Oxygenation, Labs & Diagnostics
1. Overview of Oxygenation & Cardiopulmonary System
Oxygenation is the process of delivering oxygen to cells, tissues, and organs.
Four systems assist with oxygenation:
Musculoskeletal (MS) and Neurological (Neuro): Regulate air movement.
Pulmonary (Respiratory): Oxygenates blood.
Cardiovascular (CV): Circulates oxygenated blood.
2. Cardiovascular System Functions
Circulation: Blood flow through the body.
Perfusion: Blood flow to capillary beds to nourish tissues.
Heart Structure: Four chambers (2 atria, 2 ventricles) with valves.
Cardiac Cycle: Atria contract, followed by ventricles, regulated by electrical impulses.
Cardiac Output: Heart rate (beats/min) x Stroke volume (L/beat).
Blood Vessels: Arteries → Arterioles → Capillaries (exchange gases) → Veins (return to heart).
Respiration: Exchange of O₂ and CO₂.
3. Respiratory System Functions
Ventilation: Air movement; includes:
Inspiration: Diaphragm contracts, air flows in.
Expiration: Diaphragm relaxes, air flows out.
Respiration: Gas exchange at alveoli level.
Controlled by neural and chemical signals.
4. Common Cardiovascular Disorders
Coronary Artery Disease (CAD): Narrowed coronary arteries lead to reduced blood flow.
Arrhythmias: Irregular heartbeats affecting oxygen delivery.
Congestive Heart Failure (CHF): Heart can’t pump effectively; leads to fluid buildup.
Peripheral Vascular Disease (PVD): Reduced blood flow to limbs.
5. Respiratory Disorders
Chronic Obstructive Pulmonary Disease (COPD): Includes emphysema (loss of elasticity) and chronic bronchitis (inflammation).
Asthma: Airway constriction due to irritants.
Pneumonia: Lung infection with symptoms like fever and difficulty breathing.
Atelectasis: Collapse/blockage of alveoli. Risk factors include anesthesia and bed rest.
6. Hematologic Factors Affecting Oxygenation
Anemias: Lowered oxygen-carrying capacity of blood, affecting overall oxygenation.
7. Assessment Techniques
Health History: Chief complaints, focused questions on symptoms.
Physical Exam:
Vital Signs: BP, respiratory rate, pulses.
Inspection & Palpation: Chest shape, muscle usage, heart vibrations.
Auscultation: Lung sounds for abnormalities; heart sounds.
Vascular Assessment: Peripheral pulses, skin color/texture, capillary refill, edema.
8. Laboratory & Diagnostic Tests
Pulmonary Function Tests (PFTs): Measure air movement; tracks disease progress.
Arterial Blood Gases (ABGs): Assess oxygen and CO₂ levels.
Basic Metabolic Panel: Detects electrolyte imbalances which can cause arrhythmia.
9. Management of Impaired Gas Exchange
Goals:
Stabilize respiratory rate (16-24 breaths/min).
Increase SpO₂ above 85%.
Improve lung sounds and reduce dyspnea.
10. Promotion of Oxygenation
Airway Management: Deep breathing, coughing, incentive spirometry.
Oxygen Therapy: Monitor effectiveness, safety measures, document patient tolerance.
Suctioning: Clear airways, collect sputum.
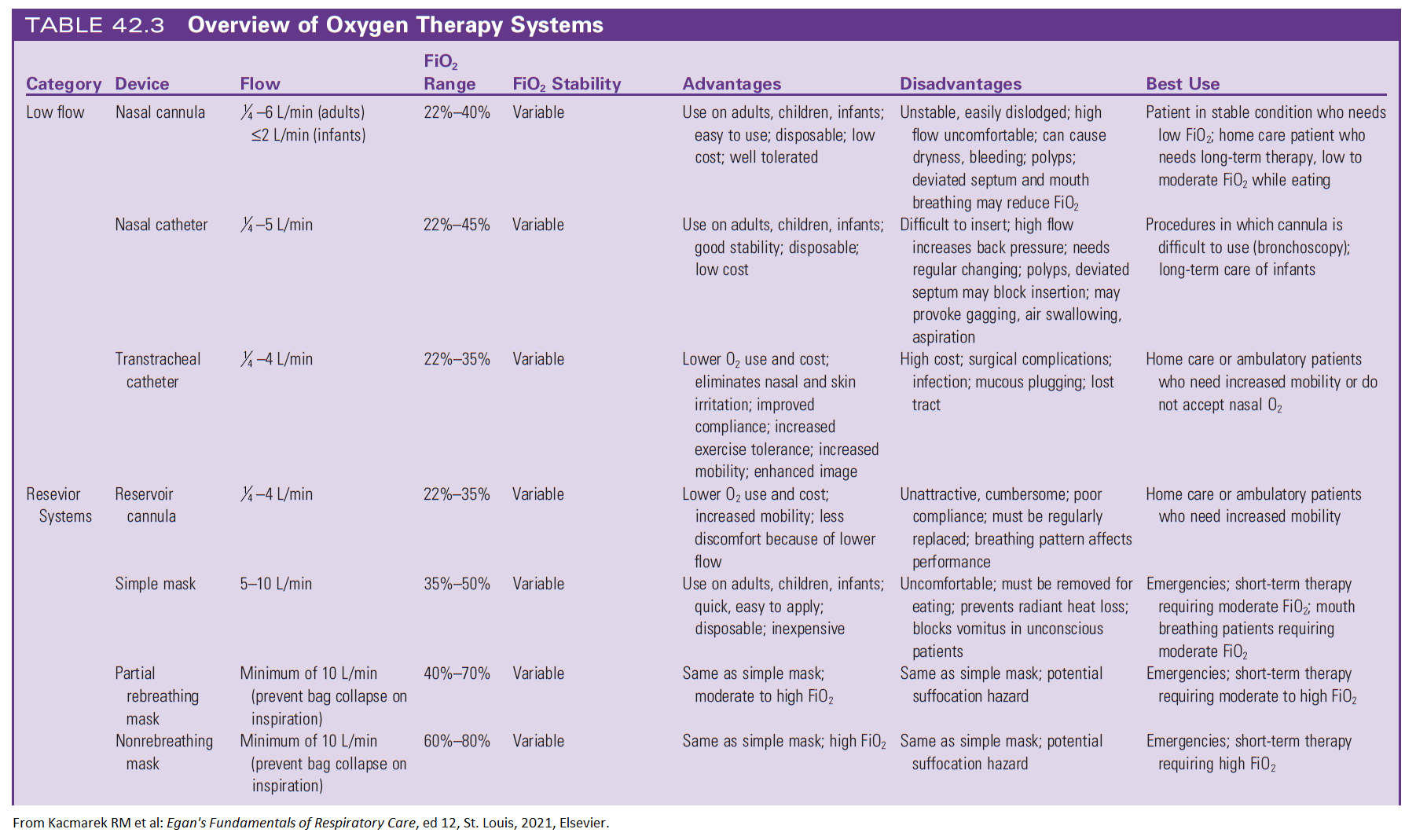
Oxygen Delivery Systems:
Nasal Cannula: Low flow.
Masks (Simple, Rebreather, Venturi): Higher flow, specific O₂ delivery.
CPAP & BiPAP: For sleep apnea, pneumonia, COPD.

11. Medication Administration
Bronchodilators: Open airways.
Corticosteroids: Reduce inflammation.
Mucolytics: Thin secretions.
12. Additional Therapeutic Measures
Hydration: 2800 mL/day recommended, avoid caffeine.
Chest Physiotherapy: Postural drainage, deep breathing.
Pharyngeal Airways: Prevent airway obstruction.
13. Patient Education & Positioning
Educate on lifestyle changes: diet, exercise, and smoking cessation.
Importance of vaccinations (influenza, pneumonia).
Proper positioning for optimal lung expansion.
14. Nursing Roles in Diagnosis and Care
Diagnostic Communication: Relay test results and patient status to the healthcare team.
Patient Monitoring: Continuous assessment and adaptation of care plans based on response to treatment.
15. Blood Cell Types and Functions
WBCs (Leukocytes): These cells are essential to the body’s immune and inflammatory responses, defending against infections and foreign substances.
RBCs (Erythrocytes): These contain hemoglobin, a crucial protein for oxygen transport to tissues and carbon dioxide removal. RBCs contribute to maintaining acid-base balance and are formed in the bone marrow.
Platelets (Thrombocytes): Key players in blood clotting; they aggregate at the site of a vessel rupture to form a plug, stopping bleeding. They are also formed in the bone marrow.
Plasma: The fluid part of blood, primarily composed of water, carries substances necessary for homeostasis:
Electrolytes: Help maintain body functions.
Hormones: Regulate physiological processes.
Nutrients: Transport essential molecules for cell function.
Plasma Proteins:
Albumin: Maintains fluid balance by regulating osmotic pressure.
Fibrinogen: Important for blood clot formation.
Globulins: Involved in immune functions.
16. Pre-procedure Essentials
Standard Precautions: Follow infection control practices to ensure safety.
Patient Identification and Allergies: Confirm identity and check for allergies, especially to medications and latex.
Informed Consent: Ensure that the patient has given consent after understanding the procedure’s purpose and risks.
Medication Review: Note any medications the patient is taking that could affect the procedure.
Venipuncture: Familiarize yourself with the proper technique, selecting appropriate sites for blood draw.
Labeling: Ensure that specimens and containers are accurately labeled to prevent errors.
Documentation: Record all relevant information about the procedure and patient response.
17. Blood Tests Overview
Venous Blood Sample: Frequently used to measure various blood components and assess overall health.
Arterial Blood Sample: Used for arterial blood gas (ABG) analysis to measure oxygen and carbon dioxide levels, pH, and bicarbonate.
Capillary Blood Sample: Typically used for quick tests like fingerstick glucose, especially in diabetic patients.
18. Complete Blood Count (CBC)
CBC: A common test that measures different components of the blood, giving insights into general health and detecting conditions like anemia or infection.
RBC Count: Indicates oxygen-carrying capacity.
Hemoglobin: The iron-containing protein essential for oxygen transport.
Hematocrit (HCT): Measures the proportion of RBCs in blood, providing information about fluid balance and anemia.
WBC Count and Differential: Evaluates immune function, identifying specific types of WBCs (like neutrophils and lymphocytes) which help diagnose infections and immune disorders.
RBC Indices (MCV, MCH, MCHC): Provide details about RBC size and hemoglobin content, which can indicate types of anemia.
19. Coagulation Studies
Platelets: Assess clotting ability and diagnose conditions like thrombocytopenia, where there is a low platelet count.
Prothrombin Time (PT): Measures how long it takes blood to clot, commonly used to monitor warfarin therapy effectiveness.
International Normalized Ratio (INR): Standardized PT measurement, important for patients on anticoagulants like warfarin.
Partial Thromboplastin Time (PTT): Assesses the intrinsic pathway of coagulation, useful for monitoring heparin therapy and detecting bleeding disorders.
20. Basic Metabolic Panel (BMP)
Electrolytes (Sodium, Potassium, Chloride, Bicarbonate): Critical for cellular function, fluid balance, and pH regulation.
Carbon Dioxide (CO2): Indicates respiratory and metabolic function.
Glucose: An essential energy source, with blood levels often monitored in diabetes management.
Renal Function Tests (BUN, Creatinine): Evaluate kidney function by measuring waste products filtered by the kidneys.
Hemoglobin A1c: Reflects average blood glucose over 2-3 months. An A1c > 6.5% suggests diabetes, while levels above 7% indicate poor glucose control.
21. Capillary Glucose Testing
Purpose: Monitors blood glucose, especially in diabetes, to gauge insulin needs and therapy effectiveness.
Instructions for UAP:
Test timing (before meals, at bedtime) as ordered.
Avoid areas with cuts, bruises, or scars.
Use preferred sites, typically the sides of the fingers.
Adhere to policy for sample collection and handling to ensure accuracy.
22. Renal Function Tests
Blood Urea Nitrogen (BUN): Reflects protein metabolism; elevated levels indicate reduced kidney function.
Serum Creatinine: Waste from muscle metabolism, indicative of kidney filtering capacity.
23. Lipoprotein Profile
Purpose: Diagnoses hyperlipidemia and cardiovascular disease risk.
Cholesterol: Total amount of cholesterol in the blood.
LDL (Low-Density Lipoprotein): “Bad” cholesterol, high levels linked to atherosclerosis.
HDL (High-Density Lipoprotein): “Good” cholesterol, helps remove LDL, reducing heart disease risk.
Triglycerides: Stored fats, used as energy, high levels associated with increased cardiovascular risk.
24. Liver Function Tests
Albumin and Bilirubin: Assess protein production and waste clearance.
Liver Enzymes (ALT, ALP, AST, GGTP): High levels suggest liver cell damage from conditions like hepatitis or cirrhosis.
25. Cardiac Markers
Purpose: Identifies myocardial injury.
Creatine Kinase (CK) and CK-MB: Elevated levels indicate muscle damage, especially in the heart.
Myoglobin: Early marker of muscle damage.
Troponins I and T: Highly specific to cardiac tissue; elevated levels signal heart attack.
26. Urinalysis and Stool Analysis
Urinalysis: Routine test to detect UTIs, kidney disorders, and other conditions.
Stool Analysis: Assesses GI function, detects blood, fat, or parasites.
Cultures: Identify infectious agents in various fluids; guides antibiotic therapy by determining sensitivity.
27. Sputum Culture
Purpose: Diagnoses respiratory infections like pneumonia or tuberculosis.
Proper collection is critical to avoid contamination with saliva.
Specialized containers may be needed for TB or other specific pathogens.
28. Radiography and Contrast Studies
X-rays: Non-contrast images for bones and soft tissues; mammograms for breast cancer screening.
Contrast Studies: Used in IVP, Upper GI Series, and Barium Enema for enhanced detail; assess for allergies to contrast media (e.g., iodine).
Nurse’s Role: Monitor for allergic reactions, ensure adequate hydration, and promote barium elimination post-procedure.
29. MRI and ECG
MRI: Used for detailed imaging, particularly for brain and joint conditions; involves no radiation but may be contraindicated in patients with metal implants.
Claustrophobia can be an issue; sedation may be required.
EKG (ECG): Measures electrical activity of the heart, valuable in diagnosing arrhythmias and other cardiac issues.
30. Endoscopy and Ultrasound
Endoscopy: Directly visualizes organs (e.g., for biopsies); requires informed consent.
Ultrasound: Non-invasive imaging for soft tissues and fetal monitoring; utilizes sound waves to create real-time images.
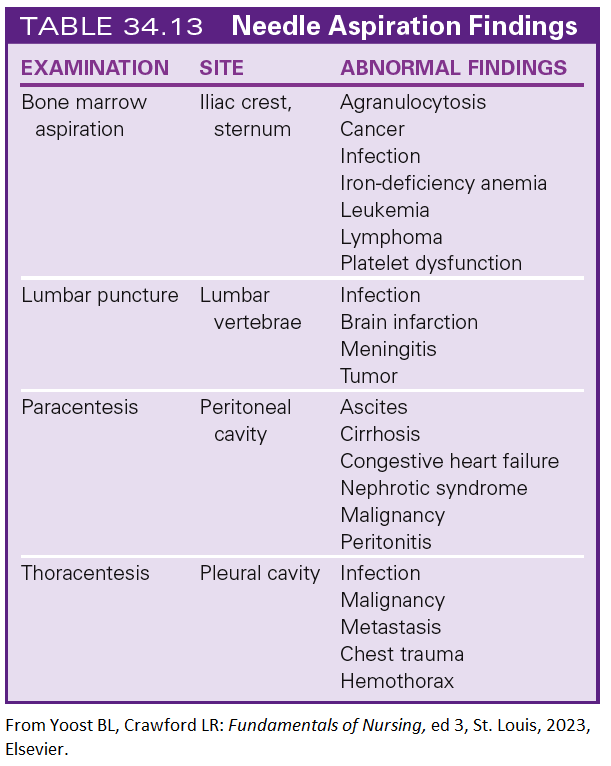
31. Needle Aspirations
Purpose: Collects fluid or tissue samples with minimal invasiveness.
Paracentesis: Removes fluid from the abdomen.
Thoracentesis: Removes fluid from the pleural space.
Biopsy: Diagnoses cancer by sampling cells from a tumor or mass.