Cardiac
Includes blood, heart, and blood vessels.
Cardiovascular disease is leading cause of death in US and MI is primary cause of cardiovascular related death. MI can occur with no warning.
Modifiable Risks
Elevated lipid levels (diets can help)
Hypertension
Smoking
Diabetes mellitus
Sedentary lifestyle
Stress
Obesity
Nonmodifiable Risks
Age
Gender (more common in men, more common in woman after menopause)
Genetics
Race
Hypertension: Primary cause is unknown. Secondary cause is underlying health problems. over 140/ over 90
Primary Hypertension: Risk factors are overweight/obesity, tobacco use, and high sodium diet.
Secondary Hypertension: Caused by systemic disease or medications.
Effects of hypertension: Silet killer, builds up slowing over time and is really hard on smaller blood vessels in the eyes, kidneys and brain that lead to vision loss, kidney damage, and memory problems.
Complications: Renal damage, aneurysms, stroke, hypertensive crisis, vision loss, memory problems.
Symptoms: Patients can be completely asymptomatic, but some symptoms include headache, SOA, nosebleeds, and severe anxiety. Some signs include an elevated BP on consecutive readings.
Hypertensive Emergencies: Over 180 and Over 120 in the presence of end organ failure.
Malignant hypertension: End organ damage where the kidney, eyes, and brain are affected.
Hypertensive Encephlopathy: Cerebral edema leading to neuro symptoms like confusion and headaches.
Symptoms include nausea, vomiting, chest pain, SOA, blurry vision, confusion, LOC
Person is likely about to have a stroke by blowing out blood vessels in the brain
Atherosclerosis
Plaque composed of cholesterol fat and other substances builds up inside the arteries, narrowing them and potentially leading to serious health problems. Starts with damage to inner lining of arteries. Inflammatory cells and cholesterol accumulate at these damaged areas forming plaque and as that builds up, it hardens and causes arteries to narrow, reducing blood flow.
Atherosclerosis can affect any artery in the body but are common in coronary and carotid arteries.
Cause and risk factors
High cholesterol
High BP that damages artery walls
Smoking
Diabetes that damages blood vessels
Obesity that increases the risk of high cholesterol
Lack of physical activity that leads to high cholesterol
Increases with age
Chronic inflammation in body
Varicose Veins (Venus Insufficiency)
Not life threatening. Due to damaged valve
Vein in which blood has pooled.
Related to trauma or prolonged standing on feet. Can also be genetic.
Thrombus/Embolus
More dangerous, often seen in the calf. Do not massage!
A thrombus is a blood clot that forms in a blood vessel, obstructing blood flow in that location. It is often a result of a combination of factors, including damage to the vessel wall, changes in blood flow, or increased coagulability of the blood. Thrombi can be classified as either venous or arterial, depending on the type of blood vessel in which they form.
An embolus, on the other hand, is a thrombus or a fragment of it that has broken free and is traveling through the bloodstream. It can obstruct blood flow to distant sites in the body, potentially causing serious complications, such as a stroke or pulmonary embolism, depending on where the embolus lodges. Emboli can also consist of other materials, such as fat, air, or amniotic fluid, but the thrombus and its fragments are the most common causes of emboli.
Types include fatty plaques, blood clot formation, dehydration, prolonged sitting, air from IV, fat that is associated with trauma of long bones, bacteria, and amniotic fluid that is seen after birth.
Deep Vein Thrombosis
Venous
Pulse present, skin color is rubor, skin temp is warm, and edema is present. Usually unilateral.
Symptoms: Dry flakey hyperpigmentation, discoloration of extremities, edema may obliterate pule, venous stasis ulcers, paresthesia.
Stages
C1 spider veins
C2 varicose veins
C3 edema
C4 skin changes
C5, C6 venous ulcers
Complicastions:
Pulmonary embolism: Most serious. Blood clot breaks off and travels to lungs. Causes chest pain, SOA, and death.
Chronic Venous Insufficiency: Long term. Leads to swelling, pain, and skin ulcers.
Post Thrombotic Syndrome: Group of symptoms that develop after DVT. Pain, swelling, decoration. Chronic and debilitating.
Pulmonary Embolism
Sudden sharp chest pain that worsens when breathing deep, SOA, coughing up pink and frothy blood, dizziness, anxiety and a sense of impending doom, sweating, tachycardia, possible pain on one leg if from a DVT
Requires immediate medical treatment to dissolve the clot and prevent further damage to lung
Diagnosed with D-dimer, PT/INR, aPTT, CT pulmonary angiograph, Doppler ultrasound of leg, ABG to look for acidosis, O2 saturation, an EKG to rule out MI
Treatment: O2, anticoagulants, thrombolytics, possible surgery.
Nursing Care
Elevate HOB, do a lung assessment, administer O2, give IV fluids, use pulse oximetry, monitor cardiac
Administer medications like anticoagulants and thrombolytics
Bleeding precautions
Patient education, prepare patient for imaging
DVT precautions (Avoid massaging legs, use pressure stocking)
Peripheral Artery Disease (PAD) (Arterial Insufficiency)
There is inadequate blood flow through the arteries due to
Atherosclerosis: Buildup on fatty deposits (plaque) in arteries and narrows them
Blood clots: Clots in arteries block blood flow
Trauma: Injuries that damage arteries like a big bruise.
Signs: Discoloration, shiny hairless skin, cool to tough, slow capillary refill, ulcers
Pain, Pallor, Pulselessness, Paralysis, Paresthesia
Ealy signs:
Shiny, tight, hairless skin often on shin of one or both legs. Skin may be glossy, thin and stretched
Caused by reduction of O2 to skin
Toenails become brittle, skin is easily damaged and slow to heal
Later Signs:
Symptoms are from insufficient blood flow to extremity invoolved
Intermittent claudication (pain in legs during exercise that resolves with rest)
Reduces blood flow to muscles, leading to pain when they are exerted.
Symptoms: Pain in legs usually in calves, thighs and buttock. Pain in legs that worsen with exercise but improve with rest. Cramping or burning sensation. Numbness or tingling in legs. Shiny or cold skin on affected legs.
Numbness or tinging in feet or toes
Coldness to extremities
Ulcers on feet or toes that do not heal
Weak or absent pulses in legs or one leg pulse is weaker than the other
Gangrene
Arterial thrombus is cause of PAD
Clot in artery. Location of symptoms depends on location of clot
Pain is sharp, throbbing, cramping
Pulse is weak and absent
Skin color is pale or cyanotic
Skin temp is cool
There is minimal to no edema.
Raynaud’s Syndrome
Vasoconstriction, not a clot. Blood vessels in extremities temporarily narrow in response to cold or stress
Triphasic Color Change
Pallor
Cyanosis
Rubor (red) when blood returns
Linked to autoimmune disorder, more common in women. Symptoms start before the age of 30. Genetic.
People often have more than 1 autoimmune with Raynaud’s such as lupus or Rheumatoid arthritis
Risk Factors: Hyperlipidemia, tobacco smoking, diabetes, hypertension, aging
Clinical manifestation more severe and prolonged in Raynaud’s disease
Clinical Features
Primarily affects fingers but can affect toes, thumbs, nipples, nose, and earlobes.
Episodes precipitated by cold exposure and emotional stress.
Episodes accompanied by pain with or without numbness
Pulses present
Necrosis suggestive of secondary cause if it goes on for a long time.
Thromboangitis Obliterans (Buerger Disease)
More severe and serious than Raynaud’s disease because you can lose extremities.
Rare disease where blood vessel so hands and feet get inflamed, swollen, and blocked
Course in unknown but it is more common in young men who are of middle eastern or Asian descent who are heavy tobacco users.
Inflammatory disease of peripheral arteries accompanies by thrombi inflammation and vasospasms, leads to gangrene and amputation
S/S:
Enlarged, red, tender cordlike veins
Pain or tenderness, numbness and tingling in limbs
Discoloration
Usually, two or more limbs affected
Pain may increase with activity and decrease with rest
Symptoms may worsen with exposure to cold or emotional stress
Pulse may be decreased or absent in affected extremity
Leads to Critical Limb Ischemia, skin ulcers, and gangrene
Aneurysms
Malformation of artery. Localized abnormal weakness of a blood vessel, usually an artery. Due to congenital defect or weakness in the wall of the vessel
Can occur in any blood vessel in the body
Some people are born with a weakness in the blood vessels of the brain, which lead to cerebral aneurysms which can rupture when stressed.
Symptoms of Brain Aneurysms: Headache, weakness, vision changes, eye pain, numbness or tingling on head or face
Saccular: Characterized by a localized, balloon-like bulge in the wall of an artery. This type of aneurysm typically has a narrow base and bulges out from one side of the vessel wall, resembling a sac. Saccular aneurysms can occur in various locations in the body but are commonly found in the brain and are at risk of rupturing, which can lead to severe complications such as bleeding or stroke. They often arise due to weaknesses in the arterial wall, which can be congenital or acquired.
Fusiform: Characterized by a spindle-shaped, symmetrical dilation of an artery. Unlike saccular aneurysms, which have a localized bulge, fusiform aneurysms affect a larger segment of the artery's circumference, causing the vessel to widen uniformly. They can develop in various arteries throughout the body and often occur due to atherosclerosis or other degenerative vascular conditions. Fusiform aneurysms are also at risk of rupture and can lead to severe complications depending on their location and size.
Dissecting: Serious condition in which there is a tear in the wall of an artery. This tear allows blood to flow between the layers of the artery wall, separating them and causing a split (dissection). It can occur in various arteries but is most commonly associated with the aorta. Dissecting aneurysms can lead to severe complications, including rupture of the artery, which can be life-threatening. Symptoms may include sudden severe chest or back pain that may be described as a tearing sensation, as well as possible loss of consciousness or other neurological symptoms if blood flow to the brain is affected.
Aortic Dissection: Life threatening emergency, symptoms vary depending on location and severity of tear. Usually described as sudden severe chest or upper back pain that feels like tearing or ripping sensation that spreads to neck or down back. Includes sudden severe stomach pain, SOA. nausea and vomiting, weakness or numbness on one side of body, difficulty speaking, vision loss, leg pain, BP discrepancies. Look similar to MI or stroke.
Aortic Aneurysm: Aorta is particularly susceptible to aneurysm formation and can occur anywhere along the aorta such as the arch, the thoracis area, or down in the abdomen.
Aortic Disease Risk Factors: Smoking, gender (more common in men), age over 65, long standing, hypertension, hyperlipidemia, COPD, family history, and trauma
S/S: Chest and back pain that feels like tearing radiating from front to back, SOA, dysphagia, abdominal discomfort, sense of fullness, wide aortic pulsation palpable in abdomen, tachycardia, BP discrepancies where the BP is different in each arm.
Most serious complication of an aortic aneurysm is the rupture of the aorta
Heart
Circulation of blood through the heart:
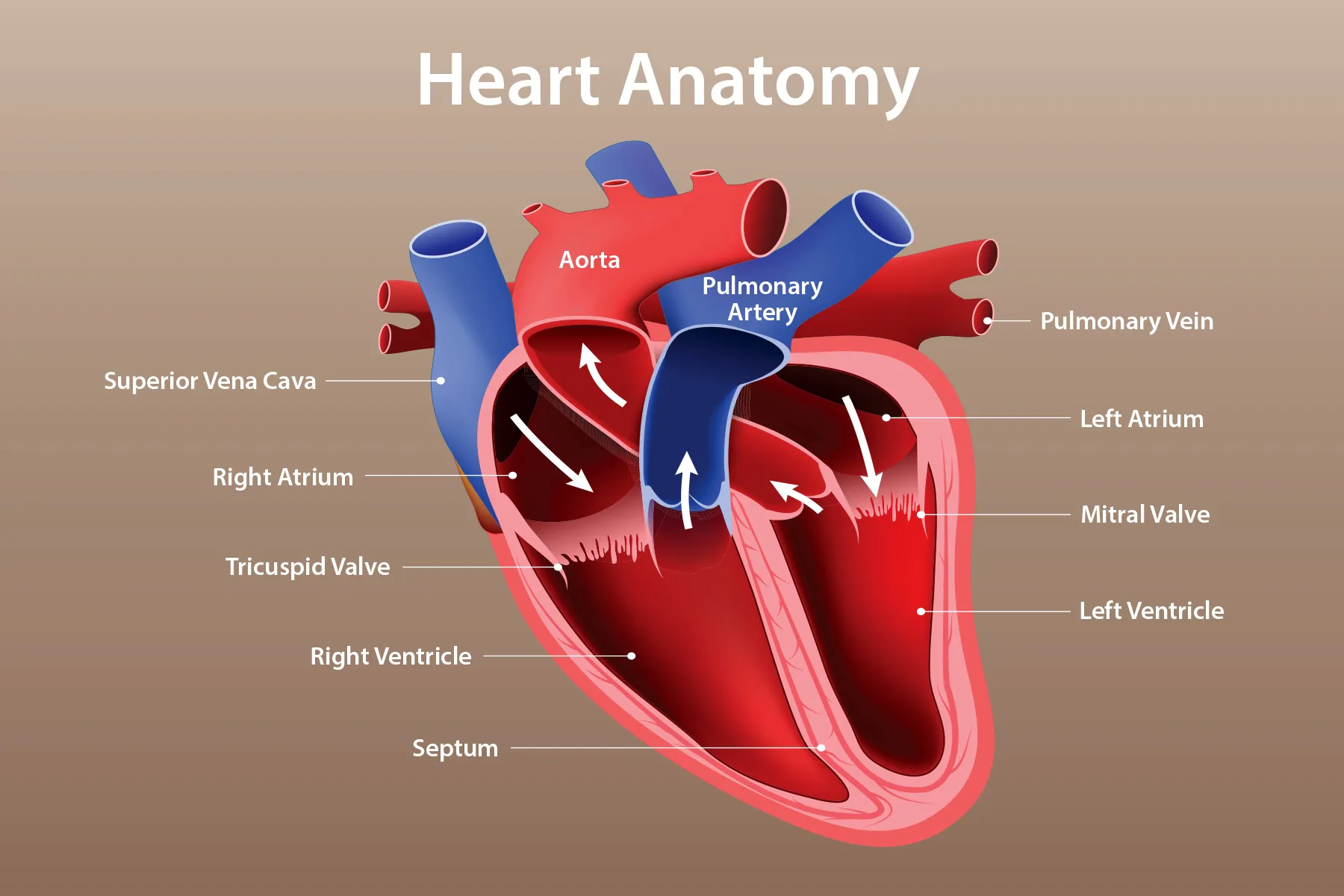
Deoxygenated blood:
Enters superior or inferior vena cava
Right atrium
Tricuspid valve
Right ventricle
Pulmonary valve
Pulmonary artery
Lungs
Oxygenated blood:
Pulmonary veins
Left atrium
Mitral valve
Left ventricle
Aortic Valve
Aorta
Body
Long QT Syndrome: less likely to have a next beat and flatline.
Atrial Fibrillation: Not regular rhythm, there is no pattern. Annoying but not usually immediately deadly. Much more likely to have a stroke.
Ventricular Fabulation: Deadly. Chaotic rhythm and rate.
Coronary Artery Disease (CAD): Pathogens similar to peripheral artery disease. Something builds up and blocks blood vessels that provide O2 and nutrients to cardiac muscle, resulting in damage to heart. Caused by fatty plaques or embolus that becomes thrombus in a coronary artery.
Risk factors: Hypertension, hyperlipidemia, obesity, smoking, gender, race, genetics
Angina: Chest pain from ischemia
Unstable Angina or Acute Coronary Syndrome: Pain does not go away with rest. Tissue is not dead yet, this is reversable.
MI
NSTEMI: Non-ST elevation MI
STEMI: ST elevation MI
Sudden cardiac death
MI
Death of myocardium from a sudden blockage of coronary artery blood flow
Decreased blood blow to cardiac tissue due to some blockage of coronary arteries.
Most common cause is atherosclerosis
Imbalance between O2 and myocardial demand
Chest pain due to ischemia
Stable: Pain on exertion that goes away at rest. Short amount of pain that goes away after 1-5 minutes. Not a medical emergency but a warning.
Unstable: Pain doesn’t go away at rest. Stays for longer than 15-20 minutes. Medical emergency.
Silent Ischemia
In Men: Chest pain radiating down left arm and into jaw
Women: Low back pain, fatigue, nausea
Other Symptoms with men and women: Dyspnea, diaphoresis, nausea
Complications: Arrythmias, Congestive heart failure, Cardiogenic shock, and mechanical complications
Acute Pericarditis
Inflammation on pericardium which is the lining around the heart
Etiology: Infection, trauma, uremia, mediastinal radiation, MI (Dressler’s Syndrome), post-surgical
Complication: Pericardial effusion which is lots of fluid build up
S/S: Sharp, piercing chest pain over the center or left side of chest, which is generally more intense with inhalation, orthopnea, heart palpitation, low grade fever, overall weakness, cough, pericardial friction rub, sharp pain with deep inhale.
Pericardial Effusion
Accumulation of fluid in pericardial cavity
Muffled heart sounds due to fluid
Pulses paradoxes (decreased pulse pressure when breathing in)
Slow capillary refill time
Causes: Inflammation following heart surgery or MI, autoimmune disease like Lupus, cancer metastasis, cancer treatments like chemo or radiation, uremia from kidney failure, hypothyroidism, infection, and chest trauma.
Constructive Pericarditis
Pericardium gets fibrous and thick that puts pressure on heart. Thickened by over 5 mm
Symptoms: Dyspnea on exertion, chest discomfort, fatigue, abdominal symptoms
Signs: JVD, Kussmaul sign, pleural effusion, pericardial knock
Complication:
Cardiac tamponade: Serious medical condition in which blood or fluid fill space between the sac that encases the heart and heart muscle. S/S include muffled heart sounds, JVD, and hypotension
Myocarditis: Inflammation on myocardium, the heart muscle
Usually viral and hard to treat (Flu, Coxsackie, cytomegalovirus, adenovirus, Hep C, herpes, HIV) Can be bacterial
S/S: Flulike symptoms, dyspnea, dysthymias, tachycardia, heart murmurs, cardiac enlargement, chest pain, pale and cool extremities, syncope, decreased urine output, joint pain and swelling
Cardiomyopathy: Progressive disease of the heart muscle that causes it to become enlarged and thick or rigid making it harder to pump blood.
Etiology: genetic, due to high BP, due to diabetes
Treat with med or implanted devices.
Dilated: Big and enlarged
hypertrophic: Thick septum
restrictive: Rigid
S/S: SOA, poor exercise tolerance, fatigue, palpations, pulmonary congestion, biventricular failure
Risks: Genetic, risk increases with age, African American men, chemo, alcoholism, pregnancy, infection, diabetes,
Vocab
D-Dimer: lab to measure clotting factors
Anticoagulants: Prevent more clots
Thrombolytics: Dissolve clots
Preload: Volume of blood in ventricle at end of diastole. Increases with Hypervolemia, regurgitation of cardiac valve, and heart failure
Afterload: Resistance left ventricle must overcome to circulate blood. Increases with hypertension and vasoconstriction.
EKG: Cardiac Electrical Activity. P wave is atria depolarization. QRS complex is ventricular depolarization. T wave is ventricular repolarization
Normal: P wave corresponds to depolarization of SA node and atria. QRS complex corresponds to ventricular depolarization. T wave corresponds to ventricular repolarization. Atrial repolarization is masked by the larger QRS complex.
Dysrhythmias: Abnormal electrical activity.