Topic 13: Innate Defense System
- Overview of Host Resistance
* immune system
* composed of wide variety of cells, tissues, and organs
* recognizes foreign substances or microbes and acts to neutralize or destroy them
* “probiotic—up to 500 species”, “prebiotic” – up to ¾ immune system reside in your gut
* probiotic line intestine (mental health importance; dependent on nutrition)
* said will not ask # of species
* know difference between the two?
* compromised by stress, health problems & unhealthy food / lifestyle
* immunity
* ability of host to resist a particular disease or infection
* immunology
* science concerned with immune responses - Terminology
* Susceptibility: Lack of resistance to a disease
* Immunity: Ability to ward off disease
* Innate immunity: Defenses against any pathogen
* “nonspecific immunity”
* Adaptive immunity: Immunity, resistance to a specific pathogen - Types of immune responses
* Innate (nonspecific) defense system
* responds quickly, offers resistance to any microbe or foreign substance, lacks immunological memory, and consists of:
* First line of defense – skin and membranes
* Second line of defense – antimicrobial proteins, phagocytes, and other cells
* Inhibit spread of invaders throughout the body (stop the invaders)
* Inflammation is its hallmark and most important mechanism (cause of swelling, heat, redness)
* Where did you hear phagocytosis?
* WBC will “eat” them; bacterias with capsule resistant to phagocytosis - Immunity
* Innate Immunity
* First Line of Defense
* Intact skin
* Mucous membranes and their secretions
* Normal Microbiota (antagonism)
* antagonism is your normal bacteria on skin that keeps you “clean” → will be “mean/antagonize” new bacteria
* Second Line of Defense
* Natural Killer cells and phagocytic WBC
* Inflammation
* Fever
* Antimicrobial substances
* Adaptive Immunity (“specific”)
* Third Line of Defense
* Specialized lymphocytes: T and B cells (T cells are HIV’s target; B cells give antibodies)
* Antibodies
* received by getting sick and producing B cells or getting vaccine with B cells - Adaptive (specific) defense system
* Also called acquired or induced immunity, has immunological memory, responds to a very particular foreign substance (why some substances last a shorter time than others? they don’t know yet; COVID is one that doesn’t have a long memory)
* about 2 weeks to produce antibodies (don’t get vaccine when people are already sick, do it sooner)
* Third line of defense
* Takes longer to react than the innate system
* Works in conjunction with the innate system
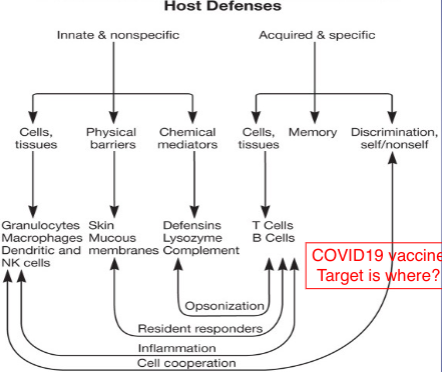
- Components of the Innate Immune System
* Skin (biggest organ)
* Mucous
* most pathogens go through mucous membrane (eyes, nose, mouth)
* Covid going for respiratory; cytocines? caused continous inflammation
* Chemical
* stomach acid
* food poisiong indicates eating a lot of bacteria
* bacteria can go up through urinary tract and cause UTI, if not treated the bacteria can travel upwards
* lysozyme cuts galasidic bond?
* smokers cough in morning because paralysis of cilia (cilia moves the fluid upwards) - Innate (non-specific) defense systems
* Surface Barriers: Skin, mucous membranes, and their secretions make up the first line of defense
* sebaceous glands → oils (sebum)
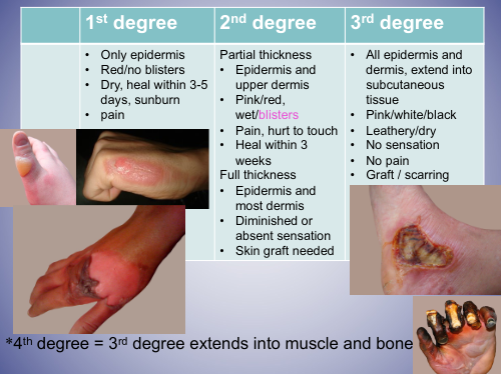
- Skin
* Largest organ (20 sqft), 10+/- pounds
* strong mechanical barrier to microbial invasion
* keratin produced by keratinocytes (=basal cells) in outer layer
* resists absorption of water and most inorganic chemicals; allows absorption of many organic and a few inorganic chemicals - Skin infection/reaction by microbes
* Cellulitis: inflammation due to infection
* does not have to be an open cut
* Warts: viral infection cause excess skin growth
* Herpes: HSV-1&HSV-2, periodic blisters around lips or genitals
* cold sores
* Hives: allergic reaction – not infection
* Tinea: skin mycosis
* fungal skin infection
* Shingles: varicella zoster virus (linear DNA, lipid enveloped, herpes group)
* DNA virus, enveloped, hide when young but “come out” when older
* younger people can get it as well - Skin = inhospitable environment for many microbes
* attached organisms removed by shedding of outer skin cells = part of your soap scum, eww
* pH 3-5 = acidic
* high NaCl concentration = why?
* skin bacteria have a high salt toleration and dryness (mannitol salt agar!)
* subject to periodic drying
* Lysozyme in saliva and tears – function
* prevents infection
* Fungistatic fatty acids in sebum
* Transferrin** in blood (who’s the bad guy?)
* *Antagonisms: competitive exclusion of normal microbiota (our bacteria)
* **iron-binding blood glycoproteins - More about Skin
* specialized cells called skin-associated lymphoid tissue (SALT)
* Langerhans cell---NOT islet of Langerhans in pancreas!!!
* dendritic cell that can phagocytose antigens
* have lots of branches; can eat the pathogens (bring inside cell)
* differentiates into interdigitating dendritic cell–presents antigen to and activates T cells
* uses piece of pathogen to present to T cell - Antimicrobial Secretions
* lysozyme
* How?: tears, saliva
* cut 1-4 galoscidic bond
* lactoperoxidase
* produces superoxide radicals: toxic
* mammary and salivary gland (saliva) - The Eye
* flushing action of tears
* lysozyme, lactoferrin and secretory IgA in tears
* lactoferrin - transferrin (good?)
* Lactoferrin: multifunctional protein (antimicrobial)
* IgA = antibody
* cover antibodies later - Mucous Membranes
* form protective covering that resists penetration and traps many microbes
* are often bathed in antimicrobial secretions which contain a variety of antimicrobial substances
* contain mucosal-associated lymphoid tissue (MALT)
* mucous can trap bacteria - Mucosal-Associated Lymphoid Tissue (MALT)
* specialized immune barrier
* gut-associated lymphoid tissue (GALT)
* bronchial-associated lymphoid tissue (BALT)
* two types of MALT - Respiratory system
* turbulent air flow deposits microbes onto mucosal surfaces
* COVID 19 TARGET
* Mucociliary blanket
* mucous secretions that traps microbes
* once trapped, microbes transported away from the lungs (mucociliary escalator)
* can be expelled by coughing or sneezing
* salivation washes microbes to stomach (pH 3-5)
* alveolar macrophages
* phagocytic cells in alveoli of lungs
* capsule bacteria prevent digestion by phagotcytic cells - When you smoke…
* Cilia paralized, smoker’s cough
* being moved upwards
* Smokers are sick more often because……
* cilia is paralized therefore cilia isn’t moving upwards
* Morning cough
* 80% lung cancer – due to smoking, 13% survive 5+ years
* includes 2nd hand smoking
* P53 gene – nose, liver, colon, myloid leukemia
* cancer suppressing gene
* Tobacco smoke contains a deadly mix of more than 7,000chemicals. Hundreds are toxic. About 70 can cause cancer. Here are some of the chemicals. (said wouldn’t ask about chemicals, just information)
* Cancer-Causing Chemicals
* Formaldehyde: Used to embalm dead bodies
* Benzene: Found in gasoline
* Polonium 210: Radioactive and very toxic
* Vinyl chloride: Used to make pipes
* Toxic Metals
* Chromium: Used to make steel
* Arsenic: Used in pesticides
* Lead: Once used in paint
* Cadmium: Used to make batteries
* Poison Gases
* Carbon monoxide: Found in car exhausts
* Hydrogen cyanide: Used in chemical weapons
* Ammonia: Used in household cleaners
* Butane: Used in lighter fluid
* Toluene: Found in paint thinners - Helicobacter pylori –in the disease packet
* Gram -, Curved rod, Microaerophilic
* microaerophilic - likes less oxygen (strept throat test)
* 80% of infected people = asymptomatic
* Gastritis, linked to duodenal and stomach cancer – stress was to blame before the discovery
* burrow into stomach
* high salt diet dissolves membrane in stomach (high salt diet = higher chance of stomach cancer)
* Stomach acid gradient chemotaxis
* urea in stomach acid
* Urease –Ammonia production, ph?
* metabolize protein, pH increases
* 1st infection – antibody test
* 2nd and after – Urea or stool test
* because possible antibodies from last infection
 Picture: blood has plasma and cells (red blood cells, platelets, and white blood cells); centrifuge separates layers
Picture: blood has plasma and cells (red blood cells, platelets, and white blood cells); centrifuge separates layers
- Blood Plasma – approx. 55%
* Glucose, fat
* Protein – (antibodies 1/3)
* Clotting factor
* Electrolytes, vitamins
* Hormones
* BP, pH
* less fluid increase BP; neutral pH
* CO2
- Donations
* Blood donation ---- NO NO
* Have tested positive for hepatitis B or hepatitis C, lived with or had sexual contact in the past 12 months with anyone who has hepatitis B or symptomatic hepatitis C.
* After donation, test for ….HIV, hepatitis, syphilis, Human T-lymphotropic virus
* Platelets donation – not from mama. Why????
* pregnant - may have antibody from baby
* Plasma donation – no tuberculosis, malaria, sickle cell anemia, cancer etc..
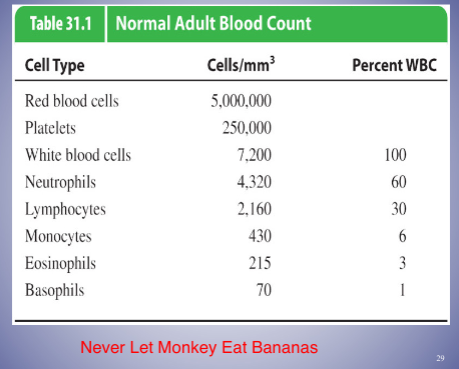
* screening - White Blood Cells and the Nonspecific and Specific Responses
* white blood cells (WBCs) - major role in the innate and specific responses
* Hematopoesis – hematopoetic stem cell differentiation process (all blood components)
* stem cells that differenate
* umblitical cord has stem cells
* development of white blood cells in bone marrow of mammals
* WBCs that mature prior to leaving bone marrow, e.g. macrophages and dendritic cells, become part of innate immune system and will respond to all antigens
* WBCs that are not fully functional after leaving bone marrow become part of the adaptive immune response, e.g.B and T cells and could differentiate in response to specific antigens
* know the differences
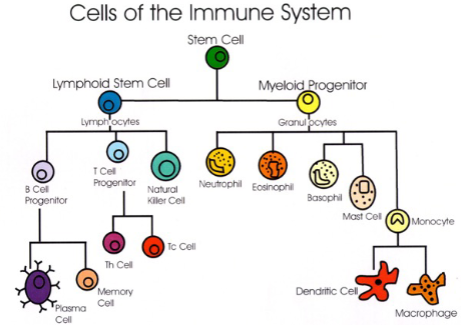
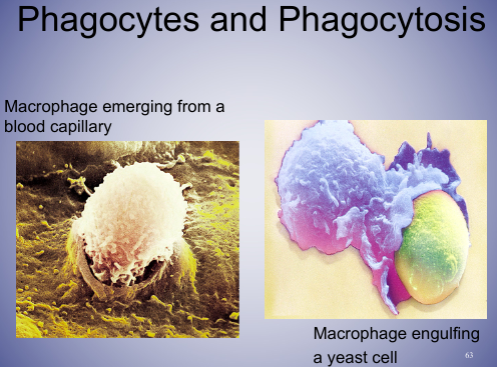
- Monocytes and macrophages
* highly phagocytic cells, 6% of WBC
* engulf pathogen, lysosome digests pathogen
* make up monocyte-macrophage system
* monocytes
* are mononuclear phagocytic leukocytes
* after circulating for ~8 hours, mature into macrophages
* macrophages
* reside in specific tissues
* have a variety of surface receptors
* senses the pathogens
* named according to tissue in which they reside
- Dendritic Cells: Antigen-presenting cells (APC)
* present in small numbers in blood, skin, and mucous membranes of nose, lungs, and intestines
* contact, phagocytose and process antigens → display foreign antigens on their surfaces (antigen presentation)
* bring antigen/pathogen to surface to show other cells (i.e macrophages) - Basophils
* stain bluish-black with basic dyes, 1% of WBC
* Non-phagocytic
* release histamine, heparin, prostaglandins, serotonin, and leukotrienes from granules
* histamine most important
* play important role in development of allergies and hypersensitivities (inflammation)
* antihistamines - Eosinophils
* stain red with acidic dyes, 3% of WBC
* defend against parasites (protozoan and helminthes)
* play a role in asthma/allergic reactions along with mast cells - Neutrophils
* stain at neutral pH
* 60% of WBC - majority
* highly phagocytic - 1st to go to site
* circulate in blood then migrate to sites of tissue damage
* sequeeze through capillary walls
* kill ingested microbes with lytic enzymes and reactive oxygen metabolites
* high neutrophil count = bacterial infection
* pus is normally dead neutrophils - Mast Cells
* differentiate in blood and connective tissue
* contain granules containing histamine, heparin, and other pharmacologically active chemicals, over 200+ chemicals
* play important role in development of allergies and hypersensitivities
* Mast cell activation syndrome
* idopathic - don’t know what it is, may be genetic - Lymphocytes
* major cells of the immune system, 30% of WBC
* major populations include T cells, B cells, and natural killer (NK) cells
* B and T lymphocytes differentiate in bone marrow from stem cells - B Lymphocytes
* B cells (B lymphocytes)
* mature mostly in lymph nodes and other lymph tissues
* circulate in blood
* can settle in lymphoid organs
* after maturation and activation are called plasma cells and produce antibodies
* memory and antibodies (after ~10 days)
* outside of pathogens - T Lymphocytes
* T cells (T lymphocytes)
* Mature primarily in the thymus gland
* can remain in thymus, circulate in blood, or reside in lymphoid tissue
* like B cells, require antigen binding to surface receptors for activation and continuation of replication
* need a signal (i.e antigen presenting cell - dendritic cell)
* they have no memory or antibodies
* cytokines, chemicals that have effects on other cells, are produced and secreted by activated T cells - Natural Killer (NK) Cells
* small population of large non-phagocytic granular lymphocytes
* kill malignant cells and cells infected with pathogens
* two ways of recognizing target cells
* bind to antibodies which coat infected or malignant cells (antibody-dependent cell-mediated cytotoxicity (ADCC))
* recognizes cells that have lost their class I major histocompatibility (MHC) antigen due to presence of virus or cancer
* organ transplant
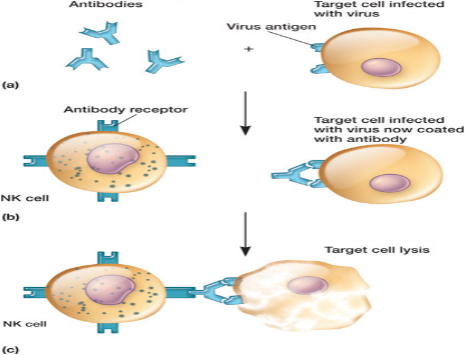
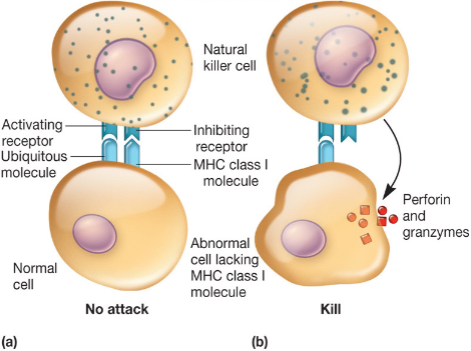
- Cytotoxic T Cells and Natural Killer Cells
* Cytotoxic T-cells : the specific antigens presented by their MHC class I molecule
* recognize receptor and present it
* NK cells : the absence of MHC class I molecules, specific types of antibodies, and \n some type of cellular stress
* Know the difference!
- Primary Lymphoid Organs and Tissues
* immature undifferentiated lymphocytes (generated in the bone marrow) → mature
* obtain a specific antigenic specificity within the primary lymphoid organs and tissues, bone marrow and thymus gland
* unique to pathogens - Secondary Lymphoid Organ/Tissue
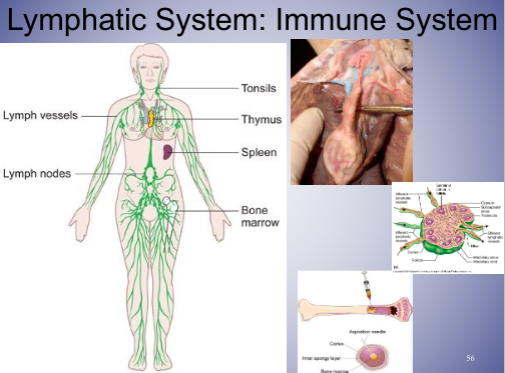
* Secondary lymphoid tissue includes: lymph nodes, tonsils, adenoids, Peyer’s patches (intestine), spleen
* throughout the body
* interface between innate and acquired host immunity (overlap)
* act as areas of antigen sampling and processing
* determine if the threat needs to be neutralized
* some lymphoid cells are found closely associated with specific tissues
* e.g., skin-associated lymphoid tissue (SALT)
* e.g., mucous-associated lymphoid tissue (MALT)
* e.g. bronchial associated lymphoid tissue (BALT) - Secondary Lymphoid Organ/Tissue
* spleen
* highly organized lymphoid organ
* filters blood - scanning
* trap microbes and antigens
* present antigens to B and T cells
* most common way that lymphocytes become activated to carry out their immune functions
* lymph nodes
* highly organized lymphoid tissue
* filter lymph
* microbes and antigens trapped and phagocytosed by macrophages and dendritic cells
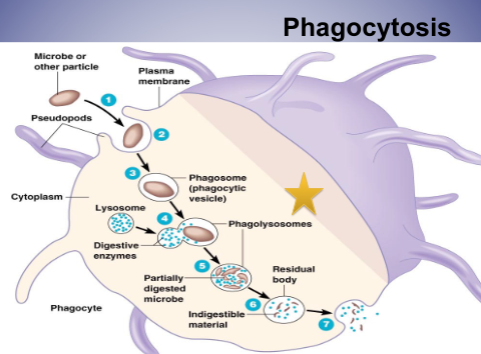
* B cells differentiate into memory and plasma cells within lymph nodes - Phagocytosis
* process by which phagocytic cells (monocytes, tissue macrophages, dendritic cells and neutrophils) recognize, ingest and kill extracellular microbes
* How bacteria resist?
* capsule
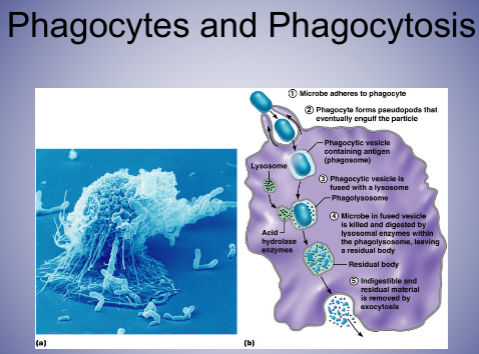
- Phagocytosis
* two mechanisms for recognition of microbe by phagocyte
* opsonin-independent (nonopsonic) recognition
* opsonin-dependent (opsonic) recognition
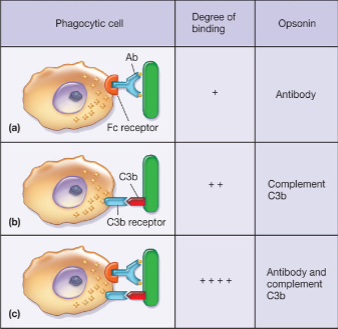
* phagocytosis can be greatly increased by opsonization - Opsonization (stopped here w/ anki)
* opsonin – Greek: prepare for eating
* opson – Greek: delicious side dish
* process in which microbes are coated by serum components in preparation for recognition/ingestion by phagocytic cells
* molecules that carry out above are called opsonins = antibodies, complement molecules
* some complement proteins are opsonins
* bind to microbial cells, coating them for phagocyte recognition - Opsonin-Independent Mechanism
* involves nonspecific and specific receptors on phagocytic cells
* four main forms:
* recognition by lectin-carbohydrate interactions
* recognition by protein-protein interactions (PPI)
* recognition by hydrophobic interactions
* detection of pathogen-associated molecular patterns (PAMPs) by pattern recognition receptors (PRRs, e.g., toll-like receptors)
* *lectin: carbohydrate binding proteins
* *PPI: Alzheimer’s, CJD, Cancer - Pathogen-Associated Molecular Patterns (PAMPs)
* PAMPs are unique to microbes, not present in host
* Examples of unqiue features
* e.g., lipopolysaccharide (LPS) of gram negative bacteria
* e.g., peptidoglycan of gram positive bacteria
* PAMPs recognized by pattern recognition receptors (PRRs) on phagocytic cells - Toll-Like Receptors (TLRs)
* recognize and bind unique PAMPs of viruses, bacteria or fungi
* Innate
* Macrophages, Dendritic cells
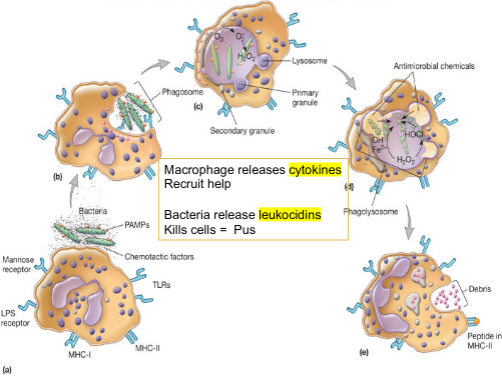
* on these cells - Intracellular Digestion
* phagolysosome
* vacuole which results from fusion of phagosome with lysosome
* presence of toxic chemicals
* e.g., degradative enzymes
* e.g., toxic reactive oxygen intermediates (ROIs) (kills microorganisms)
* e.g., reactive nitrogen intermediates (RNIs)
- Neutrophils – after digesting microbial fragments
* also phagocytic - 1st to be at site of injury
* Exocytosis
* process used by neutrophils to expel microbial fragments after they have been digested
* phagolysosome unites with cell membrane
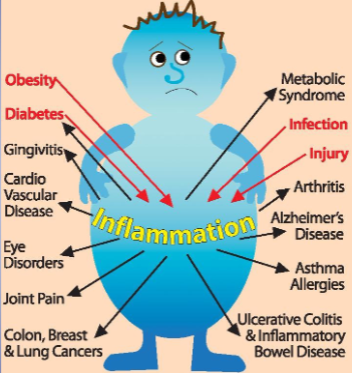
* results in extracellular release of microbial fragments - Inflammation (innate side)
* nonspecific response to tissue injury
* can be caused by pathogen or physical trauma
* acute inflammation is the immediate response of body to injury or cell death
* cardinal signs---PRISH (reactions from inflammation)
* Pain – release of chemicals such as histamine
* Redness – increased blood flow
* Immobility - altered or loss of function
* Swelling – edema (accumulation of fluid)
* application of ice pack (no more than 20 min because it slows the process of blood flow which gets rid of the waste)
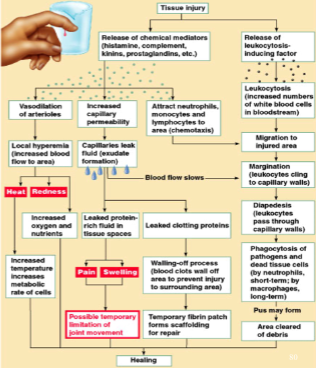
* Heat – increased blood flow - Acute Inflammatory Response
* Vascular phase first, then cellular phase
* vascular is the fluid
* the release of inflammatory mediators from injured tissue cells initiates a cascade of events which result in the signs of inflammation
* involves chemical mediators
* chemokines - signaling proteins/cytokines
* released by injured cells
* selectins
* cell adhesion molecules on activated capillary endothelial cells
* integrins
* adhesion receptors on neutrophils
* blood vessel will get loose because of histamine and neutrophils can squeeze through - Inflammatory Response Vascular Permeability
* Vasodilation
* Chemicals released by the inflammatory response stimulate mast cells next to capillaries
* Mast cells release histamines to increase permeability of capillaries
* histamines make you “leaky”
* Plasma seeps into tissue (interstitial) spaces causing local edema (swelling), which contributes to the sensation of pain
* *pain – Na+channel
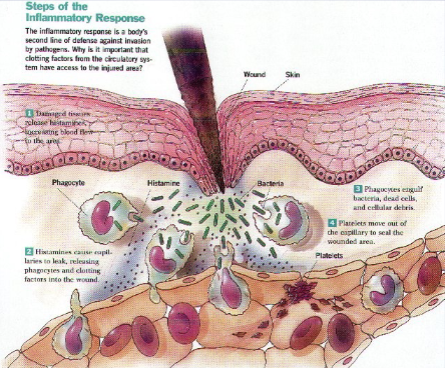
* lidocaine blocks Na+ channel - Inflammatory Response Phagocytic Mobilization
* Margination – neutrophils cling to the walls of capillaries in the injured area
* Diapedesis – neutrophils squeeze through capillary walls and begin phagocytosis
* know margination and diapedesis
* Chemotaxis – inflammatory chemicals attract neutrophils to the injury site
- Chronic Inflammation
* slow process
* may not notice
* rhuematoid arthrisis
* excema
* involves formation of new connective tissue
* usually causes permanent tissue damage
* dense infiltration of lymphocytes and macrophages at site of inflammation
* granuloma
* walled off area formed when phagocytic cells can’t destroy pathogen
- ~~Opsonization~~
* ~~process in which microbes are coated by serum components in preparation for recognition/ingestion by phagocytic cells~~
* ~~molecules that carry out above are called opsonins~~
* ~~make pathogen more visible~~
* ~~some complement proteins are opsonins~~
* ~~bind to microbial cells, coating them for phagocyte recognition~~ - Pus
* Dead leukocytes (mostly neutrophils)
* Color varies
* Abscess=enclosed in tissue
* Pimple=visible collection within/beneath the epidermis
* Pus causing bacteria = pyogenic
* Example from your lab: Staphylococcus aureus (pink eye), S. epidermidis, S. pyogenes (strept throat) (Gram+, β-hemolysis, catalase-), Escherichia coli, Pseudomonas aeruginosa - The Complement System (or cascade)
* composed of >30 serum proteins – mainly produced in liver (pro-proteins)
* augments (or “complements”) the antibacterial activity of antibody
* part of innate immunity, will NOT change over ones lifetime, does not adaptable
* genetic, pre-determined
* aide in getting rid of pathogen
- Other Functions of Complement Proteins
* function as chemotactic signals that recruit phagocytes to their activation site
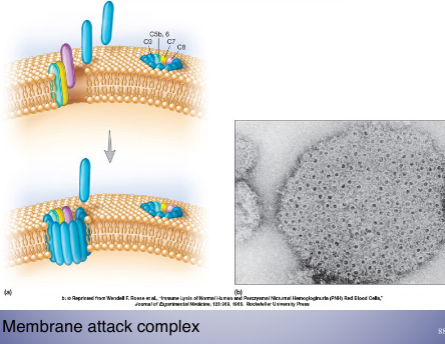
* puncture cell membranes causing cell lysis
* important function
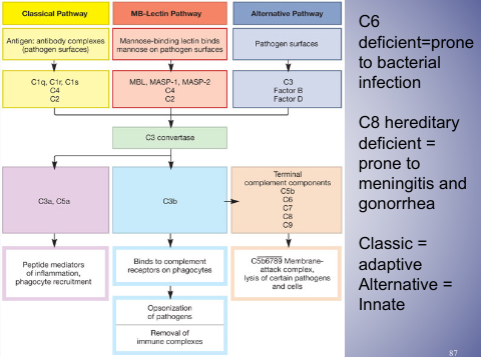
* many complement activities unite the nonspecific and specific arms of the immune system to destroy and remove invading pathogens - Complement Activation Pathways (innate)
* specific proteins are unique to the first part of each of the three complement activation pathways, but all complement pathways have the same outcome
* Opsonization - phagocytosis
* stimulation of inflammatory mediators
* lysis of microbes by membrane attack
* all pathways are activated as a cascade; the activation of one protein results in the activation of the next
* all complement proteins are in the inactive state until activation when the host is challenged by an invading microbe
- Cytokines
* soluble proteins or glycoproteins that are released by one cell population that act as intercellular mediators or signaling molecules
* monokines
* released from mononuclear phagocytes
* i.e macrophages
* lymphokines
* released from T lymphocytes
* interleukins
* released from one leukocyte and act on another leukocyte
* colony stimulating factors (CSFs)
* act on hemopoietic stem cell, stimulate growth and differentiation of immature leukocytes in bone marrow - Interferons (IFNs) =type of cytokines
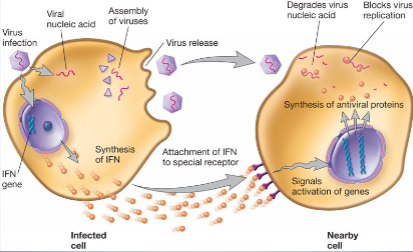
* regulatory cytokines produced by some eukaryotic cells in response to viral infection
* viral infection is important (acute)
* do not prevent virus entry into host cells, but defend against viruses by preventing viral replication and assembly
* also help to regulate the immune response
* responsible for “flu-like” symptoms
* clinical use for viral infection, MS and cancer treatment
* cancer treatment: elicit T cells (side effects: thinning hair, flu-like symptoms); T cells attack cancer
- Fever
* 37.5-38.3 °C (99.5-100.9°F) or above
* dr starts to get worried at 105
* most common cause of fever is viral or bacterial infection or bacterial toxins
* Viral --- DO NOT ask for antibiotics!!!!
* Thermostat set point located in hypothalamus - More About Fever
* in most cases, the endogenous pyrogen, a cytokine produced in response to pathogen, directly triggers fever production
* after release, pyrogens → hypothalamus and induce production of prostaglandins which reset hypothalamus to a higher temperature
* increase temp
* When the hypothalamus is reset, what has to happen to increase body temperature?
* *Pyrogen = a fever inducing substance
* **Prostaglandins = found in every tissue, hormone-like effect, lipid derived
* ***Physical activity is needed to increase metabolic rate, heat production = This accomplished by shivering thermogenesis.
* know where body’s thermostat is - Should fever be reduced with medicines?
* Yes! Because……
* Febrile seizure (epileptic seizure) – can be dangerous
* some people can get seizures from fever (temperature increases too quickly)
* Feeling awful/miserable – treating the symptom, not the cause
* fever caused by infection
* bacterial infection treated by antibiotics, no treatment for viral infection
* No! because……….
* Not high enough fever
* may hinder immune system
* Research (2014) has shown that using fever-suppressing drugs may allow patients to mistakenly feel better quicker than normal resulting in their premature return to the population
* Concerning influenza, it is estimated that this will result in a 1% increase in the number of cases and about 700 more deaths each year in the U.S.
* contributes to spread