GI Tract Pathology
Pre-Knlowge of GI Tract
- the diaphragm separates the esoágues from the stomach
- parietal cells produce HCl and KCl (gastric acid) and excrete it in gastric glands
- What happens when someone vomits for days? * hypochloremic (hyper chloride) in blood * lower pH in the stomach
- PAS staining * Staines the lining of the mucus → polysaccharides
- Bolus moves passively and actively through the esophagus( peristaltic movement)
- Different squinters in GI tract
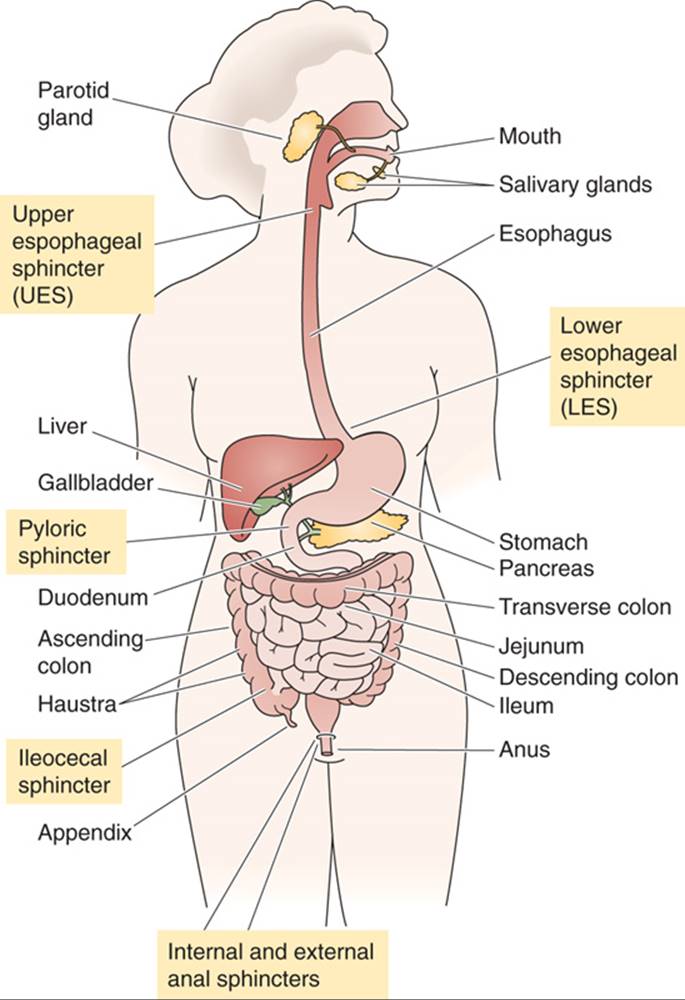
\
Functions and Characteristics of the GI tract
- %%Small intestines%% → absorption of carbohydrates, fats, minerals, proteins, water, and vitamins.
- %%Colon%%: absorption of water and electrolytes * Peyers patches →patches of immune cells that are found in ilium that detect and respond to foreign substances * most bacteria found( digest found + ferment food)
- %%Appendix%%: stores immune cells
| GI Tract Structure | Villi* | Crypts of Lieberkuhn** | Goblet Cells*** | the cell type that lines the surface |
|---|---|---|---|---|
| %%Esophagus%% | Absent | Absent | Absent | squamous cells**** |
| %%Stomach%% | Absent | Present in Gastric Glands | Absent | columnar cells ***** |
| %%Small Intestine%% | Present in the mucosa of the jejunum and ileum | Present | Present in the mucosa | columnar cells |
| }}%%Large Intestine%%}} | Absent | Present in the mucosa | Present in the mucosa | columnar cells |
*Villi: finger-like projections on the surface of the mucosa that increase the surface area for nutrient absorption to the lymphatic system and capillaries
→ they also have mussels to move bolus muscles
**Crypts: small tube-like structures that are located in the lining of the small intestine and the large intestine, produce digestive juices + harbor stem cells for epithelial lining
***Goblet cells: goblet cells secrete mucus that protects the mucosa from damage
**** Squamous cells: are flat and often found in barrier tissues
***** Columnar cells: are taller and typically found in tissues with secretory or absorptive functions.
Pathology of esophagus
- %%Heartburn%% * normally prevented by the angle of the stomach and lower esophageal sphincter(LES) * gastroesophageal reflux disease→ Barret disease of the esophagus (damaged and replaced by abnormal cells. This is usually caused by long-term acid reflux and is a risk factor for developing esophageal cancer)
- %%Eosinophilic esophagitis%% * allergy in the esophagus and a lot of eosinophils → rectaion to what pathogen is unclear maybe food
- %%IBD%%:
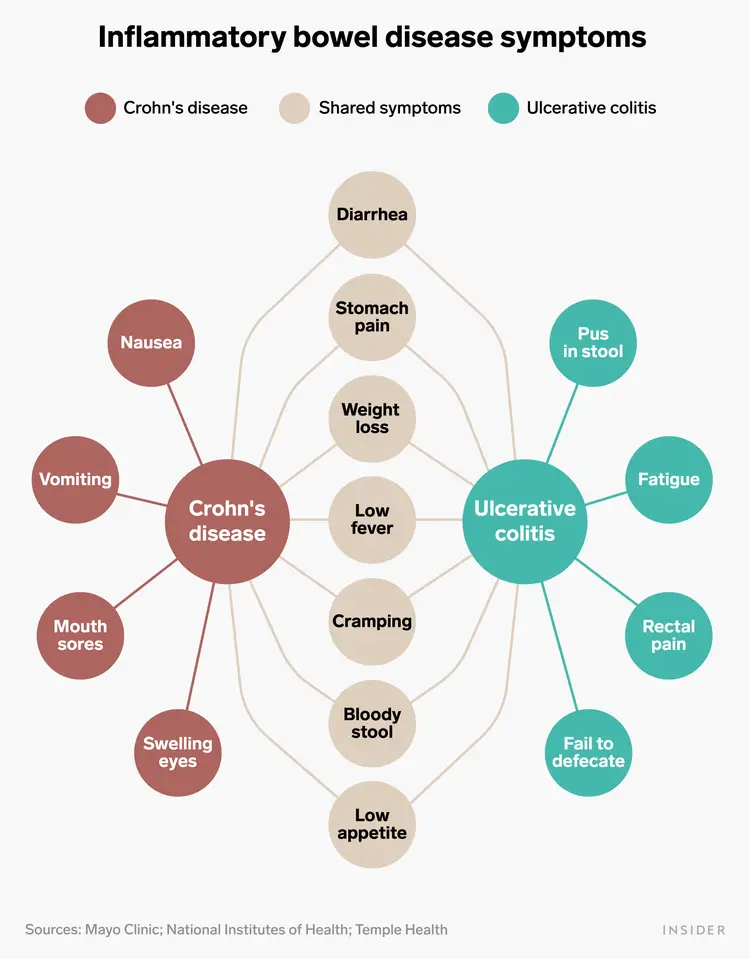
- ==Two types of IBD== (systematic disease) → due to a genetic defect, all leukocytes attack microbes and food
* the peak of onset 20 and 60 → 25% of all IBD start in childhood !!!
* symptoms come in waves and increase over a lifetime
* loss of tolerance**
* impairment of mucosal defense
* epithelial barrier defects
* Environmental factors:
* The earlier the onset, the more genetic the IBD
* Crohn’s disease
* vomiting
* Ulcerative colitis
* only concerns the colon → a lot of rectal symptoms that crawl upwards
* (difficult to diagnose because they look so similar (diarrhea with blood+ cramping + fever), but they are very different to treat
* red blood → inflammation colon
* black blood → small intestine
*
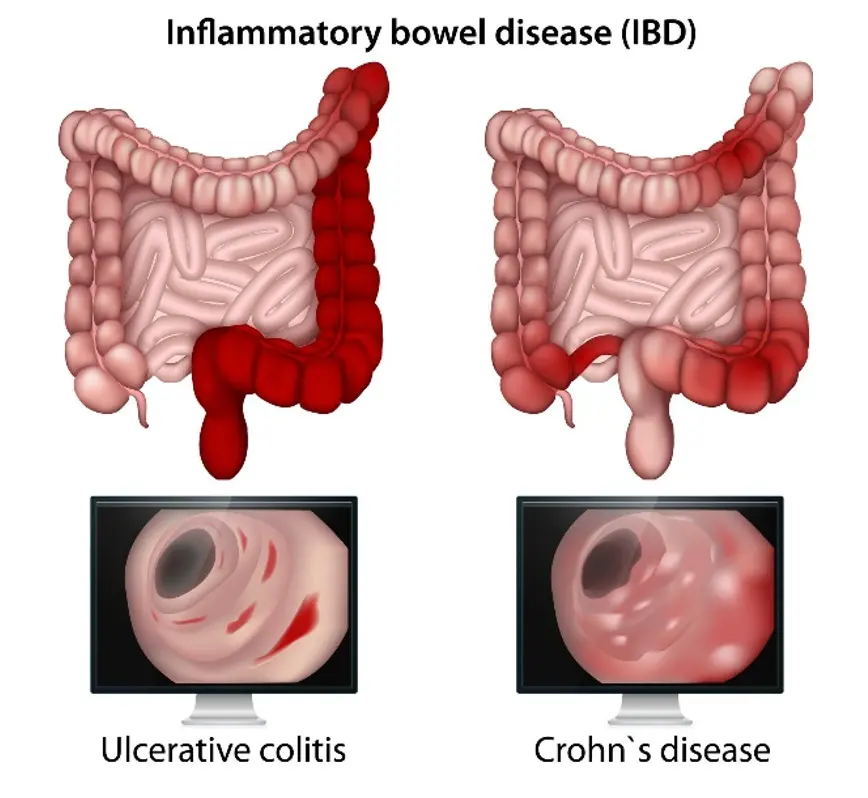
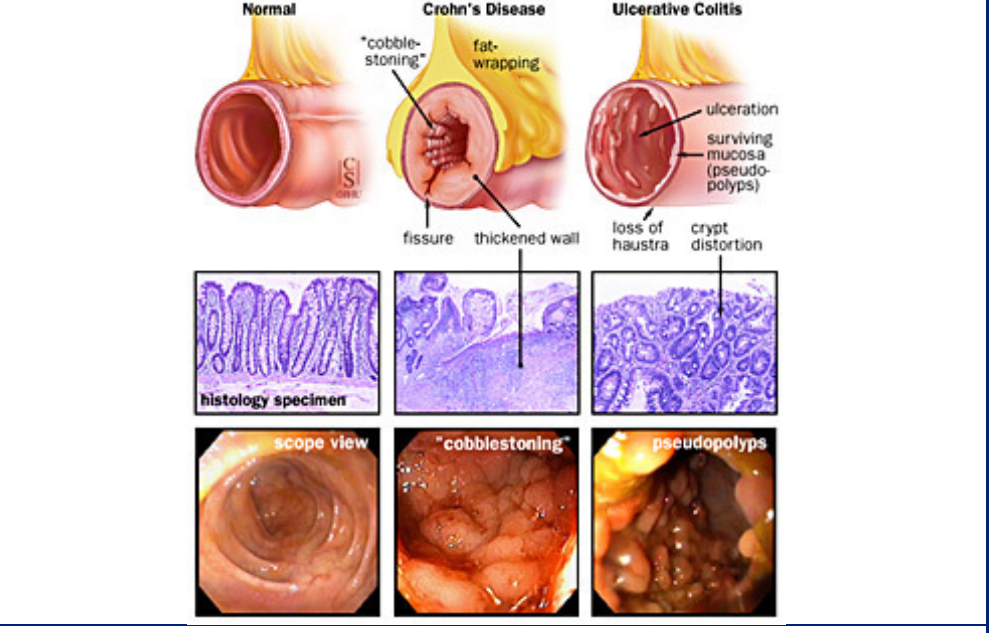
- ==Things that are specific to each disease== * * the disease can skip passages in the colon and cause inflammation → patchy inflammation * Fistulas: abnormal passageways that form between different parts of the body * → transmural ( tears through the tissue of them muscle) inflammation → feces can end up in urine * granulomas: clusters of cells that form when the body's immune system attempts to contain and eliminate foreign substances or bacteria * muscle hypertrophy * cobblestone appearance * fat wrapping * serological marker: ASCA
- @@Ulcerative colitis@@
* crypt distortions
* always originates in the rectum and then moves up until half of the colon or the entire colon
* serological markers: pANCA
* ulceration within the mucosa
* in children it does not have to start in rectum
*
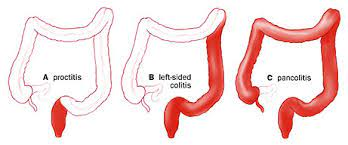
- {{Manifestation of IBD{{ * code in the lymph node that triggers an intestine attack * you can only have skin irritation and no intestine → due to gene alteration * because innate immune system is not working( NOD 2 intracellular bacterial receptor) there is an overload of B and T cells → underlying explanation of IBD
- **Tolerance in immunology * there is recognition of everything in our body by the immune system; in a normal state, there is a tolerant state; however, in IBD there is a loss of accepting new things * inflammation vs. tolerance ( too much aggressive inflammatory cells or too few protective cells)
- }}Treatment options}} * take out the colon in colitis to decrease inflammation →; however, inflammation will always stay because you can’t take out return * in crohns you can’t take out the colon because inflammation will continue in small intestines * steroids * targeted immunosuppression for specific immune cells
\