THE CIRCULATORY SYSTEM
THE CIRCULATORY SYSTEM
FUNCTION OF THE CIRCULATORY SYSTEM
The circulatory system's primary function is to deliver blood to tissues and facilitate the exchange of blood gases, nutrients, and waste products. This system ensures that tissues receive adequate oxygen and nutrients while removing carbon dioxide and metabolic wastes.
COMPONENTS OF THE CIRCULATORY SYSTEM
The circulatory system consists of two main components:
Venous System
- Responsible for returning deoxygenated blood back to the heart.Arterial System
- Distributes oxygenated blood from the heart to the body's tissues.
STRUCTURE OF THE ARTERIAL AND VENOUS SYSTEMS
The circulatory system is composed of various types of blood vessels, organized into the arterial and venous systems with distinct structures:
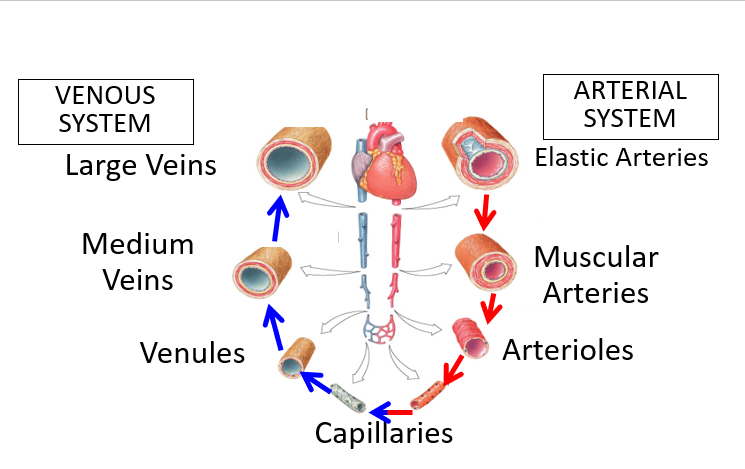
ARTERIAL SYSTEM
Elastic Arteries
- Also known as conducting arteries.
- Examples include the aorta and pulmonary arteries.
- Function: Conduct blood away from the heart; must withstand pressure changes.
- Structure: Thick wall with a substantial layer of elastic tissue in the tunica media, allowing for expansion with the heartbeat.
Muscular Arteries
- Also known as distribution arteries.
- Function: Carry blood to specific areas of the body requiring increased flow.
- Structure: Thick tunica media predominantly composed of smooth muscle enabling vasoconstriction and vasodilation.Arterioles
- Also known as resistance arteries.
- Function: Regulate blood flow and pressure by contracting or relaxing, increasing or decreasing resistance to blood flow.
- Tunica media consists mainly of smooth muscle tissue.
Capillaries
- Structure: Composed of a single layer of endothelial cells surrounded by a thin basement membrane.
- Average Diameter: 8 µm, which is comparable to a red blood cell's diameter of 7.8 µm.
- Function: Site of two-way exchange of materials (gases, nutrients, wastes) between blood and tissues.
Types of Capillaries
Continuous Capillaries
- Characterized by endothelial cells that have no gaps (found in the brain).Fenestrated Capillaries
- Contain pores between endothelial cells (found in the small intestine).Sinusoids
- Feature large openings and no basement membrane, allowing new blood cells to enter circulation (found in the bone marrow).
VENOUS SYSTEM
Venules
- Postcapillary Venules: Small venules that are similar to capillaries and allow some material exchange.
- Muscular Venules: Larger venules with thicker walls; no exchange takes place here.Veins
- Structure is similar to arteries but thinner walls and larger lumens, reflecting lower pressure.
- Larger veins contain valves to prevent backflow of blood. Venous return is aided by these valves and skeletal muscle contractions.
BLOOD FLOW AND PRESSURE
Blood flow is directly proportional to blood pressure (BP):

High BP results in high blood flow, while low BP leads to low blood flow.
Blood Pressure in Different Vessels
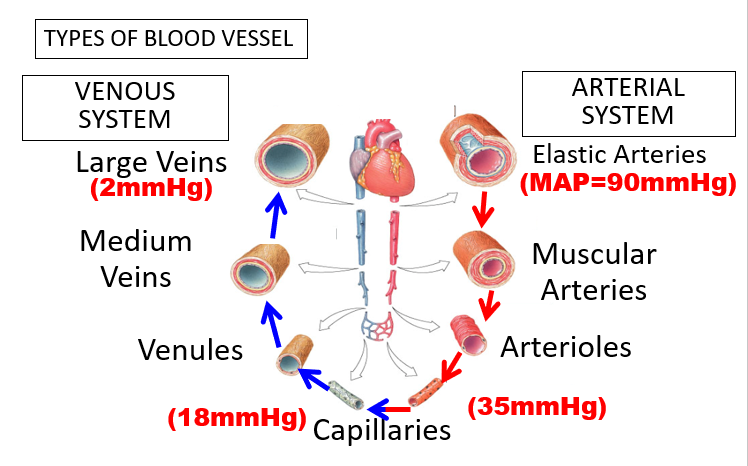
Blood pressure varies significantly in different types of blood vessels:
- Elastic Arteries & Muscular Arteries: Higher pressures (e.g., 120 mm Hg to 60 mm Hg)
- Veins & Venules: Much lower pressures (e.g., approaching 0 mm Hg near the vena cavae)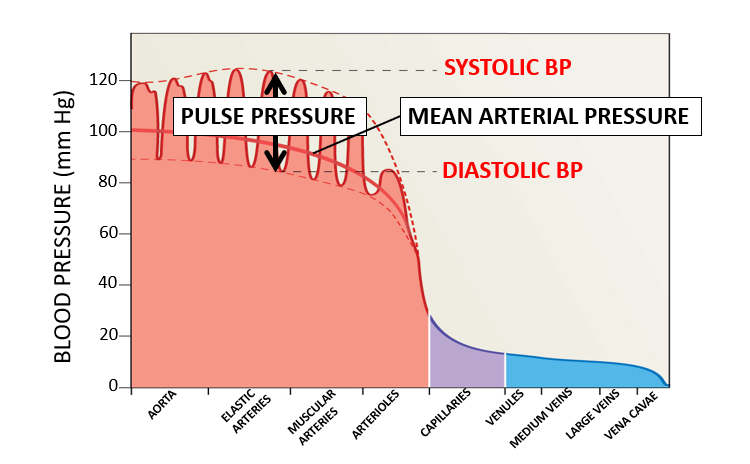
Blood Pressure Components
Systolic Pressure: The pressure in the arteries when the heart ventricles contract.
Diastolic Pressure: The pressure in the arteries when the heart ventricles relax.
Pulse Pressure: Calculated as systolic pressure minus diastolic pressure.
Mean Arterial Pressure (MAP): Calculated using the formula: diastolic pressure + (pulse pressure/3)
PERIPHERAL RESISTANCE
Peripheral resistance refers to the opposition faced by blood flow in the circulatory system:

If peripheral resistance (PR) is high, blood flow (F) is low.
Factors Affecting Peripheral Resistance
Width of the Lumen: Smaller lumen results in higher resistance.
Blood Vessel Length: Longer vessels contribute to higher resistance.
Blood Viscosity: Higher viscosity results in greater resistance.
Smoothness of Endothelium: Irregularities lead to turbulence and increased resistance.
ATHEROSCLEROSIS
Atherosclerosis is characterized by the development of atheroma, a build-up of materials that narrows the lumen of blood vessels, leading to reduced blood flow.
Consequences include:
- Cerebral Circulation: May lead to cerebrovascular accidents (strokes) and neurological symptoms such as paralysis or aphasia.
- Peripheral Circulation: Can result in gangrene.
- Coronary Circulation: Blockage in coronary arteries can result in myocardial infarction (heart attack).
Summary of Key Points:
The circulatory system is essential for transporting blood.
There are different types of blood vessels, each with specific functions in regulating blood flow, pressure, and distribution.
Peripheral resistance plays a crucial role in managing blood flow, influenced by factors such as vessel diameter and length, blood viscosity, and the condition of the endothelial surface.
Atherosclerosis has serious implications for cardiovascular health, leading to potentially life-threatening diseases.