Chapter 3: Histology
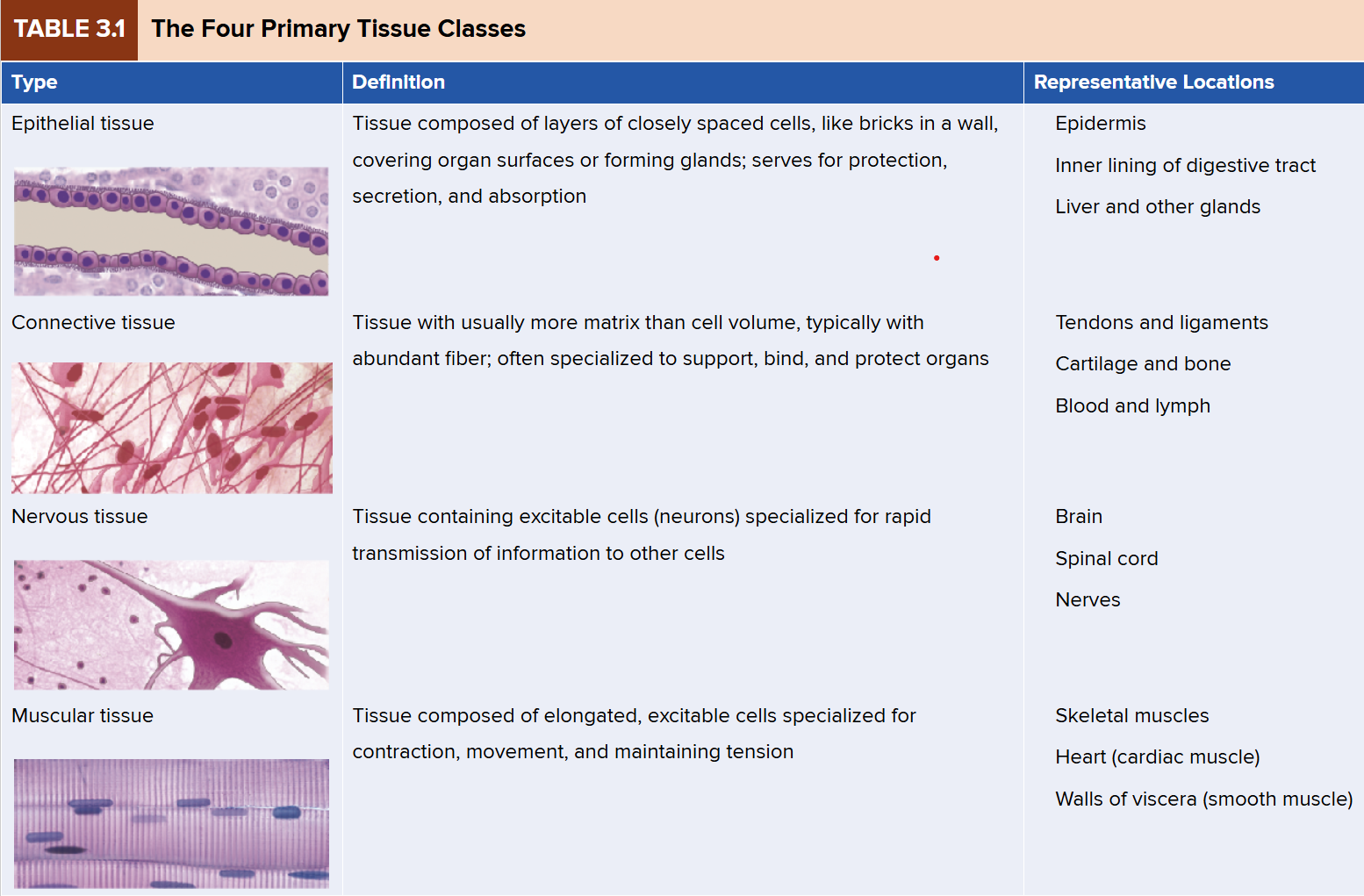
Epithelial Tissue
covers organ surfaces, forms glands
protection, absorption, secretion
Characteristics
1+ layers
closely adhered cells
Avascular - no blood vessels passing through
form surfaces
Basement membrane delivers nutrients
basal surface connects to basement membrane
apical surface is the “upper” part of the cell
Classes of Epithelium
simple
every cell is connected to basement membrane
simple cuboidal, simple, cuboidal, simple columnar,
pseudostratified columnar
connected to basement membrane
goblet cells - specialized columnar cell that produces mucin
stratified
two or more layers
named by shape of the top layer
stratified squamous, stratified cuboidal, urothelium (transitional)
Cell Shapes
Squamous
Cuboidal
Columnar
Simple Squamous
Simple Cuboidal
single layer of square/round cells
glandular
often with brushed border
absorption and secretion
representative locations: liver, bronchioles, kidney tubules, most glands
Simple Columnar
nucleus is elongated and oriented towards basal surface
tend to have microvilli
may possess goblet cells
representative locations: stomach lining, intestines, gallbladder
absorption secretion of mucus, movement of egg/embryo in uterine tube
Pseudostratified Columnar
looks multilayered, but all cells attach to basement membrane
often with goblet cells
often ciliated
representative locations: URI (nasal cavity → bronchi)
portions of male urethra
secretes and propels mucus
Keratinized Stratified Squamous Epithelium
multiple cell layers becoming increasingly flat and scaly towards surface
surface coverd with compact dead cells w/out nuclei
Non-keratinzed stratified squamous epithelium
same as keratinized epithelium but without surface layer of dead cells
resists abrasion and penetration by pathogenic organisms
representative locations: tongue, vagina
Stratified Cuboidal
two or more layers of cells, surface cells roughly square or round
sweat glands, ducts
Urothelium (Transitional Epithelium)
can distend without damage
urinary tract
protects underlying tissue from osmotic and acidic effects
Connective Tissue
more matrix than cell volume
specialized cells for supporting, binding, and protecting organs
most prevalent tissue in the body
Functions
binding of organs, support, physical protection, immune protection, movement, storage, heat production, and transport
Fibrous
Fibers
Collagen - tough and flexible (white fibers of tendons/ligaments)
Reticular - thin collagen fibers (framework of spleen, lymph nodes)
Elastic - stretch and recoil; made of protein elastin (abundant in lungs)
Cells Types
fibroblasts/fibrocytes: produce fibers and ground substance
leukocytes - neutrophils, lymphocytes, macrophages,
adipocytes
Types
Loose Connective Tissue
areolar - abundant; binds epithelia to deeper tissue; a classification of “fascia”; abundant ground substance; network of collagen and elastic tissue in ground substance
Reticular connective tissue - (loose) network of reticular fibers and cells
Dense Regular Connective Tissue
highly organized, mostly made up of collagen fibers
many fibroblasts
slow to recover
is considered other classification of '“fascia”
Dense Irregular Connective Tissue
random arrangement of collagen fibers
resists stress (due to randomized structure)
Most of the dermis in skin
Protective “capsules”
Adipose Tissue
stores energy and provides protection
white - more abundant in adults
brown - more abundant in infants, for thermoregulation
Cartilage
Cells/Structures of Cartilage
chondroblasts/chondrocytes
produce and maintain ECM
Lacuna
house mature chondrocytes
Fibroblasts
ECM
Types of Cartilage
Hyaline Cartilage
dispersed collagen fibers, not usually visible
small clusters of 3-4 cells (cell nests) eclosed in lacunae
usually covered by perichondrium
Elastic Cartilage
elastic fibers form weblike mesh amid lucunae
always covered by perichondrium
external ear, epiglottis
Fibrocartilage
no perichondrium
parallel collagen fibers
rows of chondrocytes in lacunae between collagen fibers
menisci, intervertebral discs, pubic symphysis
resists compression and absorbs stress
Bone
Types
Spongy (trabecular)
Compact (cortical)
arranged in osteons with a central canal
lamellae
lacunae with osteocytes,
canaliculi - little channels
Blood
made of plasma and formed elements
plasma - water, salts, proteins
formed elements - erythrocytes (RBC), leukocytes (WBC), platelets
Nervous Tissue
specialized for rapid communication with other cells
the longest cells in body
Nervous cell types
Neuroglia (glial) cells
Neurons
transmit information
parts of the neuron
neurosoma (cell body)
dendrites - receive information
axon - transmits signal
Muscular Tissue
composed of elongated, excitable cells
Types of muscular tissue
Skeletal muscle
cells: muscle fibers
voluntary
striated *
cardiac muscle
cells: cardiomyocytes
striated *
intercalated discs
involuntary
Smooth muscle
cells: fusiform myocytes - tapered at ends
non-striated *
involuntary
Skeletal Muscle
attached to bones
arranged in long muscle fibers parallel to each other
each cell (fiber) is multi-nucleated - nuculei play critical role in protein development
Cardiac Muscle
cardiomyocytes form most of the heart wall
arranged in long muscle fibers that are branched
striated
intercalated discs with gap junctions
involuntary
Smooth muscle
fusiform (spindle-shaped) myocytes found in walls of hollow organs
non-striated
involuntary
Tissue Growth and Development
Growth
* Hyperplasia - cell multiplication
growth
repair
* Hypertrophy - enlargement of cell
Neoplasia - tumor development
Changes
differentiation - specialization of form or function
e.g., stem cells
metaplasia - changes from one tissue to another
e.g., ossification of cartilage
Repair
regeneration - replacement of dead cells
fibrosis - scar tissue development
occurs in circumstances of extensive damage
Shrinkage and Death
atrophy - reduction in size/number
“use it or lose it”
shrinkage
necrosis - pathological death of tissue
infarction - blood supply cut-off
gangrene - inadequate blood supply (necrosis)
more often a chronic condition
apoptosis - programmed cell death, normal function