Type 2 Diabetes: Dietary Management
Learning Outcomes
Understand the importance of glycaemic control to reduce the risk of complications in type 2 diabetes:
Dietary approaches involve glycaemic control
Key components include:
Glycaemic index
Carbohydrate content
Meal timings
Understand the role of macronutrients (particularly carbohydrates and fats) on glycaemic control
Nutritional strategies for preventing and managing complications of cardiovascular disease (CVD)
Role of weight management in diabetes prevention
Glucose Targets
Target HbA1c level: 48 mmol/mol
Lifestyle and diet adjustments are key for maintaining this target.
For individuals not achieving control with a single drug, if HbA1c rises to >= 58 mmol/mol:
→ Reinforce advice about diet, lifestyle, and adherence to drug treatment
→ Support aiming for an HbA1c level of 53 mmol/mol
→ Intensify drug treatment as necessary.
Complications of Type 2 Diabetes
Acute Complications
Hypoglycaemia: Blood sugar levels drop too low, generally below 4 mmol/L
Treatment options include: 15-20g glucose
Fast-acting glucose shots (e.g., 60ml of glucose drink)
Five glucose or dextrose tablets
Four jelly babies
Small glass of sugary (non-diet) drink (150-200ml)
Small carton of pure fruit juice (200ml)
Glucose gel tubes like GlucoGel® or RapiloseⓇ Gel
Products like Lift Shots®
→ Recheck BG level after 15 mins, may need to take some slow releasing carbs to maintain BG level.
→ From dietetic perspective, frequent hypos increase calorie intake - first stage is ~ 60kcals, also not good for dental health.
Hyperglycaemia and Hyperosmolar Hyperglycaemia State (HHS)
Dietary Management Recommendations
Guidelines from the NICE (National Institute for Health and Care Excellence) published on Dec 2, 2015, updated June 29, 2022.
Recommended Dietary Approaches:
Healthy, cardioprotective diet
Low glycaemic index/load
Calorie-controlled diet
Low carbohydrate diet
Total diet replacement strategy
Emphasis on no one-size-fits-all approach
Engage with individual dietary needs and preferences.
Eatwell Guide Principles
Utilize the Eatwell Guide to balance healthier and sustainable food consumption, highlighting:
Portion sizes and groups of foods for a balanced diet.
Daily recommendations include:
5 portions of a variety of fruit and vegetables.
Lower fat, salt, and sugars.
Focus on wholegrain options for starchy carbohydrates.
Limit fruit juice to a maximum of 150ml daily.
Portion control in consuming meats, dairy, and processed foods.
Important to use relevant Eatwell guide e.g. South Asian Eatwell guide.
Dietary Principles for Type 2 Diabetes
Follow general healthy eating advice, which includes:
High-fibre, low-glycaemic-index carbohydrate sources (fruits, vegetables, wholegrains, pulses)
Low-fat dairy products
Regular intake of oily fish
Control the intake of saturated and trans fatty acids
Discourage the intake of products specifically marketed for individuals with diabetes.
Carbohydrate and Alcohol Intake Recommendations
Individual recommendations necessary for carbohydrate and alcohol intake.
Specific aim to reduce hypoglycaemia risk for individuals using insulin or an insulin secretagogue.
Glycaemic Index and Glycaemic Load
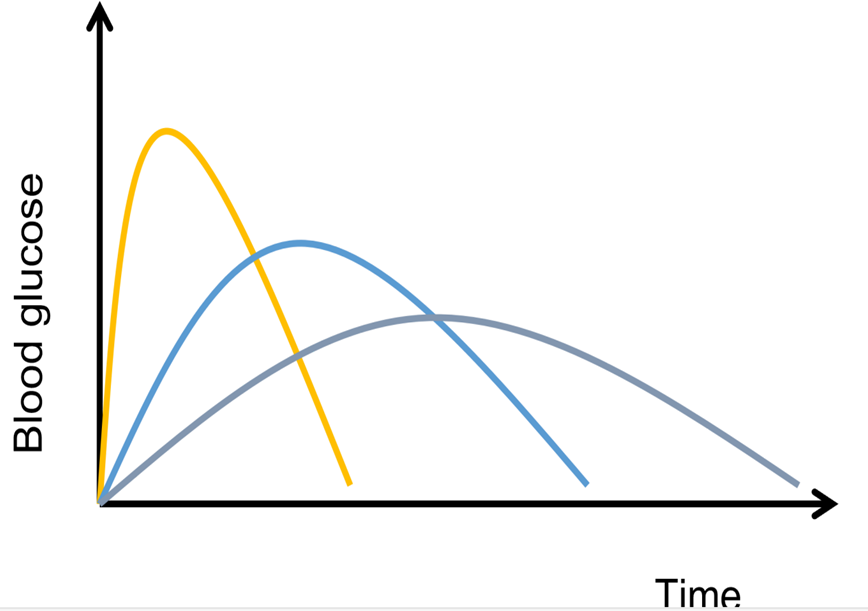
Glycaemic Index (GI): Ranks carbohydrate-containing food according to how much it raises blood glucose (BG) levels compared to a reference food (pure glucose or white bread).
Glycaemic Load (GL): Calculated as GI multiplied by the available carbohydrate (g) in the serving divided by 100.
Important to note that other factors can influence overall glycaemic affect: meal composition - fats and proteins can slow down glucose rise, cooking type/methods, type of starch.
Cardiovascular Disease Management in Diabetes
Target management strategies include from Landmark UKPDS study:
Maintaining blood pressure at or below 140/80 mmHg
If kidney issues present, aim for 130/80 mmHg
Total cholesterol should be < 4 mmol/L
Dietary adjustments: Reduce salt intake (<6g/day), increase intake of oily fish (two portions weekly), improve consumption of wholegrains, fruits, vegetables, and legumes while decreasing red and processed meats, refined carbohydrates, and sugar-sweetened beverages.
Replace saturated fats with unsaturated fats and limit trans fats.
Alcohol intake should be limited to < 14 units/week.

Aim for modest weight loss (at least 5%) in overweight individuals and encourage at least 150 minutes of moderate-intensity physical activity weekly.
Managing weight
Benefit | |
Mortality | >20% fall >30% fall in diabetes related deaths |
Blood Pressure | Fall of 10mmHg systolic Fall of 20mmHg diastolic |
Diabetes | Fall of 50% in fasting glucose |
Lipids | Fall 10% total cholesterol Fall of 15% low density lipoprotein Fall of 30% triglycerides Rise of 8% high density lipoprotein |
For overweight or obese individuals with type 2 diabetes:
For T2D remission, aim for weight loss of approximately 15kg as soon as possible after diagnosis.
To improve glycaemic control and CVD risk, 5% weight loss aim achieved by reducing calorie intake and increasing energy expenditure.
Individualized strategies may include dietary modifications, physical activity, surgical options, and medications.
Low Carbohydrate Diet
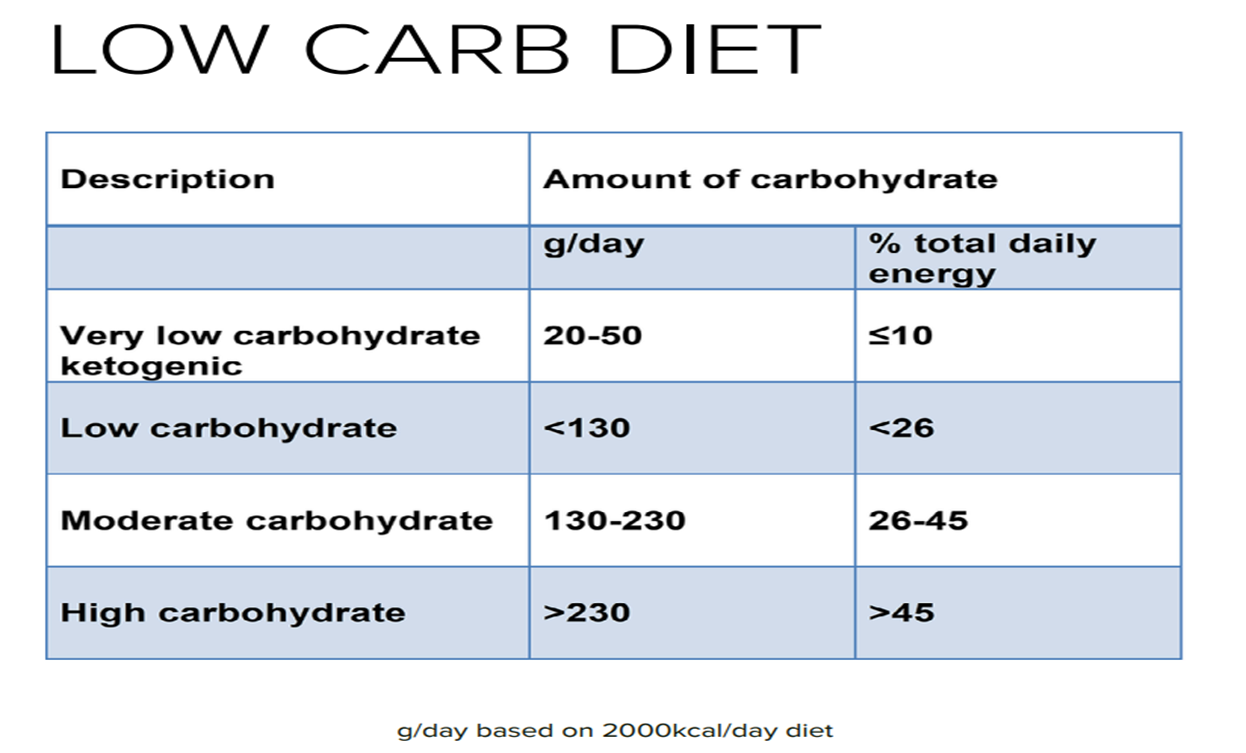
Defined categories of carbohydrate intake in daily diets based on a 2000 kcal/day diet:
Very Low Carbohydrate: 20-50g/day (≤10% of total daily energy)
Ketogenic: Same as very low carbohydrate
Low Carbohydrate: <130g/day (<26%)
Moderate Carbohydrate: 130-230g/day (26-45%)
High Carbohydrate: >230g/day (>45%)
Brain needs glucose to function and needs 100-120g per day - how low carb and very low carb diet intake calculated.
Very Low Carbohydrate and Ketogenic Diets
A very low carbohydrate diet contains 20 to 50 grams of carbohydrates per day (less than 10% of a 2000 kcal/day diet), while a ketogenic diet is formulated to induce ketosis through a very low carbohydrate, high fat diet.
Total Diet Replacement (DIRECT Trial)

Treatment Methodology:
Weight Loss Stage: Total Diet Replacement involving shakes and soups.
Duration: 12 Weeks with weekly or biweekly appointments for targets.
Intake during weight loss is 810+ calories/day.
Reintroduction Stage: Gradual introduction of portion-controlled meals over another 12 weeks.
Maintenance Stage: Focus on maintaining lifestyle changes over 6 months, including up to 18 monthly appointments for ongoing support and potential weight loss medication.
Almost half (46%) of patients were in remission after 1 year.
Outcomes from ReTUNE Study (2022)
The mechanistic changes behind type 2 diabetes remission among patients considered non-obese by BMI standards were the same as those observed in patients who were considered obese.
Results Post 12 Months:
Average BMI reduced to 22.4 kg/m² from 24.8 kg/m².
70% of participants achieved remission from type 2 diabetes with half achieving it after the first weight loss cycle.
Intervention was low calorie diet.
Participants needed to lose an average of 8% body weight for remission.
In 14 out of 20 participants who went into remission, their average HbA1c fell from 53mmon/mol at start to 45mmol/mol. Their bp dropped despite taking less medication to treat this.
Participants liver and pancreas fat levels were higher than expected at start of trial but decreased to normal levels after weight loss.
NHS Type 2 Diabetes Path to Remission Programme
A joint initiative providing total diet replacement treatments for eligible overweight or obese individuals with type 2 diabetes.
Physical Activity Recommendations
Definition of Physical Activity: Movement resulting in energy expenditure; includes planned, repetitive exercise for fitness, divided into:
Aerobic: Endurance-focused.
Anaerobic: Strength and power.
Resistance Training: Specific muscle group exercises against resistance.
Benefits for Adults and Older Adults:
Sleep improvement
Weight management
Stress relief
Reduction of type 2 diabetes risk by 40%
Cardiovascular disease risk reduction by 35%
Falls and depression risk reduction by 30%
Joint and back pain reduction by 25%
Cancer risk (colon and breast) reduction by 20%.
Aim for at least 150 minutes of moderate-intensity activity per week, with recommendations for strength and balance exercises for older adults.
Structured Education in Diabetes Management
The DESMOND program provides structured education to adults with type 2 diabetes at diagnosis, with annual reinforcement and review.
Emphasizes the significance of structured education as part of overall diabetes care.
Evidence-Based Nutrition Guidelines
Nutrition guidelines for diabetes management suggest strategies for prevention and management, established in March 2018 for consistent application across treatment plans.
Conclusion
The importance of glycaemic control in preventing complications, dietary approaches, macronutrient roles, and weight management in diabetes management have been extensively covered and should inform therapeutic strategies.