Human Physio Renal function and fluid balance
Structure & Function of the Urinary System
Functions
- Regulation of extracellular fluid volume & blood pressure * works with CVS to ensure tissues get enough O2 and BP within normal values
- Regulation of plasma osmolarity
- Maintenance of ion balance * in response to diet intake, urinary loss helps to maintain proper levels of Na+, K+, Ca2+ ions
- Homeostatic regulation of pH * remove or conserve either H+ or HCO3- (bicarbonate ions) as needed
- Excretion of waste * removes metabolic wastes dissolved in plasma e.g. uric acid and creatine
- Secretion of hormones and enzymes * erythropoietin (RBC production), renin (sodium balance and BP homeostasis) & vit D conversion to control Ca2+ balance
Structure of nephron
the nephron is the functional unit of the kidney
Renal corpuscle filters blood plasma:
- Glomerulus capillary network
- Glomerular (Bowman’s) capsule double walled up surrounding glomerulus
Renal tubule filtered fluid passes into:
- proximal convoluted tubule
- descending, loop of henle (nephron loop) and ascending
- Distal convoluted tubule
Distal convoluted tubule of several nephrons empty into single collecting duct
Renal exchange processes
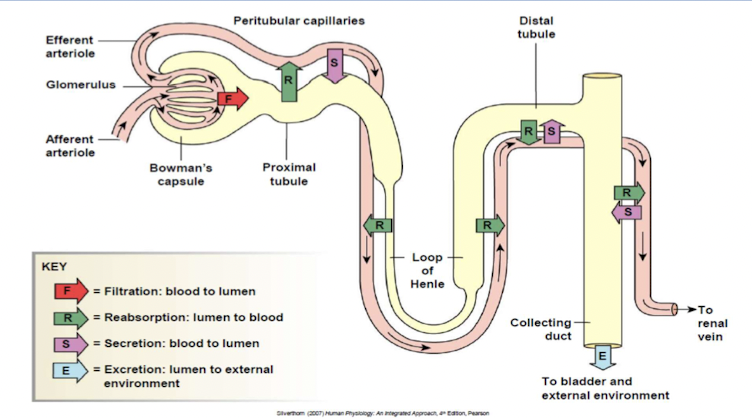
- Urinary excretion of substance depends on its filtration, reabsorption and secretion.
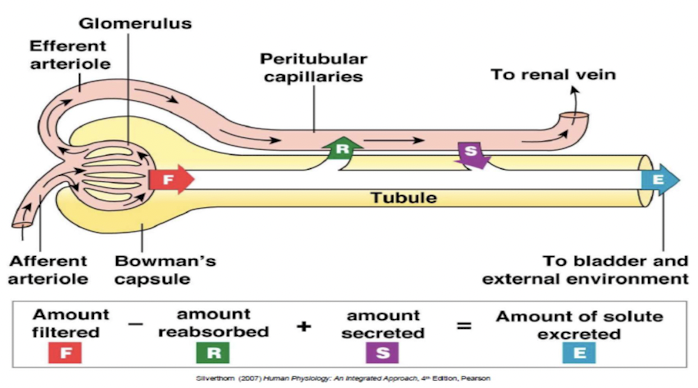
Glomerular filtration
Filtration barriers:
- Glomerular capillary endothelium
- Basal lamina
- Epithelium of Bowman’s capsule- podocytes
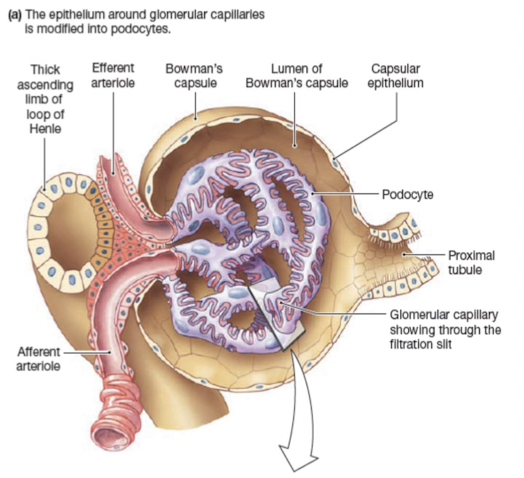
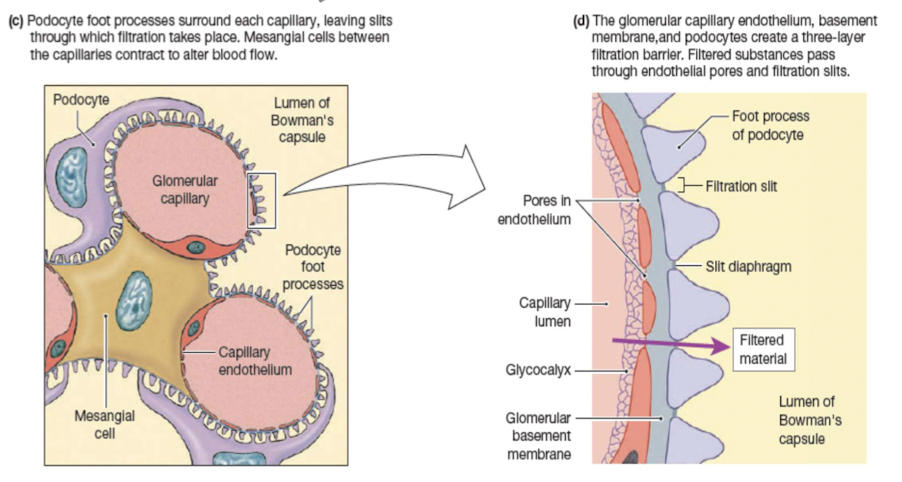
Forces that influence glomerular filtration:
- Hydrostatic/blood pressure (55 mmHg) * pressure of flowing blood in glomerular capillaries * favors movement of filtrate into Bowman’s capsule
- Colloid osmotic pressure (30 mmHg) * plasma proteins entering capsule create a gradient that favors movement back into capillaries
- Hydrostatic fluid pressure (15 mmHg) * in fluid up in enclosed Bowman’s capsule * creates a gradient that favors movement back into capillaries
Glomerular filtration rate (GFR)
- volume of fluid that filters into Bowman’s capsule per unit time
- average GFP 125mL/min or 180L/day
- Factors influencing GFP * Net filtration pressure * Filtration coefficient * surface area of glomerular capillaries * permeability between capillary & Bowman’s capsule
- 20% of plasma volume that pass through glomerulus is filtered
- <1% of filtered fluid is excreted
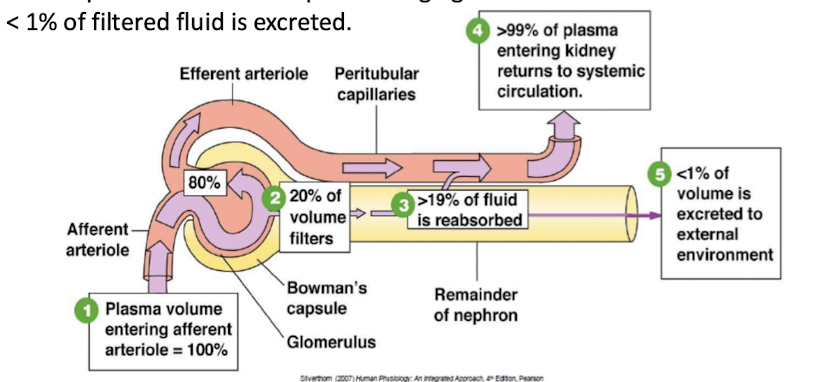
- Autoregulation of glomerular filtration rate takes place over a wide range of blood pressures.
Regulation of glomerular filtration rate
Myogenic response
- Intrinsic ability of vascular smooth muscle to respond to pressure changes
- ↑afferent arteriole resistance →↓GFR
- ↑efferent arteriole resistance → ↑GFR
Tubuloglomerular feedback
- Paracrine control through loop of Henle
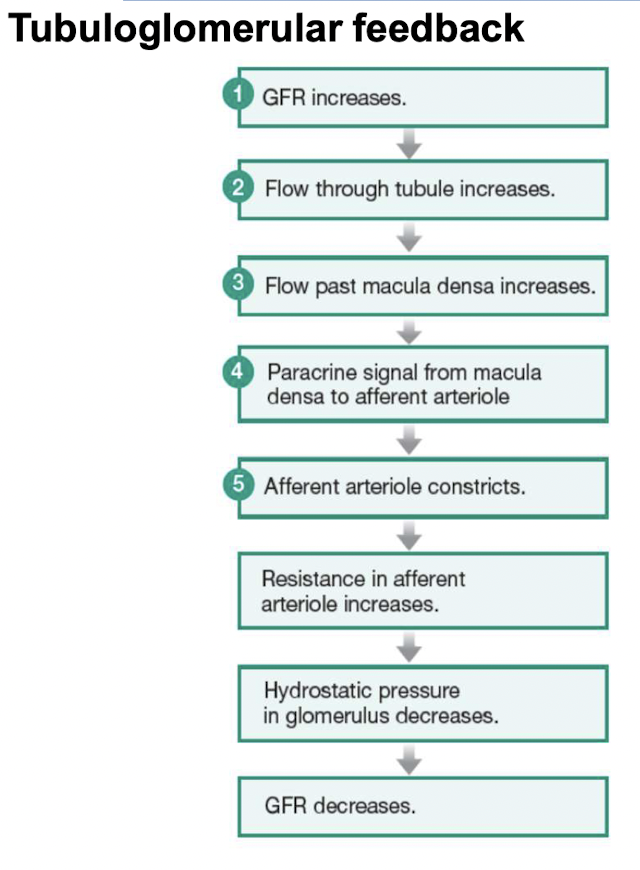
Hormones and autonomic neurons
- By changing resistance in arterioles
- By altering the filtration coefficient
- ==Angiotensin II== - vasoconstrictor
- ==Prostaglandins== - vasodilators
Reabsorption
- movement of filtered solutes and water from lumen of tubule back into plasma
- takes places in proximal tubule and distal segment of nephrons
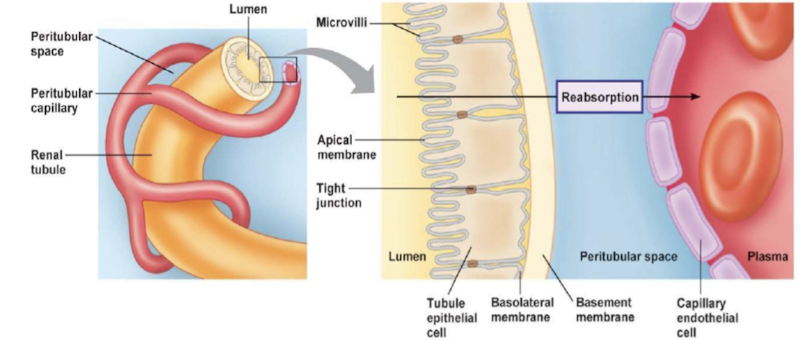
Principles governing tubular reabsorption of solutes & water:
- active transport to create concentration of electrochemical gradient
- water osmotically follow solutes
- Transepithelial transport (passing through cells) * substances cross both apical and basolateral membrane
- Paracellular pathway (passing around cells) * substances pass through junction between two adjacent cells
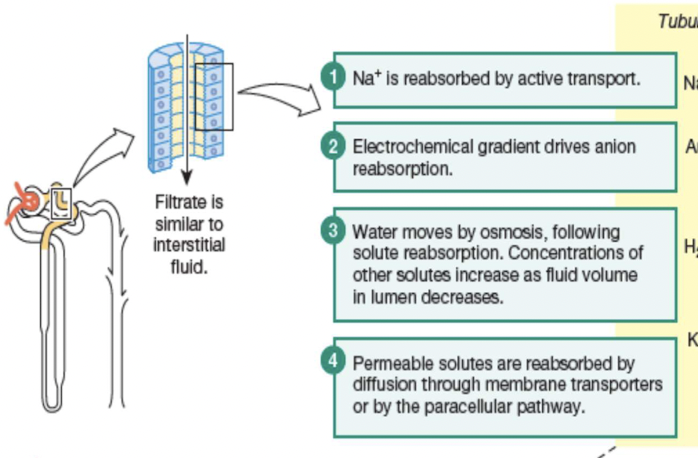
Principles governing the tubular reabsorption of solutes:
Some solutes and water move into and then out of epithelial cells (transcellular or epithelial transport); other solutes move through junctions between epithelial cells (the paracellular pathway). Membrane transporters are not shown in this illustration.
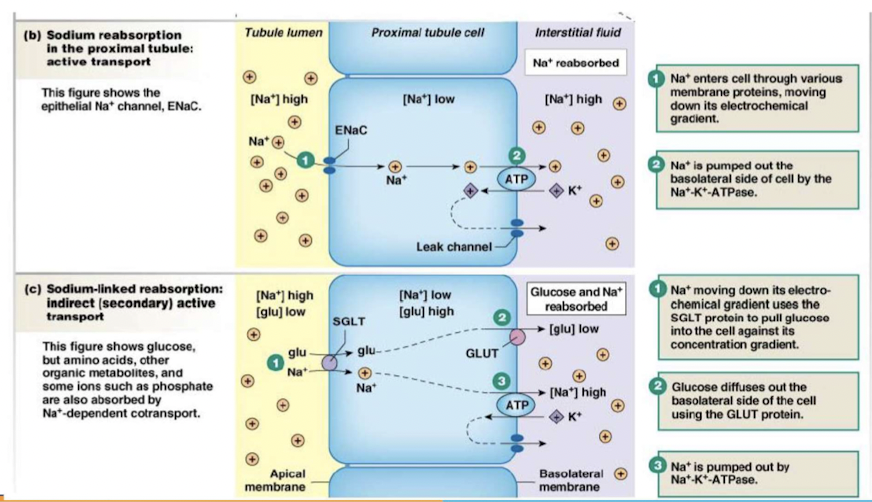
Secretion
Transfer of molecules from extracellular fluid into lumen of nephron:
- dependent on membrane transport proteins to move organic compounds
- active process move substrates against concentration gradient & use secondary active transport to move into lumen
- secretion of K+ and H+ is important in homeostatic regulation
- enables nephron to enhance excretion of substance * adds to substances collected during filtration, making excretion more effective
Fluid & Electrolyte Homeostasis
Water balance in the body
- Water makes up 50-60% of total body weight
- main entry of water is through food & drink
- most lost water in urine
- homeostasis maintains water balance unless there is pathology or an abnormal ingestion of water
Kidneys in water balance
- Kidneys cannot replenish lost water; only preserve or get rid of excess amounts
- volume loss replaced from the environment
- renal filtration will stop if there is a major loss causing extremely low blood pressure and blood volume
Urine concentration
- Osmolarity of urine measure of how much water is excreted by kidneys
- osmolarity changes as filtrate flows through nephron
- Diuresis - removal of excess water in urine * diuretics: drugs that promote urine excretion
- Kidney controls urine concentration * varying amounts of water and Na reabsorbed in distal nephron (distal tubule & collecting duct)
Osmolarity changes through nephron
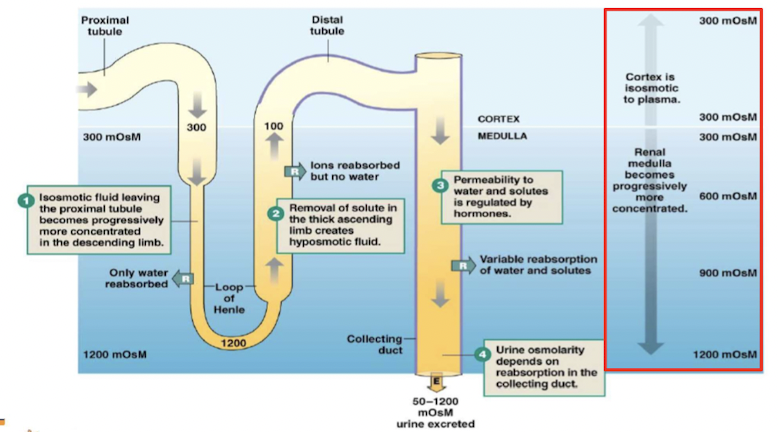
Countercurrent multiplier system
Exchange is enhanced by active transport of solutes
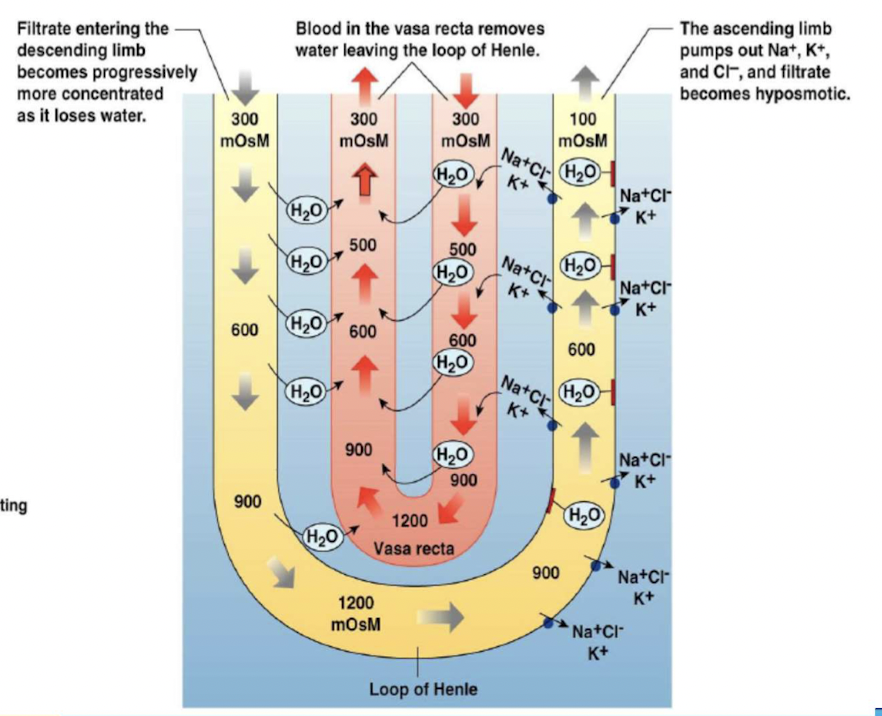
- Two components: * loops of Henle that leave the cortex, dip down into the more concentrated environment of the medulla, then ascend into the cortex again. * peritubular capillaries - vasa recta, also forming hairpin loops.
Water reabsorption
- Distal tubule and collecting duct cells alter permeability to water
- process involves adding or removing water pores (aquaporins) in apical membrane
- depends on secretion of vasopressin/antidiuretic hormone (ADH)
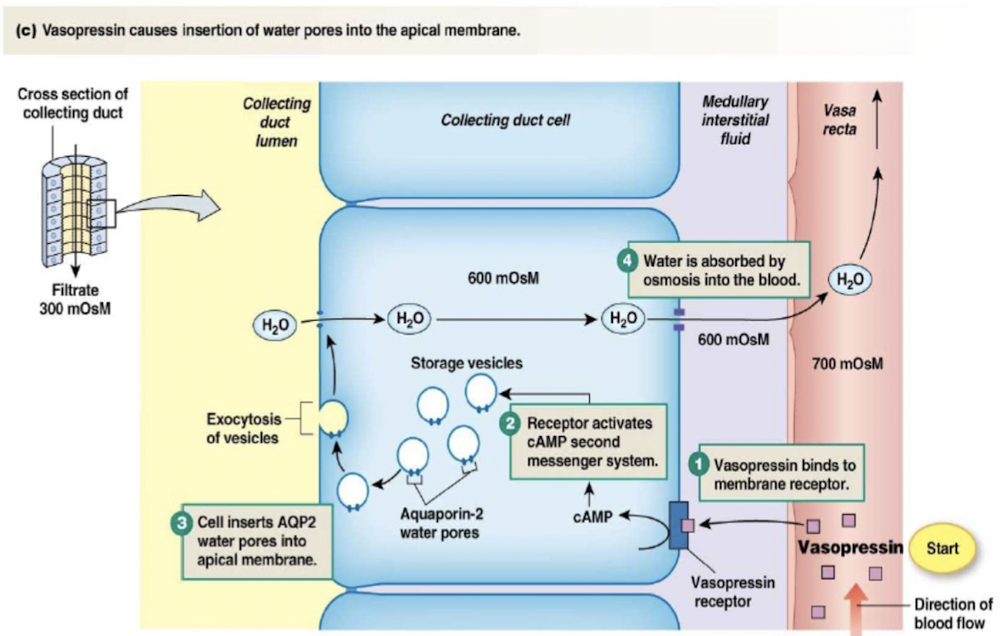
Control of vasopressin secretion
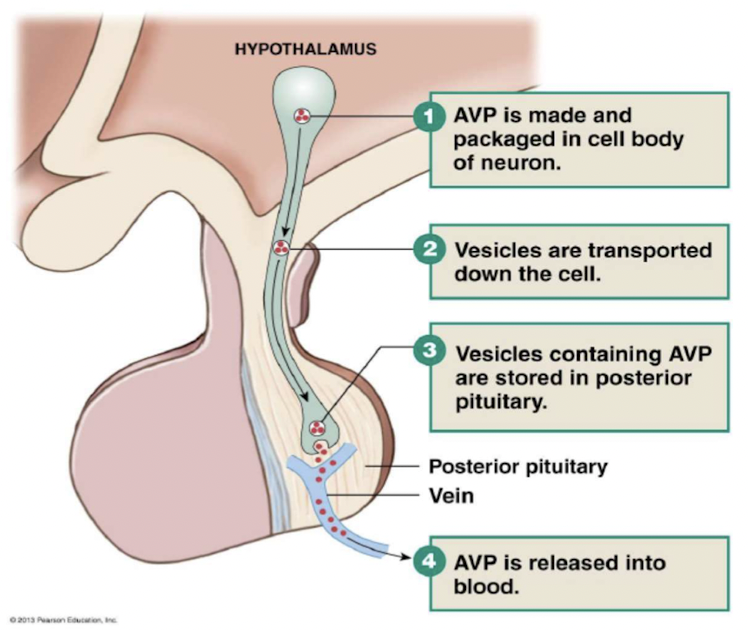
3 stimuli controlling vasopressin secretion:
- {{Plasma osmolarity > 280mOsM{{ * higher the osmolarity, more vasopressin released by posterior pituitary * osmoreceptors in hypothalamus detect changes in osmolarity
- {{Blood pressure{{
- {{Blood volume{{
Renin-Angiotensis-Aldosterone System (RAAS)
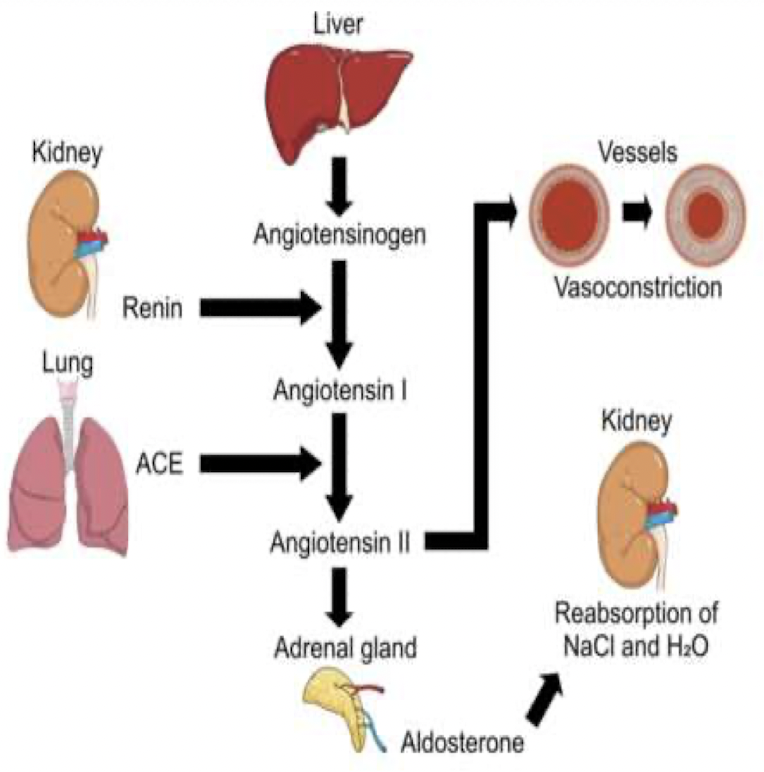
- Angiotensis II (ANG II) is the usual signal controlling aldosterone release from the adrenal cortex
- The RAS pathway begins when afferent arterioles secrete renin
- Renin converts inactive angiotensinogen, into angiotensis I (ANG I)
- ANG I converted into ANG II by angiotensis-converting enzyme (ACE)
- ANG II → adrenal gland → synthesis and release of aldosterone
- Aldosterone reabsorb Na+ at collecting duct
ACE2 & SARS-CoV-2 (COVID-19 Virus)
- ACE2 is present in many cell types and tissues including the lungs, heart, blood vessels, kidneys, liver and gastrointestinal tract.
- ACE2 is highly abundant on type 2 penumocytes in alveoli
- When the SARS-CoV-2 virus binds to ACE2, it prevents ACE2 from performing its normal function to regulate ANG II signalling
- ANG II increases blood pressure and inflammation, death of cells in alveoli
\ \ \