Labor and Delivery Notes Review
Overview: role and flow in labor and delivery
Labor and delivery (L&D) nurses guide the mother through admission, assessment, monitoring, and management of labor, delivery, and the immediate postpartum period.
Key priorities: establish baselines (vital signs, fetal heart rate), obtain health history, determine birth preferences, monitor contractions and fetal status, and respond to complications.
Respect patient autonomy: honor birth plans (medicated vs unmedicated, water birth, home birth considerations) within safety limits; escalate if harm could occur.
First Stage of Labor
Admission assessment upon arrival:
Vital signs, health history (age/DOB, allergies, past medical/surgical history, obstetric history).
Birth plan and preferences (medicated vs unmedicated, water birth, home birth, etc.).
Fetal heart rate monitoring and maternal monitoring begins.
Typical sequence on admission:
Reassess contractions: frequency, intensity, duration; contractions listed as every five minutes in example.
Monitor fetal heart rate (top monitor over baby) and contractions (bottom monitor for contractions).
Check membranes: rupture status (SROM vs AROM), color and odor of amniotic fluid, time since rupture (critical for infection risk).
Membrane rupture details:
Prolonged rupture of membranes (PROM) is a concern; infection risk increases with time: aim to deliver within ~20-24 hours after rupture in an ideal scenario; in practice, treat as PROM and may give antibiotics if prolonged.
SROM: spontaneous rupture of membranes
AROM: artificial rupture of membranes
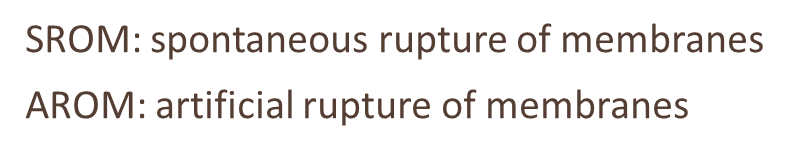
Amniotic fluid color expectations:
Clear to lightly pink-tinged; a small yellow tinge acceptable.
Green/brown color indicates meconium passage, risk for meconium aspiration and distress.
Time since rupture is important for infection risk and to guide management.
Cervical checks and dilation:
Dilation is measured in centimeters from 0 to 10, with full dilation at 10 centimeters indicating readiness for delivery. It is crucial to assess dilation regularly, as it provides insight into the progress of labor and potential interventions when labor stalls.
Effacement is expressed as a percentage
Initial cervix may be closed; dilation and effacement occur together as labor progresses.
Station relates to the baby’s descent in the pelvis, determined during checks (see Station below).
Fetal presentation and positioning:
Fetal presentation is what part of the baby is presenting first; ideally the cephalic (head) presentation.
Breech (butt or feet presenting) is less common and may lead to cesarean if not easily managed.
Leopold’s maneuvers help determine fetal presentation and position in the pelvis.
Occiput anterior (OA) is the ideal fetal position: back of the baby’s head toward the front of the mother’s pelvis.
Occiput posterior (OP) can cause back labor and may require rotation or intervention.
Fetal monitoring and cord considerations:
External or continuous fetal monitoring assesses fetal heart rate and contraction frequency/intensity.
Watch for cord issues (nuchal cord around neck; prolapsed cord if cord slips ahead of the baby during rupture or descent).
If prolapsed cord occurs, emergent delivery is usually required.
Labor progression and interventions:
Cardinal movements guide the baby’s descent through the birth canal (descent, flexion, rotation, internal rotation, extension, restitution, expulsion).
Peanut ball and positioning options can aid labor progression, especially with an epidural.
Episiotomy vs tearing: episiotomy is a surgical cut to allow space for delivery; 1st–4th degree tears describe increasing depth of perineal injury.
Pain management & mobility:
Epidural vs spinal anesthesia:
Epidural: catheter in the epidural space, continuous analgesia; can affect blood pressure and mobility.
Spinal anesthesia: single-dose, no catheter; often used for cesarean delivery or rapid pain relief for vaginal birth.
If on an epidural, mobility may be limited; the patient may need to lie down or sit with bed head elevated.
Alternatives include nonpharmacologic methods and, if appropriate, other analgesics (e.g., antiemetics like Zofran) with varying effects on the baby.
A doula may accompany and support the birthing person.
Nursing considerations during first stage:
Continuous education and reassurance; assess contractions, fetal heart rate, pain, vitals, and overall well-being.
Be prepared for potential changes in plan (e.g., transition to C-section if fetal distress or malpresentation occurs).
Fetal Station and Presentation Details
Station system:
Station zero corresponds to the level of the ischial spines in the maternal pelvis.
Negative stations indicate the baby is higher in the pelvis; positive stations indicate descent toward delivery.
As the baby descends (toward positive), delivery becomes more imminent; historically, a positive three is often described as baby well engaged in the pelvis.
Note: You don’t necessarily start pushing at exactly a particular station; pushing typically begins once dilation is about 10 cm and the patient is fully effaced, but some progression can begin when the baby is sufficiently descended.
Fetal presentation concepts:
Head presentation is ideal; breech (butt) or other presentations may require cesarean delivery depending on the situation.
Shoulder dystocia risk with oblique or transverse fetal positions; management often requires quick maneuvers by the clinician.
Fetal position inside the pelvis:
Occiput anterior (OA) is ideal; occiput posterior (OP) can cause longer labor and back pain.
Leopold maneuvers help determine fetal lie and orientation.
Second Stage of Labor (Delivery)
Trigger and process:
Begins at full dilation (usually 10 cm) and ends with the birth of the baby.
Pushing is coordinated with contractions to maximize effectiveness; do not push between contractions.
Methods of pushing and position:
With an epidural, options may be limited and hospital protocols suggested positions (lying on back, bed head up, etc.).
Alternatives for comfort and effectiveness include side-lying, peanut ball, and upright positions when feasible.
Cardinal movements and obstetric assistance:
The baby descends and rotates through the birth canal; physician may assist rotation and delivery as needed.
Episiotomy vs spontaneous tearing:
Episiotomy is a surgical incision to facilitate delivery; may prevent more extensive tearing but is not universally required.
Complications in the second stage:
Shoulder dystocia can occur if shoulders get caught; careful maneuvers are required.
Vacuum or forceps assisted delivery may be used in certain situations to expedite delivery and reduce risk to mother/baby.
Third Stage of Labor (Placenta Delivery)
What it is:
The interval from birth of the baby to delivery of the placenta.
Typical duration: about .
Management:
Often minimal patient effort is required; physician may request a light push to help deliver the placenta.
Cord clamping: delayed cord clamping may be performed by parental preference to allow more placental blood transfer to the newborn.
Cord blood donation is an option for families (donation to a bank or for personal use).
Retained placenta and hemorrhage risk:
Retained placenta increases risk of infection and hemorrhage; careful inspection of placenta after delivery is essential.
Placental function and structure:
Nutrient and gas exchange between mother and fetus occurs via the placenta; oxygenation occurs in the placenta rather than the fetal lungs pre-birth.
Umbilical cord anatomy:
A typical 3-vessel cord consists of two arteries and one vein:
Umbilical vein carries oxygenated blood from placenta to fetus.
Umbilical arteries carry deoxygenated blood from fetus back to placenta.
In total, the vessels ensure bidirectional flow for gas and nutrient exchange.
Fetal circulation (in utero) quick review:
Three fetal shunts to bypass nonfunctioning lungs:
Ductus venosus connects the umbilical vein to the inferior vena cava (IVC).
Foramen ovale connects the right atrium to the left atrium, bypassing the lungs.
Ductus arteriosus connects the pulmonary artery to the aorta, bypassing the lungs.
After birth, these shunts typically close due to changes in pressure and lung expansion; sometimes closures take 24–48 hours or longer, and some newborn murmurs may occur temporarily.
Practical notes:
If a murmur is detected, follow-up (e.g., echocardiography) may be performed to assess shunt status.
VBAC considerations: previous cesarean incision type affects the option for a future vaginal delivery; low transverse incisions are more compatible with VBAC than classical incisions.
Fourth Stage of Labor (Immediate Postpartum)
Time frame:
1 to 4 hours after birth.
Maternal physiology:
Blood pressure often stabilizes or decreases; heart rate may rise briefly; uterus should contract to prevent hemorrhage.
Uterus (fundus) should be firm and midline; a boggy uterus indicates risk for hemorrhage and requires fundal massage and cessation of bleeding.
Bladder considerations:
Bladder distension can displace the uterus and increase bleeding risk; ensure patient voids regularly when possible.
Perineum and lochia:
Inspect perineal area for tears or episiotomy repair status.
Lochia (vaginal discharge after birth) is initially red (lochia rubra) and changes over time.
Clots are possible; large clots or bleeding more than one pad per hour warrants attention.
Bonding and feeding:
Skin-to-skin contact and early breastfeeding are encouraged when mother and baby are stable; supports temperature regulation and early bonding.
Postpartum nursing priorities:
Monitor vital signs, bleeding, pain, fundal height/tone, bladder function, and perineal healing.
Apgar Scoring and Newborn Assessment
Apgar score purpose:
Quick assessment of the newborn at 1 and 5 minutes after birth (and as needed).
Five components (each 0, 1, or 2 points):
A = Appearance (skin color) – flesh tone and color
P = Pulse (heart rate) – heartbeat strength and rate
G = Grimace (reflex irritability) – response to stimulation
A = Activity (muscle tone) – tone and movement
R = Respirations (respiratory effort) – breathing quality
Typical scoring guidance:
Total possible score: , with higher indicating better condition.
In many hospitals, a secondary scoring may be used for more detailed context; expect a quick, structured newborn assessment by the NICU or nursery staff after birth.
Immediate post-birth care:
Baby is weighed and measured; assessed for temperature; dried and kept warm; placed on mother’s chest when stable; quick respiratory and heart assessments performed.
Cesarean Delivery (C-Section) Overview
Indications for C-section:
Fetal malpresentation (e.g., breech not safely deliverable vaginally).
Active genital herpes infection (to prevent neonatal transmission).
Cord prolapse or fetal distress requiring rapid delivery.
Cephalopelvic disproportion or pelvic constraints (small pelvis or disproportion with large head).
Prior uterine surgery concerns; VBAC decisions depend on incision type and clinical scenario.
Fetal or maternal health risk necessitating urgent operative delivery.
Typical C-section approach:
Procedure is performed in the operating room; standard low transverse uterine incision is common today; classical incisions are less common but may be used in certain cases.
VBAC considerations influenced by prior incision type; a prior classical incision may limit future VBAC.
Preop: consent, IV access, Foley catheter after spinal, abdominal prep, draping, and presence of a care partner if allowed.
Anesthesia options:
Spinal anesthesia: rapid onset, no catheter; suitable for cesarean delivery and certain vaginal procedures.
Epidural anesthesia: catheter with ongoing analgesia; can be used for cesarean as well but typically used for labor analgesia; if a spinal is required, the patient will be converted to a spinal block.
General anesthesia: reserved for high-risk scenarios or emergency situations where regional anesthesia is not feasible.
Postpartum considerations after C-section:
Postoperative monitoring in recovery; risk of pain, infection, and delayed gut motility; recovery plan includes early mobilization when feasible and pain control.
Induction and Augmentation of Labor
Induction strategies often used when pregnancies pass a certain post-term threshold or when maternal/fetal conditions require it.
Cervical ripening methods:
Cervadil (dinoprostone): vaginal insert that softens and ripens the cervix and may induce contractions.
Cytotec (misoprostol): tablet form used for cervical ripening and induction; typically more potent than Cervadil.
Augmentation with Pitocin (oxytocin):
Pitocin is given intravenously to stimulate uterine contractions when labor is not progressing adequately.
When Pitocin is used, continuous fetal and maternal monitoring is typically required.
Typical sequence when inducing labor:
Cervical ripening agents are often given overnight to ready the cervix, followed by Pitocin the next day to initiate or augment contractions.
Rationale for induction/augmentation:
Reduce risks associated with post-term pregnancy (e.g., stillbirth risk, placental insufficiency) and manage maternal/fetal conditions.
Key Physiological Concepts to Remember
Placenta and fetal oxygenation:
In utero, the placenta handles oxygenation; the fetus does not rely on its lungs for oxygen until after birth.
The umbilical cord carries blood between the placenta and fetus; oxygenated blood flows via the umbilical vein to the fetus, while deoxygenated blood returns via the umbilical arteries to the placenta.
Fetal circulation shunts and their closure:
Ductus venosus: shunts some blood from umbilical vein to the IVC (bypassing the liver).
Foramen ovale: shunts blood from right atrium to left atrium, bypassing the lungs.
Ductus arteriosus: connects the pulmonary artery to the aorta, bypassing pulmonary circulation.
After birth, these shunts close as lung function begins and systemic pressures normalize; in some infants, closures may take up to 24–48 hours or longer.
Postpartum anatomy and healing:
The uterus contracts to prevent hemorrhage; fundal tone (firmness) is critical in the third and fourth stages of labor.
Lochia transition through stages (rubra, serosa, alba) as healing progresses; color and amount change over time.
Documentation and safety considerations:
Use of color, amount, and time for membranes and lochia; odor assessment if possible.
Avoidance of risk factors for infection, hemorrhage, and neonatal distress; ensure timely interventions when abnormalities are detected.
Practical Scenarios and Ethical Considerations
Birth plans and autonomy:
Clinicians should honor reasonable birth preferences (medicated vs unmedicated, water birth, etc.) within safety limits.
There may be extenuating circumstances where overrides are necessary to protect mother or baby; these should be carefully considered and discussed with the patient when possible.
Interprofessional communication:
Consistency between nurses and physicians in cervical checks (dilatation and effacement) reduces miscommunication and ensures appropriate care decisions.
Education and informed consent:
Provide clear explanations of procedures (epidural vs spinal, induction methods, cesarean rationale) and expected timelines to reduce patient anxiety and improve outcomes.
Quick Reference: Key Terms and Numbers
Dilation scale:
Effacement scale: 0 ext{ to }100 ext{%}
Prolonged rupture of membranes: >24 ext{ hours}
Stages of labor: First (labor), Second (delivery), Third (placenta), Fourth (postpartum recovery)
Typical cord vessels: two arteries and one vein (3 vessels total)
Apgar components: Appearance, Pulse, Grimace, Activity, Respirations (0–2 points each; total 0–10)
Common anesthesia types: Epidural (with catheter) vs Spinal (no catheter) vs General anesthesia
Placental functions: Nutrient and gas exchange; oxygenation occurs in the placenta, not in fetal lungs pre-birth
In utero shunts: Ductus venosus, Foramen ovale, Ductus arteriosus
Common induction agents: Cervadil (dinoprostone), Cytotec (misoprostol), followed by Pitocin (oxytocin)
Summary for Exam Preparation
Know the sequence and responsibilities in admission, assessment, stabilization, and ongoing monitoring through all four stages of labor.
Be fluent with terminology: dilation, effacement, station, presentation, lie, engagement, and the cardinal movements.
Understand fetal circulation in utero vs after birth, especially the three shunts and how closures occur.
Distinguish epidural vs spinal anesthesia, including implications for mobility, catheter presence, and hypotension risk.
Recognize indications for cesarean delivery and VBAC considerations, including incision types and historical practice.
Be able to identify scenarios requiring urgent interventions (cord prolapse, nonreassuring fetal status, shoulder dystocia, malpresentation).
Review the stages of labor timelines, common complications, and postpartum assessment priorities (fundus, lochia, bladder status, perineum, and skin-to-skin bonding).