The Process of Hemostasis
HEMOSTASIS
Hemostasis is a complex and essential biological process that prevents and stops bleeding, involving multiple steps and various clotting factors. It maintains the balance between clot formation and breakdown, ensuring that blood coagulation occurs only when necessary to prevent excessive blood loss while allowing for the normal flow of blood in the circulatory system.
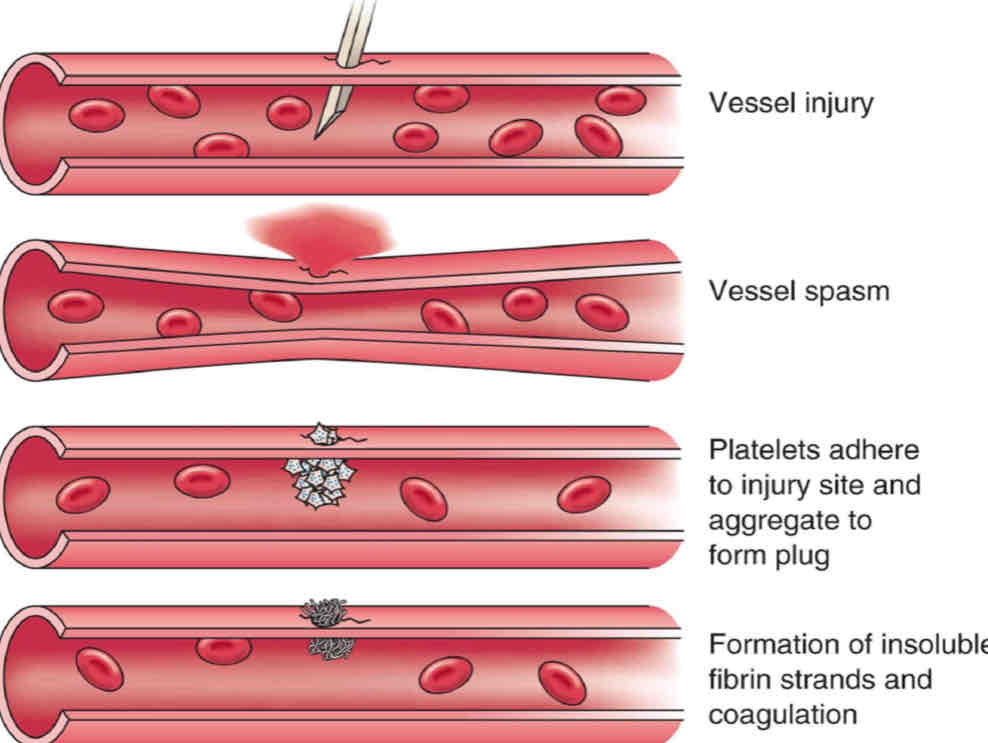
Steps in Hemostasis (VPCCF):
1. Vascular Phase (30 mins)
Cutting or damaging blood vessels initiates the vascular phase, leading to a vascular spasm that produces vasoconstriction. This response aims to slow down or even completely stop blood flow, minimizing blood loss at the injury site. Vasoconstriction is a temporary reaction that helps reduce the amount of blood exiting the wound area.
2. Platelet Phase
In larger blood vessels, platelets begin to adhere to the surfaces of damaged endothelial cells. This adhesion is critical for the following steps:
Platelet Aggregation: Once the platelets adhere to the site, they become activated and aggregate to form a platelet plug.
Role of Platelets: Platelets are small cell fragments that play a key role in hemostasis. They contain granules filled with substances that promote further clotting and healing. The formation of this plug is essential to quickly cover the wound and prevent further bleeding.
Factor III: Also known as thromboplastin, this factor is released by damaged tissues and plays a crucial role in platelet activation and aggregation, signaling other platelets to join the process.
3. Coagulation Phase
The coagulation phase consists of a series of biochemical events that culminate in the transformation of plasma protein fibrinogen into fibrin, which forms a mesh or network that stabilizes the platelet plug, creating a thrombus or a stable clot. Key components include:
Thrombin: An enzyme that converts fibrinogen into fibrin.
Coagulation Cascade: This refers to the sequence of events that lead to thrombin's activation, typically occurring about 30 seconds after the platelet phase. The intricate process involves multiple clotting factors, including Factor IV (calcium ions) and Factor X, which is a common factor between both extrinsic and intrinsic pathways.
Pathways to Thrombus Formation:
There are two primary pathways that lead to thrombus formation:
Extrinsic Pathway: Initiated by factors external to blood, this pathway is very rapid and typically leads to smaller clots.
Intrinsic Pathway: This pathway is triggered when blood contacts exposed collagen in the damaged vessel wall, resulting in a slower, more robust response that leads to larger clots.
4. Clot Formation
After 2 to 3 days post-injury, the clot undergoes contraction, a process facilitated by contractile proteins within the platelets. These proteins pull the edges of the wound together, further reducing blood loss, and assist in tissue repair. The clot provides a temporary barrier that protects the underlying tissues while they heal.
5. Fibrinolysis
Fibrinolysis is the process of clot dissolution, crucial for restoring normal circulation after the tissue has healed. The powerful proteolytic enzyme Plasmin breaks down fibrin into soluble fragments, effectively removing the clot. This step must proceed efficiently to prevent complications such as thrombosis, where excessive clotting occurs, obstructing blood flow.
Thrombin's Role: Thrombin not only aids in converting fibrinogen to fibrin but also influences the fibrinolytic system, regulating the balance of clot formation and breakdown.
Conversion Process: Plasminogen, the inactive precursor in the clot, is converted into plasmin, which then acts on the fibrin mesh, completing the hemostatic process.
In summary, hemostasis is a finely-tuned process that relies on the timely interaction of vascular responses, platelet activity, coagulation cascades, and eventual clot breakdown to maintain blood integrity and prevent hemorrhage following vascular injury.