Behavioral Neuroscience - Neuropharmacology
- Neuropharmacology * the study of how substances affect our nervous system and behavior * one of the main areas of neuroscience research today * usually starts with animal research, once safety is established moves to human clinical studies * often (but not always) involves comparing active substances to a placebo (saline solution) * may use “active” placebo and may use double-blind research design
- Basic terms * Agonist --- increases NT activity * Antagonist --- decreases NT activity * Placebo --- an inert substance that is given to an organism instead of a physiologically active drug; used experimentally to control for the effects of mere administration of a drug * sometimes creates same effect as the drug
Research terms
- Half-life --- time it takes 1/2 of the drug to leave the body * used as a safety and maintenance factor * must examine drug “metabolites” as well as active ingredients * Drug metabolism: the process by which the body breaks down and converts medication into altered chemical substances * can be active or inactive * may not cause desired effect but affect other things; active = produce effect, inactive don’t * Elimination of a drug characterized by more than one half-lif every time half is eliminated = half-life * Time required for a drug concentration to reach steady state is determined by half-life * in most clinical situations, the attainment of steady state can be assumed after 3-5 half-lives * When the drug concentration is around 5% it is said to be negligible, therefore around 4 or 5 half-lives must elapse until the drug is eliminated * Time for drug “negligibility” = half-live * 5
- Dose-response curve
* a graph of the relationship between drug doses and the effects
* attempts to find effective and safe dose of drug
* can be used to plot the results of many kinds of experiments; X-axis usually drug/hormone concentration, Y-axis plots response (can be almost anything) \n
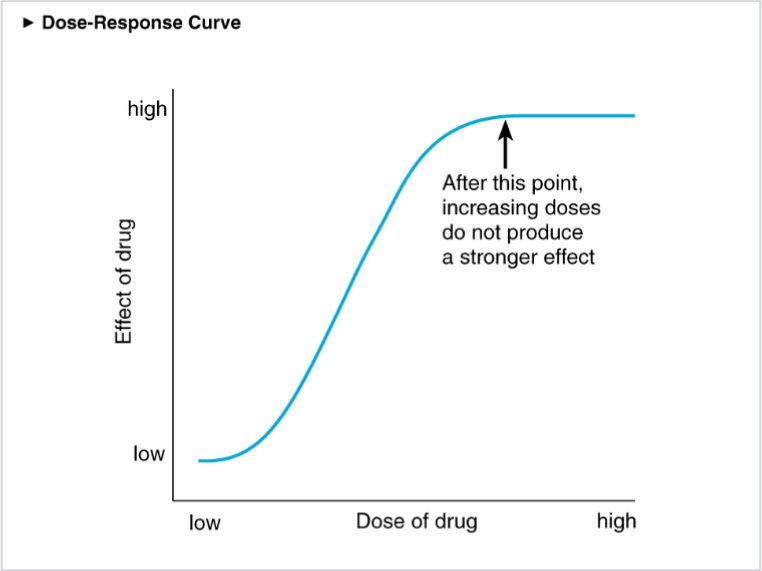 * the specific measurement (DV) will be defined b/c pharmacological agents can have multiple effects
* plots increasing drug dose (usually on a logarithmic scale) against increasing strength of the response being studied
* the dose at which the drug shows half of its maximal effect is termed the effective dose 50% (ED50)
* the specific measurement (DV) will be defined b/c pharmacological agents can have multiple effects
* plots increasing drug dose (usually on a logarithmic scale) against increasing strength of the response being studied
* the dose at which the drug shows half of its maximal effect is termed the effective dose 50% (ED50) 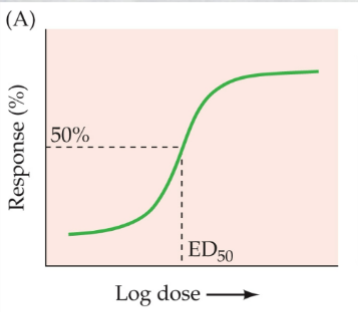 * Therapeutic window--- many drugs only work at specific doses; high and low often have little effect
* Nonmonotonic DRC --- a DRC that is normal up to a point but then reverses and the measured response begins to decrease with larger doses
* Therapeutic window--- many drugs only work at specific doses; high and low often have little effect
* Nonmonotonic DRC --- a DRC that is normal up to a point but then reverses and the measured response begins to decrease with larger doses 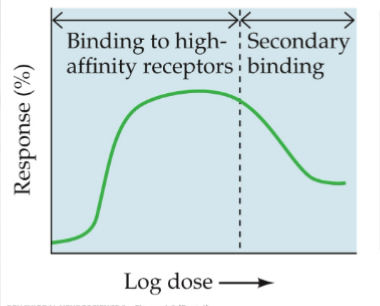
- Dose-response functions
* Minimum effective dose (ED50) --- lowest dose to produce desired effect in 50 % of clinical subjects
* Median Toxic dose (TD50) --- dose which produces the first signs of toxicity in 50% population
* high build-up in blood
* Threshold dose --- smallest dose to produce detectable change
* change must be defined by therapeutic effect
* We can assess the relative potency of two drugs by comparing their ED50 values
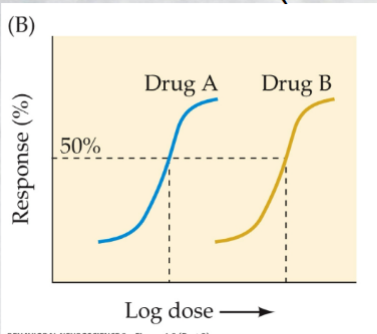 * Maximum response (max dose) --- the greatest degree of response that can be achieved with a specific drug
* usually there is a plateau effect past which further dose do not increase effect
* sometimes higher doses decrease effect (like amphetamines) because other effects begin to interfere with desired effect
* We can compare drug efficacies by evaluating maximal responses, rather than doses
* Partial agonist/antagonist - a drug of only moderate efficacy
* Therapeutic index (TI) --- the separation between the effective dose and a toxic one
* Safe index - ratio between TD50/ED50
* TI = 100x safe (over-the-counter), TI =10x hazardous
* becomes an issue with uncontrolled recreational use---tolerance to recreational effect occurs very quickly
* Maximum response (max dose) --- the greatest degree of response that can be achieved with a specific drug
* usually there is a plateau effect past which further dose do not increase effect
* sometimes higher doses decrease effect (like amphetamines) because other effects begin to interfere with desired effect
* We can compare drug efficacies by evaluating maximal responses, rather than doses
* Partial agonist/antagonist - a drug of only moderate efficacy
* Therapeutic index (TI) --- the separation between the effective dose and a toxic one
* Safe index - ratio between TD50/ED50
* TI = 100x safe (over-the-counter), TI =10x hazardous
* becomes an issue with uncontrolled recreational use---tolerance to recreational effect occurs very quickly - Clinical efficacy---refers to the degree to which a drug is able to induce a given effect * related to maximal response * DRC can allow the comparison of difference drugs
- Potency-- the amount of a drug needed to produce a desired effect * lower the needed dose, more potent
Drug interactions
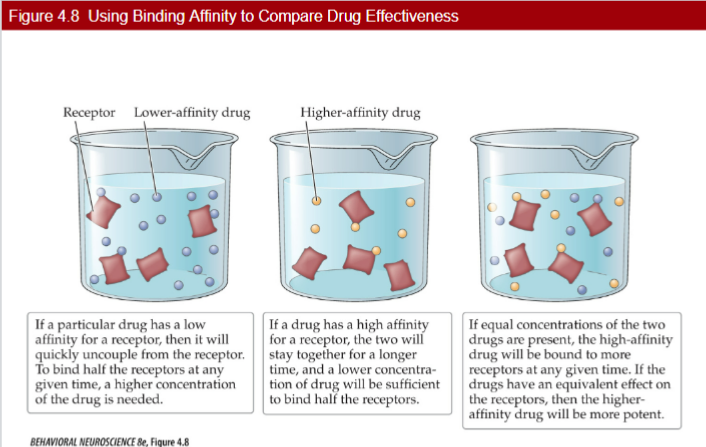
- Affinity - capacity of a compound (drug) to maintain contact or be bound to a receptor
- binding affinity = the degree of chemical attraction between a ligand and a receptor
* a drug with a high affinity for its receptor will be effective at very low doses
* when two substances are being taken, one with the most affinity will have greater effect
* penicillin and alcohol
Tolerance/Dependency
- Tolerance - when there’s a decreased susceptibility or increase in amount of drug being taken needed * represented by a rightward shift in the dose response curve * has a physiological and psychological component
- Factors * Metabolic tolerance --- organ systems become more effective at eliminating the drug * Elevation in Hepatic Microsomal Enzyme (HME) - reduces drug to metabolites so they become ineffective and easier to eliminate * ‘hepatic’ = liver * creates inactive and easier-to-eliminate metabolites * with repeated use of the brain creates more HMEs * associated with cross-tolerance to related substances * tolerance to once drug gives pre-existing tolerance to another (ex. surgical, analgesics, and narcotics) * creates dangerous interactions between drugs that share the same HMEs---sedatives and alcohol * biotransformation produces active metabolites that may produce side effects * Functional tolerance: target tissue may show altered sensitivity to the drug * up and down-regulation of receptors * with repeated drug use nervous sys can respond by altering the density of post-synaptic receptors * increase density = up-regulation, antagonist * lower density= down regulation; agonist
- Drug dependent
- Physical dependency: when
\