Unit 3 Cram Sheet || MedInt PLTW
3.1
Detecting Cancer
Cancer is the second leading cause of death in the United States, second to only heart disease.
Half of all men and a third of all women will develop cancer in their lifetime.
Cancer can affect any part of the body.
Normal Cells
uniform (the same)
same number of nuclei
similar shapes and sizes
large cytoplasm
fine chromatin
Cancer Cells
abnormal cells in which the processes that regulate normal cell division are damaged
can appear to have:
— multiple nuclei
— an abnormal number of chromosomes
— irregular shapes and sizes
— small cytoplasm
— coarse chromatin
may appear to grow on top of each other
not uniform in configuration
genes that would normally regulate cell behavior are mutated.
Common Tools for Detecting Cancer
most cancers are initially recognized when signs or symptoms appear.
X-rays
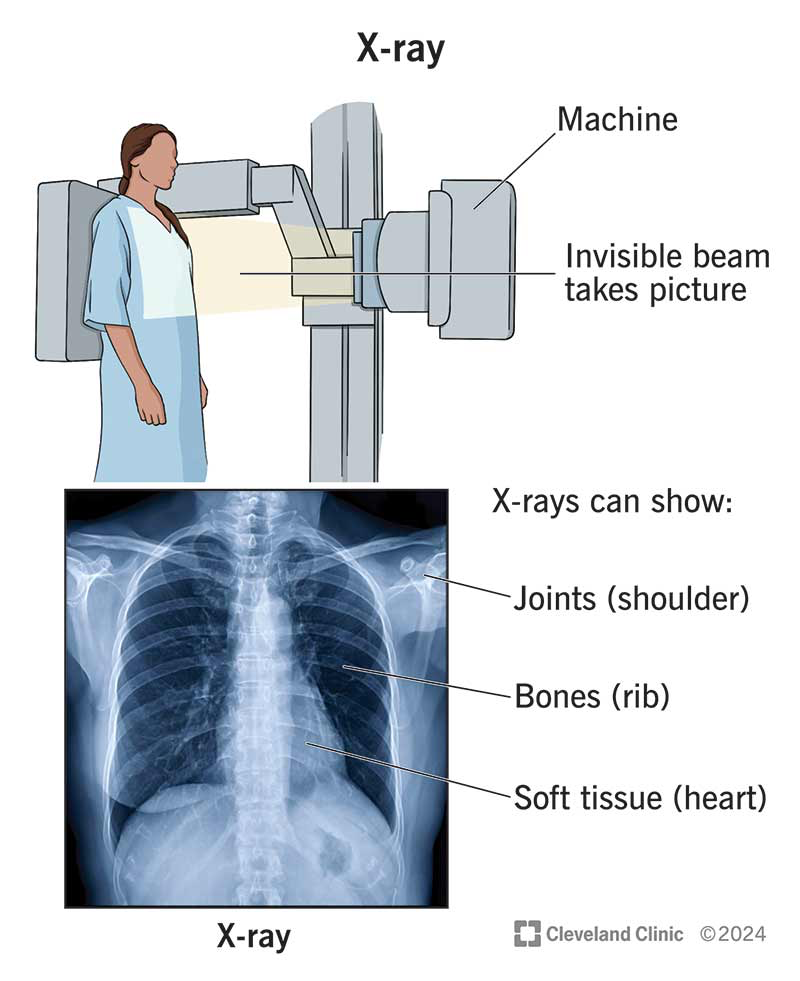
work by passing electromagnetic waves through the body
non-invasive medical test used to produce images of the inside of the body to help diagnose medical conditions.
electromagnetic waves pass easily through soft tissues and absorbed by hard tissues, such as bones, making them appear on an x-ray film.
special dyes used to highlight areas of the body
uses iodizing radiation
two-dimensional images
CT Scans
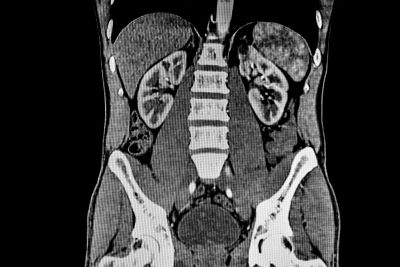
Computed Tomography (CT) Scans are specialized X-rays
noninvasive
patient lies down and an X-ray machine is rotated around their body, forming a three-dimensional image.
sensitive in detecting diseases that are in internal organs.
can image bone, soft tissue, and blood vessels.
can be used on patients with medical devices.
uses ionizing radiation
uses dyes
MRIs

Magnetic Resonance Imaging (MRI)
do not use X-rays
uses radio waves that are sent into the gody and collects the signal that is emitted from the hydrogen atoms in the cells
detailed images of soft tissue
3d
images are cross-sections
uses dyes
Bone Scans

noninvasive
produces images of only bones
used to track progression of different bone diseases
injects radioactive material
2d
Biopsies
test for nearly every type of cancer
involved removing a small sample of tissue from the body
invasive
tests are performed on biopsy
look for abnormalities in the cell
Detecting Genes Involved in Cancer
a key difference between cancerous cells and healthy cells is the number of genes turned on
compare gene expression through the use of DNA microarray technology
every cell in the body contains the same 20,000 genes (*with the exception of RBCs, which contain no DNA)
not every gene is active in every cell
genes are only turned on in the cell that is supposed to perform that function
mRNA is only produced in a cell when the cell is constructing a protein, so if mRNA is produced from a gene, we can assume that this gene is turned on.
DNA Microarrays
scientists use DNA microarrays to scan multiple genes at a time and measure gene expression for each gene.
microarrays are glass, plastic, or silicon slides that have been spotted with thousands of short segments of DNA.
segments of DNA are single-stranded and contain a piece of the gene of interest
Process of developing a DNA microarray slide:
A gene thought to be involved in a particular type of cancer is located within the human genome sequence. (the portion of the gene of interest is located)
Primers are designed to run PCR reactions that will make copies of the portion of the gene of interest
The double-stranded DNA from each DNA copy is separated into single strands.
Microscopic droplets of each single-stranded DNA sample are placed onto a specific spot on the microarray slide.
The first four steps are followed to produce single-stranded DNA samples for each gene of interest the researcher wants to investigate. these samples are spotted in ordered rows and columns on the microarray slide.
Computers are used to keep track of all the gene spots on the microarray and ensure that each spot contains equal amounts of DNA.
Once the slide is created, it can be used for a microarray experiment. This begins with a process to separate the DNA, proteins, and RNA.
- The samples are washed over small beads that attract mRNA only.
- A cDNA (complementary DNA) strand must be created that is fluorescent.
- Once the samples are made, they are added to the microarray slide.
For every molecule of cDNA, there is a matching spot of single-stranded DNA on the microarray.
- When the two find each other, they base pair and hybridize together, and become bonded.
- Anything that does not bond is washed off, then the microarray is put through a scanner that picks up the fluorescent dye in the cDNA.
This gives data about gene expression in healthy tissue and cancer tissue from the same patient.
A saturated green color indicates that the gene is highly expressed in healthy cells.
A saturated yellow color indicates that a gene is highly expressed in both healthy and cancerous cells.
A saturated red color indicates that a gene is highly expressed in cancerous cells.
A black color/clear (*depends on type of microarray) indicates that this gene is not expressed in that particular cell.
3.2
Risk Factors and Simple Prevention
Behavioral Risk Factors
Behaviors that you can actively change
smoking, diet, exercise, etc.
Environmental Risk Factors
Toxins found in your surrounding environment that increase your cancer risk
lead, radon, asbestos, etc.
Biological Risk Factors
Physical characteristics
Age, gender, race, etc.
Genetic Risk Factors
Inherited genes
Mutations causing cancer
mutations lead to changes in a cell’s life process
Chemicals, UV, age, etc. can cause changes at the DNA level or people can just be born with incorrect genes
Tumor Suppressor Genes
A gene that suppresses cancer
work inside of cells
if cells become abnormal (example; p53) tumor suppressor genes work to correct the process.
if not possible, triggers apoptosis (death of the cell)
when mutated or changed, these can cause cancerous cells to go unchecked.
Proto-oncogenes
a group of genes that cause normal cells to become cancerous when they are mutated.
encode proteins that function to stimulate cell division, inhibit cell division, and halt cell death
BRCA1 & BRCA2
Oncogenes
mutated (cancerous) version of a proto-oncogene
exhibit increased production of these proteins, leading to increased cell division, decreased cell differentiation, and inhibition of cell death
tumor suppressor genes may not be able to identify these as harmful
Marker Analysis
a technique where the gene mutation is analyzed using a genetic marker instead of directly analyzing the gene itself.
a genetic marker is a short sequence of DNA associated with a particular gene or trait with a known location on chromosome.
STRs (Short Tandem Repeats | microsatellites)
the genetic markers used in marker analysis are short DNA sequences called STRs.
a region of DNA composed of a short sequence of nucleotides repeated many times.
the number of repeated STRs var from person to person
the alternative forms of a given STR correspond with different alleles.
the more repeats present in an STR, the longer the DNA fragment will appear.
3.3
Radiation Therapy and Chemotherapy
Radiation Therapy
used to target and kill leftover cancer cells in the area where the mass was found.
works to “clean” cancerous material out of the area where the tumor was found
considered a “local” treatment; it only affects the area where the tumor was located
can be used to kill cancer without surgery in some cases
radiation works with a beam of high-energy rays that destroy or slowly kill the growth.
possible to insert radioactive pellets near the cancerous site
Chemotherapy
systematic treatment that is designed to destroy and cancer cells that may have metastasized (moved) and spread throughout the body
drugs are inserted directly into the bloodstream and travel throughout the body
given in cycles with recovery periods in-between
more side effects
Biofeedback Therapy
a technique used to make unconscious or involuntary processes (like heartbeat or brain waves) perceptible to the senses in order to manipulate them by conscious control.
involves learning how your body responds to stimulus such as pain or fear.
yoga, meditation, breathing, etc.
Amputation and Prosthetics
during an amputation procedure, whatever possible bone is removed and the remaining tissues reshaped to form a well-rounded stump that can be outfitted with a prosthetic.
a prosthetic device can allow patients more freedom and independence
prosthetics require a loot of maneuverability