FSHN 3620 Exam 2
1/79
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
80 Terms
what are the benefits of breastfeeding for the baby?
helps build strong immune system - contains antibodies and WBCs
lowers risk for many diseases
lowers hospitalization rate and doctors visits
lowers infant mortality rate
increased cognitive ability
analgesic effects
healthy weight gain
changes in composition to meet baby’s nutritional needs over time
what are the benefits of breastfeeding for the mother?
lowers risk of disease (cancer, T2D, CVD)
quicker recovery from childbirth - oxytocin helps uterus return to normal size, reduces bleeding
increases physical and emotional bonding
establishes trust
gives mother self-confidence
may help lose weight
what specific diseases/health issues does breastfeeding lower the risk of for the mother?
cancer (breast, ovarian, endometrial, thyroid)
osteoporosis
type 2 diabetes
CVD
postpartum depression
high BP
high cholesterol
why is breastmilk said to be isosmotic?
it has the same osmotic pressure as the baby’s blood and body fluids, which ensures ideal hydration
breastmilk is ___ in protein and ___ in lipids
(low/high?)
LOW in protein - so baby’s kidneys are not overloaded
HIGH in lipids - to meet essential fatty acid needs
what are HMOs?
human milk oligosaccharides: complex sugars that act as prebiotics to nourish the baby’s gut bacteria
e.g. the Bifidious factor selectively nourish Bifidobacterium in the baby’s gut, which is crucial for immune development and reduce infection risk
what is lactogenesis?
human milk production
what are the stages of lactogenesis?
Lactogenesis I: milk formation begins last trimester of pregnancy at ~16 weeks through the first days postpartum
Lactogenesis II: 3-8 days postpartum - milk comes in
Lactogenesis III: 9 days postpartum, milk supply and composition become stable
what are the names for the different types of breastmilk in each stage of lactogenesis?
lactogenesis I = colostrum
lactogenesis II = transitional milk
lactogenesis III = mature milk
what is the composition of colostrum?
in comparison to human milk (produced over 2 weeks after birth):
higher concentrations of nutrients: sodium, potassium, vitamin E
higher in proteins and minerals
higher in vitamin A
primary proteins: secretory immunoglobin A and lactoferrin
lower in carbohydrate, fat, vitamins
what is the major component of human milk?
water (major) and energy (0.65-0.75 kcal/mL)
what is the second largest component of human breast milk?
lipids provide half the calories of human milk, but fat content can vary from mother to mother
what especially important lipids for development are present in human milk?
DHA: essential for retinal development - impacted by maternal diet
Cholesterol: needed for growth and replication of cells - not impacted by maternal diet
what is hindmilk? what has a higher fat content - hindmilk or foremilk?
hindmilk - milk expressed at end of feeding
has higher fat content than foremilk

does breastmilk change over time?
yes, it changes over a single feeding, over a day, based on infant age, presence of infection, or maternal nutrition status. It changes to meet the specific nutritional needs of the infant for a given time.
what is the dominant carbohydrate in human milk?
lactose. it enhances calcium absorption
what fat-soluble vitamin does colostrum have in significantly high amounts?
colostrum has twice the concentration of vitamin A compared to mature milk
what is the role of vitamin D?
calcium absorption and bone mineralization
what is the role of vitamin E?
potent antioxidant that protects cells
why is vitamin K so important?
it supports development of clotting factors to prevent bleeding in newborn infnats
what category of vitamins are reflected by a mother’s diet and supplementation?
water-soluble vitamins
what minerals are high in bioavailability in breast milk?
magnesium, calcium, iron, zinc
despite low iron content of milk, exclusively breastfed infants have a LOW/HIGH risk of anemia
low
what are the functional units of the mammary gland?
alveoli: rounded or oblong-shaped cavity in breast
secretory cells: secrete milk
myoepithelial cells: surround secretory cells, responsible for milk ejection into ducts
what does prolactin do?
stimulated by suckling, it stimulates milk production
what does oxytocin do?
responsible for ejection of milk, and is stimulated by nipple stimulation or suckling
also acts on uterus around delivery time
what is the letdown reflex?
it stimulates milk release from the breast
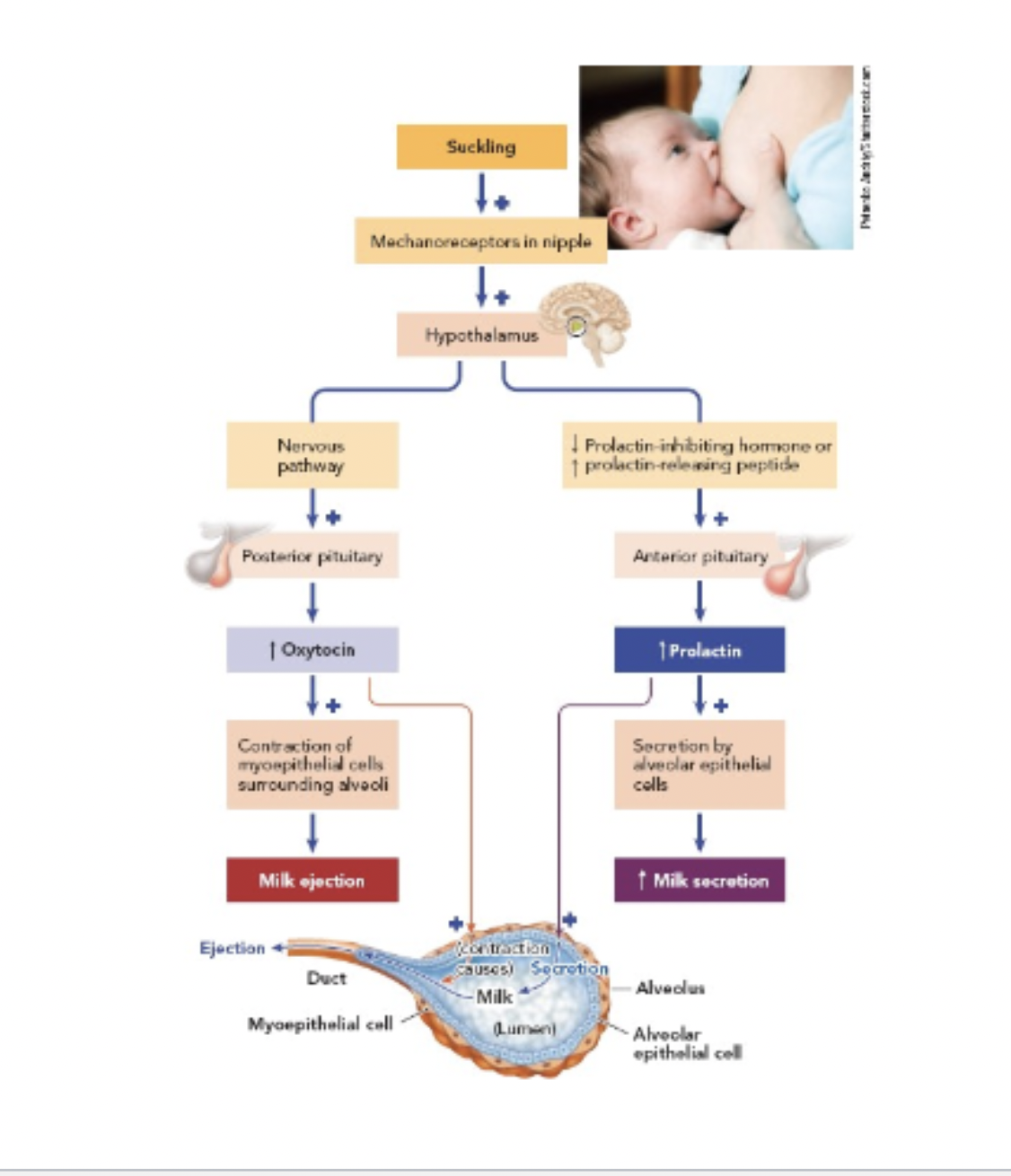
which gland releases prolactin? which gland releases oxytocin?
the anterior pituitary releases prolactin, and the posterior pituitary releases oxytocin
comparison diagram of the different types of breastmilk

what is milk banking?
a system that provides donated human milk to infants who cannot be breastfed by the mother
what are the general infant reflexes for a breastfeeding infant?
suckling reflex: 34 weeks gestation
gag reflex: 28 weeks gestation - developed to prevent intake of food and fluid into lungs
oral search reflex: infant opening mouth and thrusting tongue forward to breast
rooting reflex: infant turns to side when stimulated on that side
how do you identify hunger in infants?
cues like bringing hands to mouth, sucking on them, moving head from side to side
crying is a ___ sign of hunger
late
how many feedings per day is normal for infants?
10-12 feedings
what two supplements are necessary for infants?
vitamin K at birth
vitamin D beginning in first 2 months of life
how many calories per day are needed for milk production within the first 6 months?
540 cal per day
how many calories per day are needed for milk production from 7 to 12 months?
380 cal per day
what is the overall recommendation for additional calories per day for lactating women?
additional 500 calories
what kind of supplementation may be needed when a mother has a vegan diet?
vitamin B12 supplementation
what is colic?
a condition where the baby is crying for more than 3 hours a day, more than 3 days a week, for longer than 3 weeks with no known medical cause. May be influenced by components of maternal diet (e.g. cow’s milk, onions, cabbage, broccoli, chocolate)
what percent of women report breastfeeding problems in the first week?
over 90%
what is engorgement?
when breasts overfill with milk, due to the fact that the supply and demand process is not yet established.
Best prevention is to nurse or pump frequently
what is mastitis?
inflammation or bacterial infection of the breast that occurs in 3-20% of breastfeeding women, commonly between 2-3 weeks postpartum. Caused by cracked nipple or missed feeding and associated with flu-like symptoms
what are galactagogues?
substances (like metoclopramide, fenugreek) used to increase milk supply
what are medical contraindications to breastfeeding?
galactosemia — missing or dysfunctional galactose-1-phosphate uridyltransferase enzyme so baby can’t process galactose
mother on drugs
HIV infection (transmission rates increase with prolonged breastfeeding)
what is hyperbilirubinemia?
bilirubin is the by-product from the breakdown of RBCs, and is a cell toxin that is supposed to be excreted by the baby. hyperbilirubinemia common in infants, and most frequent cause for hospital readmission
what is neonatal jaundice?
characterized by a yellow color of skin due to high amounts of bilirubin in the blood. Can cause permanent neurological damage, and treated by phototherapy.
what is the difference between physiologic and pathologic newborn jaundice?
physiological:
begins after first day of birth, peaks around day 5
bilirubin < 12 mg/dL
resolves itself within several days
pathological:
begins within first day, rises faster and lasts longer
bilibrubin > 8 mg/dL in first day
medical intervention required with phototherapy
what is kernicterus?
severe condition when bilirubin levels are so high they move from the blood to brain tissues, causing brain damage and permanent injury if not treated promptly.
what is the mortality rate of kernicterus?
50%
how do breastfeeding benefits apply to mothers of twins and higher ordered multiples?
direct correlation — breastfeeding benefits are multiplied
how are late preterm infants defined?
infants born 34-37 weeks
what are the risks/complications of late preterm infants?
makes breastfeeding difficult, risk for insufficient milk intake
risk for: hypoglycemia, jaundice, poor weight gain, rehospitalization, cardio-respiratory instability, poor temp control, immature immune system
how do you best manage late preterm infants?
build and maintain human milk supply
pump if needed
feed infant
encourage skin to skin contact
what percent of pregnant/breastfeeding women receive maternal medication?
94%
are herbal remedies always safe for mothers to use?
can have significant side effects, so medicinal herbs should be viewed as drugs. not always appropriate during lactation.
what is the result of nicotine (smoking cigarettes) on lactation?
lower milk volumes and decreased fat concentrations, resulting in potential poorer infant growth and affected sleep patterns. nicotine levels in breastmilk are 1.5-3x higher than in mother’s blood
what effects does marijuana have on lactation?
it is transferred and concentrated in breast milk, and there is potential for increased risks of neurodevelopmental problems
what effects does caffeine have on lactation?
moderate intake causes no problems for most, and levels in breast milk are only 1% of maternal plasma. However, if levels accumulate in infants, it can interfere with sleep or cause hyperactivity.
what are two important measures of assessing newborn health?
birthweight and gestational age
full-term infants with normal birthweights are generally healthy
how is a full term infant defined?
37-42 weeks
what are the two most important predictors of an infant’s survival later health?
age and birthweight
how are premature babies defined?
37 weeks of pregnancy
what is the leading cause of infant mortality worldwide?
preterm birth
what are the 4 newborn growth assessment indicators?
gestational age
birthweight
length
head circumference
what does AGA, SGA, and LGA stand for?
AGA = appropriate for gestational age
SGA = small for gestational age
LGA = large for gestational age
define physical growth
increase in body mass that occurs at genetically determined rates, patterns, and ages
what is the average infant measurements at birth?
weight: 7-7.5 lbs
length: 20 in
head circumference: 13-15 in
infants generally ____ their birth weight by 4-6 months
double
in one year, a full term infant generally ___ in birth weight
triples
what are the two different kinds of growth charts?
weight for age and length
length and head circumference for age
crossing what percentile for growth charts is a cause for concern?
two percentile lines
WHO vs CDC growth charts
WHO - created from data points of growth from healthy children in optimal conditions
CDC - created from data in US children during the 1970s and 1990s
what are the CDC recommendations for using growth charts?
from 0-2 years, use WHO growth charts. From 2-19 years, use CDC growth charts
what are signs of cognitive development in babies?
perception, object permanence, object recognition, language
what is motor development?
ability to control voluntary muscle movement
what are critical periods?
fixed times during which certain behaviors emerge that are necessary for sequential learning skills
at birth, what nutrients can a healthy newborn digest?
fats, proteins, and simple sugars
infant requirements for many nutrients are ____ more than adults per kg of body weight
2-3x