Module 7: Cardiophysiology
there are two types of heart cells:
autorhythmic- self-stimulating, non-contractile cells
Na+ and Ca2+ depolarize
K+ repolarizes
no resting potential
contains the mainly the SA node and some of the AV node
contractile-
Na+ depolarizes
K+ repolarizes
Ca2+ acts as a second messenger
autorhythmic cells
phase 1.) the unstable membrane potential is activated by ion channels and initiate pacemaker potential
Na+ and Ca++ depolarize
K+ repolarize
Na+ first, Ca++ later
no resting potential
phase 2.) voltage gated Ca2+ channels open at threshold
Ca++ is being used for depolarization
AP rises
phase 3.) K+ leak and repolarization occurs when during an increased outflow of K+ and Ca2+ decrease
phase 4.) K+ channels close and AP drifts towards threshold
phase 5.) hyperpolarization = pacemaker potential returns to lowest point
conduction system - autorhythmic cells are organized into nodes and pathways
intercalculated disks- connections between cells (both types)
desmosomes hold all cells together
gap junctions allow for AP flow between cells triggering depolarization to spread across the heart
SA node- “pacemaker” of the heart because the rate of depolarization is the fastest
AV node- AV node delay
AV bundle (bundle of HIS)- carries signal to interventricular septum through non-conductive tissue that separates atria from ventricles
bundle branches (left and right) - carries signal to interventricular septum through non-conductive tissue that separates atria from ventricles
conduction pathways (purkinje fibers) - spreads signal out from the apex of the heart
contractile cells

AP involves voltage gated Na+ and K+ channels
Ca++ acts as a second messenger
initiated and stimulated by influx of ions through gap junctions, not neural stimulation
phase 0.) rapid depolarization caused by voltage-gated Na+ channels
phase 1.)
early repolarization
faster opening of K+ channels cause repolarization
phase 2.)
plateau
Ca2+ influx delays repolarization
efflux of K+ leads to plateau making AP and refractory period last longer and nearer to 0 charge
phase 3.)
rapid repolarization caused by slow opening of K+ channels
phase 4.) resting potential
increased cardiac output (sympathetic)
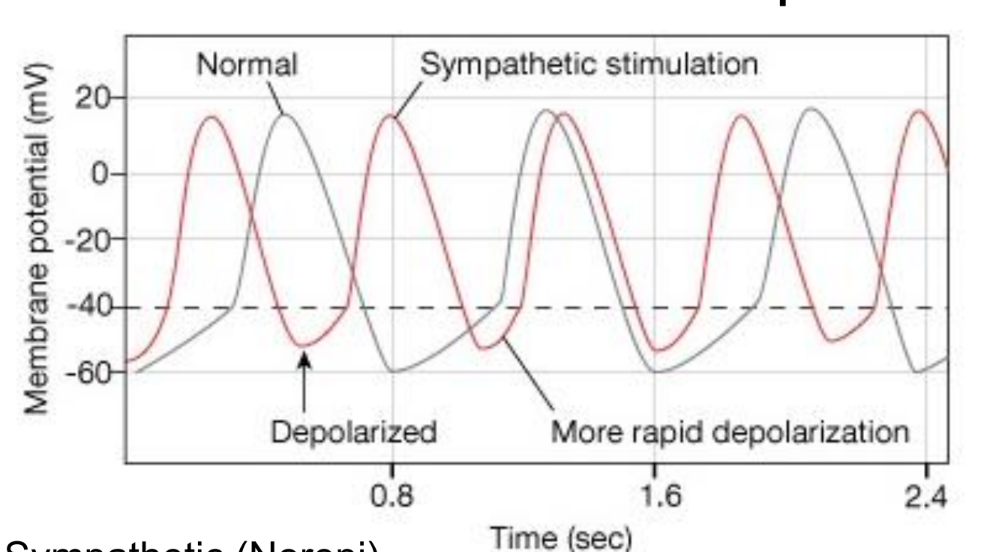
increase in Na+ and Ca2+ permeability
decrease in K+ permeability
decreases AV node delay; less delay
increased depolarization
decreased cardiac output (parasympathetic)
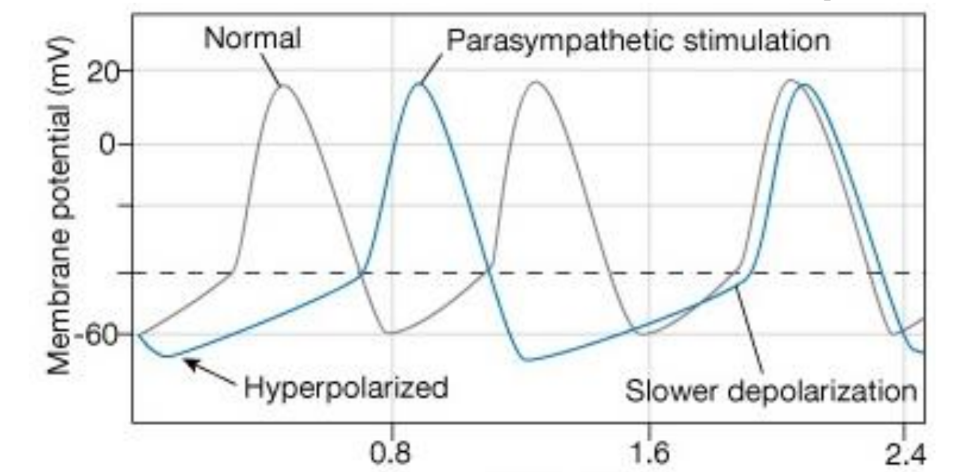
K+ permeability increases
Ca2+ permeability decreases
increases hyperpolarization
increases AV node delay
shortens AP in atria
EKG
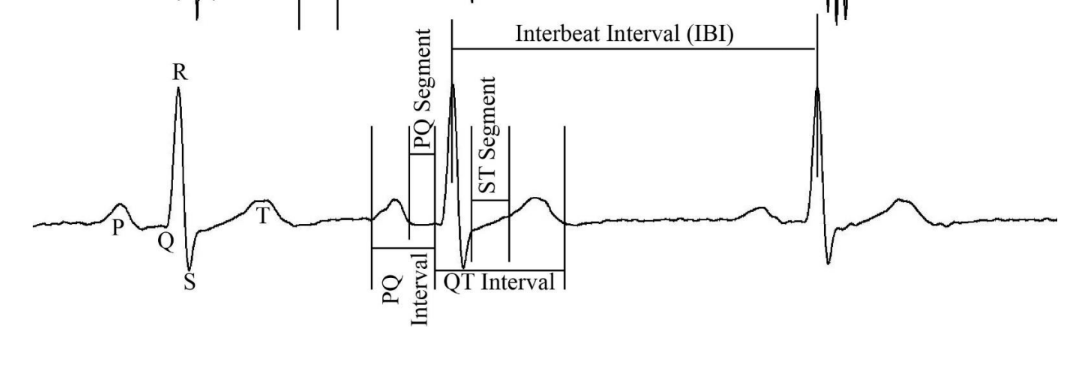
QRS complex
Q wave- initial depolarization interventricular septum
R wave- depolarization from interventricular septum to apex
S wave- depolarization from apex to ventricular myocardium (lub)
T wave- repolarization of ventricles leading to ventricular diastole (dub)
Intervals and segments – named sections of EKG trace
Segment – space between two waves, not including a wave
Interval – includes one or more waves
Interbeat Interval (IBI) - Time between beats, one complete cycle, usually R wave to R wave
P-R Interval (or P-Q Interval) - from start of P wave to start of Q wave, time for atrial depolarization
and contraction
P-R Segment (or P-Q Segment) - From end of P wave to start of Q wave (or R if Q is not easily seen),
time for atrial contraction and AV node delay
S-T Segment – From end of S wave to start of T wave
Q-T Interval - From start of Q wave to end of T wave, time for ventricular depolarization, contraction, and repolarization cycle