3.4 The heart
Blood and Cardiovascular System
The Heart
The heart is a muscular organ that pumps blood throughout the body.
It plays a crucial role in the circulatory system by supplying oxygen and nutrients to tissues.
Functions of the Heart
Pumping Blood: Acts as a muscular pump to circulate blood through two main vascular circuits: pulmonary and systemic.
Regulating Flow: The heart valves ensure unidirectional blood flow and prevent backflow (regurgitation).
Location, Shape, and Size of the Heart
Located in the thoracic cavity, specifically in the mediastinum.
Mediastinum: The area between the lungs (the pleural sacs covering the lungs)
Posterior to the sternum and inferior to the sternal angle (angle of Louis).
Position corresponds to the level of 2nd costal cartilages (T4/T5 vertebrae).
Generally conical in shape with an apex pointing to the left side, measuring about the size of a fist.
Heart Structure
Chambers of the Heart
4 Chambers:
Atria: Two upper chambers (right and left atria) that receive blood.
Ventricles: Two lower chambers (right and left ventricles) that pump blood out.
Valves of the Heart
Atrioventricular (AV) Valves: Located between atria and ventricles, including the tricuspid and mitral (bicuspid) valves.
Semilunar (SL) Valves: Located between ventricles and major arteries (aorta and pulmonary trunk).
Coronary Circulation
Right Heart: Comprised of right atrium and right ventricle; receives deoxygenated blood and pumps it to the lungs.
Left Heart: Comprised of left atrium and left ventricle; receives oxygenated blood from lungs and pumps it to the body.
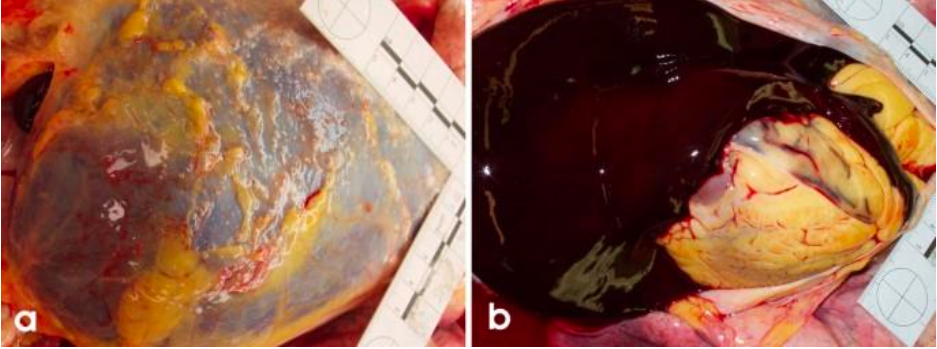
Cardiac tamponade
Cardiac tamponade is a medical emergency that occurs when fluid accumulates in the pericardial cavity, exerting pressure on the heart. This pressure impairs the heart's ability to pump blood effectively, leading to decreased cardiac output and potentially resulting in life-threatening complications. Causes of cardiac tamponade can include trauma, inflammation, or malignancy. Symptoms typically include shortness of breath, chest pain, and low blood pressure.
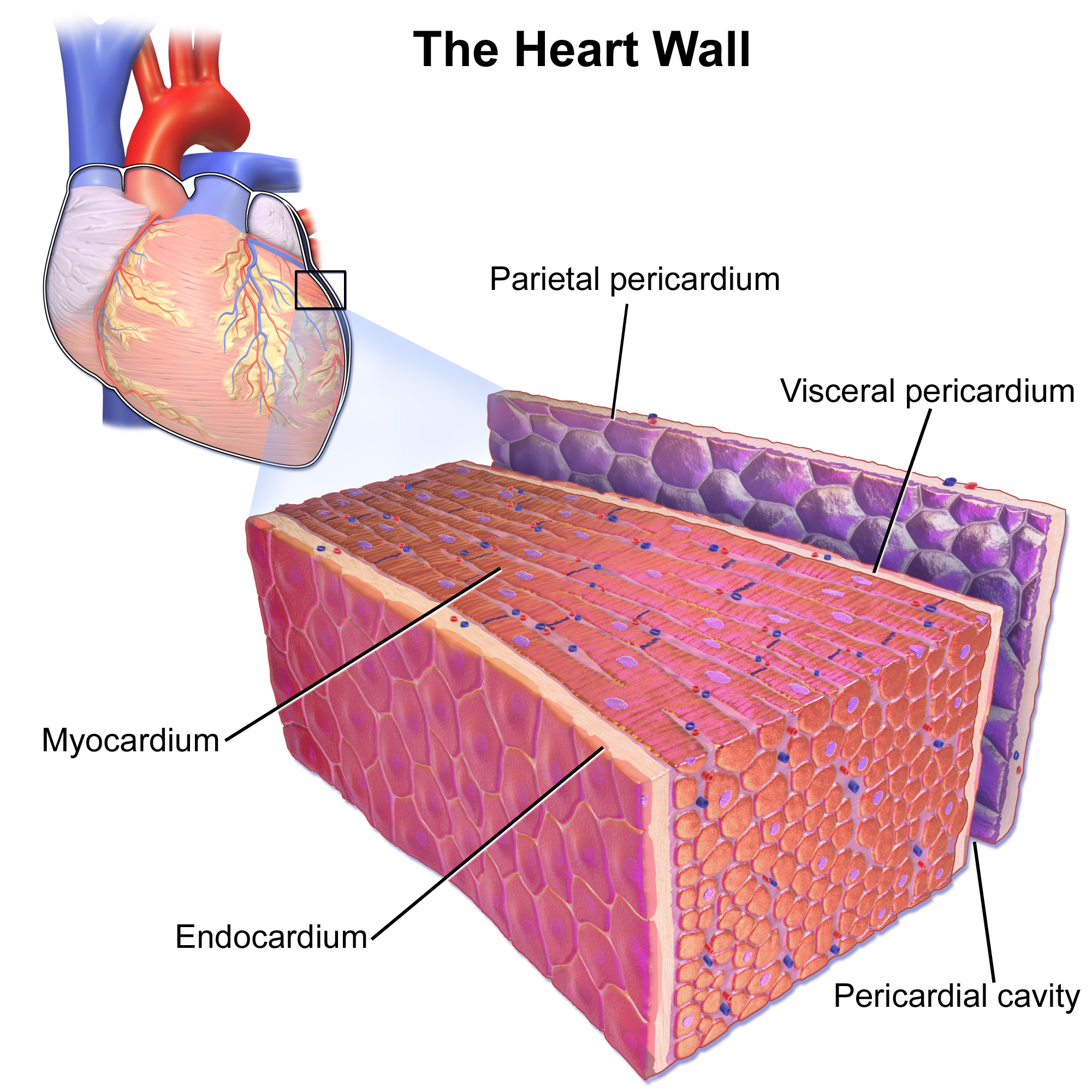
Layers of the heart
Parietal pericardium
The parietal pericardium is a fibrous and serous membrane that forms the outer portion of the pericardial sac. It has two layers:
Fibrous Layer: The tough outer layer that protects the heart and anchors it to surrounding structures.
Serous Layer: The inner layer that secretes pericardial fluid, allowing for smooth movement as the heart beats.
Pericardial cavity
The pericardial cavity is the space between the parietal pericardium and the visceral pericardium. It contains pericardial fluid, which acts as a lubricant to reduce friction between the heart and surrounding structures during the heartbeat.
Viceral pericardium
The visceral pericardium, also known as the epicardium, is the inner layer of the pericardial sac that directly adheres to the surface of the heart. It serves as a protective layer and contains blood vessels, nerves, and connective tissue that support the heart.
Myocardium
The myocardium is the thickest layer of the heart wall, composed of cardiac muscle tissue. This layer is responsible for the contracting action of the heart, enabling it to pump blood throughout the body. The myocardium's composition supports the heart's high oxygen demand and is essential for maintaining effective circulation.
Endocardium
The endocardium is the inner lining of the heart, varying in thickness. It provides a smooth surface for blood to flow over and is composed of endothelial cells. This layer also forms the valves of the heart, ensuring proper blood flow and preventing backflow between the heart chambers.
Surfaces and Apex of the Heart
Surfaces:
Sternocostal (anterior): Faces the sternum.
Diaphragmatic (inferior): Sits atop the diaphragm.
Pulmonary (left/right): Related to the lungs.
Apex: Located at the 5th intercostal space in the midclavicular line.
Base (posterior): Mainly formed by the left atrium and a portion of the right atrium.
Detailed Anatomy of the Heart
Right Atrium
Structures include:
Auricle: Increases capacity.
Pectinate muscles: Projections that increase surface area.
Crista terminalis: A ridge that separates the smooth part of the right atrium from the rough part, enhancing electrical conduction.
Fossa ovalis: Remnant of fetal circulation.
Coronary sinus opening: Drainage from the heart muscle.
Sinus venarum: The smooth-walled part of the right atrium that receives deoxygenated blood from the superior and inferior vena cavae, facilitating efficient blood flow into the right atrium.
Superior Vena Cava SVC and Inferior Vena Cava IVC: Superior vena cava (SVC) and inferior vena cava (IVC): Major veins that transport deoxygenated blood from the upper and lower body, respectively, into the right atrium.
Right Ventricle
Components include:
Tricuspid valve: Controls blood flow to the right ventricle.
Papillary muscles: Anchor valve leaflets.
Tendinous cords: Plays a crucial role in preventing the valves from inverting during ventricular contraction, ensuring that blood flows in the correct direction and preventing regurgitation.
Conus Arteriosus: A conical pouch that leads to the pulmonary artery, facilitating the flow of deoxygenated blood from the right ventricle to the lungs for oxygenation.
Pulmonary valve: Controls flow into the pulmonary artery.
Interventricular septum: A muscular wall that separates the left and right ventricles, preventing the mixing of oxygenated and deoxygenated blood, and providing structural support during the contraction of the heart.
Trabeculae carnae: Irregular muscular columns on the inner surface of the ventricles, which help to prevent the walls from sticking together during contraction and contribute to the efficient pumping of blood.
Left Atrium
Components include:
Pulmonary veins: Returns oxygenated blood from lungs.
Left auricle: Increases capacity.
Floor oval fossa: A depression in the interatrial septum that marks the location of the foramen ovale in the fetal heart.
Left Ventricle
Key features:
Ventricular wall: The left ventricular wall is significantly thicker than that of the right ventricle, allowing it to generate the high pressure needed to pump oxygenated blood to the entire body.
Mitral valve: Regulates blood flow into the left ventricle.
Aortic valve: Controls blood flow into the aorta.
Papillary muscles: These muscles are attached to the ventricles and chordae tendineae, helping to prevent the inversion or prolapse of the heart valves during contraction.
Trabeculae carnae: These irregular muscular columns are found on the inner surface of the ventricles, providing structural support and helping to facilitate the contraction of the heart muscle.
Heart sounds
Aortic valve: Right 2nd intercostal space next to the sternum
Pulmonary valve: Left 2nd intercostal space next to the sternum
Tricuspid valve: Left 5th intercostal space next to the sternum
Mitral valve: Left 5th intercostal space and midclavicular line
The skeleton of the heart
Provides structural support and electrical insulation between the atria and ventricles, ensuring coordinated contractions.
Support of leaflets and cusps
4 fibrous rings (annuli fibrosi)
Cardiac Valves and Skeleton
Valves:
Function: Support the direction of blood flow, avoid regurgitation
Atrioventricular (AV) — Leaflets
Semilunar (SL) — Cusps
Dense Connective Tissue Core: Known as fibrosa.
Covering: Covered on either side by fibroelastic connective tissue and endothelium.
Cardiac Skeleton:
Function: Provides structural support and electrical insulation between the atria and ventricles, ensuring coordinated contractions.
Support of leaflets and cusps
4 fibrous rings (annuli fibrosi)
Deep Endocardial Fibro-Collagenous Region:
Dense irregular connective tissue located at the level of heart valves.
Anchors valves and chambers together.
Tissue extends into the core of valve leaflets.
Coronary Circulation Basics
Coronary Arteries
Coronary Arteries: Left Coronary Artery (LCA) and Right Coronary Artery (RCA); they supply blood to the heart muscle itself.
LCA mainly serves the anterior part of the heart.
RCA supplies the posterior and diaphragmatic areas.
Surrounded by epicardial fats
Originate from the aorta superior to the aortic valves
Right Coronary Artery (RCA) supplies the Sinu-atrial (SA) node and the Atrioventricular (AV) node
Coronary Veins
Coronary Veins: Transports deoxygenated blood back to the right atrium.
Anterior cardiac venae
Drains to: Right atrium
Great Cardiac vena
Tributaries
Anterior interventricular vena
Left marginal vena
Oblique vena of left atrium
Drains to: Coronary Sinus
Left posterior ventricular vena
Drains to: Coronary Sinus
Middle cardiac vena
Drains to: Coronary Sinus
Small cardiac vena
Tributaries
Anterior venae of right ventricle
Right marginal vena
Drains to: Coronary Sinus
** Venae (vv.) is the plural form of Vena (v.) **
Basic Heart Histology
Muscular pump
Composes of 4 chambers, 2 receiving and 2 pumping, that distributes blood to 2 vascular circuits
Structure of Heart Wall
Composed of three layers:
Endocardium: Inner lining, varies in thickness.
Myocardium: Thickest layer, composed of cardiac muscle.
Epicardium: Outer layer, also known as visceral pericardium.
Wall thickness varies according to chamber type and workload
Atrial walls thinner than verticular walls
Right ventricle wall thinner than left ventricle wall
Main difference is the thickness of myocardium (middle layer)
Pericardial Sac
Encloses the heart, consists of an inner serous layer and an outer fibrous pericardium layer.
Separated from the heart by pericardial cavity: The pericardial cavity provides a lubricated space, allowing the heart to beat without friction against surrounding structures.
Functions:
Keeps the heart in place and prevents overexpansion.
Lubricates to reduce friction with beating.
Protects against infection and injury.
Structure:
Mesothelium: A simple squamous epithelium covers the surface facing the pericardial cavity.
Fibrous (dense) connective tissue: Comprising the outer layer,
Outermost connective tissue anchors into surrounding structures, such as the diaphragm.
Layers of heart walls
Epicardial/Visceral Pericardium (outer most layer)
Mesothelium: A simple squamous epithelium that secretes lubricating pericardial fluid, preventing friction as the heart beats.
Underlying Connective Tissue: Contains:
Adipocytes
Nerves
Coronary vessels: Arteries originating from the aorta sending branches into the myocardium.
Myocardium (Middle layer of the heart)
Thick, Middle Layer of Heart:
Composed of cardiac muscle fibers arranged in concentric layers.
Forms a figure 8 pattern around the atria and the bases of the great vessels.
Encircles the ventricles as they proceed toward the apex.
Superficial Layers:
Ventricular muscle wraps around both ventricles.
Functionality:
Muscle arrangement allows the heart to pump blood more effectively.
Vascular Connective Tissue:
Present between muscle fibers.
Contains loose connective tissue.
Endomysium: Surrounds muscle fibers.
Abundant Blood Capillaries: Supports high oxygen demand to sustain the beating of the heart.
Contains nerves.
Endocardium (Internal lining of the heart)
Internal Lining of All Heart Chambers:
Varies in thickness in different areas (thickest in atria, thinnest in ventricles).
3 Sublayers:
Endothelium: In contact with blood.
Subendothelial Connective Tissue Layer: Dense, regularly arranged collagen and elastin fibers.
Deep Connective Tissue Layer: More irregular and looser arrangement of collagen.
Purkinje Fibers: May be present within this layer.
Cardiac muscle
Striated: Distinct striped appearance due to organized sarcomeres.
Branched Fibers: Fibers branch and connect with adjacent fibers.
Central Nuclei: Each cardiac muscle cell has one or two central nuclei.
Direct Cell-to-Cell Communication: Communicates directly via intercalated discs, allowing synchronized contractions.
Abundant Mitochondria: Makes up about 25% of the cell volume, supporting high energy needs.
Large Energy Stores: Contains significant glycogen stores for energy reserves.
High Oxygen Demands: Relies primarily on aerobic respiration for energy.
Largest Diameter Fibers: Present in the left ventricle where workload is greatest.
Purkinje Fibers
Modified Cardiac Muscle Cells:
Specialized fibers for rapid transmission of signals.
Allow for coordinated, unified contraction of heart muscle.
Larger cells, paler staining than contractile cardiac muscle cells due to fewer myofibrils.
Contain large stores of glycogen.