Hunger notes
Hunger and Thirst
Introduction
Fundamental Needs for Survival:
Hunger and thirst.
Israel Kamakawiwoʻole - ‘Izzy’
Career Overview: Iconic cover of ‘Somewhere Over the Rainbow’, reached #1 on the German singles chart in 2010.
Honors: Hawai'i State Flag flown at half-staff at his funeral, a unique honor for a private citizen.
Physical Struggles: Struggled with obesity, weighing up to 757 pounds.
Death: Passed away at age 38 from heart failure in 1997.

Homeostasis and Thirst Mechanisms
Negative Feedback Systems
Definition: Main mechanisms for homeostasis.
Behavioral Response: Actions like eating and drinking occur when deviating from a set point.
Thirst Types
Osmotic Thirst: Triggered by high extracellular solute concentration.
Hypovolemic Thirst: Triggered by low extracellular/intravascular volume.
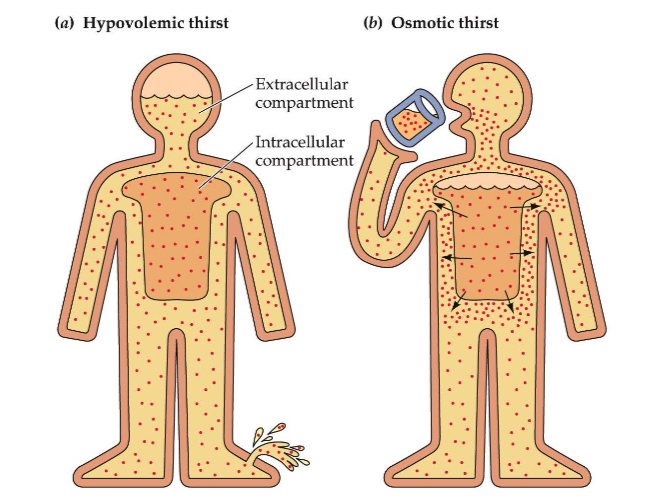
Mechanisms of Hypovolemic Thirst
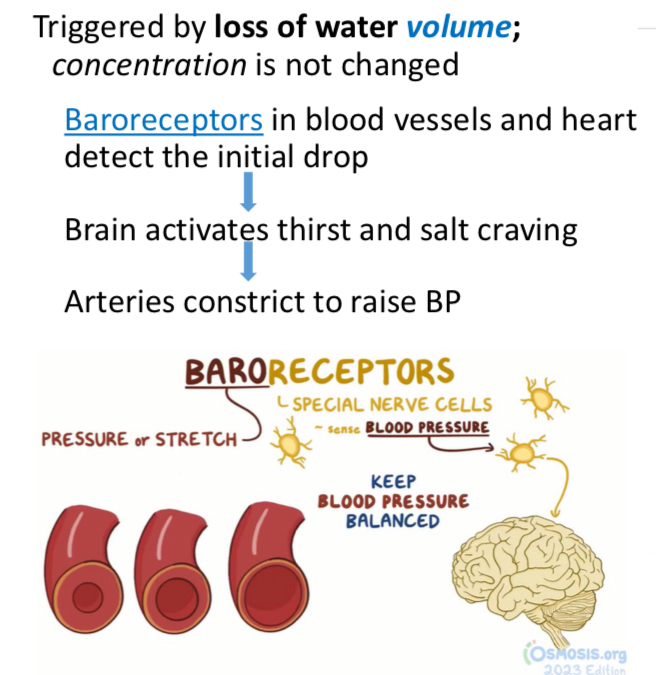
Detection: Baroreceptors in blood vessels and heart sense decreased water volume.
Response: Brain activates thirst and salt craving; arteries constrict to elevate blood pressure.
Hormonal Response
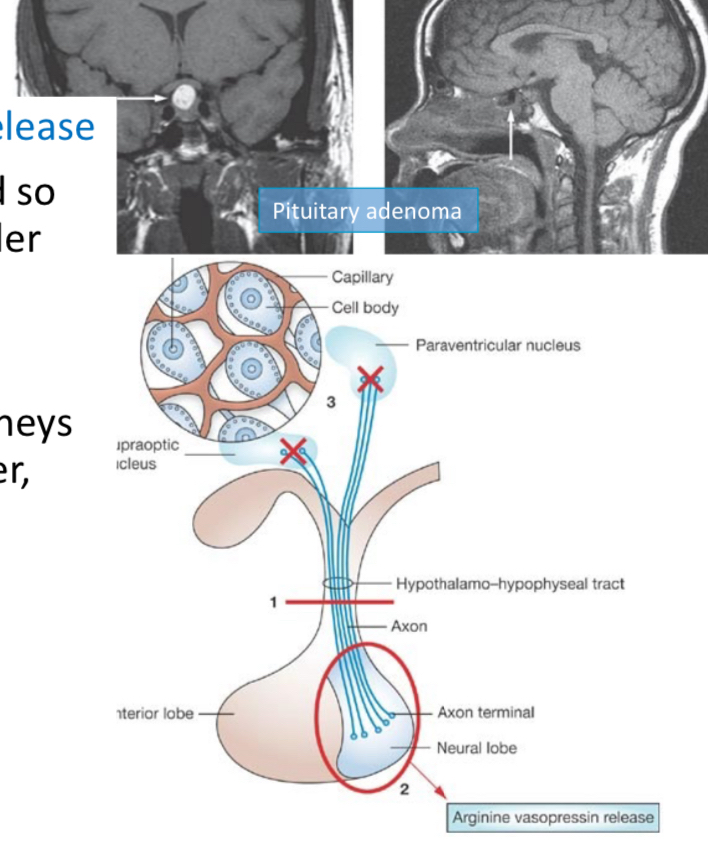
Vasopressin: Released during hypovolemia; constricts blood vessels and reduces urine output.
Vasopressin deficiency: MEANS INCREASE URINE OUTPUT TO KIDNEYS, resulting in chronic thirst
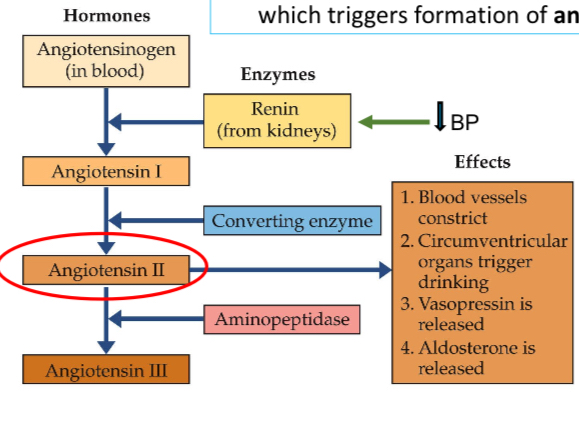
Angiotensin Cascade Process: Low blood volume triggers renin release from kidneys, producing angiotensin II, causing blood vessel constriction and stimulating drinking.
Brain Control of Drinking
Mechanism: Angiotensin II acts in the subfornical organ(Angi 2 has to be released in this region) signaling brain areas for drinking behavior.
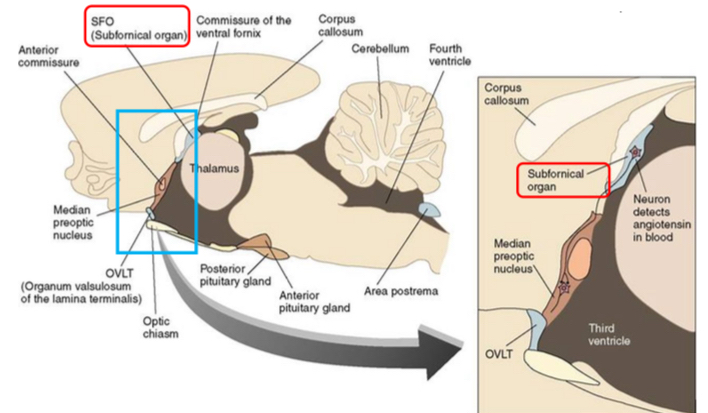
Osmotic Thirst Mechanism
Process: Osmosensory neurons in the anterior hypothalamus(OVLT) respond to increased blood osmotic pressure(salt). Na+ channels open as membranes shrink; neurons activate pituitary to release ADH.
Because there is so much salt outside the cell, the cell releases water to balance outside
ADH stimulates thirst center
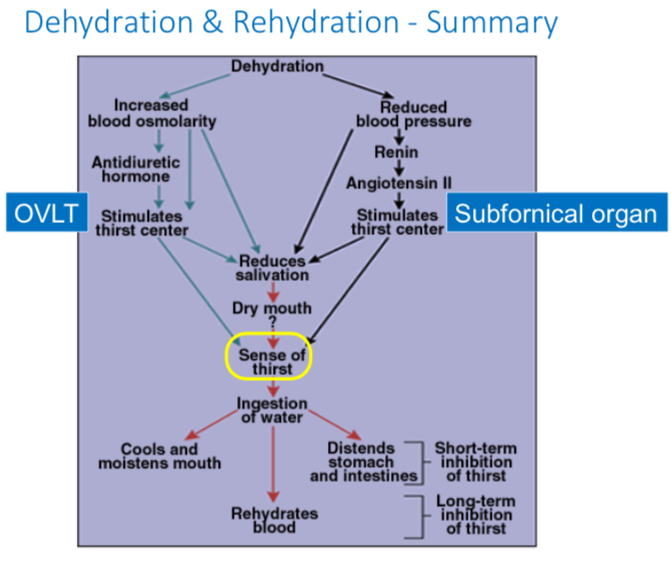
Dehydration & Rehydration Summary
Increased blood osmolarity prompts ADH release, leading to thirst and dry mouth. Drinking water rehydrates blood and reduces salivation.
OVLT neuron and subfirnical region stimulate thirst center
Hunger Awareness
Cultural Quotations: Complexities of managing hunger.
Dieting Challenges
Metabolism Adjustment: Energy expenditure declines when dieting, reducing basal metabolic rate (BMR). Longevity studies show restricted food intake may benefit rats but are uncertain for humans.
Obesity and Metabolism
BMR: Energy needed for basic functions, comprising 75% of daily energy for sedentary students; genetics also play a role.
Energy Storage and Utilization
Primary Energy Source: Glucose; glycogen serves as short-term storage.
Metabolic Rate Insights: Peaks in infancy, slows in youth, stabilizes until age 60, then declines.
Food Intake Regulation
Neurotransmitter Influences: Brain signals (NPY, a-MSH) regulate hunger and satiety, influenced by hormones and nutritional status.
Leptin and Ghrelin
Leptin: Produced by fat cells; informs the brain about body fat. Resistance leads to obesity.
Ghrelin: An appetite stimulant, elevated during fasting, low post-eating; dysregulated in Prader-Willi syndrome.
Hypothalamus and Appetite Control
Dual Functionality: Two neuron types exist; one stimulates appetite (NPY/AgRP) and the other inhibits it (POMC/CART).
Obesity Effects on Brain
Consequences of Overeating: Leads to hypothalamic inflammation, inhibiting neurogenesis and resetting hunger signals.
Eating Disorders
Anorexia Nervosa
Criteria: Refusal to maintain body weight, intense fear of weight gain; highest mortality rate among psychiatric disorders.
Bulimia
Criteria: Characterized by recurrent binge eating and inappropriate behaviors to counter it.
Co-occurrence with Other Disorders
High anxiety and depression rates associated with anorexia and bulimia; significant suicide rates among afflicted individuals.
Children and Eating Disorders
Survey reveals concerning rates of dieting and disordered eating behaviors among students in grades 5 to 8.
Treatment of Obesity (Effective Strategies)
Eating Habits:
Creating a caloric deficit of 200 calories/day requires lifestyle changes and monitoring.
Exercise:
Engaging in more than 200 minutes of strenuous aerobic activity weekly is effective combined with dietary changes.
New Drug Treatments
GLP-1 receptor agonists: Drugs like Mounjaro and Ozempic show significant long-term weight loss effects by modulating appetite and metabolic responses.