Blood Supply to the Head and Neck
Overview of Blood Supply to the Head and Neck
Introduction
Good morning, everyone! This module focuses on the extensive blood supply to and from the head and neck region, emphasizing both the arterial and venous systems. The session will provide a comprehensive overview of the critical vascular anatomy necessary for clinical practice.
Importance of Blood Supply
The brain requires adequate blood flow for optimal functioning. When blood supply is compromised, it can have severe consequences such as loss of consciousness or stroke, as exemplified by various clinical scenarios. By understanding the vascular system's anatomy, especially the role of collateral circulation, we can appreciate how different structures can adapt when primary pathways are damaged or removed.
Overview of Arterial Supply
Main Arteries Supplying the Brain
Vertebral Artery:
Source: It is the first branch of the subclavian artery and has two sections:
First Segment: Ascends without entering the transverse foramina.
Second Segment: Runs through the transverse foramina of cervical vertebrae C6 to C1.
Third Segment: Exits at C1, before entering the skull through the foramen magnum, at significant risk of kinking or compression, especially during neck extension.
Function: Supplies the brainstem and is vital for consciousness, breathing, and heart rate.
Clinical examples: Passing out while looking upward (e.g., in mechanics or salons) can occur if blood flow is restricted due to neck extension or existing vascular disease.
Bowhunter Stroke: Occurs when the neck is turned ipsilaterally, kinking the vertebral artery and potentially leading to decreased blood flow and stroke.
Basilar Artery:
Formation: Formed within the skull by the fusion of left and right vertebral arteries.
Importance: Supplies a significant portion of the blood flow to the brain (approximately one-third).
Location: Sits at the base of the skull, referred to as the basilar artery due to its position.
Common Carotid Artery

Common Carotid Artery:
Bifurcation: Splits into internal and external carotid arteries at approximately the upper level of the thyroid cartilage (around C4).
Internal Carotid Artery:
Enters the cranium via the carotid canal.
Supplies the majority of the blood flow (approximately two-thirds) to the brain.
External Carotid Artery (ECA):
:watermark(/images/watermark_5000_10percent.png,0,0,0):watermark(/images/logo_url.png,-10,-10,0):format(jpeg)/images/overview_image/1035/krGo8RCGxgWB1Ik4c9qg_arteries-of-the-head-external-carotid-artery_en.jpg)
Branches: Numerous branches supply the face and neck. Key branches include:
Superior Thyroid Artery: Supplies the thyroid gland.
Lingual Artery: Supplies the tongue.
Facial Artery: Supplies blood to the face and is palpable near the mandible.
Posterior Auricular Artery: Supplies the scalp behind the ear.
Occipital Artery: Supplies the posterior scalp.
Ascending Pharyngeal Artery: Important for supplying the pharynx.
Maxillary Artery: Provides blood to the maxilla and has up to 16 branches, crucially the middle meningeal artery supplying the dura mater and potential sites for epidural hemorrhage.
Superficial Temporal Artery: Supplies the scalp in the temporal region, notable for procedures linking ECA to ICA in bypass surgeries.
Collateral Circulation:
The posterior communicating artery plays a critical role in connecting blood supply between the internal carotid and basilar arteries. This serves as a backup when one artery is blocked, maintaining blood flow within the brain.
Clinical Implications of Carotid Anatomy
Carotid Sinus:
Function: Acts as a baroreceptor, sensing blood pressure and aiding in heart rate regulation. Overstimulation from carotid massage can prevent strokes but must be performed carefully to avoid dislodging plaque.
Carotid Body:
Function: A chemoreceptor sensing oxygen levels in the blood. Can enlarge in chronic low-oxygen situations, such as high altitude illness or chronic obstructive pulmonary disease (COPD).
Overview of Venous Drainage
Main Veins of the Head and Neck
Internal Jugular Vein (IJV):
Function: Major drainage pathway for the brain, receiving tributaries from the thyroid, facial, and pharyngeal veins.
Clinical Significance: IJV is assessed for central venous pressure; compression can lead to increased intracranial pressure.
External Jugular Vein (EJV):
Function: Drains superficial structures of the head and neck. Typically ligated during surgeries since it is not essential.
Facial Vein:
Function: Drains the face and connects with the IJV, which also includes the common facial vein.
Anterior Jugular Vein:
Function: Connects various regional veins and runs along the midline, potentially complicating surgical procedures like thyroidectomy.
Important Venous Structures
Batson's Plexus:
Description: A valveless venous plexus running from the pelvis to the skull base, significant in the metastasis of cancers.
Clinical Relevance: Enables spread of cancer cells from distant sites (e.g., prostate to brain) due to lack of valves, thus allowing unhindered flow.
Dural Venous Sinuses:
Description: Specialized venous channels formed between the two layers of dura mater, draining blood from the brain back to the IJV.
Examples: Superior sagittal sinus and transversely positioned sinuses.
Clinical Importance: Injuries or bleeding in these areas can severely affect cranial pressure and brain function.
Circulation of Cerebrospinal Fluid (CSF)
Journey: CSF is produced by the choroid plexus and circulates through the brain's ventricles, surrounding the brain and spinal cord.
Arachnoid Granulations: These structures allow CSF to exit into the venous system, typically via the inferior sagittal sinus, preventing backflow and promoting balance in cranial pressure.
Hydrocephalus: A condition resulting from blocked CSF drainage leading to increased intracranial pressure, often necessitating surgical intervention.
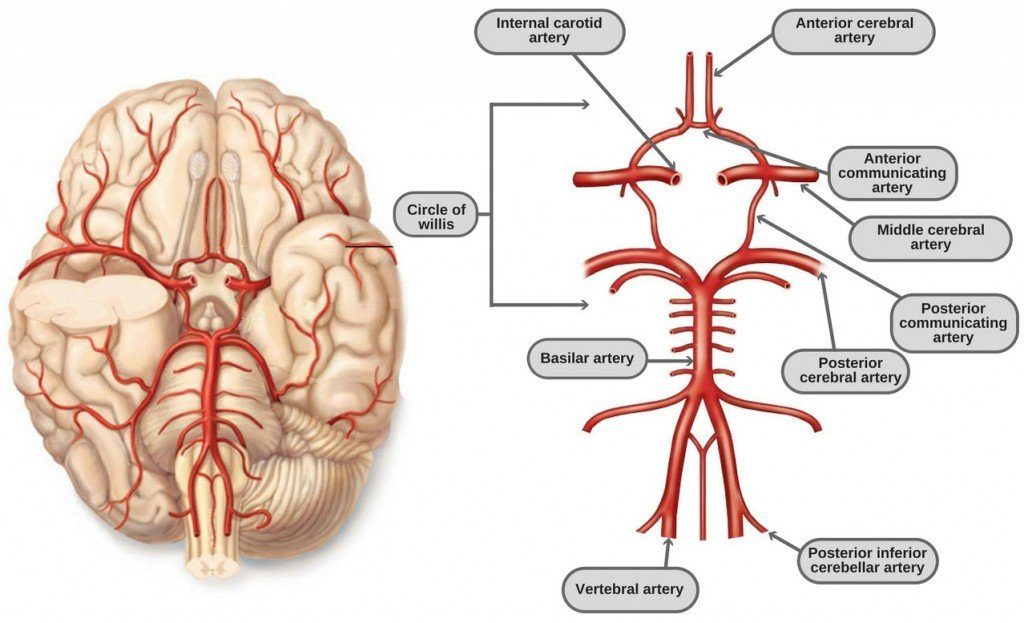
Circle of Willis
The Circle of Willis is crucial for collateral circulation. It is formed by:
Vertebral Arteries: Fuse into the Basilar artery.
Internal Carotid Arteries: Each gives rise to anterior and middle cerebral arteries.
Anterior Communicating Artery: Connects the left and right anterior cerebral arteries.
Posterior Communicating Arteries: Connect internal carotid to posterior cerebral arteries.
Clinical Relevance: Variations in the Circle of Willis can influence stroke outcomes, as absent connections may limit collateral circulation, leading to more severe effects from arterial occlusions.
Summary of Key Clinical Questions
A summary of sample clinical scenarios emphasizes the need for understanding artery function and potential clinical repercussions related to blood flow disruptions, focusing on skills relevant for future neurology studies.
In summary, the course on the vascular system of the head and neck provides foundational knowledge critical for clinical practice, offering a comprehensive understanding of both arterial supply and venous drainage mechanisms.