Traumatic Brain Injury (TBI)
What is TBI?
TBI is a brain injury caused by an external force, such as a blow, jolt, or penetration to the head. It can result from falls, car accidents, sports injuries, or violence. TBI can lead to temporary or permanent cognitive, physical, and emotional impairments.
NICE Guidelines TBI: An alteration in brain function, or other evidence of brain pathology, caused by an external force.
Severities of TBI
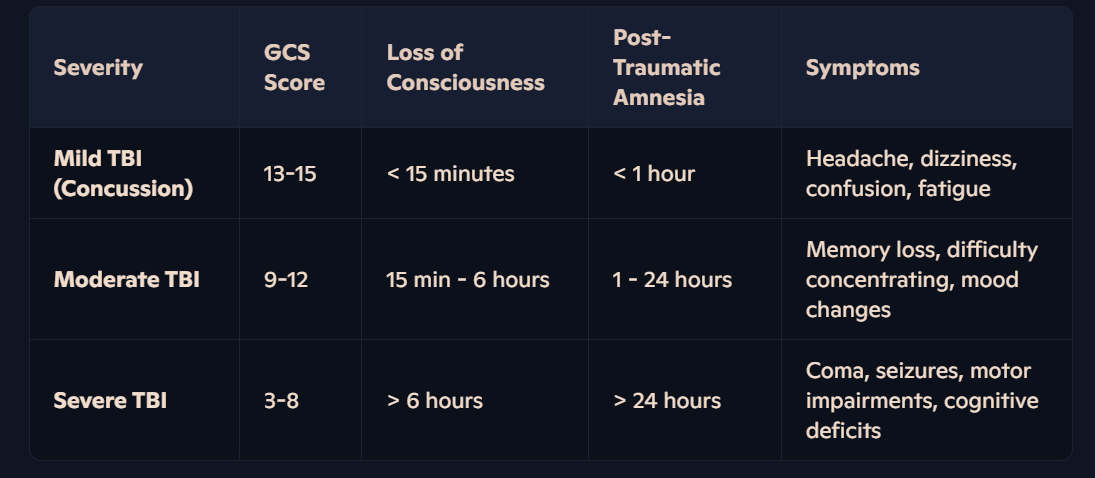
TBI is classified into three main severity levels, often assessed using the Glasgow Coma Scale (GCS). Mild, Moderate and Severe
Post-Traumatic Amnesia
Post-Traumatic Amnesia (PTA) refers to a state of confusion and disorientation following traumatic brain injury (TBI). It can last from a few minutes to several weeks or months, depending on the severity of brain injury. There are different types of post-traumatic amnesia including:
Anterograde amnesia: Inability to remember new information
Retrograde amnesia: Forgetting events that occurred prior to the injury
Dissociative amnesia: Rare type causing memory loss and identity forgetfulness
Glasgow Coma Scale (GCS) (NICE Guidelines)
In people with a head injury, the Glasgow Coma Scale (GCS) is an early assessment of the severity of any associated traumatic brain injury. It is a standardised system used to assess the degree of brain impairment and to identify the seriousness of injury in relation to outcome.
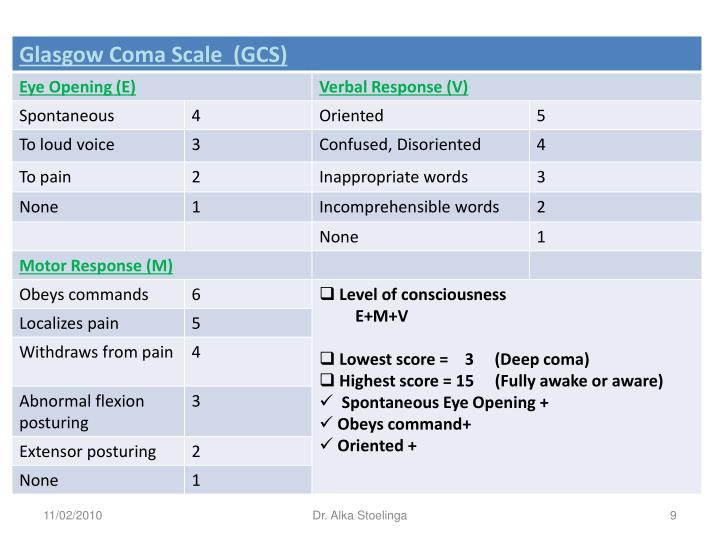
The scale has 3 domains: eye opening, verbal and motor responses. These are all evaluated independently in the scale according to a numerical value that indicates the level of consciousness and degree of dysfunction.
Eye Opening: Scored from 1 to 4 based on the patient’s ability to open their eyes spontaneously or in response to stimuli.
Verbal Response: Scored from 1 to 5 based on the patent’s ability to speak coherently or respond appropriately
Motor Response: Scored from 1 to 6 based on the patient’s ability to follow commands or exhibit purposeful movement
The scores in each element of the GCS are summed to give the overall GCS score, which ranges from 3 (unresponsive in all domains) to 15 (no deficits in responsiveness):
Mild traumatic brain injury is a GCS score of 13 to 15
Moderate traumatic brain injury is a GCS score of 9 to 12
Severe traumatic brain injury is a GCS score of 8 or less
Recent research suggests that TBI classification is evolving, with a multidimensional framework considering clinical, imaging, and biomarker factors to improve diagnosis and treatment.
How TBI Affects Visuospatial Memory
TBI can disrupt brain regions responsible for visuospatial processing, such as the hippocampus, parietal lobe, and occipital cortex. Some common effects include:
Difficulty navigating spaces (getting lost in familiar places)
Impaired object recognition (trouble identifying faces or locations)
Reduced spatial awareness (misjudging distances or bumping into objects)
Problems with visual recall (struggling to remember patterns or layouts)
Studies suggest that moderate-to-severe TBI can lead to long-term visuospatial memory deficits, affecting daily life and independence.
Differences in Visuospatial Memory Deficits Across TBI Severities
The severity of TBI influences the extent of visuospatial memory impairment:
TBI Severity | Effects on Visuospatial Memory |
Mild TBI (Concussion) | Temporary difficulties with spatial navigation and object recognition. Symptoms often improve with recovery. |
Moderate TBI | More persistent visuospatial deficits, including trouble with spatial reasoning and memory recall. |
Severe TBI | Significant and long-lasting impairments in visuospatial memory, affecting independence and daily functioning. |
Research indicates that moderate-to-severe TBI leads to greater deficits in delayed recall compared to immediate memory tasks. Additionally, working memory impairments in TBI patients can further disrupt visuospatial processing.
Daily Functioning Across TBI Severities
The impact of TBI on daily life varies depending on severity:
Mild TBI (concussion)
Morning: May experience headaches, dizziness, or fatigue upon waking
Work/School: Can return to daily activities but may struggle with concentration and memory lapses
Social Interactions: Mild difficulties in processing conversations or recalling details
Evening: Fatigue may set in earlier than usual, requiring extra rest
Most individuals with mild TBI recover within weeks to months, but some experience persistent post-concussion symptoms affecting daily life.
Moderate TBI
Morning: May need assistance with organising tasks due to memory deficits
Work/School: Struggles with multitasking, attention, and visuospatial reasoning
Social Interactions: Difficulty recognising faces or navigating familiar places
Evening: Increased cognitive fatigue, requiring structured routines
Individuals with moderate TBI often require rehabilitation to regain independence.
Severe TBI
Morning: May need full-time assistance for basic tasks (dressing, eating).
Work/School: Unlikely to return to work or school due to significant cognitive impairments
Social interactions: Difficulty processing conversations, recognising people, or navigating spaces
Evening: Requires caregiver support for daily routines.
Severe TBI can lead to lifelong disabilities, affecting independence and quality of life
Rehabilitation Strategies for Visuospatial Memory after TBI
Focus on restoring visuospatial memory and compensating for deficits
Cognitive Rehabilitation Therapy (CRT)
Memory Training: Exercises like object recall and paired associations to strengthen memory.
Visualisation Techniques: Encouraging mental imagery to improve spatial recall
Method of Loci - Associating information with specific locations to enhance memory
Multidomain Cognitive Rehabilitation Programs
Programs targeting attention, memory, visuospatial abilities, and executive functioning together have shown positive effects in TBI recovery
A 24-week neuropsychological rehabilitation program improved memory encoding, retrieval, and spatial reasoning in a patient with severe TBI-associated diffuse axon injury
Diffuse axonal injury (DAI), also known as traumatic axonal injury (TAI), is a severe form of traumatic brain injury due to shearing forces. DAI is the result of traumatic shearing forces that occur when the head is rapidly accelerated or decelerated, as may occur in car accidents, falls, and assaults. Vehicle accidents are the most frequent cause of DAI; it can also occur as the result of child abuse such as in shaken baby syndrome.
External Memory Aids
Daily Planners & Checklists: Helps organise tasks and improve recall
Smartphone Apps & Alarms: Assist with reminders for navigation and appointments
Environmental Modifications
Labeling Objects & Spaces: Helps individuals recognise locations more easily
Structured Routines: Reduces cognitive load and enhances memory retention
Neurofeedback & Cognitive Stimulation
Puzzles & Games: Activities like Sudoku, chess, and mazes improve visuospatial reasoning
Virtual Reality Therapy: Simulated enviroments help retain spatial awareness and navigation skills. VR-based rehabilitation has been effective in improving visuospatial deficits in TBI patients
Neurofeedback Training - Helps regulate brain activity to enhance cognitive function
Occupational & Physical Therapy
Motor-Spatial Coordination Training: Improves movement and spatial perception
Navigation Exercises: Practicing wayfinding in familiar and unfamiliar environments
Neuroplasticity and TBI Recovery
Neuroplasticity refers to the brain’s ability to recognise itself by forming new neural connections. This process is critical for recovery after Traumatic Brain Injury (TBI), as it allows the brain to compensate for damaged areas and restore lost functions.
Key mechanisms of neuroplasticity in TBI recovery
Synaptic Plasticity - Strengthening or weakening synaptic connections to improve communication between neurons
Structural Plasticity - Growth of new neurons (neurogenesis) and formation of new synapses (synaptogenesis)
Functional Reorganisation - Healthy brain regions take over functions previously handled by damaged areas
Long-Term Potentiation (LTP) - Strengthening neural pathways to enhance memory and learning
Research highlights that rehabilitation strategies can enhance neuroplasticity, leading to better cognitive and motor recovery.