Robbins: Chapter 3 Inflammation and Repair
- %%What is Inflammation?%%
* inflammation is a protective response to damage or infection of vascularized tissue
* it triggers immune cells from the circulatory system to eliminate offending agents
* phagocytic leukocytes, antibodies, complement proteins - %%What are the four cardinal signs of inflammation?%%
* redness
* swelling
* heat
* pain
* function ( later added) - %%What are some causes for inflammation?%%
* infections
* tissue necrosis
* foreign bodies
* immune reaction (hypersensitivity) - %%Steps in inflammation?%%
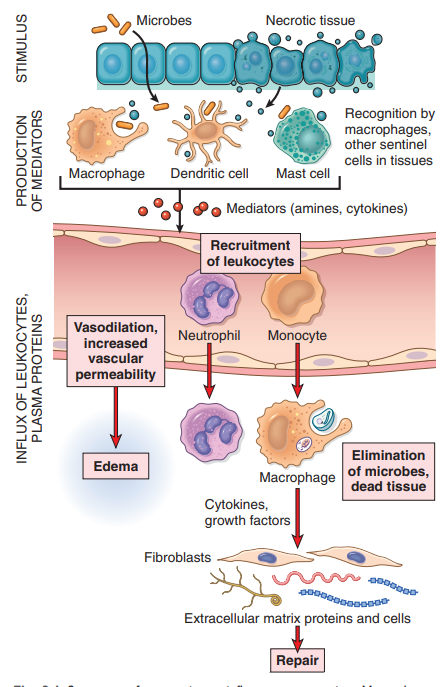
* microbe enters body/ trauma
* Recognition the skin barrier is broken and macrophage, dendritic cells, and Mast cells
* cellular receptors for microbes → PAMPs(pathogen-associated molecular patterns)
* senores of cell damage → DAMPs( damage-associated molecular patterns)
* They recognize the microbe and trigger mediates amiens and cytokines) to recruit leukocytes
* cytokines → what to do!
* chemokines → where to go!
* Removal of stimulus Monocytes → macrophages and Granulocytes eliminate microbes.
* Repair of possible damaged tissue
\
- %%3 major components of acute inflammation?%%
* dilation of small vessels leading to an increase in blood flow
* increased permeability of the microvasculature, enabling plasma proteins and leukocytes from the circulation
* emigration of leukocytes from the microcirculation, their accumulation in the focus of injury, and their activation to eliminate the offending agent - %%Difference between acute and chronic inflammation?%%
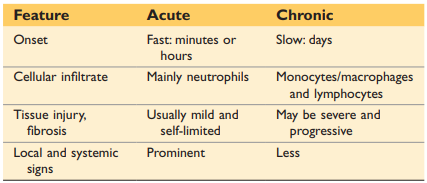
* acute inflammation: is the initial rapid response (within minutes or hours) to eliminate offenders
* characteristic:
* vasodilation
* edema (increased vascular permeability)
* emigration of leucocytes( predominantly neutrophils)
* Chronic inflammation: is triggered when the initial response fails to clear the stimulus
* characteristics:
* longer duration
* more tissue destruction
* dominated by lymphocytes and macrophages
* more proliferation of blood vessels and fibrosis
- What is exudate and transudate? how is it related to acute inflammation?
* %%exudate%%: extravascular fluid that has high protein concentration and contains cellular debris → implies existence of inflammatory process
* in big amounts it is called pus
* %%transudate%%: fluid with low protein content with little to no cellular material → produced due to hydrostatic imbalance but not due to inflammation
* in big amounts called edema - %%what are changes in vascular flow in response to inflammation?%%
* increased blood flow → vasodilation → cause of heat and redness
* increased permeability: exudate of fluid into extravascular tissue
* loss of fluid → slower blood flow(stasis) + increased viscosity
* as stasis develops neutrophils accumulate along the vascular endothelium( more this in a later question) - %%What is the multistep journey of leukocytes?%%
* (1) rolling → from center to endothelium walls with the help of selectins, which are the ligands found on leucocyte
* (2) integrin activation by chemokines
* (3) stable adhesion → integrins are the ligands found on leukocyte membrane that attach to the receptors on endothelial cells
* (4) migration through endothelium (diaphyses/transmigration) - %%What are chemoattractants? And give some examples.%%
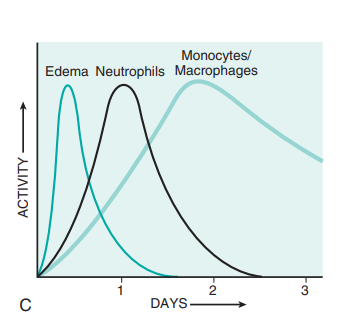
* Chemoatractes are produced by microbes and by host cells in response to n infections r tissue damage. They signal neutrophils and leukocytes towards which direction the inflammatory site is. First, neutrophils arrive to the site, but due to their short half-life, they are then replaced by Monocytes/Macrophages.
* examples:
* LTB4
* C5a
* IL-8
- %%What is key when terminating the inflammation and what are the associated steps?%%
* Phagocytosis and clearance of the offending agent
* (1) recognitions and attachment of the particle to be ingested by the leukocyte
* (2) engulfment, with subsequent formation of a phagocytic vacuole
* (3) killing or degradation of the ingested material with lysomome - %%What is the function compliant system?%%
* it only destroys bacteria by drilling holes into the cell walls of the bacteria
* if this happens in normal healthy cell this causes major tissue damage - %%What are the possible outcomes of acute inflammation ?%%
* complete resolution
* restoration of the site to normal tissue
* removal of cellular debris
* no edema
* healing by connective tissue replacement
* scarring or fibrosis
* Progression of the response to chronic inflammation - How can you recognize inflamed tissue under a microscope?
* fluid-filled space → edema
* fibrinous exudate
* accumulation of granulocytes
* purulent inflammation → pus( dead granulocytes)
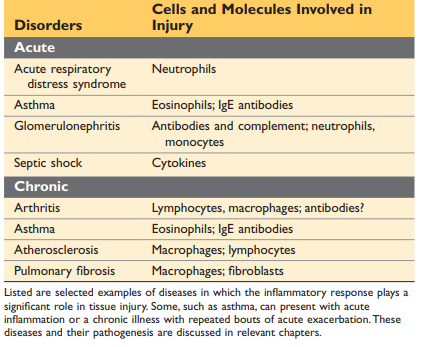
* ulcer → local tissue destruction - Name different acute and chronic inflammatory diseases:
*
- What causes chronic inflammation?
* Immune-mediated inflammatory( hypersensitivity)
* autoimmune disease
* allergies
* Persistent or prolonged exposure to microbial infections by microorganisms that are difficult to eradicate
* Due to a delayed response immune reaction
* development if granulomatous inflammation
* walling of epithelial cells due to dead granulocytes - What are two types of macrophage activation?
- what are systemic effects of inflation
* production of proteins: acute-pashe protein
* C-reactive protein (CRP) and serum amyloid A protein( SAA)
* Fever - %%when does the repair of damage start?%%
* the work simoultainsly and can´t be seen as separate processes - inflammatory vs anti
* autoimmune lymphocytes that recognize cells falsely
* autoinflammatory aggressive cells that just fire but it is not targeted - each phase of the inflammatory response are associated with disease with the off switch of proteins is faulty
- What happens when microbo flora crosses the one cell layer that protects
* the first line of defense: innate immune → 99% of invasive microbes are depleted
* epithelium
* macrophages
* neutrophils
* adapt system is triggered by an innate system via chemokines( signaling molecules)
* b and t cells - Tuberculosis is a bacterium that causes a chronic inflammatory response
* in crohns the histology looks similar because the body falsely reacts to microbes because the body confuses the two → genetic defects - If you have impairment in innate response than their is a bigger/faster response of the auqired immune system to make up for the work
- lazy leukocyte syndrome
* leuity work slower ad, therefore, cause chronic inflammation because they fulfill they job to slow - post-infectious autoimmune disease!!
* a microbe is recognized by t cell; however, after that the body confuses its own body causing chronic inflammation - granuloma
* to prevent spreading through the body
* chronic granular disease
* Hermans putlock disease - neutrophils love shortly
- regulatory t cell -→ controls immune response (dampens it)
- T-cell diseases → organ specific
* too many t cells or too little regulatory t cells - repair and regeneration
* repair → with scaring
* regeneration → exact copy of what was damaged - cholangiocytes: scar cells
- remodeling: differences in tissue in organs
- why repair and not regeneration
* repair is faster - Kupfer cells are macrophages in liver
- what happens after liver failure?
* edema
* turn yellow
* very sensitive to toxins - steps after cutting skin
* \
1. clotting
* \
2. epithelial cells
* \
3. granulation tissue
\