Oral cavity
OVERVIEW OF THE DIGESTIVE SYSTEM — EXAM NOTES
1. Components of the Digestive System
Digestive system =
Alimentary canal
Associated organs:
Tongue
Teeth
Salivary glands
Pancreas
Liver
Gallbladder
2. Major Functions
Transport of ingested food & water
Secretion of:
Fluids
Electrolytes
Digestive enzymes
Digestion (mechanical + chemical)
Absorption of digested products
Excretion of indigestible remains
3. Key Concept (VERY IMPORTANT)
Lumen of alimentary canal = physically & functionally external to the body
4. Digestion Process
Food is:
Broken down physically + chemically
Converted into absorbable products
Different segments of alimentary canal are:
Morphologically specialized for digestion & absorption
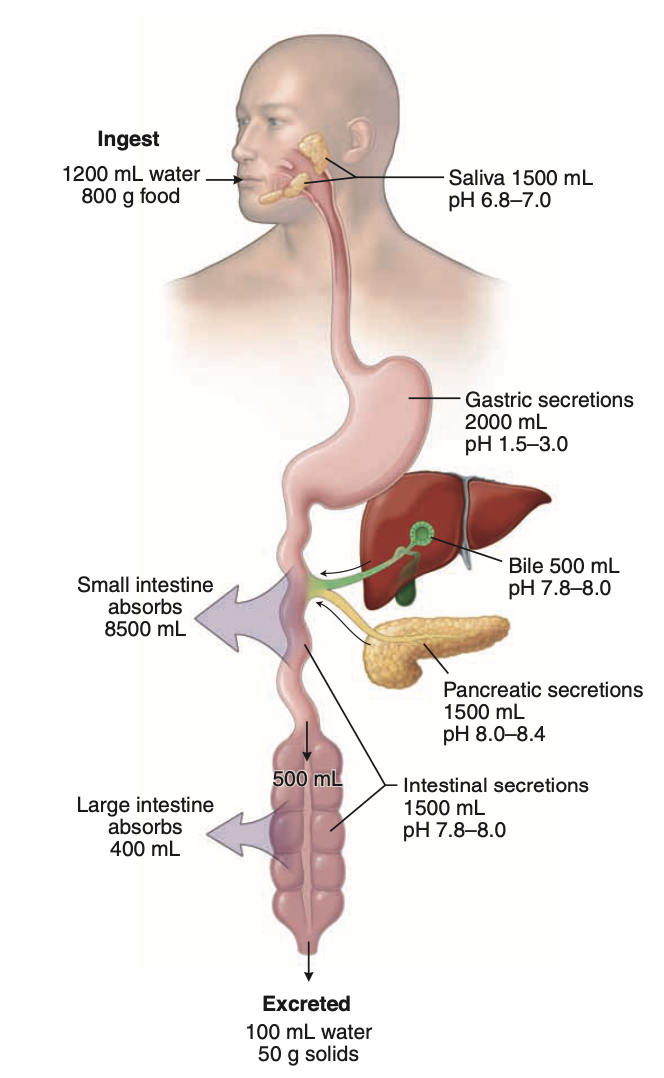
5. Daily Intake & Early Processing
~ 2 L/day of food and water ingested
In oral cavity:
Food undergoes:
Maceration
Moistening
Forms bolus
Assisted by salivary gland secretion
6. Movement Through GI Tract
Rapid passage through pharynx → keeps airway clear
Slower passage through gastrointestinal tract
Assisted by digestive juices (~7 L/day)
7. Digestion & Absorption Sites
Major processes occur in:
Stomach
Small intestine
Absorption:
Mainly in small intestine
Small portion in large intestine
8. Excretion
Undigested food + other substances (mucus, bacteria, desquamated cells, bile pigments)
Excreted as feces
HISTOLOGY-RELEVANT HIGH-YIELD SECTION
9. Alimentary Mucosa (VERY IMPORTANT)
Definition
Surface across which most substances enter the body
Role
Acts as an interface between body & environment
10. Functions of the Alimentary Mucosa
A. Secretion
Produces:
Digestive enzymes
Hydrochloric acid
Mucin
Antibodies
B. Absorption
Epithelium of mucosa absorbs:
Metabolic substrates (digestion products)
Vitamins
Water
Electrolytes
Recyclable materials:
Bile components
Cholesterol
Other essential substances
C. Barrier Function
Prevents entry of:
Noxious substances
Antigens
Pathogenic organisms
D. Immunologic Protection
Lymphatic tissue in mucosa:
First line of immune defense
ORAL CAVITY
1. Components
Mouth and its structures:
Tongue
Teeth and supporting structures (periodontium)
Major salivary glands
Minor salivary glands
Tonsils
2. Divisions of Oral Cavity
Vestibule:
Space between lips, cheeks, and teeth
Oral cavity proper:
Lies behind teeth
Boundaries:
Superior → hard & soft palates
Inferior → tongue & floor of mouth
Posterior → entrance to oropharynx
3. Major Salivary Glands (Paired)
1. Parotid gland
Largest gland
Location → infratemporal region of head
Duct → Parotid (Stensen’s) duct
Opens at:
Parotid papilla
On cheek mucosa opposite upper second molar tooth
2. Submandibular gland
Location → submandibular triangle of neck
Duct → Submandibular (Wharton’s) duct
Opens at:
Sublingual caruncle
On each side of lingual frenulum (floor of oral cavity)
3. Sublingual gland
Location → inferior to tongue within sublingual folds (floor of oral cavity)
Features:
Numerous small excretory ducts
Some ducts → enter submandibular duct
Others → open independently into oral cavity
4. Duct Length
Parotid & submandibular glands → relatively long ducts
Sublingual glands → relatively short ducts
5. Minor Salivary Glands
Location → submucosa of oral cavity
Drainage:
Empty directly into cavity via short ducts
Named by location:
Buccal
Labial
Lingual
Palatine
6. Tonsils
Aggregations of lymphatic nodules
Located around posterior opening of oral and nasal cavities
7. Tonsillar (Waldeyer’s) Ring
Lymphatic tissue forming immunologic protection
Located at shared entrance to digestive & respiratory tracts
Surrounds posterior orifice of oral & nasal cavities
8. Types of Tonsils
1. Palatine tonsils
Located:
Either side of entrance to oropharynx
Between palatopharyngeal & palatoglossal arches
2. Tubal tonsils
Located:
Lateral walls of nasopharynx
Posterior to opening of auditory tube
3. Pharyngeal tonsil (Adenoid)
Located:
Roof of nasopharynx
4. Lingual tonsil
Located:
Base of tongue (superior surface)
ORAL MUCOSA
1. Types of Oral Mucosa
The oral cavity is lined by:
Masticatory mucosa
Lining mucosa
Specialized mucosa
2. Masticatory Mucosa
Location
Gingiva (gums)
Hard palate
Epithelium
Keratinized stratified squamous epithelium
In some areas → Parakeratinized stratified squamous epithelium
Parakeratinized Epithelium
Similar to keratinized epithelium BUT:
Superficial cells retain nuclei
Cytoplasm does not stain intensely with eosin
Nuclei:
Pyknotic (highly condensed)
Persist until cell exfoliation
Lamina Propria
Thick papillary layer of loose connective tissue:
Contains blood vessels and nerves
Some nerves:
End as bare axon endings (sensory receptors)
Some end in Meissner’s corpuscles
Deep to it:
Reticular layer (denser connective tissue)
Function/Structure
Depth and number of connective tissue papillae:
Contribute to relative immobility
Protect from frictional and shearing stress
Special Attachment
Palatine raphe (midline of hard palate):
Mucosa firmly adheres to bone
No submucosa
Same applies to:
Gingiva
Submucosa (Hard Palate)
When present:
Anterior → Fatty zone (adipose tissue)
Posterior → Glandular zone
Continuous with soft palate submucosa
Collagen Bands
In submucosal regions:
Thick collagenous bands extend from mucosa to bone
3. Lining Mucosa
Location
Lips
Cheeks
Alveolar mucosal surface
Floor of mouth
Inferior surfaces of tongue
Soft palate
Structures Covered
Skeletal muscle:
Lips, cheeks, tongue
Bone:
Alveolar mucosa
Glands:
Soft palate, cheeks, inferior tongue
Features
Fewer and shorter papillae
Allows adjustment to movement of underlying muscles
Epithelium
Generally Nonkeratinized stratified squamous epithelium
In some places → Parakeratinized
Vermilion Border of Lip
Epithelium is keratinized
Nonkeratinized Epithelium Layers
(ONLY 3 layers)
Stratum basale
Single layer on basal lamina
Stratum spinosum
Several cell layers
Stratum superficiale
Surface layer
Thickness
Nonkeratinized lining epithelium:
Thicker than keratinized epithelium
Cells Present
Keratinocytes
Langerhans’ cells
Melanocytes
Merkel’s cells
Lamina Propria (Lining Mucosa)
Contains:
Blood vessels
Nerves
Bare axon endings
Encapsulated sensory endings in some papillae
Histologic Identification
Alveolar mucosa:
Numerous deep papillae
Other lining mucosa:
Shallow papillae
4. Submucosa (Lining Mucosa)
General
Present except:
Inferior surface of tongue
Contents
Large blood vessels
Nerves
Lymphatic vessels
Special Features
Contains:
Minor salivary glands (lips, tongue, cheeks)
Inferior Surface of Tongue
Submucosa contains:
Collagen fibers
Elastic fibers
Function:
Bind mucosa to underlying muscle
Sebaceous Glands
Occasionally present (without hair follicle)
Locations:
Lateral to corner of mouth
Cheeks opposite molar teeth
Called:
Fordyce spots
Visible to the eye
5. Submucosa – Vascular Supply
Contains:
Larger blood vessels
Nerves
Lymphatic vessels
Supplies:
Subepithelial neurovascular networks in lamina propria
6. Specialized Mucosa
Function:
Taste sensation
Location:
Dorsal surface of tongue
Contains:
Papillae
Taste buds → responsible for taste generation
TONGUE –
1. General Structure
Tongue = muscular organ projecting into oral cavity from inferior surface
2. Lingual Muscles
Two types:
Extrinsic muscles
One attachment outside tongue
Intrinsic muscles
Confined entirely within tongue
Muscle Arrangement
Striated muscle arranged in bundles:
Run in three planes
Each at right angles to others
Function
Provides:
Flexibility
Precision of movement
Essential for:
Speech
Digestion
Swallowing
Additional Feature
Variable adipose tissue between muscle fibers
3. Dorsal Surface of Tongue
Division
Divided into:
Anterior 2/3
Posterior 1/3
Separated by:
Sulcus terminalis (V-shaped)
Foramen Cecum
Located at apex of V
Remnant of embryonic origin of thyroid gland
4. Lingual Papillae
Cover dorsal surface anterior to sulcus terminalis
With taste buds → form specialized mucosa
Types (4)
Filiform
Fungiform
Circumvallate
Foliate
5. Filiform Papillae
Smallest & most numerous
Shape:
Conical
Elongated
Composition:
Connective tissue core
Covered by highly keratinized stratified squamous epithelium
No taste buds
Function:
Mechanical only
Distribution:
Entire anterior dorsal surface
Tips point backward
Arranged in rows:
Diverge left & right from midline
Parallel to arms of sulcus terminalis
6. Fungiform Papillae
Shape:
Mushroom-shaped projections
Location:
Dorsal surface
Scattered among filiform papillae
Visibility:
Seen as small spots
More numerous:
Near tip of tongue
Epithelium:
Stratified squamous
rare Contain taste buds
7. Circumvallate Papillae
Shape:
Large, dome-shaped
Location:
Just anterior to sulcus terminalis
Number:
8–12 papillae
Structure
Surrounded by:
Moat-like invagination
Lined by:
Stratified squamous epithelium
Contain:
Numerous taste buds
Associated Glands
Lingual salivary (von Ebner’s) glands
Ducts open into base of moats
Secrete serous fluid
Function:
Flush material from moat
Allow rapid response of taste buds
8. Foliate Papillae
Structure:
Parallel low ridges
Separated by deep mucosal clefts
Orientation:
At right angles to long axis of tongue
Location:
Lateral edge of tongue
9. Posterior Tongue (Base)
Dorsal surface shows:
Smooth bulges
Cause:
Presence of lingual tonsil in lamina propria
TASTE BUDS & TASTE –
1. Location of Taste Buds
Present on:
Fungiform papillae
Foliate papillae
Circumvallate papillae
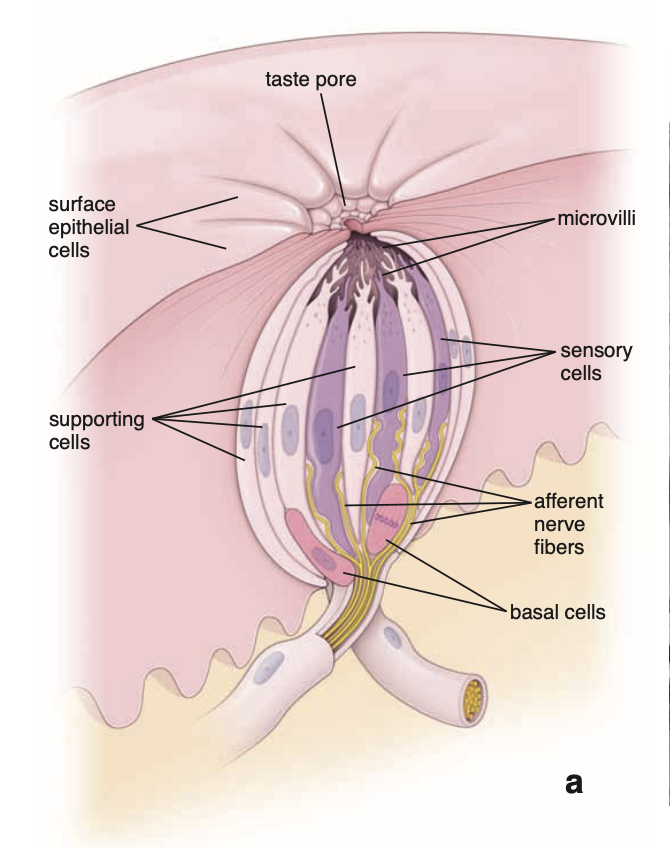
2. Structure of Taste Buds
Appear as:
Oval, pale-staining bodies
Extend through:
Full thickness of epithelium
Taste Pore
Small opening at apex of taste bud
Opens onto epithelial surface
3. Cell Types in Taste Buds (3)
1. Neuroepithelial (Sensory) Cells
Most numerous
Elongated cells:
Extend from basal lamina → taste pore
Apical surface:
Contains microvilli
Connections:
Tight junctions with neighboring cells
Base:
Form synapse with afferent sensory neurons of:
Facial nerve (CN VII)
Glossopharyngeal nerve (CN IX)
Vagus nerve (CN X)
Turnover time:
~10 days
2. Supporting Cells
Less numerous
Elongated:
Extend from basal lamina → taste pore
Features:
Microvilli on apical surface
Tight junctions present
Do NOT synapse with nerve cells
Turnover time:
~10 days
3. Basal Cells
Small cells
Located:
Basal portion near basal lamina
Function:
Stem cells for other two cell types
4. Additional Locations of Taste Buds
Glossopalatine arch
Soft palate
Posterior surface of epiglottis
Posterior wall of pharynx (down to level of cricoid cartilage)
5. Taste – Basic Concept
Chemical sensation
Caused by:
Interaction of tastants with receptors on:
Apical surface of neuroepithelial cells
6. Five Basic Taste Stimuli
Sweet
Salty
Bitter
Sour
Umami
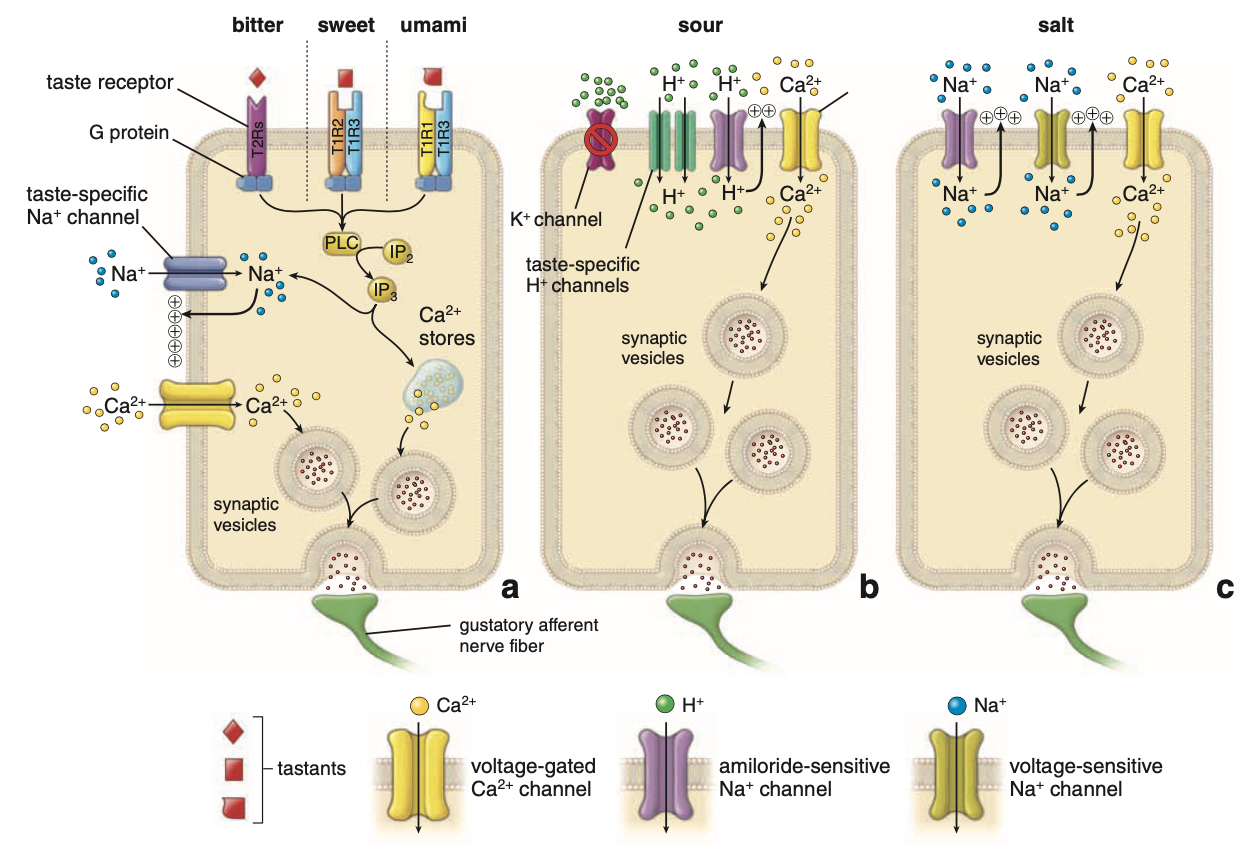
7. Mechanisms of Taste Transduction
General Mechanisms
Tastants act by:
Opening ion channels → (salt, sour)
Closing ion channels → (sour)
Activating G protein–coupled receptors → (bitter, sweet, umami)
8. Taste Receptors
Belong to:
T1R and T2R receptor families
All are:
G protein–coupled receptors
9. Bitter Taste
Detected by:
~30 types of T2R receptors
Each receptor:
Single transmembrane protein
Coupled to its own G protein
10. Signal Transduction Pathway
Tastant → activates receptor → activates G protein
G protein stimulates:
Phospholipase C
Leads to:
↑ Inositol 1,4,5-triphosphate (IP₃)
IP₃ Effects
Activates:
Taste-specific Na⁺ channels
Causes:
Na⁺ influx → depolarization
Depolarization
Opens:
Voltage-gated Ca²⁺ channels
Result
↑ Intracellular Ca²⁺:
From extracellular influx
From intracellular stores (via IP₃)
Leads to:
Neurotransmitter release
Generates:
Nerve impulses in gustatory afferent fibers
11. Sweet Taste
Receptors:
G protein–coupled
Two subunits:
T1R2
T1R3
Mechanism:
Same second messenger cascade as bitter
12. Umami Taste
Stimulated by:
Amino acids:
L-glutamate
Aspartate
Related compounds
Common in:
Asparagus
Tomatoes
Cheese
Meat
Receptors
Two subunits:
T1R3 (same as sweet)
T1R1 (unique)
Mechanism
Same as bitter taste pathway
Special Note
Monosodium glutamate (MSG):
Stimulates umami receptors
13. Important Functional Concept
Neuroepithelial cells:
Express only one class of receptor proteins
Therefore:
Different tastes (e.g., bitter vs sweet)
Are transmitted via different nerve fibers to CNS
SALTY & SOUR TASTE + TASTE DISTRIBUTION
1. General Concept
Sodium ions (Na⁺) → responsible for salty taste
Hydrogen ions (H⁺) → responsible for sour taste
Both:
Act directly on ion channels
Mechanisms:
Similar to signaling in synapses and neuromuscular junctions
2. Sour Taste
Cause
Generated by:
H⁺ protons from hydrolysis of acidic compounds
Mechanism
H⁺:
Blocks K⁺ channels
→ alters membrane potential
→ causes depolarization
H⁺ also:
Enters cell via:
Amiloride-sensitive Na⁺ channels
Specific channels:
PKD1L3
PKD2L1
Further Steps
Entry of H⁺:
Activates:
Voltage-sensitive Ca²⁺ channels
Ca²⁺ influx:
Causes:
Migration of synaptic vesicles
Vesicle fusion
Neurotransmitter release
Result:
Action potentials in sensory nerve fibers
3. Salty Taste
Cause
Stimulated by:
Table salt (NaCl)
Derived from:
Na⁺ ions
Mechanism
Na⁺ enters neuroepithelial cells via:
Amiloride-sensitive Na⁺ channels
Same channels involved in sour taste
These channels:
Different from voltage-sensitive Na⁺ channels (nerve/muscle)
Further Steps
Na⁺ entry:
Causes:
Depolarization
Leads to activation of:
Voltage-sensitive Na⁺ channels
Voltage-sensitive Ca²⁺ channels
Final Outcome
Ca²⁺ influx:
Triggers:
Neurotransmitter release from synaptic vesicles
Result:
Stimulation of gustatory nerve fibers
4. Regional Taste Sensitivity (Exam Point)
Tip of tongue:
Detects → Sweet
Immediately posterolateral to tip:
Detects → Salty
More posterolateral regions:
Detect → Sour
Circumvallate papillae:
Detect → Bitter and Umami
LINGUAL TONSIL + NERVE SUPPLY OF TONGUE
1. Lingual Tonsil
Definition
Accumulations of lymphatic tissue at the base of the tongue
Location
In lamina propria of root/base of tongue
Located:
Posterior to sulcus terminalis
Structure
Contains:
Diffuse lymphatic tissue
Lymphatic nodules with germinal centers
Epithelium
Epithelial crypts:
Invaginate into lingual tonsil
Epithelium may be:
Difficult to distinguish due to:
Large number of lymphocytes infiltrating it
Between nodules:
Epithelium resembles lining epithelium
Associated Glands
Mucous lingual salivary glands:
Present within lingual tonsil
May extend into muscle of base of tongue
2. Nerve Supply of Tongue
General Concept
Complex nerve supply provided by:
Cranial nerves
Autonomic nervous system
3. General Sensation
Anterior 2/3 of tongue
Carried by:
Mandibular division of trigeminal nerve (CN V)
Posterior 1/3 of tongue
Carried by:
Glossopharyngeal nerve (CN IX)
Vagus nerve (CN X)
4. Taste Sensation
Anterior to sulcus terminalis
Carried by:
Chorda tympani (branch of facial nerve, CN VII)
Posterior to sulcus
Carried by:
Glossopharyngeal nerve (CN IX)
Vagus nerve (CN X)
5. Motor Innervation
Musculature of tongue supplied by:
Hypoglossal nerve (CN XII)
6. Autonomic Innervation
Type
Sympathetic and parasympathetic nerves
Function
Supply:
Blood vessels
Small salivary glands of tongue
Ganglion Cells
Present within tongue
Belong to:
Postsynaptic parasympathetic neurons
Function:
Supply minor salivary glands
Sympathetic Neurons
Cell bodies located in:
Superior cervical ganglion
TEETH
1. General
Teeth consist of:
Several layers of specialized tissues
2. Main Tissues of Teeth (3)
1. Enamel
Characteristics:
Hard
Thin
Translucent
Type:
Acellular mineralized tissue
Location:
Covers crown of the tooth
2. Dentin
Most abundant dental tissue
Location:
Lies:
Deep to enamel (in crown)
Deep to cementum (in root)
Structure & Function
Has:
Tubular structure
Specific biochemical composition
Function:
Supports:
Enamel
Cementum
3. Cementum
Characteristics:
Thin
Pale-yellowish
Type:
Bone-like calcified tissue
Location
Covers:
Dentin of the root
Properties
Compared to dentin:
Softer
More permeable
Clinical Note
Easily removed by:
Abrasion
Especially when:
Root surface exposed to oral environment
ENAMEL –
1. General Features
Hardest substance in the body
Composition:
96–98% calcium hydroxyapatite
2. Basic Characteristics
Acellular mineralized tissue
Covers:
Crown of the tooth
Once formed:
Cannot be replaced
3. Origin & Nature
Derived from:
Epithelium
Unlike bone:
Not formed from connective tissue
Properties:
More highly mineralized and harder than any other mineralized tissue
4. Crown Definitions
Clinical crown:
Portion visible above gum line
Anatomic crown:
Entire portion covered by enamel
Includes part below gum line
6. Boundaries
Root:
Covered by cementum
7. Enamel Rods (Key Feature)
General
Enamel composed of:
Enamel rods
Rods:
Span entire thickness of enamel
Structure
Made of:
Nonstoichiometric carbonated calcium hydroxyapatite crystals
Extent
Each rod:
Extends from:
Dentinoenamel junction → enamel surface
Cross-section Appearance
Keyhole shape:
Head:
Ballooned part
Oriented superiorly
Tail:
Directed inferiorly toward root
Crystal Orientation
In head:
Crystals → parallel to long axis of rod
In tail:
Crystals → more oblique
Interrod Region
Spaces between rods:
Also filled with enamel crystals
8. Incremental Lines
Striations (Contour lines of Retzius):
Represent:
Rhythmic growth of enamel
9. Neonatal Line
Seen in:
Deciduous teeth
Feature:
Wide hypomineralized line
Significance:
Marks:
Nutritional changes between prenatal and postnatal life
10. Post-Eruptive Enamel
Lacks:
Cells
Cell processes
Not static:
Influenced by salivary gland secretions
11. Role of Saliva
Essential for:
Maintenance of enamel
Contains:
Digestive enzymes
Secreted antibodies
Inorganic (mineral) components
ENAMEL DEVELOPMENT (AMELOGENESIS) –
1. Cells Producing Tooth Tissues
Enamel → produced by:
Ameloblasts (of enamel organ)
Dentin → produced by:
Neural crest–derived odontoblasts
From adjacent mesenchyme
2. Enamel Organ
Origin
Derived from:
Ectodermal epithelial cells of oral cavity
Tooth Development – Initial Stage
Begins with:
Proliferation of oral epithelium
Forms:
Dental lamina
Horseshoe-shaped band of tissue
Bud Stage
Further proliferation from dental lamina:
Forms:
Rounded, bud-like outgrowth
One for each tooth
Projects into:
Underlying mesenchyme
Represents:
Early enamel organ
Cap Stage
Cell mass enlarges
Develops:
Concavity opposite origin from dental lamina
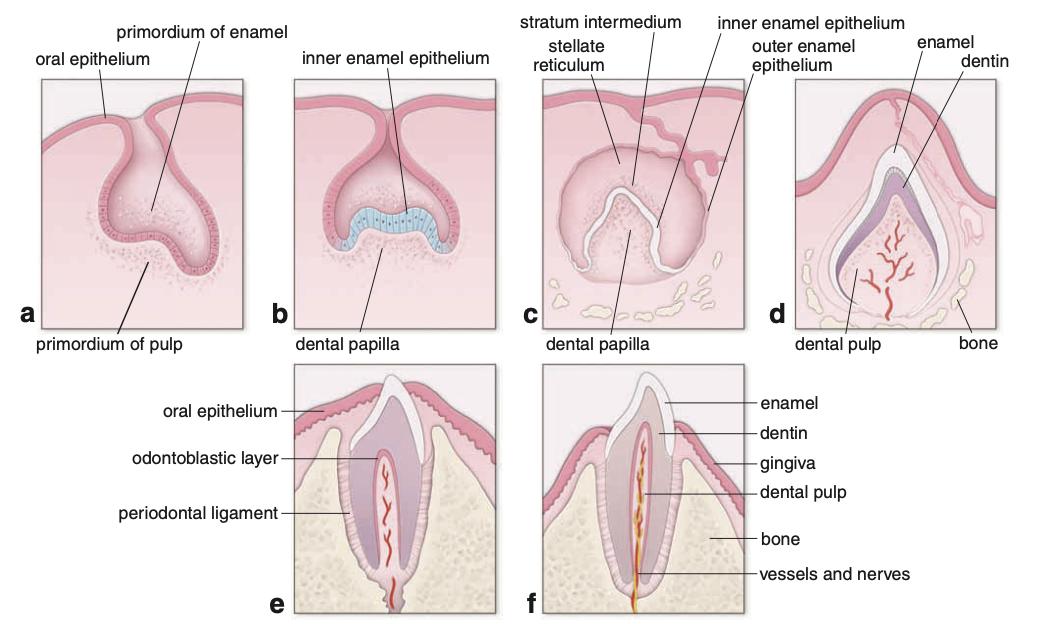
Bell Stage
Further growth leads to:
Bell stage
Enamel organ now has 4 cellular components:
1. Outer enamel epithelium
Single cell layer
Forms:
Convex surface
2. Inner enamel epithelium
Single cell layer
Forms:
Concave surface
3. Stratum intermedium
Cell layer:
Internal to inner enamel epithelium
4. Stellate reticulum
Cells:
Stellate appearance
Occupy:
Inner portion of enamel organ
3. Odontoblast & Ameloblast Formation
Odontoblasts
Derived from:
Neural crest–derived preodontoblasts
Location:
Adjacent to inner enamel epithelium in bell stage
Features:
Become columnar
Epithelial-like appearance
Function:
Form dentin
Ameloblasts
Derived from:
Inner enamel epithelium cells
Along with:
Stratum intermedium
Function:
Enamel production
Dental Lamina
Degenerates:
Early stage (before dentinogenesis & amelogenesis)
Result:
Tooth primordium becomes:
Detached from origin
4. Amelogenesis (Enamel Formation)
Defined as:
Matrix-mediated biomineralization process
5. Stages of Amelogenesis
1. Matrix Production (Secretory Stage)
Also called:
Secretory stage
Sequence
Dentin is produced first
Then:
Partially mineralized enamel matrix
Deposited on:
Surface of previously formed dentin
Cells
Secretory-stage ameloblasts
Function
Produce:
Organic proteinaceous matrix
Cellular Machinery
Activity of:
Rough endoplasmic reticulum (rER)
Golgi apparatus
Secretory granules
Outcome
Enamel matrix production continues:
Until full thickness of enamel is achieved
2. Matrix Maturation Stage
Process
Maturation of partially mineralized enamel involves:
Removal of organic material
Continued influx of:
Calcium
Phosphate
Cells
Maturation-stage ameloblasts
Function
Act as:
Transport epithelium
Move substances:
Into and out of enamel
Cell Changes
Undergo:
Cyclical morphological alterations
Correspond to:
Cyclical calcium entry into enamel
AMELOBLASTS & ENAMEL MATRIX –
1. Secretory-Stage Ameloblasts
General
Polarized columnar cells
Function:
Produce enamel
Location
Lie:
Directly adjacent to developing enamel
Tomes’ Process
Present at:
Apical pole
Surrounded by:
Developing enamel
Cytoplasmic Features
Cluster of mitochondria
Actin filaments:
In proximal terminal web (base of cell)
Responsible for:
Eosinophilic staining (H&E)
Nucleus:
Located adjacent to mitochondria
Main cytoplasm contains:
rER
Golgi apparatus
Secretory granules
Other cell elements
Junctional Complexes
Present at:
Apical and basal parts
Function:
Maintain:
Integrity
Orientation of ameloblasts
Role:
Movement away from dentinoenamel junction
Actin Filaments
Associated with junctional complexes
Function:
Help movement of ameloblast over developing enamel
Enamel Rod Formation
Rod follows:
Path of ameloblast
Therefore:
Direction of enamel rod:
Reflects path of secretory-stage ameloblast
Basal Relation
Adjacent to:
Stratum intermedium
Stratum Intermedium (Related Feature)
Plasma membrane contains:
Alkaline phosphatase
Function:
Enzyme active in calcification
Stellate Reticulum
Located external to:
Stratum intermedium
Separated from blood vessels by:
Basal lamina
2. Maturation-Stage Ameloblasts
Function
Transport substances needed for enamel maturation
Histologic Feature
Presence of:
Striated (ruffled) border
Cycle Types
Ruffled border cells:
~70% of cycle
Smooth-ended cells:
~30% of cycle
Structural Changes During Maturation
No:
Stratum intermedium
Cells from:
Stratum intermedium
Stellate reticulum
Outer dental epithelium
Undergo:
Collapse
Reorganization
Become:
Indistinguishable as separate layers
Papillary Layer
Formed by:
Invagination of blood vessels
Contains:
Stellate papillary cells
Located adjacent to:
Maturation-stage ameloblasts
Cellular Features
Maturation-stage ameloblasts & papillary cells:
Contain numerous mitochondria
Indicates:
High energy requirement
Function as:
Transporting epithelium
3. Enamel Matrix Proteins
General
Enamel matrix:
Highly heterogeneous
Contains proteins:
Encoded by multiple genes
1. Amelogenins
Function:
Establish & maintain:
Spacing between enamel rods
Important in:
Early enamel development
2. Ameloblastins
Produced by:
Ameloblasts (early secretory → late maturation stages)
Function:
Not well understood
Suggested roles:
Guide mineralization
Control:
Elongation of enamel crystals
Form:
Junctional complexes between enamel crystals
3. Enamelins
Distributed:
Throughout enamel layer
Undergo:
Proteolytic cleavage during maturation
Low-molecular-weight products:
Retained in mature enamel
Often on surface of enamel crystals
4. Tuftelins
Location:
Near dentinoenamel junction
Properties:
Acidic and insoluble
Function:
Aid in:
Nucleation of enamel crystals
Enamel Tufts
Contain:
Tuftelins
Feature:
Hypomineralization
Have:
Higher organic content than rest of enamel
4. Final Maturation Changes
Continued mineralization:
Leads to enamel becoming:
Hardest substance in body
Protein Removal
During maturation:
Amelogenins and ameloblastins removed
Mature Enamel Contains
Only:
Enamelins
Tuftelins
Fate of Ameloblasts
Degenerate:
After enamel formation complete
Timing:
Around tooth eruption through gum
DENTIN –
1. General
Calcified material
Forms:
Most of the tooth substance
2. Location & Composition
Lies:
Deep to enamel (crown)
Deep to cementum (root)
Hydroxyapatite content:
~70%
Less than enamel
More than bone and cementum
3. Odontoblasts
Function
Secrete:
Dentin
Location
Form:
Epithelial-like layer
Situated:
On inner surface of dentin
In contact with:
Pulp
Cell Features
Columnar cells
Contain:
Well-developed rER
Large Golgi apparatus
Other organelles for protein synthesis & secretion
Apical Surface
In contact with:
Forming dentin
Junctional Complexes
Present between odontoblasts
Function:
Separate:
Dentin compartment
Pulp chamber
4. Dentin Formation & Tubules
Odontoblast Movement
As dentin is deposited:
Odontoblasts:
Retreat inward
Dentin Tubules
Odontoblast processes remain:
Embedded in dentin
Located in:
Narrow channels → dentinal tubules
Growth
Tubules & processes:
Continue to elongate
Due to:
Rhythmic dentin deposition
5. Incremental (Growth) Lines
Formed by:
Rhythmic growth of dentin
Types
Incremental lines of von Ebner
Lines of Owen (thicker)
Significance
Mark:
Important developmental events:
Birth → neonatal line
Exposure to substances (e.g., lead)
6. Predentin
Definition
Newly secreted organic matrix
Location:
Closest to odontoblast cell body
Status:
Not yet mineralized
Composition
Proteins similar to bone
Contains two unique proteins:
7. Predentin Proteins
1. Dentin Phosphoprotein (DPP)
~45 kDa
Highly acidic phosphorylated protein
Rich in:
Aspartic acid
Phosphoserine
Function:
Binds large amounts of calcium
Involved in:
Initiation of mineralization
Control of:
Mineral size
Mineral shape
2. Dentin Sialoprotein (DSP)
~100 kDa
Type:
Proteoglycan
Rich in:
Aspartic acid
Glutamic acid
Serine
Glycine
Chondroitin 6-sulfate
Function:
Involved in:
Mineralization process
8. Abacus Bodies
Formation
Present in:
Golgi vesicles of odontoblasts
Structure
Arrays of:
Filamentous collagen precursor
Associated with:
Calcium-containing granules
Function
Give rise to:
Abacus bodies
Maturation
Become:
More condensed
Develop into:
Secretory granules
1. General
Calcified material
Forms:
Most of the tooth substance2. Location & Composition
Lies:
Deep to enamel (crown)
Deep to cementum (root)
Hydroxyapatite content:
~70%
Less than enamel
More than bone and cementum
3. Odontoblasts
Function
Secrete:
Dentin
Location
Form:
Epithelial-like layer
Situated:
On inner surface of dentin
In contact with:
Pulp
Cell Features
Columnar cells
Contain:
Well-developed rER
Large Golgi apparatus
Other organelles for protein synthesis & secretion
Apical Surface
In contact with:
Forming dentin
Junctional Complexes
Present between odontoblasts
Function:
Separate:
Dentin compartment
Pulp chamber
4. Dentin Formation & Tubules
Odontoblast Movement
As dentin is deposited:
Odontoblasts:
Retreat inward
Dentin Tubules
Odontoblast processes remain:
Embedded in dentin
Located in:
Narrow channels → dentinal tubules
Growth
Tubules & processes:
Continue to elongate
Due to:
Rhythmic dentin deposition
5. Incremental (Growth) Lines
Formed by:
Rhythmic growth of dentin
Types
Incremental lines of von Ebner
Lines of Owen (thicker)
Significance
Mark:
Important developmental events:
Birth → neonatal line
Exposure to substances (e.g., lead)
Application
Useful in:
Forensic medicine
6. Predentin
Definition
Newly secreted organic matrix
Location:
Closest to odontoblast cell body
Status:
Not yet mineralized
Composition
Proteins similar to bone
Contains two unique proteins:
7. Predentin Proteins
1. Dentin Phosphoprotein (DPP)
~45 kDa
Highly acidic phosphorylated protein
Rich in:
Aspartic acid
Phosphoserine
Function:
Binds large amounts of calcium
Involved in:
Initiation of mineralization
Control of:
Mineral size
Mineral shape
2. Dentin Sialoprotein (DSP)
~100 kDa
Type:
Proteoglycan
Rich in:
Aspartic acid
Glutamic acid
Serine
Glycine
Chondroitin 6-sulfate
Function:
Involved in:
Mineralization process
8. Abacus Bodies
Formation
Present in:
Golgi vesicles of odontoblasts
Structure
Arrays of:
Filamentous collagen precursor
Associated with:
Calcium-containing granules
Function
Give rise to:
Abacus bodies
Maturation
Become:
More condensed
Develop into:
Secretory granules
SUPPORTING TISSUES OF TEETH (PERIODONTIUM) –
1. Components
Supporting tissues include:
Alveolar bone (of maxilla & mandible)
Periodontal ligament
Gingiva
2. Alveolar Processes
Contain:
Sockets (alveoli) for roots of teeth
3. Alveolar Bone Proper
Thin layer of compact bone
Forms:
Wall of alveolus
Function:
Site of attachment for:
Periodontal ligament
Remaining alveolar process:
Consists of:
Supporting bone
4. Periodontal Ligament (PDL)
Definition
Fibrous connective tissue
Joins:
Tooth to surrounding bone
Functions
Bone remodeling (during tooth movement)
Proprioception
Tooth eruption
Histology
Tissue Types
Contains:
Dense connective tissue
Loose connective tissue
Dense Connective Tissue
Contains:
Collagen fibers
Fibroblasts
Elongated
Parallel to long axis of collagen fibers
Fibroblast Function
Move back and forth:
Leave trail of collagen fibers
Contain:
Internalized collagen fibrils
These fibrils:
Digested by:
Lysosomal hydrolytic enzymes
Function:
Produce collagen
Resorb collagen
Adjust continuously to:
Tooth stress and movement
Loose Connective Tissue
Contains:
Blood vessels
Nerve endings
Additional Fibers
Oxytalan fibers:
Thin
Longitudinally disposed
Attach:
Bone ↔ cementum
Some associated with:
Adventitia of blood vessels
5. Gingiva
Definition
Part of mucous membrane:
Commonly called gums
Location
Around:
Neck of tooth
Attachment
Firmly attached to:
Tooth
Underlying alveolar bone
Parts of Gingiva
1. Gingival mucosa
Same as:
Masticatory mucosa
2. Junctional Epithelium (Attachment Epithelium)
Function:
Adheres firmly to tooth
Attachment Mechanism
Secretes:
Basal lamina–like material
Adheres to tooth surface
Cells attach via:
Hemidesmosomes
Epithelial Attachment
Includes:
Basal lamina + hemidesmosomes
Age-related Change
Young individuals:
Attachment to enamel
Older individuals:
Attachment to cementum
Due to:
Passive tooth eruption
Gingival recession
6. Gingival Sulcus
Located:
Above epithelial attachment
Description:
Shallow crevice
Lined by:
Crevicular epithelium
Continuous with:
Junctional epithelium
7. Periodontium (Definition)
All tissues involved in:
Attachment of tooth to maxilla & mandible
Includes
Crevicular epithelium
Junctional epithelium
Cementum
Periodontal ligament
Alveolar bone