I&I
HANDOUT IN INFECTIOUS, INFLAMMATORY AND IMMUNOLOGIC RESPONSE
• Introduction
• Nurses are directly involved in providing a biologically safe
environment….Microorganisms exist everywhere in water, soil and on body surfaces
such as skin, intestinal tract, and other areas open to the outside ( mouth, upper
respiratory tract, vagina
• and lower urinary tract).
• Most microorganisms are harmless, and some are even beneficial in that they perform
essential function in the body.
• Some microorganisms found in the intestines (enterobacteria) produce substances that
repress the growth of other microorganisms……
• Some microorganisms are normal RESIDENT FLORA (the collective vegetation in a
given area) in one part of the body, yet produce infection in another. Eg. Escherichia coli
is normal inhabitant of the large intestine but a common cause of infection in the urinary
tract.
• Definition of Terms
• Immunology – Branch of medicine that concerns with the study of human response to
foreign substances
• Immunity –the body’s specific protective response to an invading foreign agent or
organism.
• Immune system – this consist of complex and vital network of organs and cells that is
responsible for protecting the body from invading microorganisms.
• Antibody – protein substance developed by the body in response to and interacting
with a specific antigen.
• Antigen – substance that induces the production of antibodies
• B- Cells – cells that are important for producing a humoral immune response
• T-Cells – cells that are important for producing a cellular immune response
• Definition of Terms
• Humoral immune response – immune system’s 2 nd line of defense; often termed the
antibody response.
• Cellular immune response – immune system’s 3 rd line of defense, involving the attack
of pathogens by T-cells.
• Complement – series of enzymatic proteins in the serum that when activated, destroy
bacteria and other cells
• Interferons – protein formed when cell are exposed to viral or foreign agents; capable
of activating other components of the immune system.
• Overview of the Lymphatic System & Immunity
• Functions of the Immune system
• Defense against physical injury and infection
• Maintenance of homeostasis (state of equilibrium of the internal environment)
• Functions
• LYMPH
• Fluid that goes between capillary blood and tissues.
• LYMPH VESSELS
• Transport excess tissue fluid back into circulatory system.
• LYMPH NODES
• Produce lymphocytes, filter out harmful bacteria.
• SPLEEN
• Produces lymphocytes and monocytes, blood reservoir, recycles old red cells.
• THYMUS GLAND
• Produces T-LYMPHOCYTES
• LYMPH
• 1. Carries digested food, O2, and hormones to cells
• 2. Carries wastes back to capillaries for excretion
• 3. Since lymphatic system has no pump, skeletal muscle action squeezes Lymph along
• 4. Lymph in tissues is interstitial fluid
• Lymph Vessels
• 1. Valves prevent backward flow
• 2. Lymph flows in only one direction – from body organs to heart
• 3. Closely parallel veins
• 4. Tissue lymph enter small lymph vessels which drain into larger lymph vessels
(lymphatics) into two main lymphatics – the thoracic duct and right lymphatic duct
• Organs & tissues of the Immune system
• Bone marrow
• Thymus
• Lymph nodes
• Spleen
• Tonsils & other mucoid tissues
• Liver
• Bone marrow
• Specialized soft tissue filling the spaces in cancellous bone of the epiphyses.
• Responsible for:
1. Releasing mature B lymphocytes into blood circulation
2. Moving T lymphocytes from bone marrow to the thymus.
• Thymus
• Single unpaired gland located in the mediastinum
• Primary central gland of the lymphatic system
• Function is to allow T - lymphocytes to develop before migrating to the lymph nodes &
spleen
• Lymph nodes
• Are rounded structures varying in sizes from that of small seeds that are distributed
along the lymphatic vessels
• Functions:
a. Transporting lymph
b. Filtering & phagocytizing (processing & killing) antigens
c. Generating lymphocytes & monocytes
• Spleen
• highly vascular bean-shaped, gland like organ beneath the diaphragm and behind to the
left of the stomach
• Functions:
a. Removing worn-out erythrocytes from blood
b. Storing blood & platelets
c. Filtering & purifying blood
• First lines of defense
• Pathogens
• = disease causing micro-organisms
• bacteria
• virus
• fungi,
• protozoa,
• parasite,
• Prion
• Helminths
• Second lines of defense
• Involves white blood cells
• Non-specific response
– invading pathogens are targeted by macrophages
• Specific response
– lymphocytes produce chemicals called antibodies that target specific pathogens
• Phagocytes
• Phagocytes
• Monocytes and macrophages
• Provide a non-specific response to infection
• Phagocytosis
• Stages in phagocytosis
1. Phagocyte detects chemicals released by a foreign intruder (e.g. bacteria)
2. Phagocyte moves up the concentration gradient towards the intruder
3. The phagocyte adheres to the foreign cell and engulfs it in a vacuole by an
infolding of the cell membrane.
4. Lysosomes (organelles which are rich in digestive enzymes & found in the
phagocytes cytoplasm) fuse with the vacuole & release their contents into it.
• Phagocytosis
1. The bacterium is digested by the enzymes, and the breakdown products are
absorbed by the phagocyte.
During infection, hundreds of phagocytes are needed.
Pus is dead bacteria and phagocytes!
• Pus An accumulation of : -
– dead phagocytes
– destroyed bacteria
– dead cells
• Lymphocyte
• Lymphocytes
Provide a specific immune response to infectious diseases.
There are 2 types: -
T-cells - B-cells
They produce antibodies.
• Antigens
• all cells have surface markers called antigens.
• body can recognise these as self or non-self (foreign)
• Specific response
• Lymphocytes detect presence of foreign antigens
• Stimulated to produce specific proteins called antibodies.
• antibodies combine with their specific antigen (like a lock and key)
this renders the pathogen harmless.
• = primary response
• Immunity
• = the bodies ability to resist infection
• can be natural or acquired
• Immunological memory
• after an infection is fought off some lymphocytes become memory cells.
• if same pathogen returns memory cells stimulate the produce the specific antibody very
rapidly.
• the infection is fought off before symptoms appear = secondary response
• vaccines can stimulate same response
• Categories of Immunity
• Natural /Innate immunity (non-specific)
• Present at birth
• the body recognizes and destroys foreign substances but the response to them is the
same time the body is exposed to them.
• Acquired/Adaptive immunity (specific)
• Develops after birth
• the body recognizes and destroys foreign substances but the response improves each
time the foreign substances is encountered.
• Nonspecific Defenses
• Major Categories:
– Physical categories
• Mechanical categories
– Tears
– Urine flow
– Normal Peristaltic activity
– Vomiting and diarrhea
• All flush out bacteria & other toxins from the body
• Perspiration
• Certain fatty acids on the skin surface
• GIT and vaginal secretions
• Enzymes (lysozyme)
Leukocytes – a mobile system originate in the bone marrow when large pools
of mature cells are stored until they are needed and released in the
circulation and emigrate to the center of the cellular injury.
• a. 2 major classes of Leukocytes
Agranulocytes and Granulocytes
• b.Complement
• c.Perforin
• Inflammatory response
Is a localized protective response elicited by injury or destruction of tissues, which
serves to destroy, dilute, wall off both injurious agent and injured tissue.
• Functions of Inflammatory Response
• The delivery of effector molecules and cells to the sites of infection
• The formation of a physical barrier to the spread of tissue damage or infection.
• Wound healing and tissue repair
• Systemic response to inflammation
a. Fever is the most common sign of systemic response to injury caused by endogenous
pyrogens
b. During this process, leukocytosis occur thus general nonspecific symptoms develop
including malaise, loss of appetite, aching and weakness.
• Manifestations of Inflammation
• Local manifestations
Erythema
Warmth
Pain
Edema
Functional impairment
• Systemic Manifestations
T > 100.4 F (38C) or 96.8F (36C)
P> 90/min
R> 20/min (tachypnea)
WBC > 12,000mm3 or > 10% bands
• Factors affecting the outcome of the Inflammatory Process
1. Nature of the stressor
a. Number or amount
b. Virulence
c. The spreading factor
d. Resistance of phagocytosis
2. Nature of the person stress response
a. Age
b. Nutrition
c. Economic standing
d. Social setting
e. Tissue affected
f. Presence of chronic diseases
g. Presence of diabetes
• NURSING interventions
1. Health History
2. Physical assessment
a. Identifying the cause of inflammation
• Physical stressors
• Chemical stressors
• Biologic stressors
b. Determining the location of the inflammation
c. Estimating the location of inflammation
• Physical Assessment
• Assess the general appearance
• Assess skin color, temperature and moisture
• Inspect the mucous membranes of the nose and mouth for color and condition
• Inspect and palpate the cervical lymph nodes for evidence of lymphadenopathy
(swelling) or tenderness
• Assess the musculoskeletal system by inspecting and palpating the joints for redness,
swelling, tenderness or deformity
• Diagnostic Assessment
• To assess the client’s response to infection, identify the infecting organism and monitor
the progress of therapy.
1. WBC count
Provides clues about the infecting organism and the body’s immune response to it.
2. Cultures of the wound, blood or other infected body fluids
Are used to identify probable microorganisms by their charac. Such as shape, growth
patterns and gram-staining qualities
After the organism is cultured it is subjected to various antibiotics known to be effective
against it…..known as SENSITIVITY TESTING
24 to 48 hours is required to grow the organism
3. Serologic testing
Provides an indirect means of identifying infecting agents by detecting antibodies to the
suspected organism.
Not as accurate as culture, serology is particularly useful for organisms that cannot
easily be cultured (Hepatitis B or HIV)
ERYTHROCYTE SEDIMENTATION RATE (ESR or sed rate)
Is a nonspecific test to detect inflammation.
An increased ESR indicate acute or chronic inflammation, TB, autoimmune disorders,
malignancies, nephritis.
Decreased ESR is found in congestive heart failure, sickle cell anemia, & polycythemia
vera
4. Radiologic examination of the chest, abdomen, or urinary system
To detect organ abnormalities indicating an inflammatory response or tissue damage
5. Lumbar puncture
> Is performed to obtain cerebrospinal fluid (CSF) for examination and culture if a CNS infection
is suspected. (Meningitis or Encephalitis)
6. Ultrasonic examination
Is a noninvasive diagnostic test to evaluate organ function such as echocardiogram or
renal ultrasonography
7. Serum protein
Measures the total protein in the blood including albumin and globulins
Adult: 6 to 8 g/dL, Albumin 3.2 to 4.5 g/dL, Globulins 2.3 to 3.4 g/dL
If Total protein levels, albumin, globulin are decreased indicative of malnutrition, liver
disease or immunologic deficencies.
8. Antibody testing
Is ordered to determine if a client has developed antibodies in response to an infection
or immunization. (Hepa, HIV ,rubella, treponema pallidum)
An elevated level of titer indicates immunity.
9. Skin testing
Can assess cell mediated immunity
An antigen such as streptokinase, tuberculin PPD or candida is injected ID. The site is
observe for induration and erythema for 24 to 48 hrs.
An induration of 10mm in diameter is (+) reaction indicating previous exposure and
sensitization to the antigen.
No reaction or ANERGY indicates depressed cell mediated immunity.
• Communicable Diseases
• Epidemiology
• Greek words epi, meaning on or upon, demos, meaning people, and logos, meaning the
study of
• Epidemiology is the study (scientific, systematic, data-driven) of the distribution
(frequency, pattern) and determinants (causes, risk factors) of health-related
states and events (not just diseases) in specified populations (patient is
community, individuals viewed collectively), and the application of (since epidemiology
is a discipline within public health) this study to the control of health problems.
• CONTAGIOUS DISEASE INFECTIOUS DISEASE
• Disease that is easily transmitted from one person to another
• Disease transmitted by direct inoculation through a break in the skin
INFECTION
-Invasion of the body by the pathogenic microorganisms that reproduce and multiply causing
disease by local cellular injury, secretion of toxin, or antibody-antigen reaction of the
host.
INFESTATION
- The presence of animal parasites in the environment, on the skin, or in the hair of the a host.
• Cont…
ASEPSIS
- The absence of disease -producing microorganisms
SEPSIS
- The presence of infection or contamination
• Cont…
MEDICAL ASEPSIS
- Clean technique
- Practices designed to reduce the number and transfer of pathogens
SURGICAL ASEPSIS
- Sterile technique
- Practices that render and keep objects and areas free from microorganisms
HOST
- A person, animal or plant which harbors and provides nourishment for a parasite
RESERVOIR
- Natural habitat for the growth, multiplication and reproduction of microorganism
ISOLATION
- The separation of persons with communicable diseases from other persons
QUARANTINE
- The limitation of the freedom of movement of persons exposed to communicable diseases
• Cont…
CONCURRENT
- is a method of disinfection done immediately after the infected individual discharges infectious
material/secretions.
TERMINAL
- applied when the patient is no longer the source of infection
BACTERICIDAL
- A chemical that kills microorganisms
BACTERIOSTATIC
- An agent that prevents bacterial multiplication but does not kill microorganisms
• CHAIN OF INFECTION
• Pathogen
(Causative or Etiologic Agent)
• Bacteria
• Viruses
• Protozoa
• Fungi
• Parasite
• Helminths
• Reservoir
• 2 Types:
HUMAN RESERVOIR
• Main reservoirs of infection
• Infected persons from whom the infectious agent is transmitted to other person
a. Frank or Typical – patient is obviously ill and manifests signs and symptoms
b. Subclinical – patient has mild or inapparent signs and symptoms
c. Carriers – does not manifest signs and symptoms
d. Contact – in close association
e. Suspect – patient displays signs and symptoms
ANIMAL RESERVOIR
• Portal of Exit from Reservoir
• Respiratory tract
• Gastrointestinal tract
• Genitourinary tract
• Blood
• MODE OF TRANSMISSION
a. CONTACT TRANSMISSION
1. Direct contact – involves immediate and direct transfer from person-to-person
• Droplet Transmission - occurs when the mucous membrane of the nose,
mouth or conjunctiva are exposed to secretions of an infected person within a
distance of three feet
• Airborne Transmission - occurs when fine particles are suspended in the air
for a long time or when dust particles contain pathogens
• Mode of transmission …
Indirect contact – occurs when a susceptible host is exposed to a contaminated
object
b. VEHICLE/ROUTE TRANSMISSION
• Transfer of microorganisms by way of vehicles or contaminated items that
transmit pathogens
Food – Salmonellosis
Water – shigellosis
Drugs – infusion of drugs with contaminated needle
Blood – AIDS, hepatitis B virus
• Mode of transmission …
c. VECTOR-BORNE TRANSMISSION
• Transmitted by biologic vectors like rats, snails and mosquitoes, anthropods
(flies, ticks, and others)
• Remember!
The EASIEST way to break the Chain of infection is through MODE OF
TRANSMISSION
• Distribution of a Disease
• SPORADIC
a. Intermittent occurrence of a few isolated and unrelated cases in a given locality
b. Disease is occasionally present here and there.
c. High number of immunes and low number of susceptibles
d. Eg. Rabies
• Distribution of a Disease
• ENDEMIC
a. Continuous occurrence throughout a period of time of the usual number of cases in a
given locality
b. Low number of immunes and low number of susceptibles
c. Eg. Malaria
• Distribution of a Disease
• EPIDEMIC
a. Occurrence of an unusually large number of cases in a relatively short period of time
b. Low number of immunes and high number of susceptibles
c. Eg. AIDS
• Distribution of a Disease
• PANDEMIC
a. Simultaneous occurrence of epidemics of the same disease in several countries
b. Worldwide epidemic
c. Low number of immunes and high number of susceptibles
d. Eg. SARS, HIV
• HERD IMMUNITY – state of immunity of the community
• STAGES OF THE INFECTIOUS PROCESS
(Stages of Illness)
• Incubation Period
- The time between exposure to a pathogenic organism & the onset of symptoms of a disease
• Prodromal Period /Catarrhal Period
– patient feels “bad” but not yet experiencing actual symptoms of the disease
• Period of Illness/Acme
– onset of typical or specific signs and symptoms of a disease
• Convalescent Period/
– signs and symptoms start to abate and client returns to normal health
• PRINCIPLES OF IMMUNIZATION
• IMMUNITY
> Is a condition of being secure against any particular disease.
• IMMUNIZATION
> Is the introduction of specific protective antibodies in a susceptible person, or animal, or the
production of cellular immunity in such person or animal.
• PRINCIPLES OF IMMUNIZATION (EPI PD 996 Providing for compulsory
Basic Immunization for Infants and Children below 8 yrs old)
• Which of the following is the Main principle of the EPI Program?
- It is based on Epidemiological situation
• Seven Preventable Diseases be given before the 1 st Birthday of the child.
1. TB
2. Diphtheria
3. Pertussis
4. Tetanus
5. Polio
6. Hepa
7. Measles
• RESISTANCE
- The body’s ability to withstand infection, but it does not absolutely mean that one who
possesses it is free from disease.
• Classes of Immunoglobulins
• TYPES OF IMMUNIZATIONS
• ACTIVE – antibodies produced by the body
– NATURAL – antibodies are formed in the presence of active infection in the
body; lifelong
– ARTIFICIAL – antigens are administered to stimulate antibody production
• PASSIVE – antibodies are produced by another source
– NATURAL – transferred from mother to newborn through placenta or colostrum
– ARTIFICIAL – immune serum (antibody) from an animal or human is injected
to a person
• Sub-clinical
Acquired through constant exposure to a particular disease or organism.
• Types of Antigen
• INACTIVATED (Killed Organism)
a. Not long lasting
b. Multiple doses needed
c. Booster doses needed
• ATTENUATED (Live Organism)
a. Single dose
b. Long lasting immunity
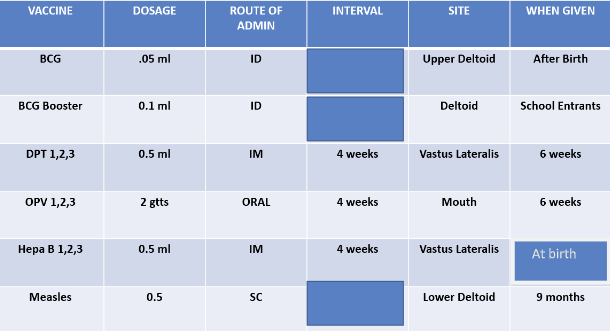
• Vaccines
• All vaccines lose their potency after a certain time.
• The expiry date should be indicated on the vaccine label
• What damages Vaccines?
• Heat & sunlight damage vaccines, especially the live ones.
• Freezing damages killed vaccines and toxoids
• Use water only in cleaning the refrigerator/freezer.
• Antiseptics, disinfectants, and detergents or alcohol may lessen the potency of vaccines.
• Safest thing is to keep all vaccines at correct cold temperature (0-8 C).
• Cold Chain System
• Concepts of Health Promotion, Wellness & Illness Prevention
• Health promotion
Activities help clients maintain or enhance their present level of health.
Ex. Routine exercise and good nutrition
Motivate people to act positively to reach a more stable level of health.
• Wellness Education
Teaches people how to care for themselves in a healthy way.
Ex. Topics such as physical awareness, stress management, and self- responsibility
• Illness Prevention
Motivates people to avoid a decline in health or functional level.
ex. Immunization (protect from actual or potential threats to health).
• Levels of Preventive Care
1. Primary prevention
Aims at health promotion and includes health education, immunization and physical &
nutritional fitness.
At birth
2. Secondary Prevention
Focuses on individuals who are experiencing health problems or illnesses and who are at
risk of developing complications or worsening conditions.
3. Tertiary prevention
Occurs when a defect or disability becomes permanent and irreversible.
Involves minimizing the effects of long-term disease or disability through intervention
directed at preventing complications and deterioration.
• Environmental Sanitation
• PD 856 – Code of Sanitation of the Philippines
1. Water Supply Sanitation Program – DOH through EHS sets policies in the following
areas:
A. Approved types of water facilities such as:
1. Level 1 (Point of Source)
> a protected well or a developed spring with an outlet but w/o a distribution system
generally adaptable to rural areas.
2. Level 2 (Communal Faucet System or Stand-Posts)
Composed of a source reservoir; a piped distribution network and communal faucets.
3. Level 3 – waterworks system or individual house connection.
B. Unapproved types of water facility or water coming from doubtful sources such as open
dug wells, unimproved springs, and well that need priming, are not allowed for drinking unless
treated through proper container disinfection.
C. Access to safe and potable drinking water
All households should be provided with a safe and adequate water supply.
D. Water quality and monitoring
Examination of drinking water shall be performed only in private and government
laboratories duly accredited by the DOH.
• Water Supply Sources that need to be disinfected:
> newly constructed water supplies facilities
Water supply facility that has been repaired or improved
water supply sources found to be bacteriologically positive through laboratory anaylsis
E. Waterworks/water system and well construction
The well site shall require approval of the Secretary of health or his duly authorized
representative
Well construction shall comply with the sanitary requirements of the DOH.
Water supply system shall supply safe and potable water in adequate quantity.
Water shall be made readily available to consumers/users.
a. Approved types of toilet facilities
1. Level 1 (Non-water carriage toilet facility)
> Pit latrines, reed odorless earth closet
> toilet facility requiring small amount of water to wash the waste into receiving space
(pour flush, aqua privies)
2. Level 2 – water sealed and flush type with septic vault/tank disposal facilities.
3. Level 3 – water carriage toilet connected to a septic tank or sewerage and treatment plant.
b. In Rural areas a “blind drainage” type of waste water collection and disposal
facility.
• Policies on Food Sanitation Program
a. Food establishments shall be appraised as to the following sanitary
conditions:
> Inspection/ approval of all food sources, containers and transport vehicles
Compliance to sanitary permit requirements
Provision of updated health certificates for food handlers, cook and kitchen helpers
Destruction o/banning of food unfit for human consumption
Training food handlers and operators on food sanitation
b. Ambulant food vendors shall also comply with the requirements as to the
issuance of health certificates.
c. Household food sanitation is to be promoted and monitored and food hygiene
sanitation is to be intensified.
• Policies on Hospital Waste Management
• All newly constructed/renovated government and private hospitals shall prepare and
implement a hospital waste management (HWM) program as a requirement for the
registration/renewal of licenses.
• Use of appropriate technology and indigenous materials for HWM shall be adopted
• Training of hospital personnel involved in waste management shall be an essential part
of the hospital’s training program.
• Local ordinances regarding the collection and disposal techniques especially incinerators,
shall be institutionalized.
• SEVEN CATEGORIES OF ISOLATION
• ISOLATION - is the separation from other person of an individual suffering from a
communicable disease. QUARATINE - is the limitation of freedom of movement of
persons or animals which have been exposed to communicable disease/s for a period of
time equivalent to the longest incubation period of that disease.
1. STRICT -prevent highly contagious or virulent infections
• Example: chickenpox, herpes zoster
2. CONTACT – spread primarily by close or direct contact
• Example: scabies, herpes simplex
3.RESPIRATORY – prevent transmission of infectious distances over short distances through
the air
• Example: measles, mumps, meningitis, tuberculosis
• SEVEN categories of Isolation …
4. ENTERIC – prevent transmission through direct contact with feces
• Example: poliomyelitis, typhoid fever
5. DRAINAGE – prevent transmission by direct or indirect contact with purulent materials or
discharge
• Ex. Burns
6. UNIVERSAL – prevent transmission of blood and body-fluid borne pathogens
• Example: AIDS, Hepatitis B
7. TB Isolation -is carried out for TB patients with positive smear or chest xray that strongly
suggests active TB, both pulmonary and extrapulmonary.