sleep
8A
Partial Sleep Deprivation
- Inadequate sleep in terms of quantity or quality.
- Sleep quantity refers to the duration of sleep.
- Sleep quality refers to the quality of sleep.
- Factors contributing to sleep deprivation include:
- Consumption of caffeine, food, drugs, alcohol.
- Work or school requirements.
- Failure to wind down before bed.
- Stress.
- Medical conditions.
- An uncomfortable sleeping environment.
- Social influences.
Negative Effects =
- Negatively impacts affective, behavioural, and cognitive functioning.
- Poor concentration leads to increased clumsiness, causing frustration.
Affective functioning
- a person’s experience of their emotions
- Emotions experience can be influenced by sleep deprivation.
- Symptoms include mood swings, emotional outbursts, sadness, depression, irritability, and crying.
- Over-annoyed responses to household chores may occur.
Behavioural functioning
- a person’s observable actions
- Sleep deprivation can lead to difficulty controlling behaviour, increased risk-taking, and impulsiveness.
- It can also reduce productivity and work efficiency.
- Children may exhibit hyperactive behaviour and increased misbehaviour.
- Sleep deprivation can cause difficulties following class rules and 'naughty' behaviour.
Cognitive functioning
- a person’s mental processing
Sleep Deprivation and Cognitive Functioning Issues:
- trouble with memory
- decreased alertness
- poor concentration
- impaired problem solving, decision making
- poor judgement
- lack of motivation
- trouble coping with change or stress
- difficulty learning new concepts
- slower thinking
- a shortened attention span.
- Example: Difficulty concentrating and remembering theory during Maths tests.
(BAC)
- Blood alcohol concentration
- the percentage of alcohol in the bloodstream
- Alcohol has harmful effects on the brain and body, leading to laws limiting blood alcohol concentration (BAC) for driving. In Victoria, the legal BAC is under 0.05%.
- A BAC level above this limit negatively affects affective and cognitive functioning, increasing as BAC increases. A study found that 17 hours of sustained wakefulness equivalent to a BAC of 0.05% or 0.10%, respectively.
Study Highlights Driving Dangers
• Importance of community understanding of sleep-deprived driving.
• Similar effects to intoxicated driving.
• Longer wakefulness over 17 hours is concerning.
• Effects of sleep deprivation are worse than legal BAC limit in Australia.
Sleep deprivation can lead to cognitive functioning issues such as:
- memory problems
- decreased alertness
- poor concentration
- impaired problem-solving
- poor judgement
- lack of motivation
- coping with change
- difficulty learning new concepts
- slower thinking
- and a shortened attention span.
8B
DSM-5-TR Sleep-Wake Disorders
- Categorizes sleep-wake disorders into 10 groups: insomnia, breathing-related sleep disorders, substance/medication-induced sleep disorder, and circadian rhythm sleep-wake disorders.
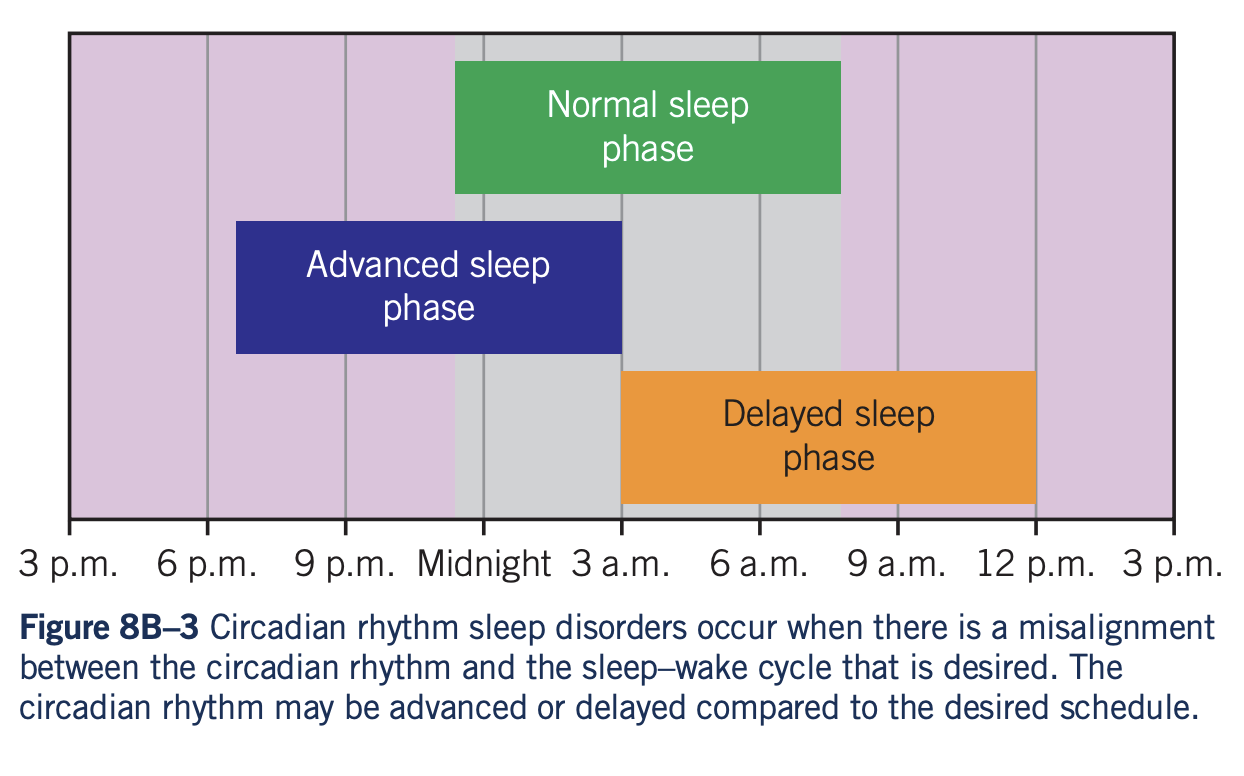
- Circadian rhythm sleep disorders are characterised by a persistent pattern of sleep disruption due to a misalignment between the circadian rhythm and the sleep-wake schedule.
- These disorders can cause excessive sleepiness, insomnia, distress, or impairment of functioning.
Three types of circadian rhythm sleep disorders:
- Delayed Sleep Phase Syndrome
- Advanced Sleep Phase Disorder and shift work.
- Treatment involves bright light therapy, which resets the sleep-wake cycle and promotes wakefulness.
- The ideal light source can be a safe but artificial source, a desk lamp, floor lamp, visor hat with attached light, or natural sunlight.
(DSPS) Delayed Sleep Phase Syndrome
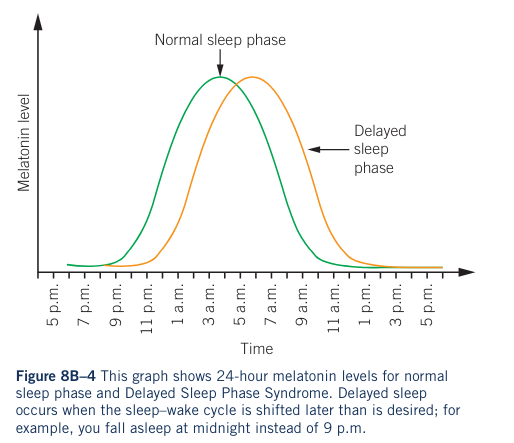
- DSPS is a circadian rhythm sleep disorder characterised by a delay in sleep onset and awakening.
- The delay is usually for two or more hours, leading to a person falling asleep later than what is conventionally accepted.
- This delay results in a need to wake up later than required for adequate sleep.
- The delay contributes to a sleep disorder when a person cannot achieve their recommended amount of sleep due to work, school, or other commitments.
- DSPS typically results in a shifted circadian rhythm, preventing a person from falling asleep at a more acceptable time.
- Diagnosis requires symptoms for more than three months.
Delayed Sleep Phase Syndrome (DSPS) Risk Factors
- Longer than average circadian period and increased light sensitivity are predisposing factors.
- Sensitivity to evening light may delay night-time signals to the suprachiasmatic nucleus, affecting melatonin release.
- Less sensitivity to morning light results in less melatonin release.
- Lifestyle adjustments can reduce sleep deprivation and symptoms.
- Bright light therapy can help shift circadian rhythm to a more suitable time.
Early Morning Light Exposure and Sleep Cycle Reset
- Reduces melatonin release earlier in the morning.
- Resets circadian rhythm, promoting sleepiness.
- Requires limiting night-time light exposure and gradually increasing bedtime.
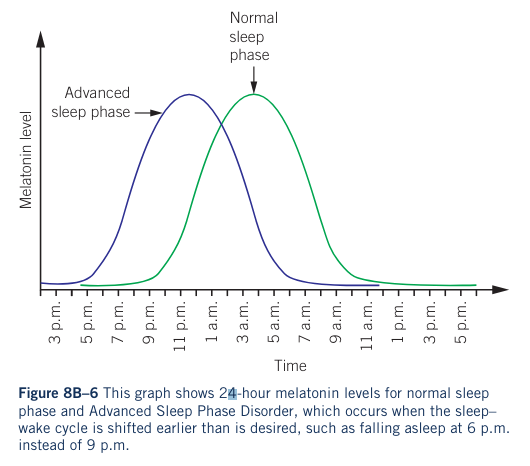
Advanced Sleep Phase Disorder (ASPD)
- A circadian rhythm sleep disorder characterised by an advance in sleep onset and awakening timing.
- Individuals may fall asleep two or more hours earlier than desired, leading to earlier waking times.
- Example: Sleeping from 8 p.m. to 4 a.m. instead of 10 p.m. to 6 a.m.
- Attempts to adhere to a more reasonable, later bedtime result in an early wake time due to the shift in circadian rhythm.
Adverse Light Exposure and ASPD
- Adverse light exposure can maintain advanced circadian rhythm, affecting sleep and wake patterns.
- Early bedtime and wake times prevent exposure to evening low and morning bright light signals, perpetuating the disorder.
- Symptoms of ASPD become more severe when work or social demands disrupt the natural sleep-wake cycle.
- Adjusting daytime sleep and wake schedules can lead to stable sleep patterns and reduced symptoms.
- Bright light therapy can help shift circadian rhythm to a more appropriate time, reducing sleepiness and resetting the sleep-wake cycle.
Shift Work
- Shift work can cause a circadian rhythm sleep disorder, especially in professions like healthcare, hospitality, factory work, transport, and travel.
- This disorder results in distress due to excessive sleepiness at work and impaired sleep at home after shift.
- It affects 5-10% of the population working during nights, especially at the middle-aged stage.
- Consequences include poor performance, interpersonal problems, increased risk of accidents, and poor mental wellbeing.
- Prolonged shift work is linked to physical health problems like gastrointestinal disorders, cardiovascular disease, diabetes, and cancer.
- Symptoms reduce when a person spends longer on one shift rotation before changing.
- Ideally, shift forward from morning to afternoon shift, to evening shift.
- Bright light therapy can help adjust circadian rhythm to suit work schedules.
8C
Improving Health through Sleep and Exercise
- Healthy diet, regular exercise, and adequate sleep are the three pillars of health.
- Poor sleep patterns are linked to physical health issues like diabetes, weight problems, hypertension, cardiovascular disease, and mental health issues like depression, bipolar disorder, anxiety disorders, and schizophrenia.
- Despite these health risks, many prioritise sleep less than healthy eating and exercise.
- Improving sleep hygiene involves avoiding devices and caffeine before bed, following a wind-down bedtime routine, minimising light and noise, ensuring a cool temperature, and having comfortable bedding.
Sleep Hygiene and Wellbeing
- Consistent sleep hygiene promotes faster and quality sleep.
Zeitgebers
- environmental cues like light, temperature, and eating patterns.
- These cues synchronise and regulate the body's circadian rhythm.
- They can shift the 24-hour sleep-wake cycle, improving mental wellbeing.
Daylight
- Daylight, both direct and indirect, is the primary zeitgeber for human circadian rhythm.
- Light's detection by the suprachiasmatic nucleus in the brain influences the release of melatonin by the pineal gland.
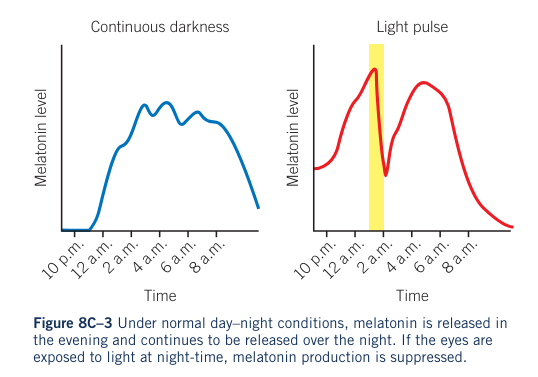
- Increased light levels suppress melatonin production, promoting wakefulness.
- Decreased light levels increase melatonin release, promoting sleepiness.
Circadian System and Artificial Lighting
- The Circadian system's ability to resynchronize daily with the external environment is evolutionary.
- Artificial lighting allows 24-hour access to light, enabling nighttime activities previously restricted to daytime.
- Blue light, emitted from smartphones, computers, TVs, LEDs, and the Sun, significantly influences circadian rhythm.
- Blue light inhibits melatonin, affecting sleep quality and quantity.
- Unintentional blue light exposure can lead to sleep disorders and poor mental and physical wellbeing.
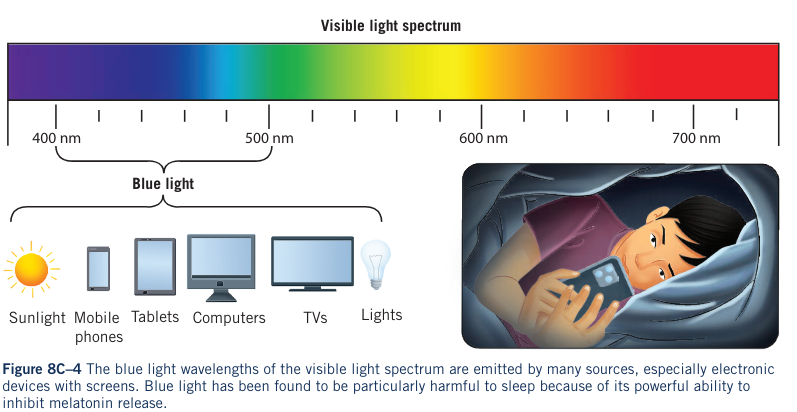
Influence of Light on Sleep and Wellbeing
- Individuals can influence their light exposure to shift disrupted sleep-wake cycle and improve mental wellbeing.
- Healthy individuals should expose themselves to natural daylight in the morning and throughout the day.
- Blocking out artificial light, especially blue light, at night before sleep can reinforce a regular sleep-wake cycle.
- Ways to avoid blue light include using in-built screen filters, 'night mode' settings, reducing screen brightness, or not using screens before bed.
- Dimming LED room lights, using red or orange lamps, or using glasses blocking blue light can also reduce sleep disturbances.

- Circadian rhythm sleep disorders can be managed by strategically using light.
- Night shift workers can increase blue light during work hours and minimize daylight exposure during sleep.
- Blue light can enhance wellbeing by keeping individuals alert, improving performance, and mood.
- Factors to consider include duration, intensity, color, and time of day.
- Exposure to daylight during waking hours and strategic use of blue light can regulate the sleep-wake cycle, leading to restful sleep and positive mental wellbeing.
- Emerging theories suggest light affects other brain areas that regulate mood, independent of its impact on the sleep-wake cycle.
Improving Sleep-Wake Cycle through
Temperature
- Temperature is a zeitgeber for sleep-wake cycle, regulated by the suprachiasmatic nucleus.
- Body temperature decreases in the early evening, with sleep onset occurring when core body temperature is at its highest.
- Increased blood flow to the skin causes skin warming, reducing body temperature.
- The lowest body temperature occurs about 2 hours after sleep onset.
- Skin warming initiates sleep, supported by bedding use, animal curling up, and nest building.
- Neural pathways promoting NREM sleep and body cooling are linked.
- Increase in melatonin coincides with decrease in core body temperature leading to sleep onset.
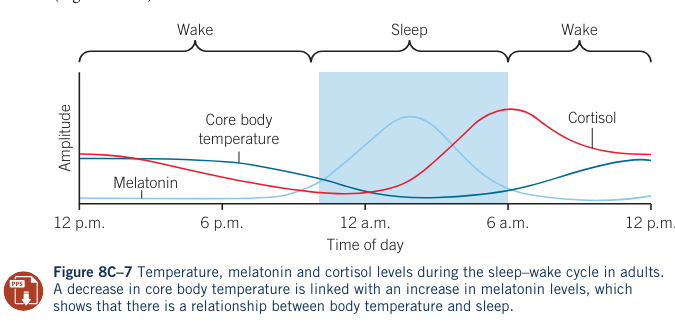
Sleep Orientation and Microclimate
- Ideal room temperature for sleep onset: 19–21°C.
- Ideal skin and bed microclimate for sleep: 31–35°C.
- Strategies include windows, fans, appropriate bedding, sleepwear, curtains, and mattress and pillow.
- Elderly individuals may benefit from these strategies due to difficulties with thermoregulation.
- Skin warming can restore age-related decrease in deep sleep and reduce early morning awakening.
- Temperature regulation improves sleep-wake cycle consistency and mental wellbeing.
Eating and Drinking Patterns and Circadian Rhythm
- The suprachiasmatic nucleus is the primary circadian rhythm keeper, influenced by light and food intake.
- It is not significantly impacted by meal timing, but can be affected by severe food deprivation, calorie restriction, and perceived starvation.
- Other peripheral body clocks, acting alongside the suprachiasmatic nucleus, receive daily resetting signals from the suprachiasmatic nucleus and are influenced by other zeitgebers, including meal timing.
- For optimal energy balance, peripheral clocks should be synchronised with the suprachiasmatic nucleus.
- Altering meal timing to the inactive, dark phase of the 24-hour cycle can disrupt the normal functioning of the body clock, disrupting the suprachiasmatic nucleus.
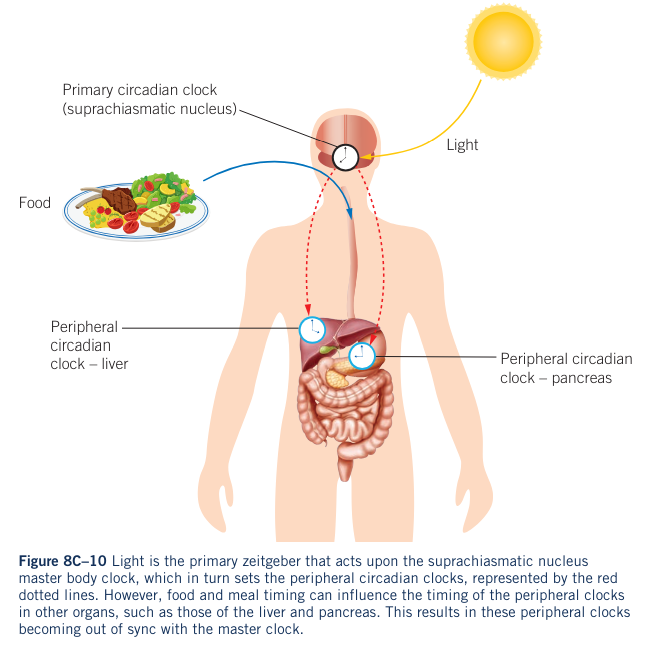
Shifting Circadian Rhythms and Metabolic Disorders
- Shifting circadian rhythm due to food consumption and low light exposure can disrupt the sleep-wake cycle.
- Shift workers and those with constant food availability may be affected by conflicting meal timings.
- Modern lifestyle influences, such as constant food availability, reduced sleep, longer active hours, and socially dictated behaviour, can lead to metabolic disorders like weight gain, obesity, and type 2 diabetes.
- Eating meals within 3-4 hours of sleep onset can negatively affect sleep quality and increase onset time and awakenings.
- Increased caffeine consumption correlates with increased sleep problems, including morning tiredness, increased awakenings, restless sleep, and reduced sleep quality.
- Dietary interventions can help reduce health problems and improve the sleep-wake cycle.
- Limiting caffeine intake later in the day and not eating right before sleep can improve sleep onset and quality.
- Resetting mealtimes during the active, light phase of the day and leaving a long fasting window during the inactive phase of night can help resynchronize peripheral clocks with the suprachiasmatic nucleus.