7.2 - the nephron
FILTRATION
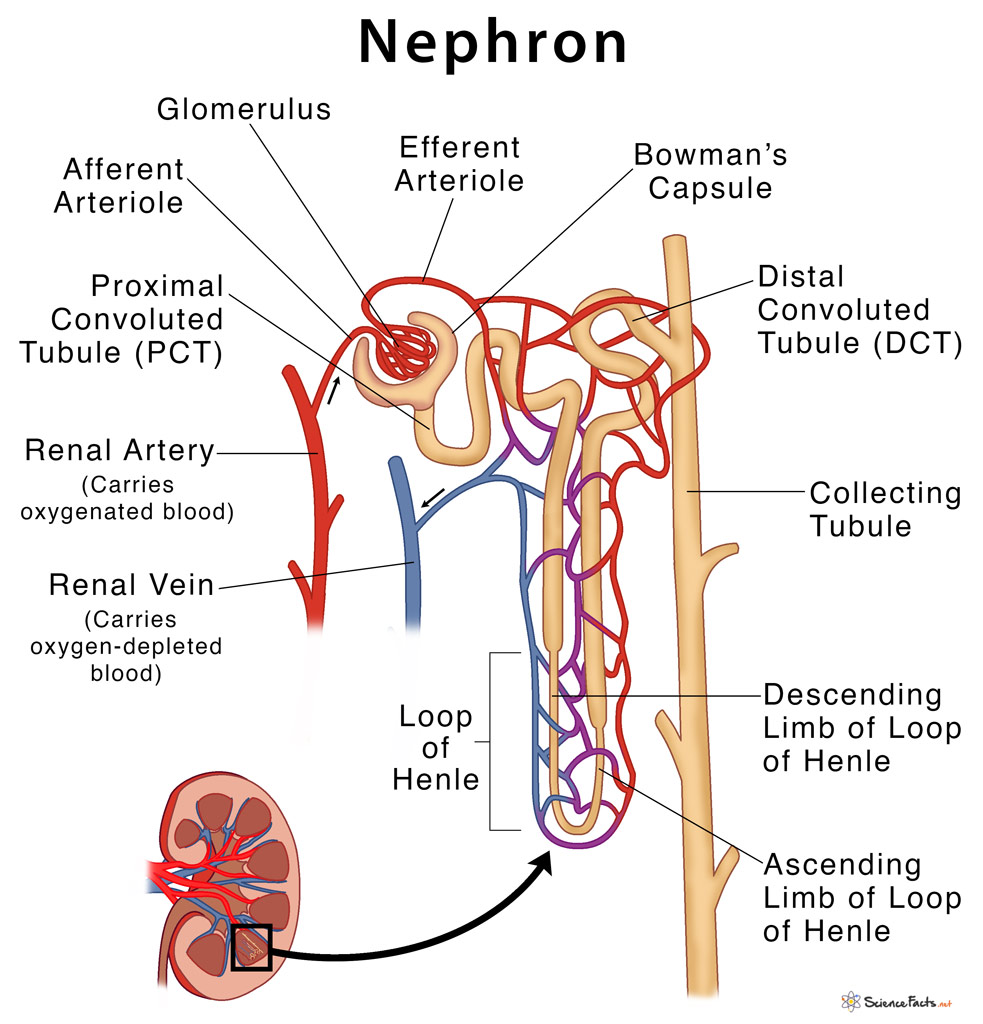
afferent (incoming) arteriole goes into the bowman’s capsule and branches into the glomerulus
blood is filtered between the glomerulus and bowman’s capsule
filtration occurs at 4x the pressure (pressure is higher so solutes/wastes can be pushed out) than in a normal capillary
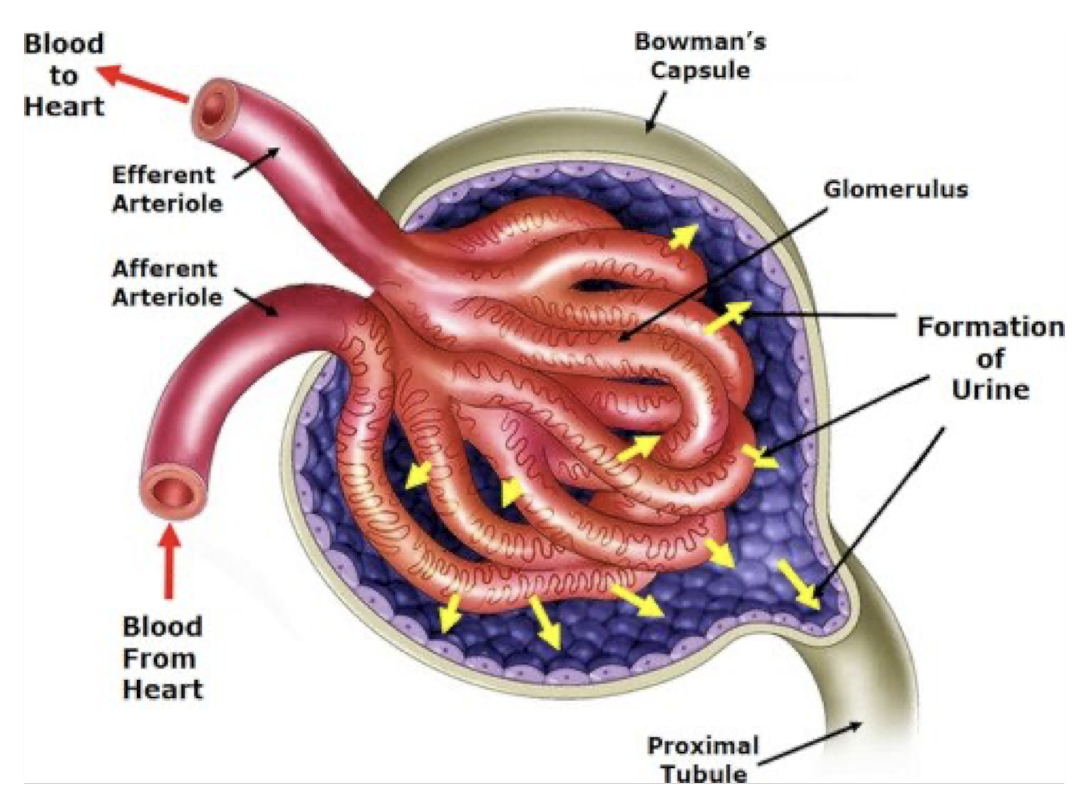
A.) FILTERABLE BLOOD COMPONENTS
dissolved substances (water, nitrogenous wastes, nutrients, ions) move from areas of high pressure to low
fluid in the bowman’s capsule is called the glomerular filtrate
(glomerular filtrate forms when high pressure in the glomerulus pushes dissolved substances into the bowman’s capsule forming fluid with the substances / glomerular filtrate)
B.) NON-FILTERABLE BLOOD COMPONENTS
the components (blood cells, proteins) of the blood that do not leave the capillaries, carry on away from the glomerulus through the efferent arteriole
BLOOD SUPPLY
the efferent arteriole forms a capillary network around the nephron called the peritubular capillary network
as filtrate flows through the nephron, many substances are reabsorbed actively (with energy - against the concentration gradient - low → high) or passively (without energy - along the concentration gradient - high → low) into the peritubular capillary network
REABSORPTION
the movement of ‘good’ substances (from filtrate) from the nephron back into the blood stream
primarily occurs in the proximal convoluted tubule and loop of henle
PROXIMAL CONVOLUTED TUBULE
is where active transport of nutrients from the glomerulus filtrate moves back into the blood stream
by the time the glomerulus filtrate reaches the loop of henle there should be no nutrients in it should be reabsorbed
glucose, amino acids, and na are all actively reabsorbed at the PCT and moved back into the blood stream in the tissue of the cortex
Cl is passively reabsorbed by following Na back into the blood through Cl channels
as solute concentration increases in the blood, water follows the concentration gradient and moves out of the filtrate
85% of water is passively reabsorbed as it moves from high water concentration to low water concentration
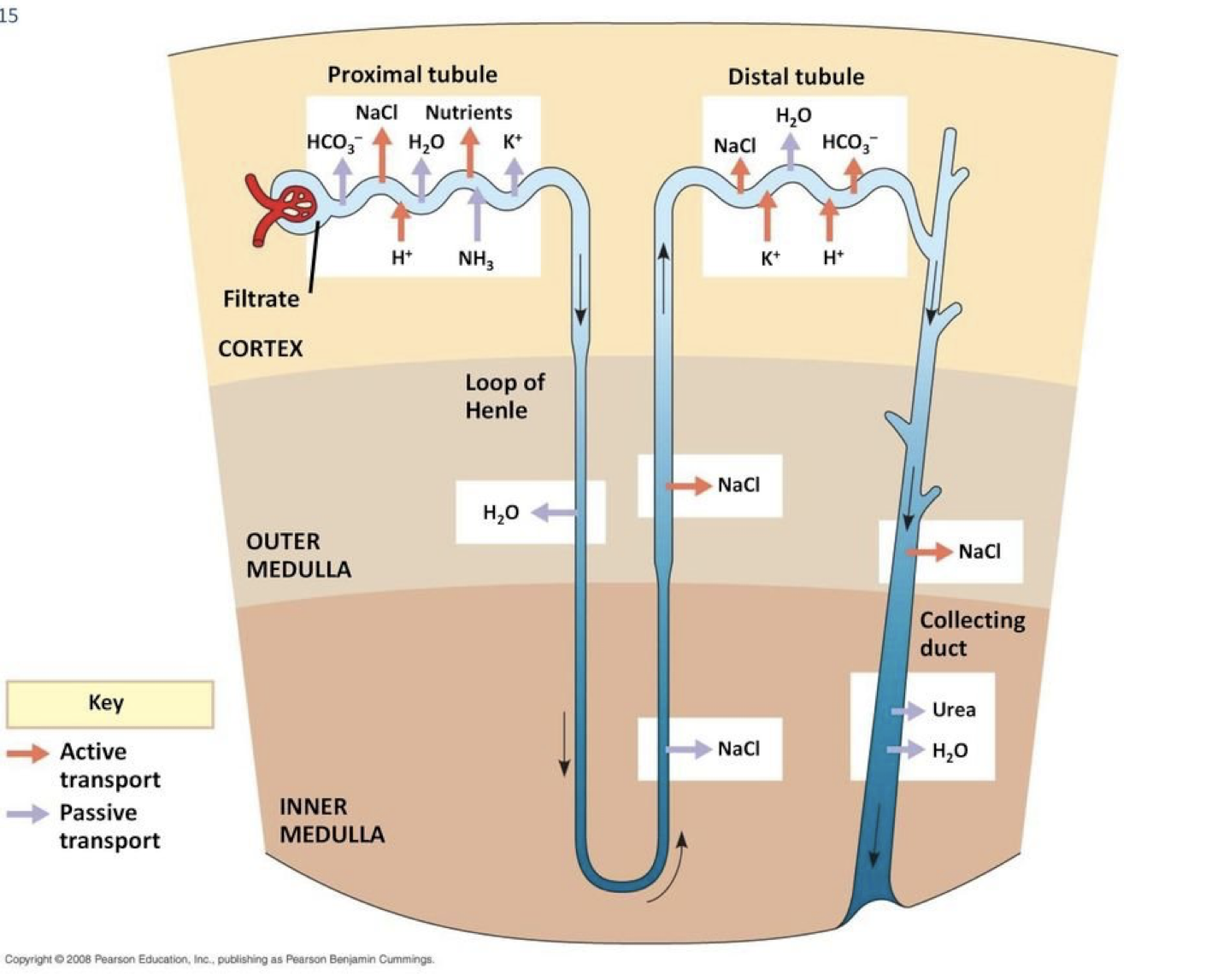
LOOP OF HENLE
the descending loop of henle is impermeable to everything except water
the ascending loop of henle is impermeable to everything except Na and Cl
(additional water / na and cl are reabsorbed here in the loop of henle back into the blood)
WATER REABSORPTION
water is also reabsorbed in the distal convoluted tubule and the collecting duct
essentially, water can be reabsorbed anywhere in the nephron except the ascending loop of henle
KIDNEY REGIONAL ENVIRONMENT
all nephrons are layered on top of each other as well as besides each other
this means that if there is a change in environment in one PCT (like altered blood), there is a change in the environment around all PCT’s
this leads to a change in environment throughout the cortex of the kidney
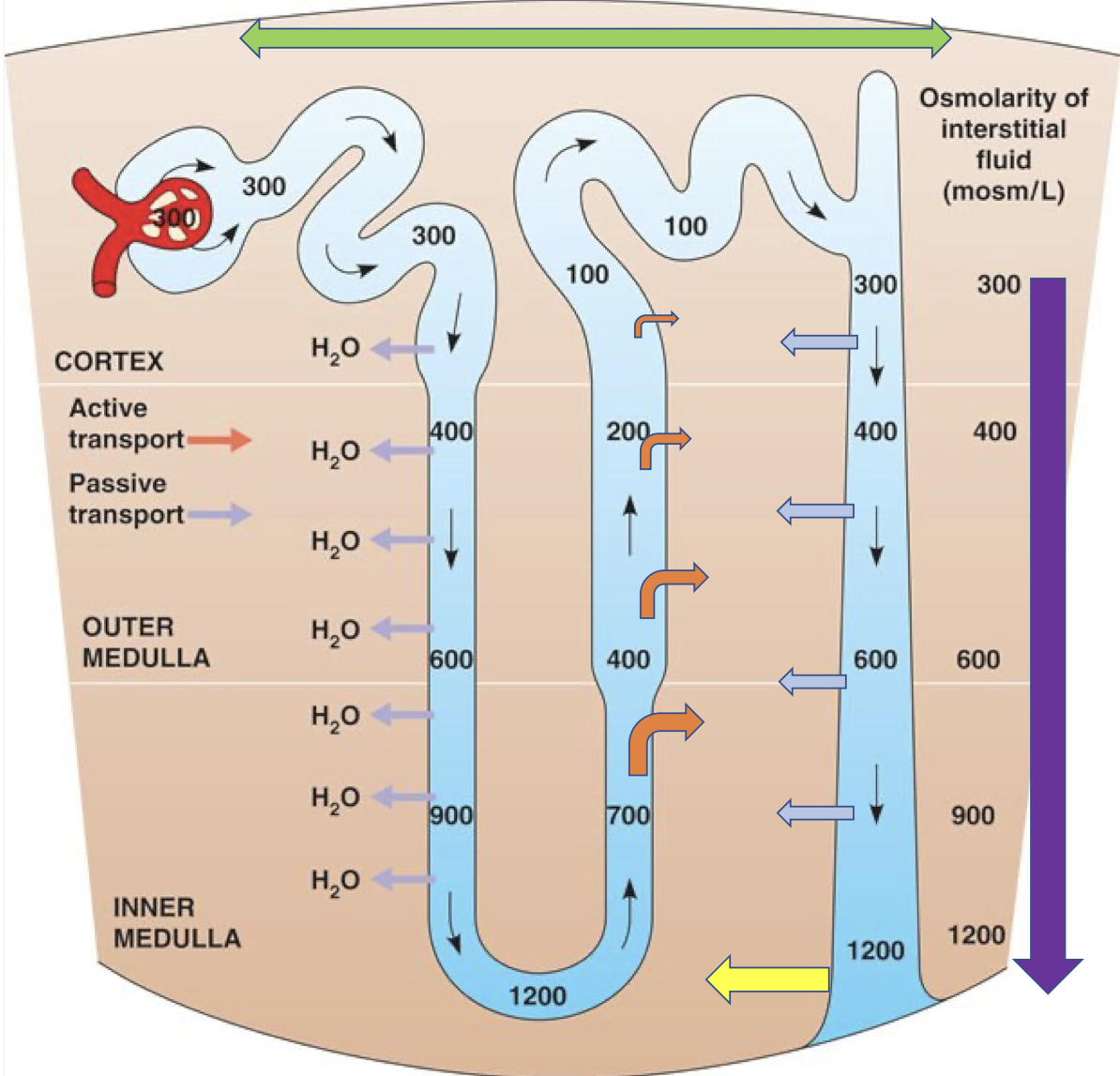
COUNTER CURRENT EXCHANGE
NaCl moves out of the thick part of the ascending loop of henle
as the fluid moves up, less NaCl becomes available to move out, therefore the outer medulla has less osmotic pressure (less solutes) than the inner medulla (higher solutes)
urea which leaks from the lower part of the collecting duct also increases the osmotic pressure in the inner medulla
the establishment of this osmotic gradient ensures that water continues to move out of the entire length of both the descending loop of henle and the collecting duct
(ascending loop - impermeable to water so it releases NaCl to ensure that the surroundings are high in solute so that water can be released later on. permeability of the loop of henle regulates the concentrations of water/osmotic gradient as the ascending loop increases the gradient)
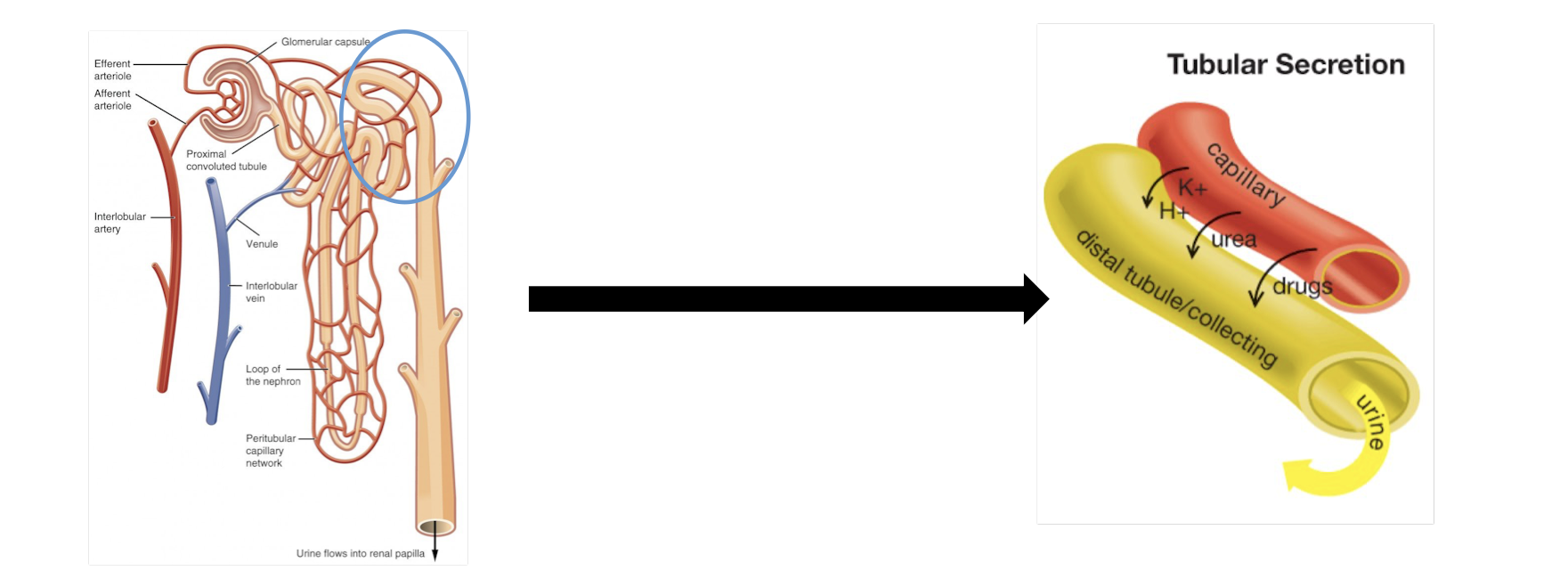
TUBULAR SECRETION
active transport of molecules (substances the body wants to remove or regulate) from the blood to the nephron
occurs in the distal convoluted tubule
uric acid, urea, K+ and H+ are secreted
penicillin and histamine are also secreted
URINE
urine is made up of the substances that have been filtered, secreted, and not absorbed
these include:
small amounts of water
nitrogenous wastes
bicarbonate, sulphates, and phosphates
excess ions
URINATION
from the renal pelvis urine goes down the ureters and into the bladder
as the bladder fills, stretch receptors send impulses to the spinal cord
impulses from the spinal cord then cause the bladder to contract and urine is released
usually, this reflex is controlled by the brain