3D Printing a Human Being: Principles, Clinical Applications, and Bioprinting
Introduction to 3D Printing in Biomedicine
Overview: The session is presented by Professor Kawal Rhode from the School of Biomedical Engineering & Imaging Sciences at King's College London, in collaboration with Guy's and St Thomas' NHS Foundation Trust and King's College Hospital NHS Foundation Trust.
Central Theme: Transitioning from "Sci-Fi to Sci-Fact" using 3D printing technology to recreate human anatomy and biological structures.
Learning Objectives:
Demonstrate knowledge and understanding of basic principles of 3D printing technology.
Understand methods to create 3D computer models.
Explore examples of applications for 3D printed organ models.
Comprehend the basic principles of bioprinting.
Cultural Context: The concept of "replicating" humans or organs has roots in science fiction, such as the Star Trek Replicator (Gene Roddenberry, 1987) and Westworld Synthetics (Michael Crichton, 1973 original and 2016 series).
Fundamentals of 3D Printing Technology
Definition: 3D printing is also known as Additive Manufacturing. It involves building a 3D object one layer at a time.
Historical Context: The first 3D printers were invented in the 1980s.
Methodology Comparison:
Additive Manufacturing: Builds objects up layer by layer from nothing.
Subtractive Manufacturing: Removes material from a solid block (e.g., milling or carving) to create a shape.
Primary Types of 3D Printing (The technology encompasses more than 10 distinct types):
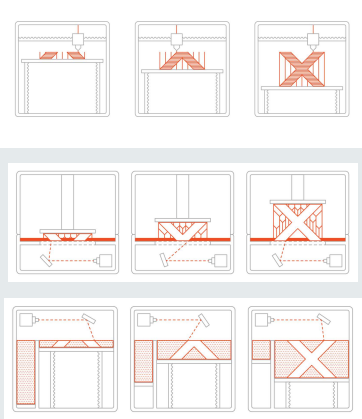
Material Extrusion: Commonly known as Fused Deposition Modeling () or Fused Filament Fabrication (). It follows a Solid-Liquid-Solid process where thermoplastic is melted and extruded through a nozzle.
VAT Polymerisation: Includes Stereolithography () and Digital Light Processing (). It follows a Liquid-Solid process where a liquid resin is cured into a solid using light.
Powder Bed Fusion: Includes Selective Laser Sintering (). It follows a Solid-Liquid-Solid process where a laser fuses powdered material into a solid structure layer by layer.
Volumetric 3D Printing: Representing the most recent development in the field, these printers project light into a rotating volume of material to create the entire object at once rather than layer-by-layer (OpenCAL technology).
Commercial Trends and Specifications
Market Expansion: There has been a rapid decrease in the cost of technology over the last 10 years, making thousands of printers available to consumers.
Entry-Level Pricing: Desktop printers can now be purchased for less than . Examples of notable consumer/prosumer printers include:
Bambu Lab A1 Combo.
Anycubic Photon M3 Max.
Anycubic Super Racer.
Material Variety:
Hard Materials: PLA, ABS, nylon, acrylic, metals, and concrete.
Soft Materials: TPU, silicone, and clay.
Organic Materials: Chocolate, icing, and cellular structures.
Technical Specifications:
Layer Thickness: Approximately .
In-plane Resolution: Approximately .
Speed: Highly variable, ranging from 10 minutes to several days depending on object size and complexity.
Thermal Requirements: For FDM using PLA, the printing temperature typically ranges between 190 < T < 210\,^\circ\text{C}.
The 3D Printing Pipeline
Step 1: Source Data: Acquiring the initial shape through surface scans or medical imaging (CT, MRI, Ultrasound).
Step 2: 3D File Creation: Converting raw data into a 3D computer-aided design () file or a processed medical file via segmentation.
Step 3: SLICER: Converting the 3D computer model into a series of thin layers. This produces a GCODE file, which contains the numerical instructions for the printer.
Step 4: 3D Printer: The hardware executes the GCODE instructions to produce the physical 3D print.
3D Printing at King’s Health Partners (KHP)
Dedicated Facilities: KHP houses dedicated 3D printing centers to support clinical applications, research, and education.
Educational Integration: 3D printing is taught to engineering and healthcare students, specifically in the Year 2 Synthetic Anatomy module.
Medical Physics Department: Operates a 3D Printing Centre that handles both clinical service delivery and research production.
Clinical Services - Cardiac Models: Used for surgical planning in patients with complex Congenital Heart Disease ().
Case Study (Valverde et al. 2017): A study across 10 international centers involving 40 complex patients.
Results: In 19 out of 40 cases, the 3D model helped refine the surgical approach. In 21 out of 40 cases, the models did not alter the planned approach.
Technology: Stratasys Objet500, a multi-material jetting printer.
Anthropomorphic Phantoms and Research
Purpose of Phantoms:
Testing novel medical devices.
Generating synthetic medical images to train AI algorithms.
Simulation for surgical training and rehearsal.
Validating biophysical modeling algorithms.
Strategic Benefits: Reducing dependency on patient data, animal experiments, and cadaver experiments, while simultaneously reducing development costs.
Cardiac Phantoms: Whole-heart models created using soft materials such as Lay-fomm 40 or Tango Plus.
Cost Examples: A model printed on a Flsun Delta FDM printer costs roughly , whereas a high-end print on a Stratasys Objet500 PolyJet can cost (Shu Wang et al. 2020).
Valve Phantoms: Created to mimic specific pathologies such as normal, rheumatic, calcified, and bicuspid valves.
Moulding Process: Involves a four-step process: (a) External Mould, (b) Internal Mould, (c) Silicone Injection, and (d) Final Fabricated Valve.
Imaging Validation: Phantoms are tested using Ultrasound and MR to ensure they mimic real tissue response.
Direct Silicone Printing: Recent advancements allow for direct silicone printing (e.g., Dragonskin 20) using custom printers based on Prusa i3 clones. This offers lower costs, larger build volumes, and reduced manufacturing time compared to traditional moulding.
Implants and Surgical Training
Surgical Training Models: Specialized models for laryngology, such as training instruments installed on ANMISI 1.2.4 (not for human use). These models won the Royal Society of Medicine Innovation Prize in 2025.
Bone Replacement Implants: Specifically for lung cancer surgery where bone involvement occurs.
Workflow: CT scan → 3D Model → Low-cost PLA print → Low-cost silicone mould → Custom PMMA (Polymethyl methacrylate) implant.
Clinical Impact: Over 15 patients implanted with no complications, showing better respiratory mechanics and improved aesthetics (Pontiki et al. 2021).
Economic Advantage: Significantly lower cost compared to traditional titanium implants.
3D Bioprinting
Definition: The use of living components (cells and biological matrices) to print tissues and organs.
Methods:
Scaffold-based: Printing a 3D scaffold (often a hydrogel) and
Bioink Printing: Printing a mixture of cells and scaffold material simultaneously. or Directly printing cells in high density.
pre processing: imaging → 3d modeling and slicing
processing: bio-ink preparation → 3d bioprinter
post-processing: bioreactor for tissue maturation → matured tissue/organ
application: invitro models or transplanted into patients
useul for research, testing frugs/devices and implants
Bioprinting Examples:
Skin: Layers mimicking the Epidermis, DEJ (Dermal-Epidermal Junction), and Dermis using bioinks with fibroblasts and keratinocytes (Pourchet et al. 2016).
Heart Muscle: Creating a functional patch of myocardium using bioink with myocytes (Gaetani et al. 2015).
Other structures: Liver, heart valves, blood vessels, and trachea have been successfully bioprinted.
Conclusion: While the printing of tissues and organs faces significant challenges, developments are rapid. Ethical considerations remain a critical part of the ongoing progress in 3D bioprinting (e.g., Chimera Bioprinter from Ourobionics).