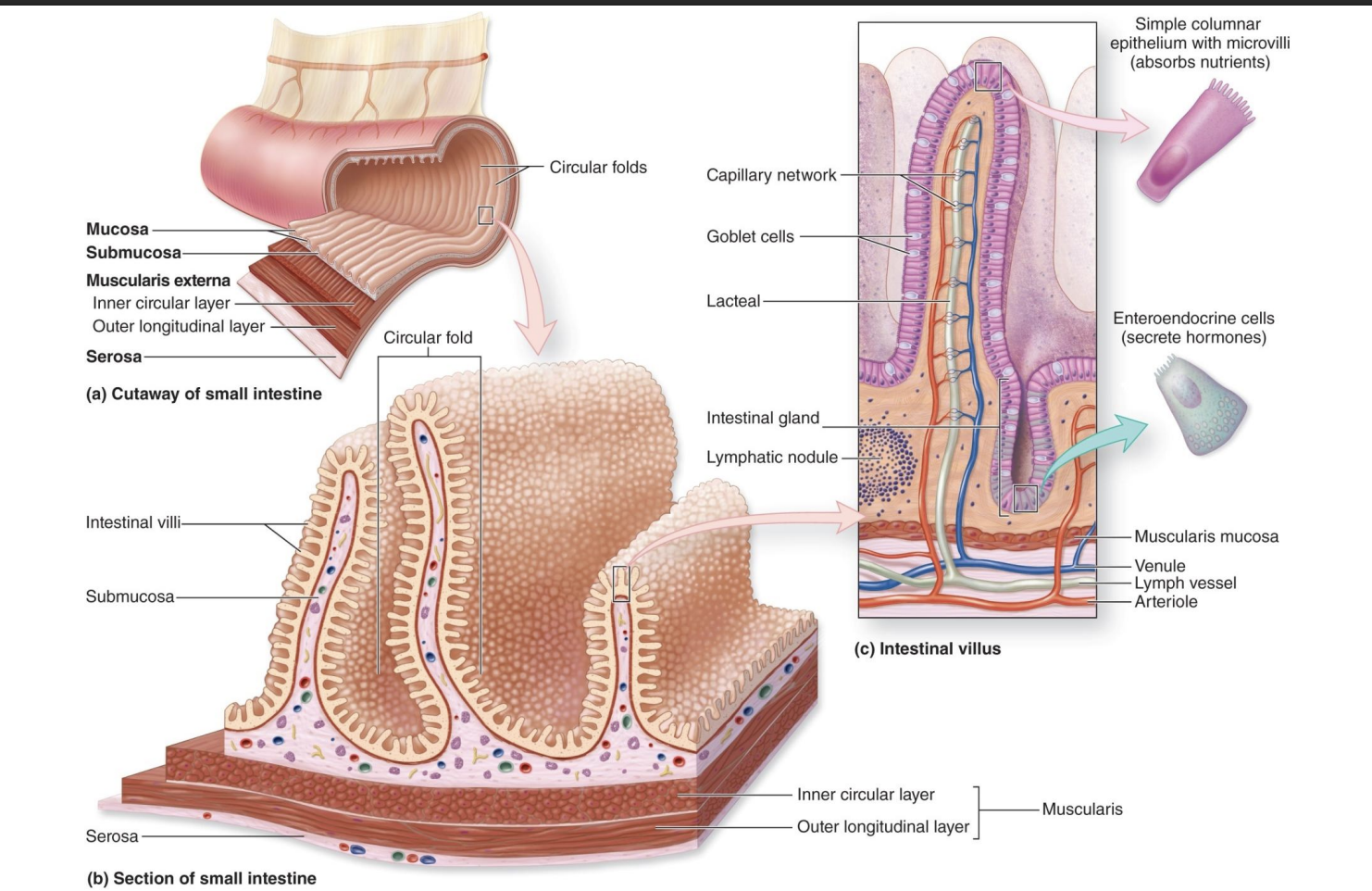
structure of SI
long length, and high SA bc of structural adaptions…
-Circular folds: largest; not smooth and creates turbulent flow so mix things around
-Villi: finger-life projections
-Microvilli: smallest; mediate absorption
_______________________________________________________________________________
-Lacteal: lympathic vessels, absorb lymphatic fats
-Goblet cells: mucous
-Capillary network: absorb other stuff
-simple columnar epithelium: mediate absorption
-enteroendorcine cells: secrete hormones
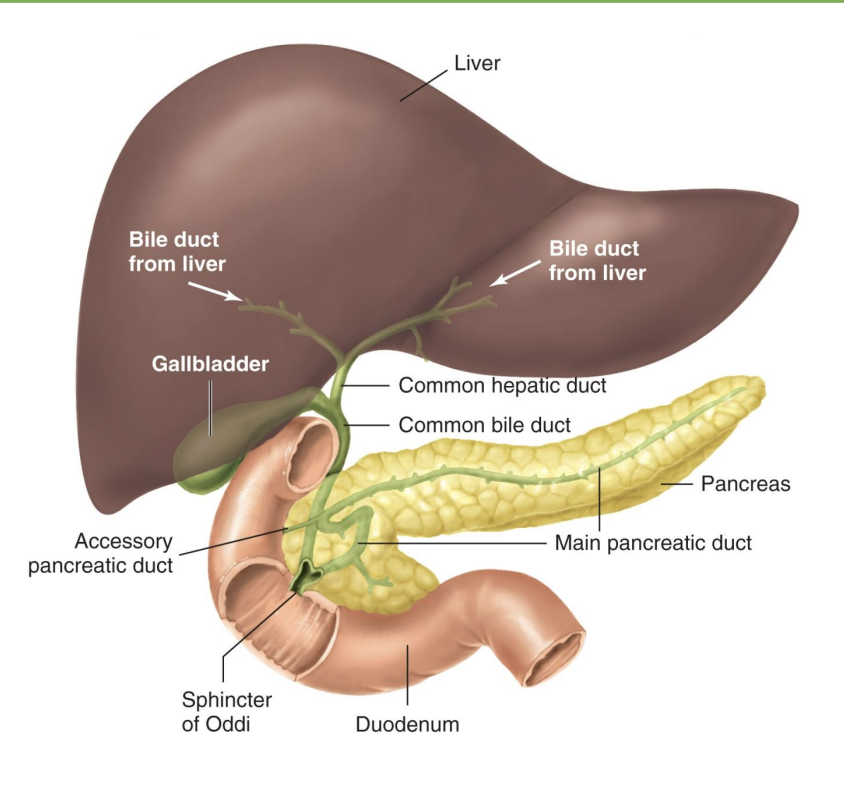
where do the liver, gallbladder, and pancreas all meet?
-Duodenum is a “mixing bowl” for chyme and secretions from liver, pancreas
*gallbladder: stores bile
*common bile duct
*pancreas: endocrine (ex=insulin) and exocrine (=digestion)
*sphincter of Oddi/Hepatopancreatic sphincter: liver and pancreas → SI
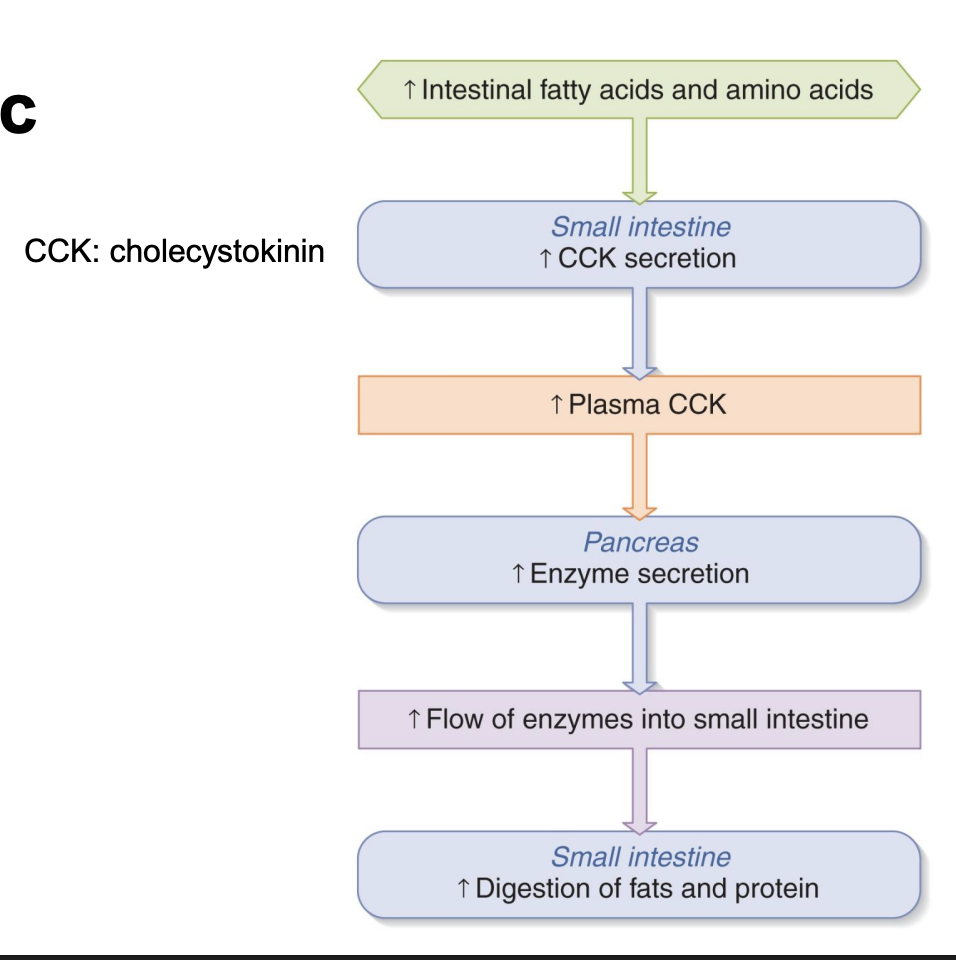
control of pancreatic enzyme secretion
-slow down stomach and release bile and pancrease secretions
-stimuli=chyme, chemoreceptor
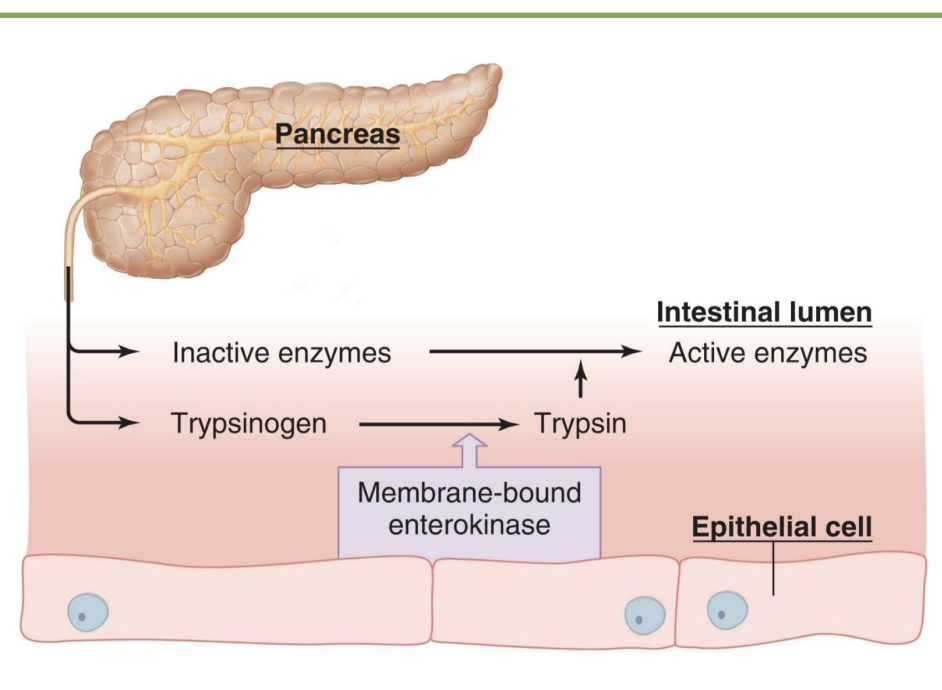
pancreatic enzymes
-Pancreas secretes enzymes that digest the major classes of molecules in food: carbohydrates, fats, proteins, nucleic acids (DNA/RNA)
-Many pancreatic enzymes are activated once they reach the lumen of the small intestine
-Brush-border enzymes: produced by intestinal epithelial cells; activate pancreatic enzymes and perform digestion (*final stage of digestion)
pancreatic amylase=starch
lipase=fats
protease=protein (*ex=enterokinase)
nucleas=nucleic acids
*before: salivary amylase and pepsin, so relatively undigested; proteins and carbs complex, lipid digestion more simple
different brush border enzymes (enzyme, location, substrate)
-Pepsin: stomach, protein
-Amylse: saliva or pancreas, starch
ex: startch → (amaylse) → matlose/2xglucose → (maltase) → glucose
-Proteases: pancreas brush border, protein
-Lipase: pancrease, fat
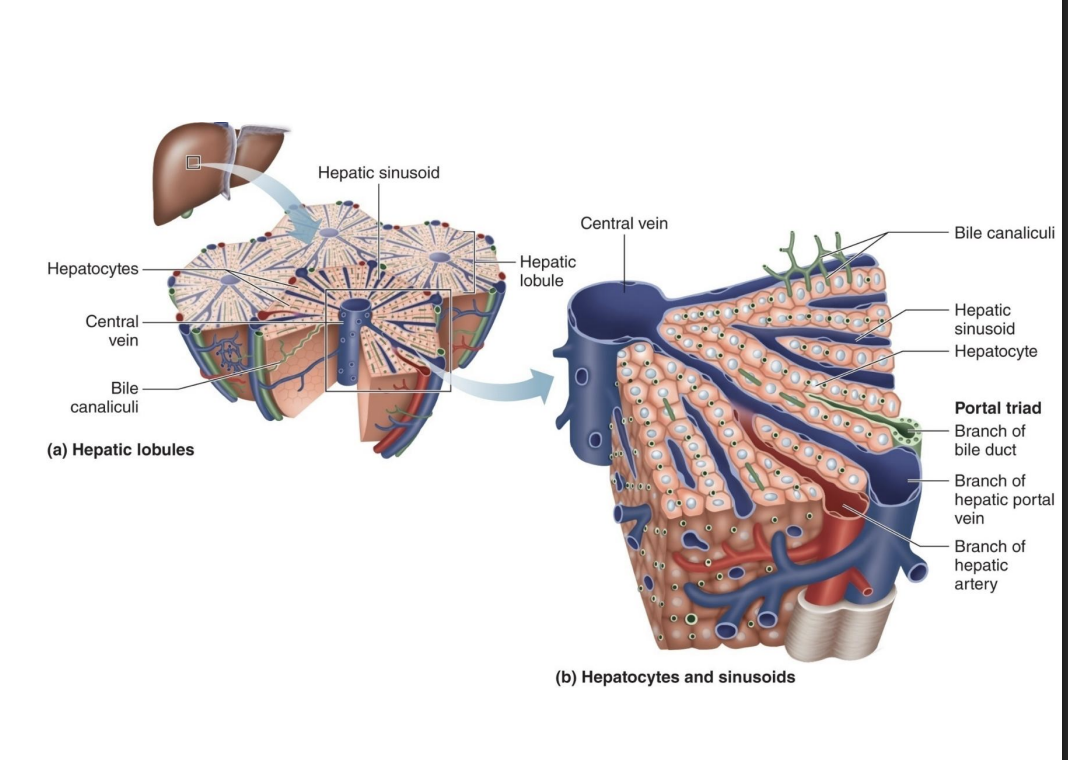
liver structure and function
-Most significant digestive function is bile production
-Bile aids in digestion by emulsifying fats (*break apart globs of fat)
-Bile also serves as a path for excretion of metabolic waste and excess cholesterol through the feces (*that can’t be filtered by kidneys easily)
enterohepatic circulation of bile salts
-bile salts intestine → hepatic portal vein + hepatic artery → liver → bile duct
-recycle bile salts, only 5% lost in feces; bile salts made of cholesterole
-liver: processes nutrients and detoxes; control regulation of nutrients and metabolism
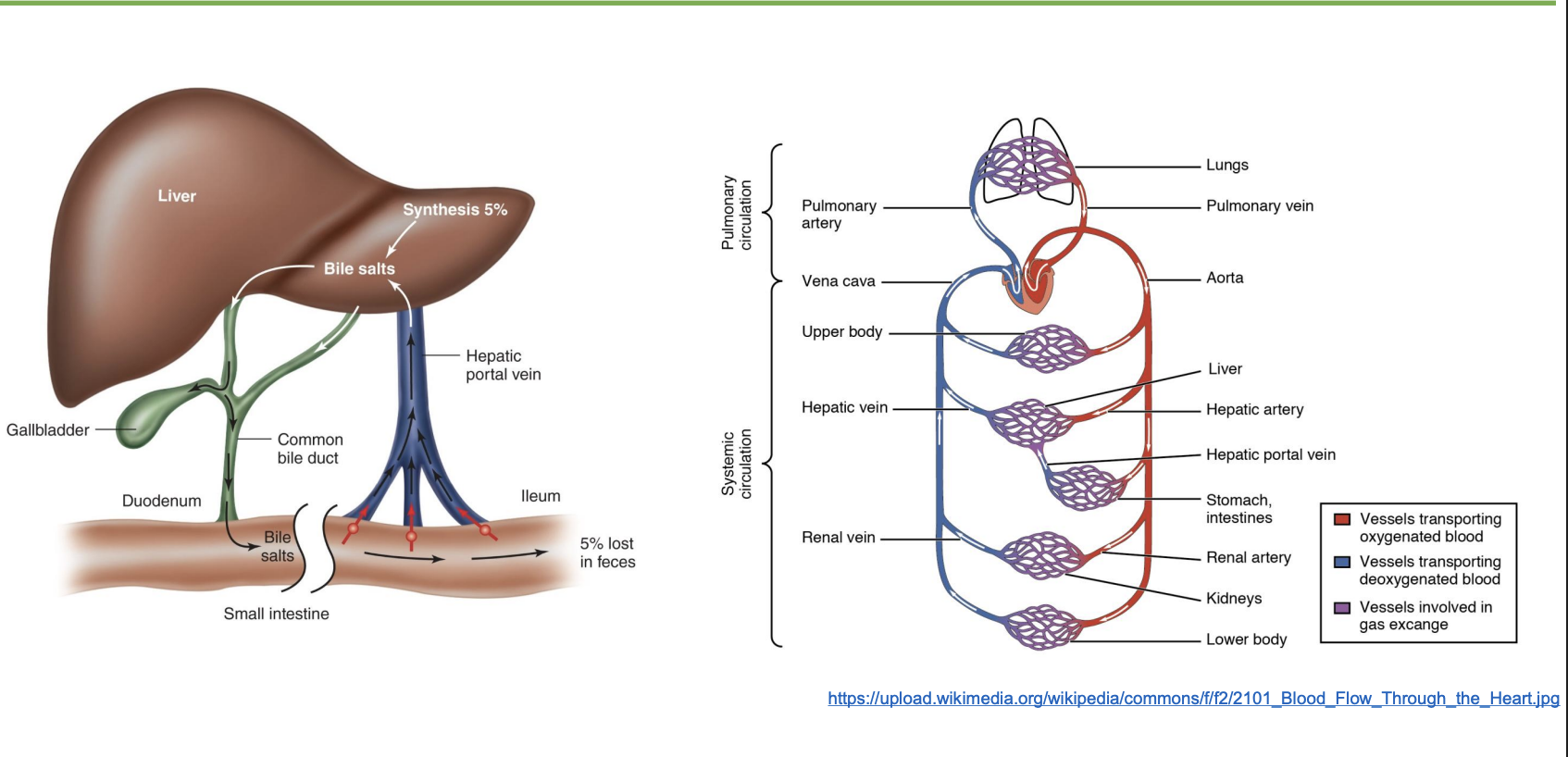
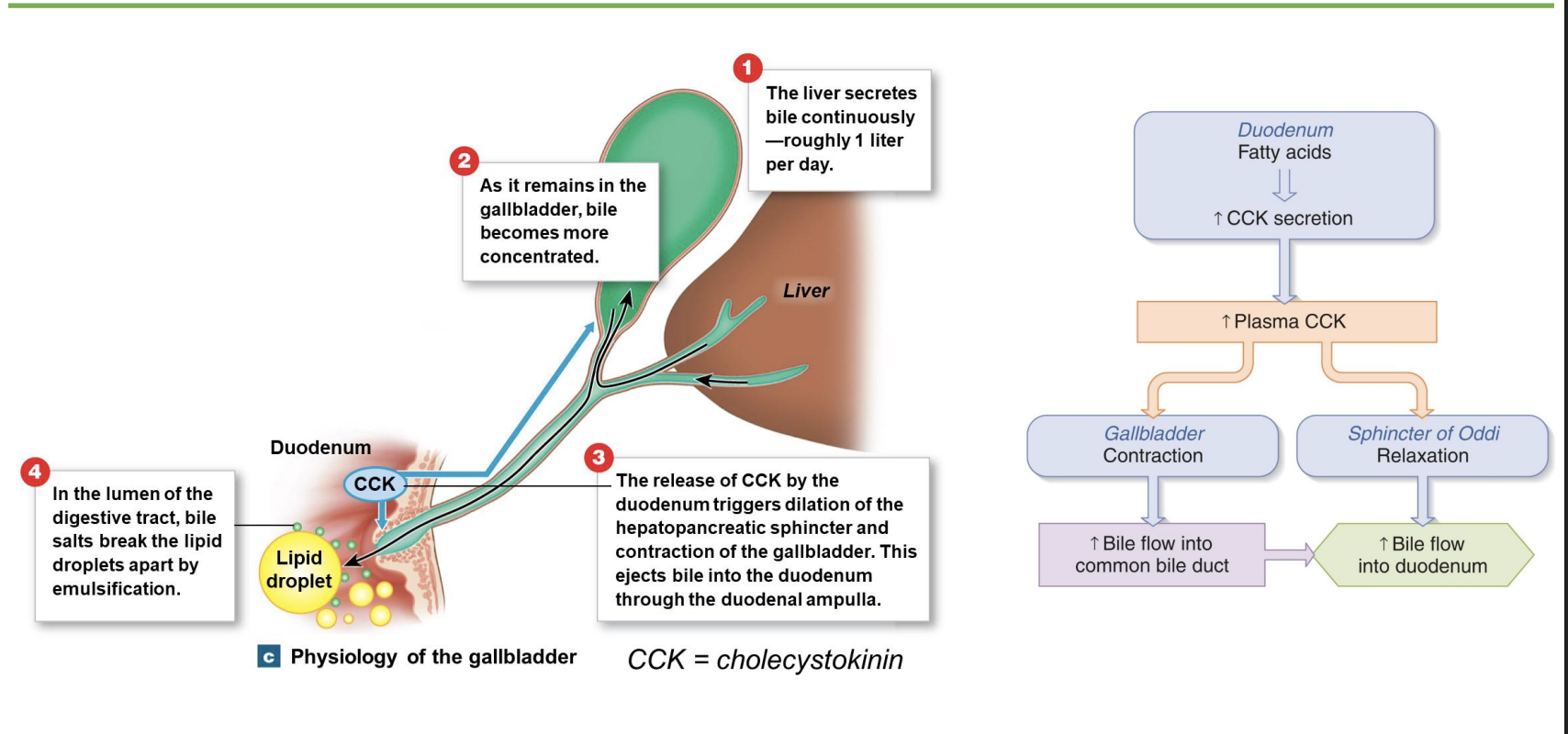
regulation of bile flow + gallstones
-liver secretes bile continuously but espically when lot of fat; CCK when feed/fat in SI; can constrict so bile goes to gallbladder
-gallstone: salts in bile percipiate out; “gallbladder attack” bc increase CCK signal and increase contraction of gallbladder
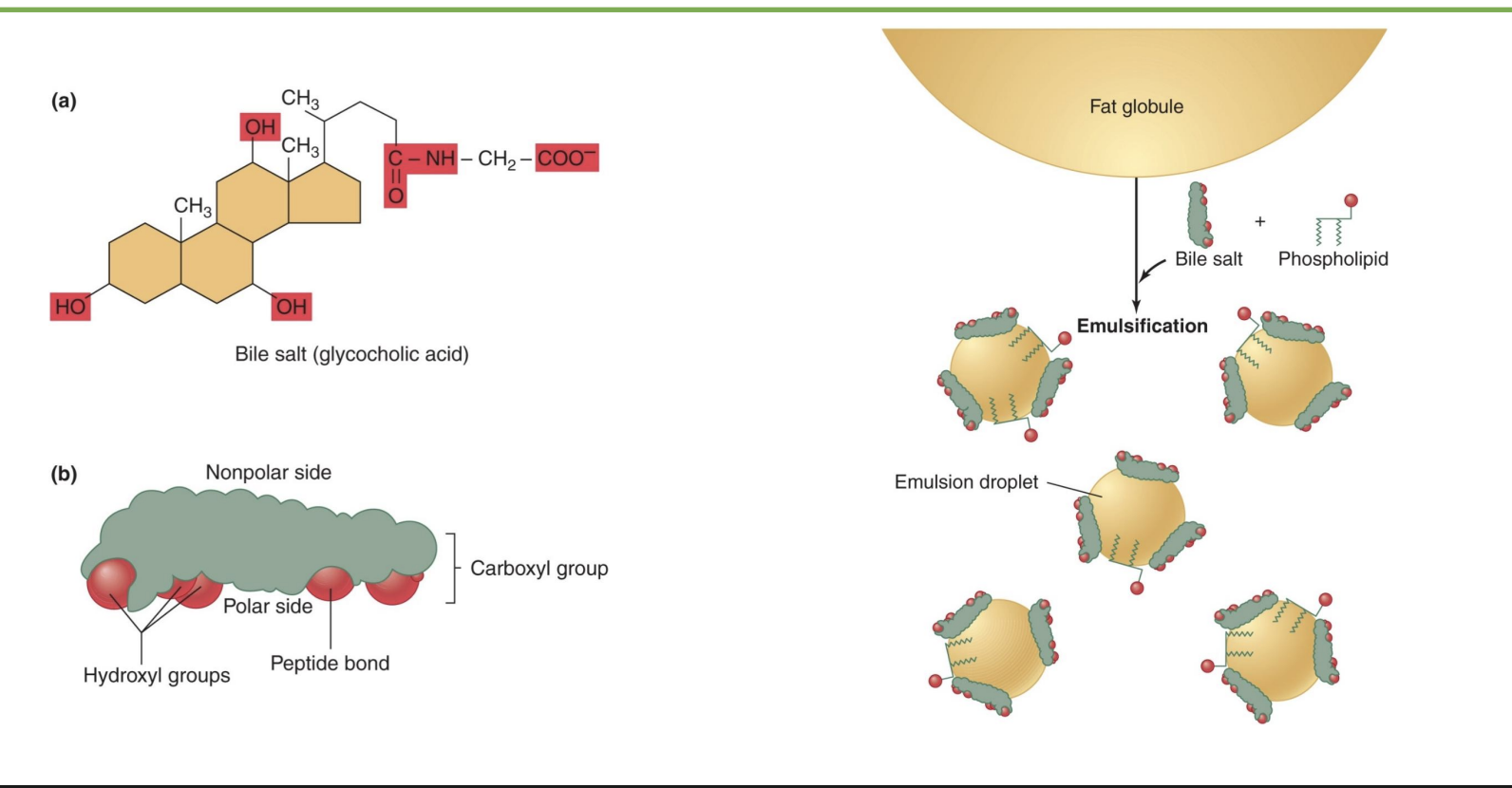
bile sal
-bile’s 4-ring structure looks similar to cholesterol
-nonpolar side inward and polar side outwards
-phopholid lipid helps bile salt emuslify fat so get emulsification droplet
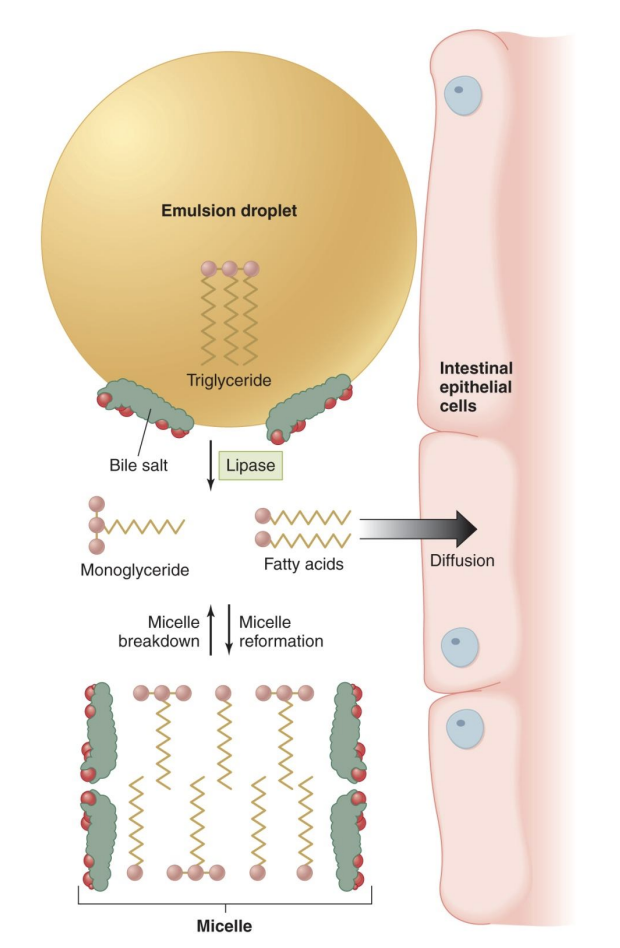
fat digestion and absorption
triglycerides → (lipase) → FFA → rebuild triglyceride in cells
carbohydrates
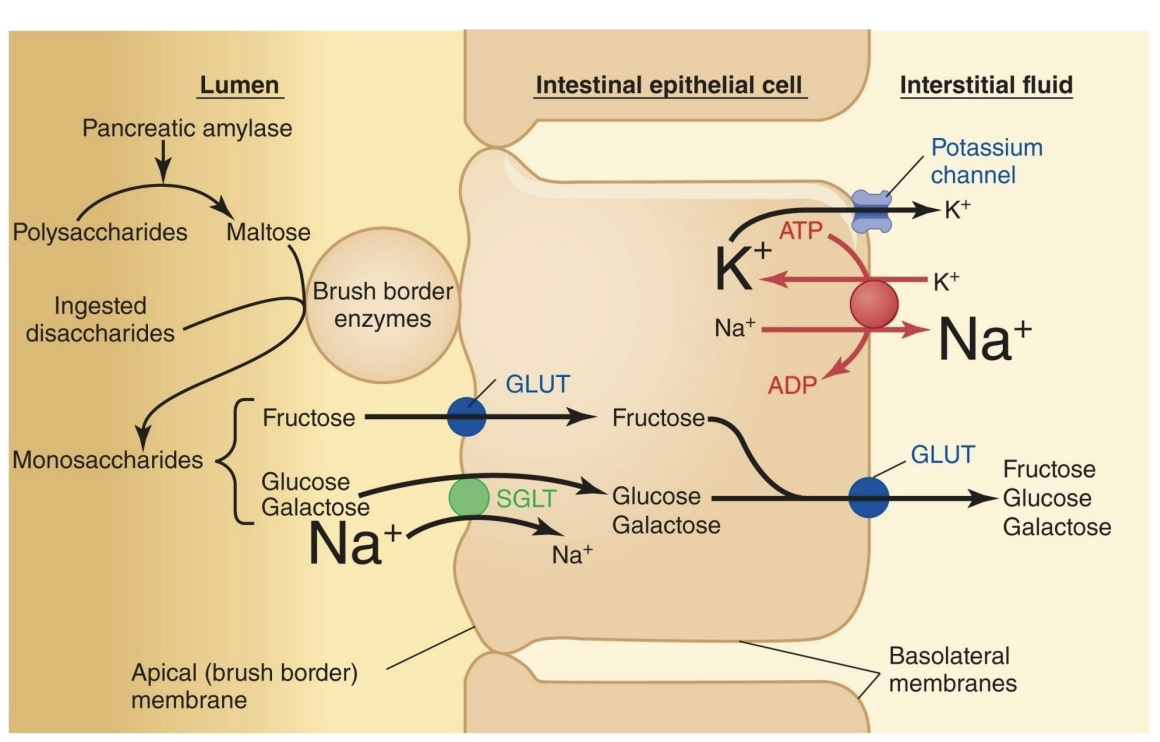
-Most carbohydrates in the diet are consumed as disaccharides or polysaccharides: Sucrose (table surgar), Lactose (dairy), Maltose (2 glucose, intermediate startch breakdown), Starch (plant, long-chain glucose), Glycogen (animal, long-chain glucose), Cellulose (non-digestible carb, dietary fiber)
-Only monosaccharides are absorbed by the intestinal cells for use in the body (*glucose, lactose, galactose)
-Disaccharides and polysaccharides must be digested to monosaccharides before they can be absorbed
carb digestion and absorption
startch → (pancreatic amylase) → maltose → (BBE maltase) → monosaccharides → dif transporters (SGLT active transport using Na+)
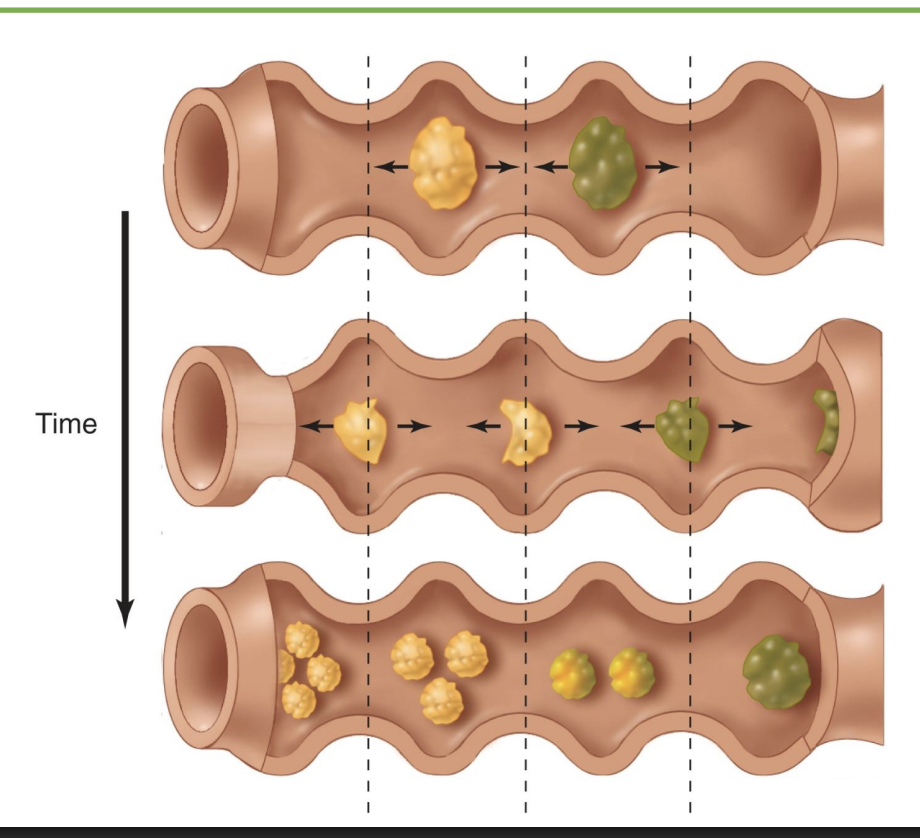
segmentation
-coordinated contraction from myenteric plexus
-mix stuff
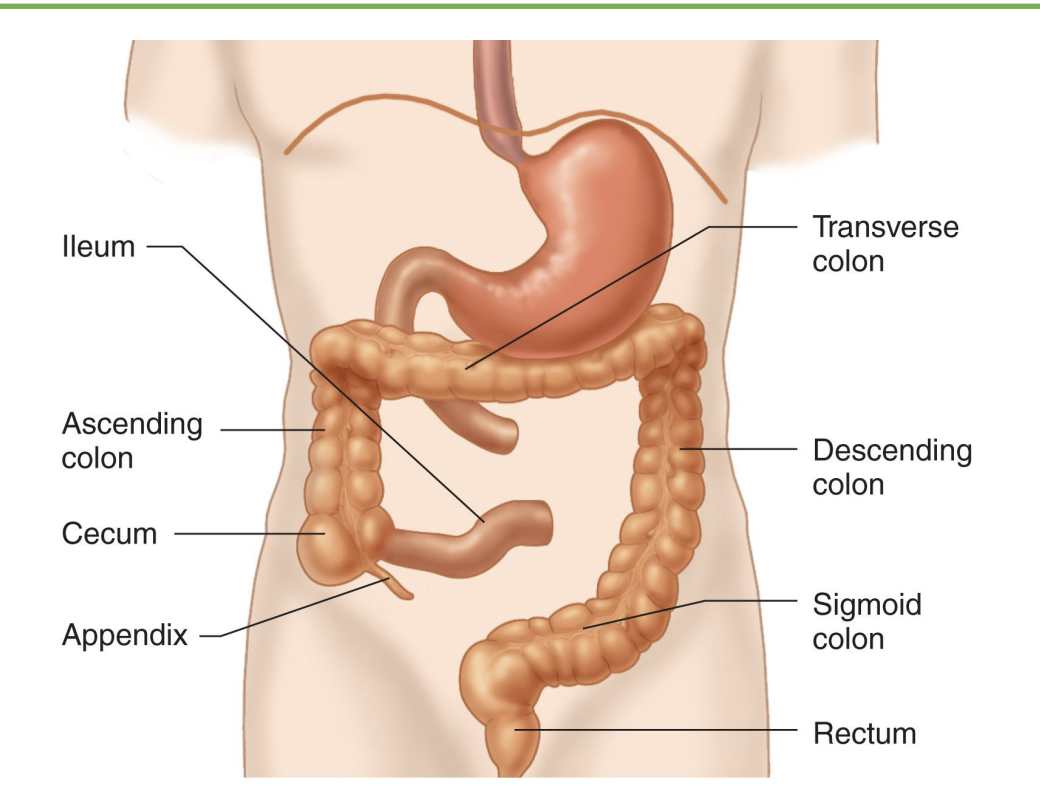
large intestine: anatomy
-ascending, transverse, descending, sigmoid: absorb
-rectum: store fecal
absorption in the large intestine
-Less than 10% of total nutrient absorption (*less than SI)
-Reabsorption of water: reduces about 1500 ml of material down to 200 ml
-Reabsorption of bile salts
-Absorption of vitamins produced by bacteria, most significant is vitamin K (*bacteria also make FFA)
*”large” bc bigger diameter
composition of feces + why color and smell
-75% water, 5% bacteria
-Remainder is indigestible material (e.g. fiber), and dead epithelial cells
epithelial cells have short lifespans so undergo constant renewable cycle
-Color due to urobilins and stercobilins – pigments that are bilirubin metabolites (*waste products that give brown/yellow colors; bilirubin=old RBC and Hb, if build-up=gnondis)
-Smell is mainly due to compounds produced by bacteria (e.g. hydrogen sulfide, which smells like rotten eggs)
Movements of material through the GI tract: different reflexes
-Gastroileal reflex: opens ileocecal valve in response to stretch in stomach (*between SI and LI)
-Stretch also causes mass movements, powerful peristaltic contractions that move material through the colon (gastrocolic reflex) (*why a meal triggers bowel movement)
-Defecation reflex triggered by stretch in rectum