Pharmacology
[[Pharmacology[[
- the study or science of drugs and their actions on living organisms
- derived from the word which means drug or medicine and also from the word logos which means science
[[Drug[[
- any chemical that affects the physiologic processes of a living organism
- includes medications such as therapeutic drugs
<<Drug Names<<
[[Chemical Name[[
- a chemical constitution and molecular structure
- ex: N-(4-hydroxyphenyl)
[[Generic Name[[
- a common name
- it is universally accepted
- ex: acetamide, acetaminophen
[[Brand Name/Trade Name[[
- propriety name
- trademark
- ex: Tylenol
<<Classifications<<
- Body system that is affected
- ex: respi, CV
- Therapeutic use or clinical indications
- ex. anti HPN, OHA
- Physiologic or Chemical action
- ex. anticholinergic
- Prescription/non-prescription drugs
- Illegal drugs
- ex. recreational drugs
<<Classification based on Chemical Nature<<
[[Inorganic Drugs Metals and their salts:[[
- Ferrous Sulphate
- ZInce Sulphate
- Magnesium Sulfate
- Non-metals: Sulphur
[[Organic Drugs[[
- Alkaloids: Atropine, Morphine
- Glycosides: Digitoxin, Digoxin
- Protein: Insulin, Oxytocin
- Esters: Amide, Alcohol, Glycerides
<<Classification based on Source<<
[[Natural Source[[
- Plants: Morphine, Atropine, DIgitoxin
- Animals: Insulin
- Microorganism: Penicillin
- Mineral: Sodium Chloride
[[Synthetic Source[[
- Suphonamides
<<Classification based on Target Organ<<
[[Drug acting on CNS[[
- Barbiturates
- Phenobarbitone
[[Drugs acting on Respiratory System[[
- Mucolytics
- to cut the production of mucus
- Bromhexine
- to cut the production of mucus
[[Drugs acting on Cardiovascular System[[
- Glycosides
- alleviate the symptoms of myocardial infarction or heart attack
- Digitoxin, Digoxin
- alleviate the symptoms of myocardial infarction or heart attack
[[Drugs acting on Gastrointestinal Tract[[
- Antibacterial
- destroys bacteria or suppresses their growth or their ability to reproduce
- Sulphadimidine
- destroys bacteria or suppresses their growth or their ability to reproduce
[[Drugs acting on Urinary System[[
- Tocolytic
- prevent the contraction of the uterus in the pre-mature labor patients
- Magnesium Sulphate - lesson the seizure of pregnant woman
- prevent the contraction of the uterus in the pre-mature labor patients
[[Drugs acting on Reproductive System[[
- Oxytocic Hormones
- induce labor or strengthen uterine contractions, or to control bleeding after childbirth
- Oxytocin
- Estrogen
- induce labor or strengthen uterine contractions, or to control bleeding after childbirth
<<Classification based on Mode of Action<<
[[Inhibitor of Bacterial Cell Wall Synthesis[[
- Treats infections caused by bacteria on the cell wall and destroys the wall
- Penicillin
[[Inhibitor of Bacterial Synthesis[[
- Tetracycline
[[Calcium Channel Blocker[[
- If calcium is produced too much, it excites the heart too much which results in dysrhythmic and then dysrhythmia
- Verapamil
- Nifedipine
<<Classification based on Physical Effects<<
[[Emollients[[
- Substances that soften and moisturize the skin and decrease itching and flaking
- Lanolin, Vaseline
[[Caustics[[
- Substances that burn or destroy organic tissue by chemical action, generally a strong corrosive alkali
- Silver Nitrates
[[Demulcents[[
- Substances that relieve irritation of the mucous membranes by forming a protective film
- For diaper rash
- Zinc oxide, Tannic acid
<<Classification of Information Sources<<
[[Primary Sources[[
- Clinical research studies both published and unpublished
- 40 population
[[Secondary Sources[[
- References that are either index or abstract are the primary literature, with the goal of directing the user to relevant primary literature
[[Tertiary Sources[[
- information that has been summarized or filtered by the author or editor to provide a quick and easy summary of a topic
- ex. textbooks, compendia, review articles in journals
[[Black Box Warnings[[
- Notifications within a prescription drug’s package inserts provided by the FDA to call attention to an extremely adverse drug effect
- Primary alerts for identifying extreme adverse drug reactions
Drug Action: Pharmacokinetics and Pharmacodynamic Process (2 Phases of Medicine)
<<Pharmacokinetic Phase<<
[[Liberation[[
- The first phase of drug action is the release of the drug from its dosage form
- Disintegration - breakdown of a tablet into smaller particles
- Dissolution - dissolving of the smaller particles in the GI fluid before absorption
%%Excipients%% - fillers and inert substances that allow the drug to take on a particular size and shape to enhance drug dissolution
Drugs are disintegrated and absorbed in faster acidic fluids (pH of 1 or 2)
<<Pharmacokinetic Phase (ADME)<<
[[Absorption[[
- movement of drug particles from the GI tract to body fluids by passive absorption, active absorption, pinocytosis
- passive absorption – occurs by diffusion (higher to
lower); no energy needed
- active absorption - requires a carrier (enzyme or
protein); needs energy
- pinocytosis – engulfing the drug particles
Nsg Mngt:
• Administer with adequate amount of fluid • Give parenteral drugs properly • Reconstitute and dilute with recommended diluent
- Drugs that are lipid soluble and nonionized are absorbed faster than water-soluble and ionized drugs
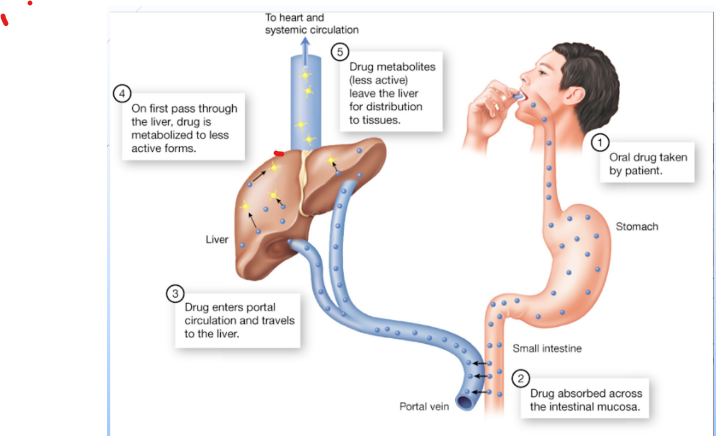
- First-pass effect (hepatic first pass) – a process in which the drug passes to the liver first
- Bioavailability – the percentage of the administered drug dose that reaches the systemic circulation 100% for IV
[[Factors that affect bioavailability:[[
a. drug form b. route of administration c. GI mucosa and motility d. food and other drugs e. changes in liver metabolism
[[Distribution[[
- transportation of drugs throughout the body by body fluids to the sites of action or to the receptors
Factors:
a. rate of blood flow b. drug’s affinity to the tissue c. protein-binding effect
%%Protein-binding effect%% - inactive drugs are bound to varying degrees
with protein (albumin)
%%Free drugs%% – active that can cause pharmacologic response
@@Nsg Resp:@@ To avoid possible drug toxicity, check the protein-binding percentage of drugs administered. Check also plasma protein and albumin levels.
General or selective
- Blood-brain barrier - only few drugs can bind
- Placental barrier - selective
[[Metabolism or Biotransformation[[
- process by which the body chemically changes drugs into a form that can be
- liver and liver enzymes (cytochrome P450 system)
%%Half-life – t1/2%%
time it takes for one-half of the drug concentration to be eliminated
affected by metabolism and excretion
short half-life (4 to 8 hours); long half-life (24 hours or longer)
%%Steady state%%
the amount of drug administered is the same as the amount of drug being eliminated
after four to five half-lives
%%Loading Dose%%
- large initial dose given to achieve a rapid minimum effective concentration in the plasma
- ex. Digoxin (Digitek, Lanoxin)
Phenytoin
[[Excretion[[
- elimination of drugs from the body
- lungs eliminate volatile drug substances and products metabolized to CO2 and H2O
- kidney filter-free unbound drugs, water-soluble drugs, unchanged drugs
- intestines (biliary excretion); taken by the liver, released into the bile, eliminated in the feces
NOTES:
- The more acidic the stomach the faster the absorption of drugs
- Lipid soluble is faster because of the fats lining inside the stomach
- Cancer affects the metabolism in the stomach
- If the liver is not functioning well, the drug that is supposed to be metabolized will not be metabolized causing toxicity
<<Pharmacodynamics<<
- study of the way drugs affect the body
- Primary effect - desirable
- Secondary effect - undesirable
ex. Benadryl
Dose Response Relationship
- Magnitude of the drug effect depending on the drug concentration at the receptor site
Graded-Dose Response Relationship
- As the concentration of a drug increases, its pharmacologic effect also gradually increases until all the receptors are occupied
- Graded effect (response is continuous and gradual)
- Potency – amount of drug necessary to produce an effect of a given magnitude
- Efficacy - magnitude of response a drug causes when it interacts with a receptor
- Maximal efficacy – point at which increasing a drug’s dosage no longer increases the desired therapeutic response
Therapeutic Index and Therapeutic Range (Therapeutic Window) Therapeutic index (TI)
- estimates the margin of safety of a drug
- relationship between a drug’s desired therapeutic effects (ED50) and its toxic dose (TD50)
PHARMACODYNAMIC PHASE