Physiology
7.1, 7.2, 7.3 - Human Energy Systems
Nutrients
chemical substances obtained from food
used by the body for processes
bodies need to supply energy, regulate cellular activities
Three key energy nutrients
carbohydrates
primary energy source
necessary for those who are very physically active
provides materials to build cell membranes and to provide energy used by cells
broken down into glucose
stored as glycogen in liver and skeletal muscle
ex. of carbs include sugars and starches
lipids (fats)
most energy dense nutrient - most energy per gram - 9kcal/g
go-to energy source for long periods of low-moderate intensity activities
stored in body as adipose tissue
broken down into fatty acids, which are stored as triglycerides
protein
only used when other energy stores are emptied out - starvation
20 amino acids that are building blocks for protein
9 are essential - must be obtained from food
4kcal
no protein energy reserves in body
protein exists as body tissues
ATP - adenosine triphosphate
obtained from food
broken down from glucose
energy is released during hydrolysis of ATP, which is used to fuel cellular processes
ATP → ADP + P + Energy
Two energy systems
anaerobic system
occurs without oxygen
happens quickly in muscle fibres
high intensity - breathing heavily at the end of exercise
aerobic system
does require oxygen
leads to the complete breakdown of glucose
can’t generate ATP quickly, but produces a lot of ATP
able to get in enough oxygen for the activity you’re doing
Three metabolic pathways
ATP-PC (anaerobic alactic)
does not use glucose
alactic = no build up of lactic acid
used for activities that require high amounts of energy for short amount of time (10 seconds or under)
ex. shotput, weightlifting, 100 m sprint
allows for quick, intense muscle contraction
ATP fuels activity for about 2 seconds
ATP is produced from phosphocreatine - small amounts stored in muscle, readily available
PC → P + C + Energy
Energy is used to resynthesize ATP
PC + ADP → ATP + Creatine
after 10 seconds, no more PC in muscles - about 2-5 minutes to recover PC
Glycolysis (anaerobic lactic)
when all of PC is used up, body uses this system
allows for longer bursts of energy - 10s - 2 minutes
partial breakdown of glucose yields 2 ATP molecules and pyruvic acid, which is converted into lactic acid in the absence of oxygen
too much lactic acid builds up around 2 minute mark - muscle shuts down
Lactic acid threshold - lactic acid build up is more than your body can remove - muscles shut down
training results in improved cardiorespiratory fitness
increased number of mitochondria, aerobic capacity, ability to clear lactic acid
untrained - 50-60% of maximum intensity
trained - 70-80% of max intensity
Cellular respiration (aerobic)
main source of energy during endurance events (2 minutes or longer)
complete breakdown of glucose produces 36 molecules of ATP - but it takes a long time to break down, which is why cellular respiration is only used for low-moderate intensity activities
occurs in the mitochondria of cells
three sub-pathways
glycolysis: break down of glucose produces 2 ATP molecules and pyruvic acid
krebs cycle: pyruvic acid does not convert into lactic acid - instead, it’s converted into acetyl CoA, which enters the krebs cycle, which takes place in mitochondria - produces hydrogen ions and 2 ATP molecules
electron transport chain: hydrogen ions enter the electron transport chain - takes place in mitochondria and yields ~ 32-34 ATP molecules
fatty acids are used during the aerobic energy system
beta oxidation is the process where fatty acids are converted into acetyl-CoA
acetyl-CoA then enters the krebs cycle
7.4 - Muscle Fiber Types and Athletic Performance
Different types of muscle fibers - every person has a different distribution of fast & slow twitch muscle fibers, different muscle fibers function differently and are more adapted to one energy system than another
Slow-twitch muscle fibers - type I fibers: slow oxidative
red or dark in colour bc of high myoglobin content
smaller
able to hold oxygen better
used in the aerobic energy system
generate small amounts of energy slowly, but a lot of muscular endurance
good for long-distance or endurance activities
Fast-twitch muscle fibers - 2 types
pale in colour
generate large amounts of force quickly
high intensity activities
uses the anaerobic energy system
type IIA: Fast-oxidative glycolytic
second fastest
used in anaerobic glycolysis system
type IIB: Fast-glycolytic
fastest contraction speed
used in anaerobic alactic system
Tonic muscle
muscles that assist with maintaining posture and stability
able to stay contracted for long periods of time
high percentage of type I fibers
Phasic muscles
good for power activities → sprinting, jumping
only used when needed/stimulated to contract
higher percentage of type IIA and IIB muscle fibers
Myoglobin
protein that stores oxygen in muscles
slow twitch muscle fibers are high in myoglobin as they require oxygen to function
fast twitch fibers have less myoglobin
Implications for training
able to change muscle fiber make up
a sprinter will benefit from doing powerful training exercises to increase the number of type II fibers
8.1 - The Structure of the Cardiovascular System
The heart
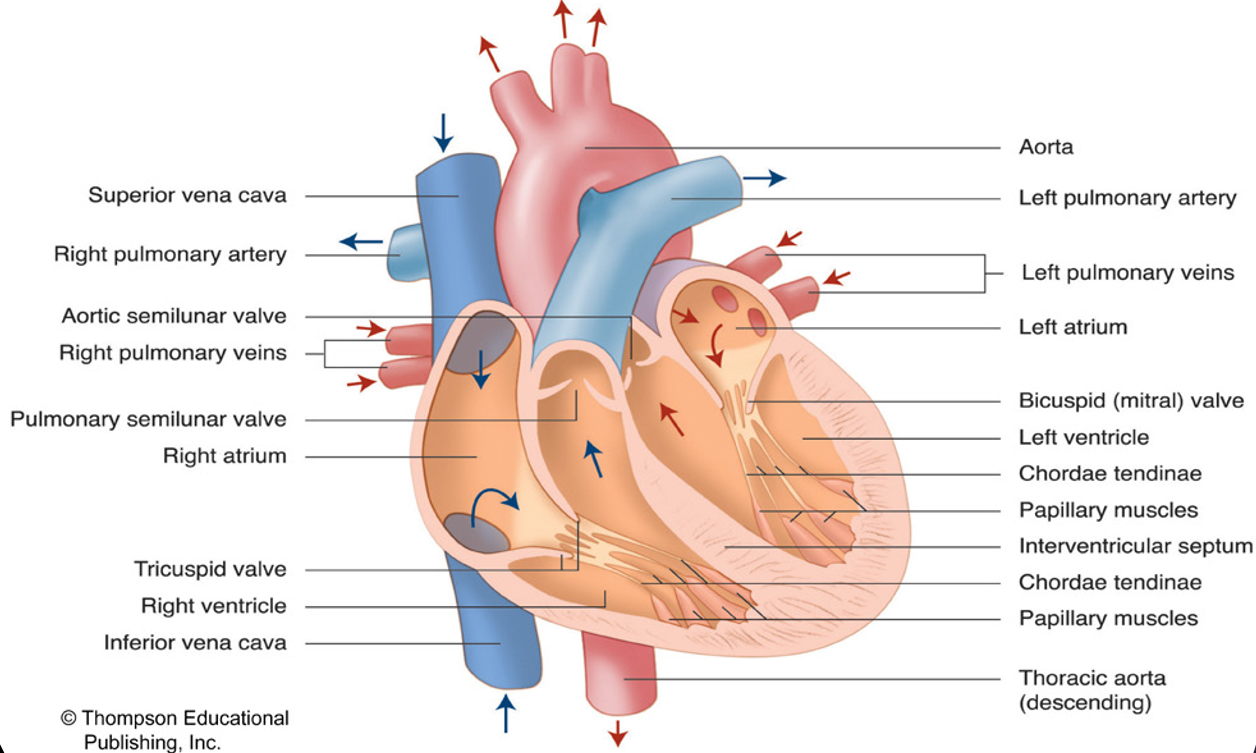
Structure of the heart
Interventricular septum
separates the heart into left and right sides
prevents oxygenated blood from mixing with deoxygenated blood
Pulmonary circulation
pumps deoxygenated blood to the lungs
Systemic circulation
pumps oxygenated blood from the lungs to the rest of the body
Pericardium
tough protective sac that fits loosely over the heart
it’s loose bc the heart needs to expand and contract
Epicardium
outer layer of heart that lies against the pericardium
Myocardium
cardiac muscle that forms the walls of the heart
lies directly under the epicardium
Endocardium
inner-most layer of heart muscle
lines the inside of the heart
Chambers of the heart
atria (sing. atrium)
upper chambers of heart
receives blood from body and pumps blood to ventricles
ventricles
lower chambers of heart
receives blood from atria and pumps blood to body
Valves
atrioventricular valves
allow blood to flow from your atria to your ventricles
attached to ventricle wall by strands of strong tissue called chordae tendinae
tricuspid valve
right side of heart
3 flaps
bicuspid valve
left side of heart
2 flaps
semilunar valves
pulmonary semilunar valve
right side valve where blood leaves ventricles
aortic semilunar valve
left side
separates aorta from left ventricle
Path of bloodflow
deoxygenated blood from your body enters the heart from the superior and inferior vena cava → enter right atrium → goes through tricuspid valve → enters right ventricle → goes out left and right pulmonary arteries → enters lungs → blood becomes oxygenated through gas exchange → blood pumped back into heart from right and left pulmonary veins → enters left atrium → goes through bicuspid valve → goes into left ventricle → goes through ascending and descending aorta and is pumped to body → gas exchange occurs in muscles and organs → deoxygenated blood travels through veins and returns to heart
Human vascular system
aorta → large arteries → medium arteries → arteriole → capillaries → venules → medium veins → large veins → vena cava
arteries
carry blood away from heart
veins
carry blood towards the heart
one-way valves prevent backflow of blood
arterioles
vessels in blood circulation that branch from arteries and lead to capillaries
surrounded by smooth muscle
regulates blood flow
contract: constricts arteriole and reduces amount of blood flow to certain area
relax: opens arteriole and increases the amount of blood flow to a certain area
arterioles that supply blood to muscles during exercise is vasodilated, increasing the blood flow to muscles
capillaries
gas exchange from blood to tissues
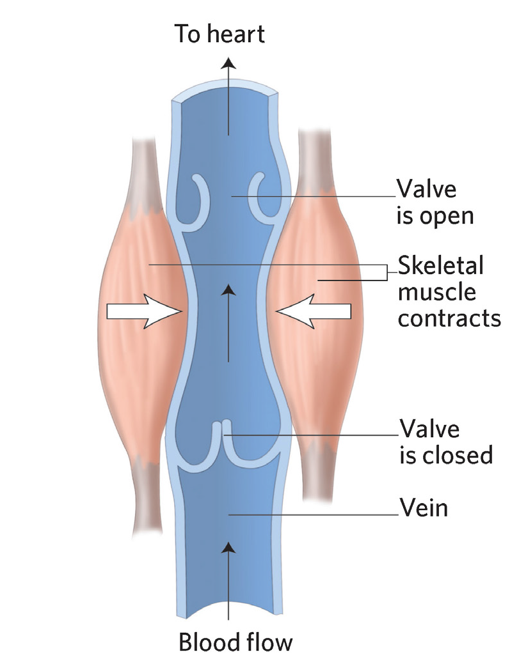
skeletal muscle pump
contraction of skeletal muscle pushes on veins, which causes blood to flow back to heart
thoracic pump
inspiration → pressure in chest cavity decreases, pressure in abdominal cavity increases
veins in abdominal cavity has high pressure and veins in chest cavity has low pressure → blood flows from the veins in abdominal to chest cavity
nervous system
venoconstriction
constricts veins to allow more blood to return to the heart
Composition of blood
plasma
makes up 55% of blood
90% water
blood cells
make up 45% of blood
red blood cells
99%
white blood cells
immune system
protects body from disease
>1%
platelets
clotting blood
>1%
Blood pressure
systolic blood pressure
max pressure observed in arteries when the ventricles contract and ejects blood to body
diastolic blood pressure
minimum pressure in arteries when ventricles relax and is filling with blood
high blood pressure → arteries and veins burst
low blood pressure → poor blood flow
8.2 - Function of cardiovascular system
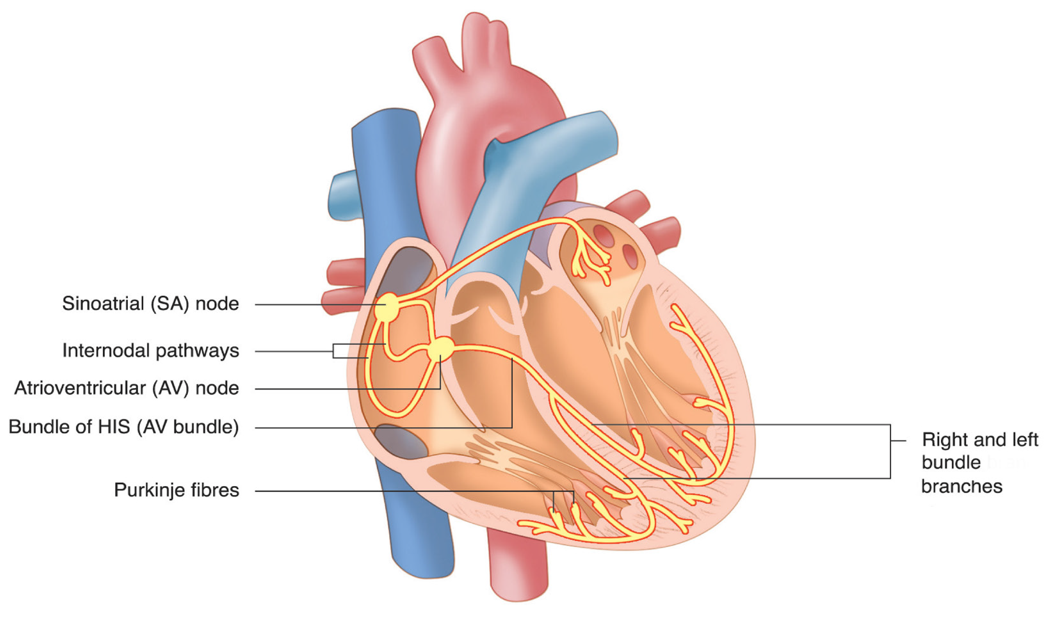
heart’s electrical conduction system
syncytium
heart with contract with an electrical stimulus
sinoatrial node
located at the entrance of the superior vena cava in the right atrium
natural pacemaker - dictates how quick or slow heart contracts
electrical impulse starts at sa nodes, stimulates atria to contract and travels to the av node
atrioventricular node
located near tricuspid valve
receives signal from sa node, then travels to the bundle of HIS, divided into the left and right bundle branches, and then to the purkinje fibers, which pass the signal to the myocardium that forms the ventricles
electrocardiogram
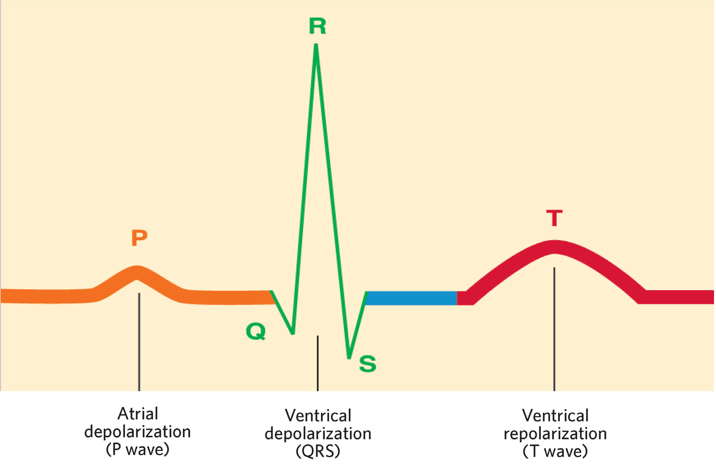
p wave
atrial depolarization (contraction)
qrs complex
atrium repolarizes (relaxes)
ventricle depolarization
t wave
ventricle repolarization
bradycardia
heart rate of 60 beats per minute or less at rest
occurs from aerobic exercises
heart gets better at pumping blood → less pumps needed
tachycardia
resting heart rate more than 100 beats per minute
cardiovascular dynamics → dramatic changes occurring in the cardiovascular system during exercise
cardiac output (q)
volume of blood pumped out of the left ventricle (blood going to body) in one minute
measured by taking stroke volume multiplied by heart rate
Q = SV(HR)
stroke volume
amount of blood per beat going out the left ventricle
LVEDV (left ventricular end diastolic volume)
amount of blood in the left ventricle after contraction of left atrium
LVESV (left ventricular end systolic volume)
amount of blood remaining in left ventricle after contraction of the ventricle
SV = LVEDV - LVESV
affected by LVEDV, blood pressure in aorta, strength of the heart, amount of blood returning to heart (venous return)
at rest → 5-6 L/min
during exercise → 30 L
more blood being pumped out
most of blood being redirected to working muscles
Venous return
venoconstriction
skeletal muscle pump
thoracic pump
nervous stimulation of heart
increase in the force of contraction of the heart increases SV
heart diseases
coronary circulation
system of vessels that supply essential materials via blood to the heart muscle
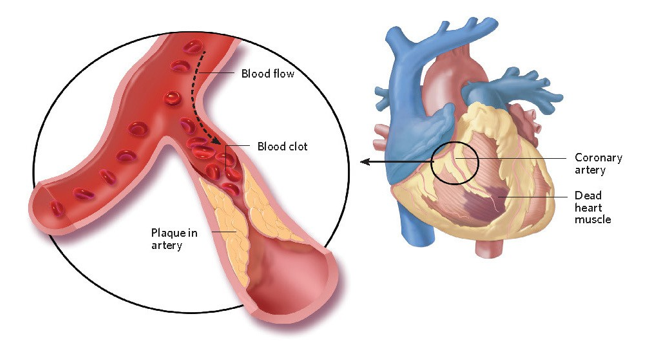
myocardial infarction (heart attack)
blood flow to section of heart becomes blocked due to plaque buildup
part of heart is not getting enough oxygen
coronary artery disease (atherosclerosis)
plaque build up
accumulation of hard deposits of cholesterol in blood vessels
causes
poor diet
smoking
elevated blood lipids
hypertension
family history
lack of physical activity
8.3 - respiratory system
Function of the respiratory system
supply oxygen to blood
remove co2 from blood
regulate blood pH level
respiration
external respiration
occurs in lungs
exchange of o2 and co2
internal respiration
exchange of gasses at the tissue level
o2 is delivered and co2 is removed
cellular respiration
process in which the cells use o2 to generate energy in the mitochondria
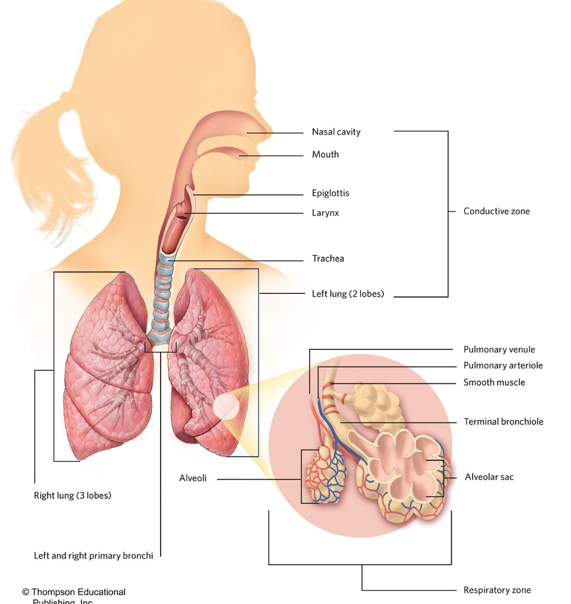
structure of the respiratory system
conductive zone
structures that transport filtered air to the lungs
includes the mouth, nasal cavity, pharynx, larynx, trachea, primary and secondary bronchi, and tertiary bronchioles and terminal bronchioles
humidifies the air, filters air
respiratory zone
gas exchange between inspired air and blood
includes the bronchioles, alveolar ducts, alveolar sacs
alveoli has large surface area and moisture ideal for gas exchange
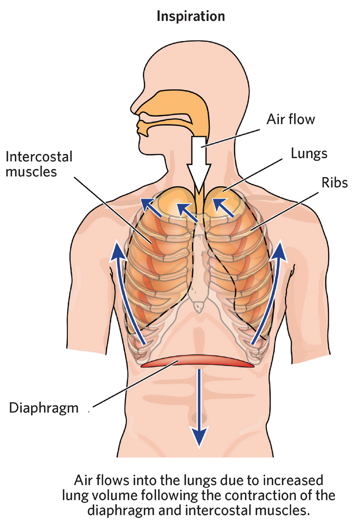
mechanics of breathing
inspiration
active process
requires contraction of respiratory muscles
diaphragm and intercostal muscles contract, causing air to flow in
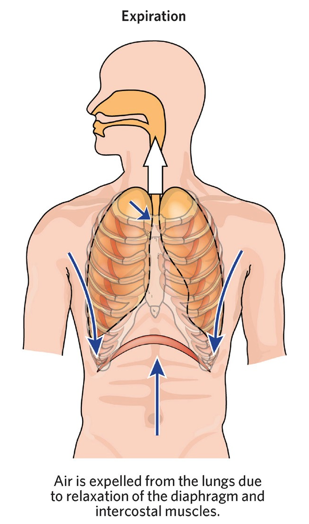
expiration
passive → does not require much energy
active → forced breathing during exercise requires the contraction of muscles in thoracic cavity and abdominal wall
diaphragm and intercostal muscles relaxes, causing air to go out
control of ventilation
stimulation from CNS conducts the contraction of muscles
breathing depends on overall need of o2, metabolic processes, muscle activity, and production of co2
gas exchange
alveoli are surrounded by capillaries
walls of each capillary are one cell thick, making gas exchange easy
diffusion mediates gas exchange
movement of gas, liquid or solid from a region of high concentration to a region of low concentration
only occurs if there is a difference in concentration, called a concentration gradient
factors that affect diffusion
size of concentration gradient (ratio of oxygen to co2)
bigger concentration gradient = faster diffusion rate
thickness of membrane
thinner = easier diffusion
surface area between the 2 areas where diffusion occurs
more surface area = faster bc more space for gas exchange to occur
oxygen transport
process by which o2 is absorbed in the lungs and carried throughout body
binds to hemoglobin
carbon dioxide transport
process by which co2 in blood is moved into the alveoli and then exhaled from the body
dissolves in plasma
binds to hemoglobin
bicarbonate system
a-vO2: arteriovenous oxygen difference
difference between amount of oxygen in arteries and veins
reflects amount of oxygen delivered to the muscle
8.4 - functioning of the respiratory system
respiratory dynamics
pulmonary ventilation (VE) - breathing
exchange of air between the lungs and the environment
depends on the intensity of work being done
3 phases
rapid on phase
very rapid increase in rate to match onset of activity
slower exponential increase
levelling off at a new steady state level
body has had enough time to catch up to the demands of oxygen
tidal volume
normal volume of air displaced during breathing
respiratory frequency
number of breaths taken per minute
external respiration
total gas exchange at lungs
factors that increase external respiration
increase in breathing
increase in blood flow to lungs
internal respiration
exchange of gasses at the tissue level
factors that increase internal respiration
increase in o2 concentration gradient
increase in concentration of co2
decrease in pH level
increase in temperature
warm → increase in gas movement
bohr shift
results from unloading o2 when theres an increase in co2 production
during exercise
increase in o2 demands for cellular respiration in skeletal muscle
greater difference between o2 in blood and muscle → greater gradient → increases diffusion from blood to muscle
increase in muscle activity
causes an increase in co2 which decreases pH, increases lactic acid, and increases temperature
decreases bond between o2 and hemoglobin, resulting in oxygen unbinding from hemoglobin and going into muscle
respiratory diseases
asthma
disease characterized by spasm of the smooth muscles that line the respiratory system, over secretion of mucous, and swelling of the cells lining the respiratory tract
can be controlled through the use of medication
COPD - chronic obstructive pulmonary disease
general term that describes a group of diseases that lead to a dramatic decrease in air flow
experience shortness of breath when doing normal activities
vo2max
maximum rate at which oxygen can be used during sustained, intense physical activity
max volume of oxygen in mL that the body can use in one minute per kilogram of body weight while breathing air at sea level
tells how efficient oxygen is being delivered → measures aerobic fitness
limiting factors
respiratory system
inadequate ventilation
oxygen diffusion limitations
cardiovascular system
inadequate blood flow, cardiac output, or inadequate oxygen-carrying capacity (hemoglobin concentration)
working muscle
lack of mitochondria
vo2
volume of oxygen consumed
proportional to the amount of work being done
more work = higher vo2
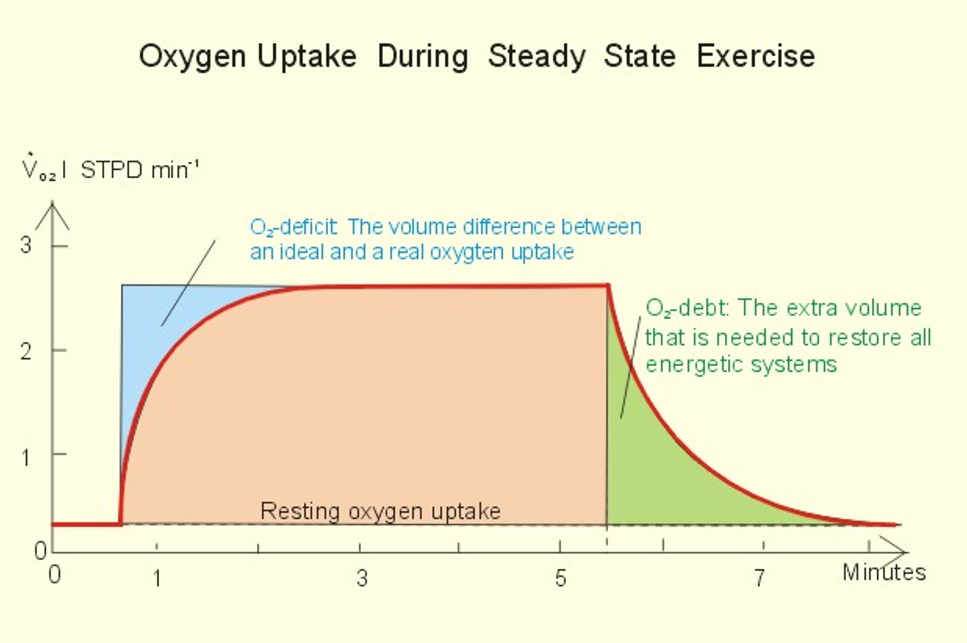
o2 deficit
build-up to get to steady state
difference between oxygen required to perform a task and the oxygen actually consumed prior to reaching a new steady state
diff between oxygen we need and oxygen we have
trained individuals reach the steady-state quicker → smaller oxygen deficit
ventilatory threshold
state which ventilation increases more rapidly than workload
breathing harder than work demands
lactate threshold
blood lactate concentration begins to rise
onset of blood lactate accumulation
when lactate levels begin to accumulate rapidly
oxygen uptake during steady state exercise graph
first 10 seconds
o2 requirement is low bc our body is using ATP PC system
10 seconds to 2 minutes
o2 levels go up
steady state
oxygen we have is matched by the oxygen we need
oxygen debt
breathing hard
replenishing oxygen that was used up