Biochem - Digestive Tract and Functions
Digestive Tract Functions
Ingestion: Process of taking in food.
Physical Breakdown: Mechanical process where food is physically broken down into smaller pieces.
Digestion (Chemical Breakdown): Enzymatic breakdown of food into simpler compounds.
Absorption: Process of transferring nutrients from the digestive tract into the bloodstream.
Excretion: Elimination of indigestible substances from the body.
Time Constraint: The entire above functions occur within the constraints of the rate of passage through the digestive tract.
The Digestive Tract Anatomy
Major Sections:
Oral Cavity: Where ingestion occurs and initial breakdown by chewing happens.
Pharynx: Junction of mouth and esophagus; serves as a crossroad for air and food passage.
Esophagus: 25 cm long muscular tube that transports food to the stomach; produces mucus; equipped with upper and lower sphincters for regulation.
Stomach: Site of chemical digestion and storage; food is mixed and transformed into semi-liquid chyme upon exiting.
Small Intestine: Divided into three segments; responsible for the majority of nutrient absorption. Includes:
Duodenum: First section, less than 1 ft long.
Jejunum: Middle section, size varies in different species; continuous with ileum.
Ileum: Last section, approximately 9 ft long.
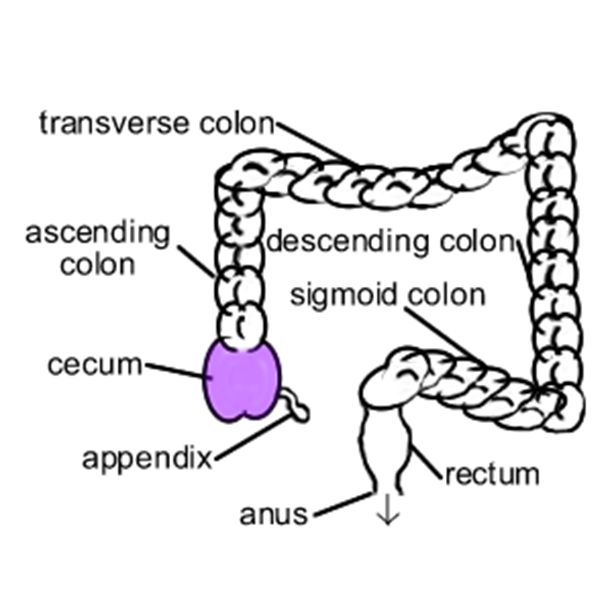
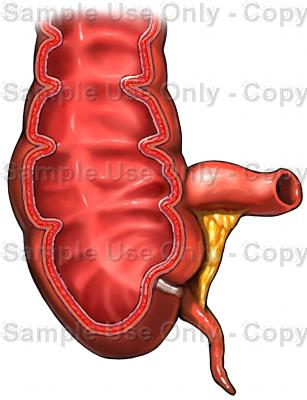
Large Intestine: Last portion of the digestive tract; subdivided into cecum, colon, and rectum.
Rectum: Terminal section of the large intestine, leading to the anus.
Accessory Organs in Digestion
Tongue: Aids in tasting and manipulating food.
Teeth: Crucial for mechanical breakdown via chewing.
Salivary Glands: Produce saliva which contains enzymes and mucus, aiding digestion.
Liver and Gall Bladder: Liver produces bile; gall bladder stores and concentrates bile for emulsification of fats.
Pancreas: Produces digestive enzymes and bicarbonate to neutralize gastric acid.
Physical Breakdown Process
Saliva:
Composition: Two types of secretion - serous (watery) and mucus (thick and slimy), providing lubrication.
Enzymes: Salivary amylase for starch breakdown and lingual lipase for fat digestion.
Buffers: Bicarbonate and phosphate to maintain pH balance.
Nutrient Recycling: Includes non-protein nitrogen and minerals. Daily production:
Humans: 1.2 L/day
Cattle: 150 L/day
Esophagus Function
Functions as a transportation conduit for food to pass from the mouth to stomach, incorporating
Muscular contractions to push food down.
Production of mucus to facilitate movement.
Stomach Functions
Chemical Digestion: Prepares food for small intestine.
Storage: Temporarily holds food before processing.
Mixing Action: Churns food with gastric juices to form chyme which is semi-liquid.
Gastric Glands and Their Functions
Goblet/Mucoid Cells: Secrete mucus for protection and lubrication.
Parietal Cells: Produce hydrochloric acid (HCl) and intrinsic factor, essential for vitamin B12 absorption.
Chief Cells: Secrete pepsinogen (inactive precursor of pepsin) and gastric lipase.
Enteroendocrine Cells (EECs): Secrete gastrin, histamine, somatostatin, ghrelin, serotonin, regulating gastric function.
Function of Hydrochloric Acid (HCl)
Conversion of Pepsinogen to Pepsin: The active form that breaks down proteins.
Denaturation of Proteins: Inactivates protein structures enhancing proteolytic breakdown by pepsin.
Nutrient Release: Facilitates the absorption of nutrients from complex organic materials.
Antimicrobial: Kills ingested bacteria to prevent infection.
Helico-bacter Pylori
Bacterial Nature: Gram-negative bacteria that survive in gastric environments.
Mechanism: Produces urease to neutralize its environment by converting urea to bicarbonate and ammonia. Provides a survival advantage against gastric acids.
Digestive Changes in Neonates
Production of Prorennin: Newborns initially produce prorennin instead of pepsinogen.
Function: Converts milk casein into curds for slower digestion.
Immune Transfer: Allows for absorption of maternal antibodies in colostrum.
Importance: Colostrum contains key growth factors and compounds critical for immune function.
Regulation of Gastric Secretions
Cephalic Phase:
Triggered by sight/smell of food; neural response via vagal nerve causes release of acetyl-choline.
Influences chief and parietal cell activity.
Gastric Acid Release: Varies based on stimuli:
Basal acid output: 4 mmol/hr
Talking about food increases release up to 15 mmol/hr.
Gastrin injection increases it up to 38 mmol/hr.
Gastric Phase:
Predominant phase; presence of food in stomach and wall stretching activates G-cells to release gastrin.
Stimulates further activation of chief and parietal cells.
Secretogogues such as alcohol and caffeine increase gastrin release.
Intestinal Phase:
Food in small intestine may also trigger continued gastric secretions.
Brief Overview of Gastric Hormones and Medications
Hormones:
Gastrin: Stimulates acid production.
Histamine: Released by ECL cells, enhances acid production.
Medications:
Prilosec, Zantac, Pepcid, etc., are used to manage gastric acid production and reduce heartburn.
Small Intestine Anatomy
Divisions:
Duodenum: Less than 1 ft long, receives secretions from pancreas and bile.
Jejunum: Major site of absorption.
Ileum: Completes absorption of nutrients; connects to the large intestine.
Approximate Lengths by Species:
Chickens: 5 ft
Pigs: 50 ft
Cattle: 120 ft
Humans: 10 ft (approximately).
Histological Structure of the Small Intestine
Villi: Finger-like projections containing blood vessels.
Microvilli: Form a brush border on enterocytes, increasing absorptive surface area to approximately 200 m² per cell.
Cells:
Enterocytes: Absorptive cells with specialized membranes.
Goblet Cells: Secrete mucus for lubrication.
Crypts of Lieberkuhn: Contain stem cells for continuous regeneration of epithelial cells, with turnover every 3 to 5 days in humans.
Important GI Hormones from Enterocytes
CCK (Cholecystokinin):
Stimulates gallbladder contraction; slows gastric emptying; controls satiety.
Secretin:
Slows gastric emptying; inhibits acid secretion; stimulates bicarbonate and enzyme secretion from pancreas.
GIP (Gastric Inhibitory Polypeptide):
Stimulates insulin release; inhibits gastric secretion and motility.
Pancreas Functions
Produces digestive enzymes that help in the breakdown of carbohydrates, proteins, and fats.
Secretes hormones such as insulin and glucagon to regulate blood sugar levels.
Exocrine Role: 98% of pancreas; produces digestive enzymes and buffers.
Endocrine Role: 2% of pancreas; regulates glucose metabolism through insulin and glucagon.
Digestive Enzymes and Their Specificities:
Enzyme | Substrate | Products |
|---|---|---|
Amylase | Starch | Limit dextrins, maltose |
Trypsinogen
| Proteins | Peptides |
Chymotrypsinogen
| Proteins | Peptides |
Proeleastase
| Proteins | Peptides |
Carboxypeptidase A | Proteins | Peptides, amino acids |
Lipase | TAGs | MAGs, Fatty Acids |
Ribonuclease | RNA | Ribonucleotides |
Deoxyribonuclease | DNA | Deoxyribonucleotides |
Liver and Gall Bladder Functions
Bile Production:
Bile Acids: Derived from cholesterol; aids in fat emulsification.
Chenodeoxycholic acid: A primary bile acid that plays a critical role in the digestion and absorption of dietary fats.
Cholic Acid: Another primary bile acid that enhances fat digestion and absorption, as well as promoting the solubilization of cholesterol.
Typically conjugated with glycine or taurine
Bile Pigments: Include bilirubin and biliverdin; waste products from hemoglobin degradation.
Enterohepatic Circulation: The recycling of bile from intestine back to liver.
Jaundice Explained
Definition: Hyperbilirubinemia; accumulation of bilirubin in blood leading to yellowing of skin/eyes.
Causes: Increased bilirubin production, impairment of liver metabolism, or excretion.
Normal Plasma Concentrations:
Dogs: 0.4-0.6 mg/dL
Cats: 0.2 mg/dL
Humans: ~0.3 mg/dL
Role of Enterocytes in Digestion
Ectoenzymes: Located on the apical membrane for nutrient digestion.
Complete digestion of oligosaccharides and peptides.
Cytosolic Peptidases: Hydrolyze di- and tri-peptides from gut lumen.
Nutrient Absorption Processes
Unmediated Passive Diffusion:
Transcellular diffusion through lipid membranes or aqueous pores.
Paracellular diffusion through tight junctions between cells.
No ATP needed for this type of transport, as substances move along their concentration gradient without energy expenditure.
Carrier/Receptor-Mediated Movement:
Facilitated Diffusion: Passive carrier-mediated transport.
Active Transport: Requires ATP; can be primary or secondary. Glucose is absorbed through active transport.
Primary active transport involves the direct use of ATP to transport molecules against their concentration gradient, utilizing transport proteins such as pumps to move ions across the cell membrane.
Secondary active transport relies on the gradient created by primary active transport to move substances across the membrane, often coupled with the movement of ions into the cell.
Vesicular Transport: Includes endocytosis for larger molecules.
Endo- means "inside," -cyt - means "cell," -osis means "a process or condition;" therefore, endocytosis refers to the process by which cells engulf substances to bring them internally, facilitating nutrient uptake and cellular signaling.
Large Intestine Overview
Structure: Begins at cecum (blind pouch), about 5 ft long in humans.
Function: Major site for water and electrolyte absorption; acts as a reservoir for microbiota.
Fermentation: Occurs in the colon, providing certain vitamins (thiamin, K, riboflavin).
No digestive enzymes secreted
Endogenous proteins: play a role in maintaining gut health by supporting the integrity of the mucosal barrier and influencing the overall function of the immune system.
Microbes produce:
gas (H2, CH4)
volatile or short-chain fatty acids (VFA or SCFA)
acetate - 2 carbon
propionate - 3 carbon
butyrate - 4 carbon
Feces is mostly made of microbial matter, then non-fermented fiber, epithelial cells, and mucus
Additional Digestive Systems
Ruminants: Digest food in two stages, first by eating and then by rumination (cud chewing).
Pre-gastric fermenters :These organisms specialize in digesting their food prior to entering the stomach, primarily through microbial fermentation in the foregut, allowing for more efficient nutrient absorption.
Post-gastric fermenters: These animals ferment their food in the hindgut, which enables them to extract nutrients after the stomach digestion, often resulting in less efficient absorption compared to pre-gastric fermenters.
Four Chambered Stomach:
Rumen: Fermentation chamber.
Reticulum: Honeycomb structure that collects smaller particles.
Omasum: Absorption of water and nutrients.
Abomasum: True stomach, similar to human stomach.
Omnivores: Organisms that consume both plant and animal materials, utilizing a more diverse range of digestive enzymes to break down various food types.
Carnivores: Organisms that eat meat , primarily relying on protein-digesting enzymes and a simpler digestive process to efficiently convert their food into energy.
Herbivores: Organisms that eat plants and have specialized stomachs to help break down tough plant fibers, often relying on symbiotic bacteria for fermentation.
Comparative Digestive Anatomy of Mammals
Gastrointestinal Volume by Animal Species:
Species | Total Contents | % Reticulurumen | % Omasum | % Abomasum | % S.I. | % Cecum | % Colon & Rectum |
|---|---|---|---|---|---|---|---|
Ruminants | |||||||
Cattle | 13-18 | 9-13 | 1.1-2.8 | 0.5 | 0.9-2.3 | 0.8 | 0.8-1.5 |
Sheep | 12-19 | 9-13 | 0.1-0.3 | 0.7-1.6 | 1.0-1.6 | 0.9 | 0.5-0.7 |
Camel | ? | 10-17 | - | - | ? | 0.1-0.3 | 1.0-2.2 |
Non-Ruminants | |||||||
Elephant | ? | - | - | ? | ? | 3.2 | 8.8 |
Horse | 16.4 | - | - | 2.6 | 2.6 | 2.4 | 8.8 |
Pig | 10.4 | - | - | 1.9 | 1.9 | 1.6 | 3.4 |
Rabbit | 7-18 | - | - | 0.6-1.8 | 0.6-1.8 | 2.5-7.8 | 0.7-1.3 |
Rodent | |||||||
Capybara | 16.5 | - | - | 1.0 | 1.0 | 11.7 | 1.3 |
Guinea Pig | 8.0 | - | - | 1.9 | 0.9 | 3.7 | 1.6 |
Rat | 3.1 | - | - | 0.4 | 0.9 | 1.0 | 0.9 |