MUSCLE PHYSIOLOGY
3 types of muscles
Skeletal muscle
Multiple nuclei in a single cell
Skeletal muscle cell = muscle fiber
Cardiac muscla
Intercalated disc
Smooth muscle
Skeletal muscle
Half of the body's mass is composed of skeletal muscle
Most skeletal muscles linked to bones by tendons
Forces and movements developed during contractions are transmitted to the skeleton
Frontalis
Deltoid
Biceps
Pectoralis
Quadriceps
Tibialis
Composed of muscle fibers(cells), connective tissue, blood vessels and nerve
Muscle fibers are long and multinucleated
Striated, voluntary (conscious control)
Nuclei are peripherally located
Develop from myoblasts
Numbers remain constant
1. Connective Tissue Sheath
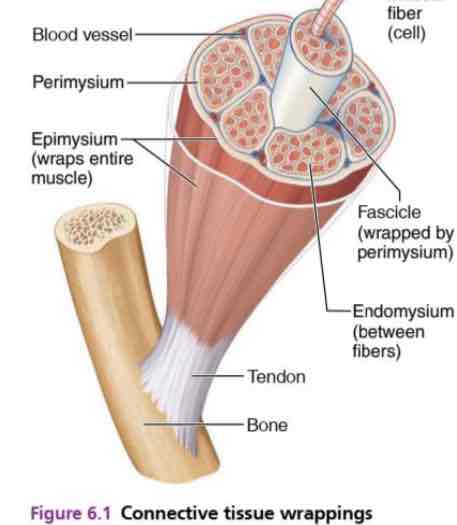
Epimysium: dense regular connective tissue surrounding entire muscle
Perimysium: collagen and elastic fibers, surrounding a fascicle (contain blood vessel and nerves)
Fascicle: a group of muscle fibers.
Endomysium: loose connective tissue surrounding individual muscle fibers.
2. Microanatomy of Skeletal Muscle
Sarcolemma: cell membrane, forms T tubules which project into cell
Myofibrils (specialized organelles): made of protein filaments. 2 main types: myosin and actin filaments
Sarcomere: contractile unit of muscle
Sarcoplasmic reticule (SR): specialized smooth ER
Stores calcium and releases it on demand
Myosin filaments
Thick filaments (16 nm)
Single filament contains roughly 300 myosin molecules
Myosin heads from cross bridges (link thick and thin filaments together during contraction)
Contain ATPase enzymes (split ATP)
Actin filaments
Has a myosin binding site (cross bridge binding site)
Tropomyosin prevent binding of myosin heads to actin when cell at rest
Troponin holds tropomyosin in place, has Ca2+ binding site
Anchored to the Z disc
Sarcomere
The smallest contractile unit of a myofibril
About 10000 sarcomere per myofibril, end to end
Composed of thick filament, thin filament and Z lines
M line: protein to which myosin attach
Z line: attachment for actin filaments
A band: dark band
I band: light band
H zone: only myosin
Cross-bridge formation
Properties of Skeletal Muscle
Excitability/responsiveness: Receive and respond to stimuli
Contractility: Ability to shorten (forcibly) when adequately stimulated
Extensibility: Muscle cells can be stretched
Elasticity: Ability to recoil and resume their resting length after being stretched
Nerve stimulus and action potential
For contraction to occur, a skeletal muscle must
Be stimulated by a motor neuron to contract
Propagate an electrical current, or action potential, along its sarcolemma
Have a rise in intracellular Ca2+ levels, the final stimulus for contraction
Motor unit – one motor neuron and all the muscle fibers it activates
One motor neuron can stimulate a few muscle cells or hundreds of them
Muscles that control fine movements have small motor units
Large weight-bearing muscles have large motor units.
Neuromuscular Junction: Region where the motor neuron stimulates the muscles
Axon of neuron branches into axon terminals
Neuromuscular junctions: contain vesicle filled with neurotransmitters
Neurotransmitter that stimulate skeletal muscle cells (acetylcholine)
Synaptic cleft: gap between axon terminal and sarcolemma of muscle cell, filled with interstitial fluid.
Troponin complex
Low cytosolic Ca2+: energized cross-bridge cannot bind to actin > relaxed muscle
High cytosolic Ca2+: cross-bridge binding sites are exposed > cross-bridge binds to actin and generates force > activated muscle
MECHANISM OF MUSCLE CONTRACTION
The sliding filament theory
Activation by nerve causes myosin heads (cross bridges) to attach to binding sites on the thin filament
Myosin heads then bind to the next site of the thin filament and pull them toward the center of the sarcomere
This continued action causes a sliding of the myosin along the actin
The result is that muscle is shortened (contracted)
Muscle response
“All or none” principle: Minimal stimulus needed to cause contraction
Force of skeletal muscle contraction can be changed by
Motor unit summation
Tetanic contraction
Length-tension relationship
Muscle force depends upon the number of fibers stimulated
More fibers contracting results in greater muscle tension
Muscles can continue to contract unless they run out energy
Graded muscle responses
Twitch: single, brief contraction. Not a normal muscle function
Tetanus (summing of contraction): One contraction is immediately followed by another
The muscle does not completely return to a resting state
The effect are added
Unfused (incomplete) tetanus: Some relaxation occurs between contractions
The results are summed
Fused (complete) tetanus: No evidence of relaxation before the following contractions.
The result is a sustained muscle contraction
Types of muscle contraction
Isotonic: Force remained constant throughout the shortening period
Isometric: muscle stays the same length during contraction
Concentric: the muscle shortens when performing an action
Eccentric: the muscle lengthens under tension
Energy for Muscle contraction
Muscle used stored ATP for energy
ATP bonds are broken to release energy
Three pathways for ATP regeneration
Direct phosphorylation of ADP by creative phosphate
Aerobic respiration
Anaerobic glycolysis and lactic acid formation
Only 25% of energy is used – rest relapsed as heat
Type of muscle fibers
Type 1: Slow oxidative (SO)
Small, contract slowly (low ATPase activity)
Use oxidative phosphorylation (aerobic)
Eg: soleus muscle in the leg
Type 2A: Fast oxidative
Medium sized, contract quickly (lots of force)
Mostly oxidative phosphorylation
Type 2B: Fast glycolytic
Large (more myofilaments), contract quickly
Use anaerobic glycolysis
Muscle fatigue and oxygen deficit
Muscle fatigue: unable to contract even with a stimulus
Common cause for muscle fatigue is oxygen debt
Oxygen deficit occurs after prolonged muscle activity, causing fatigue
Oxygen must be repaid to tissue to remove oxygen deficit
Increasing acidity (lactic acid) and lack of ATP cause the muscle contract less
Work that a muscle can do and how long without fatigue depends on blood supply
Without adequate oxygen, lactic acid accumulates and ATP supply under low which leads to fatigue
Effect of Excise on Muscles
Exercise increases muscle size, strengths and endurance
Aerobic (endurance), exercise (biking, jogging) results in stronger, more flexible muscles with greater resistance to fatigue
Makes body metabolism more efficient
Improves digestion, coordination
Resistance (isometric) exercises (weight lifting) increases muscles size and strength
Muscles and Body movements
Movement is attained due to a muscle moving an attached bone
Muscles are attached to at least two points
Origin: attachment to an immovable or less bone
Insertion: attachment to a moveable bone
Types of Ordinary Body Movements
Flexion
Decreases the angle of the joint
Brings two bones closer together
Typical of hinge joints like knee and elbow
Extension
Opposite of flexion
Increases angle between two bones
Rotation: Movement of a bone around its longitudinal axis
Common in ball and socket joints
Abduction: Movement of a limb away from the midline
Adduction
Opposite of abduction
Movement of a limb toward the midline
Circumduction
Combination of flexion, extension, abduction and adduction
Common in ball and socket joints
Smooth muscle
Key differences from skeletal muscle
No myofibrils or sarcomere (no striations)
No t-tubules
Tropomyosin does not block binding sites
No troponin but instead Calmodulin protein regulates smooth
muscle contraction
Contraction is initiated by a Ca-regulated phosphorylation of myosin
Contract in all dimensions
b. Multi-unit Smooth Muscle
Unorganized cells that contract as individual cells
Function as separate units
E.g: the iris of the eye, piloerector muscle, wall of large blood vessels.
Single-unit Smooth muscle
Form sheets of muscle
Cells are connected by gap junctions
A large number of cells respond as a single unit
Muscle fibers contract as a group
E.g: Visceral organs
Self-excitable (does not require nervous stimulation for contraction) – myogenic
Fibers become excited and contract as a single unit
Cells electrically linked by gap junctions
Contraction is slow and energy-efficient (well suited for hollow organs)
Smooth muscle contraction mechanism
Ca2+ enters mostly from ECF (voltage-gated Ca2+ channels)
Ca2 induced Ca2 released:
Ca2+ acts as second messenger, activating myosin kinase, which phosphorylates myosin
Cross bridge cycling occurs until Ca2+ no longer available ( actively pumped back to ECF and SR)
Innervation of Smooth Muscle
Innervated by autonomic nerve system
Lacks neuromuscular junctions
Innervating nerves form varicosities
Varicosities release neurotransmitters into synaptic clefts called
diffuse junctions
Smooth muscle regulation
Neurotransmitters are acetylcholine and norepinephrine
Hormones important as epinephrine and oxytocin
Neighboring cells can activates smooth contraction via gap junction
Some visceral muscle exhibits autorhythmic contractions ( spontaneous active pacemaker cell)
Tends to contract in response to sudden stretch but no to slow increase in length
Exhibits relatively constant tension: Smooth muscle tone
Norepinephrine & Epinephrine:
Depending on the type of receptors
Epinephrine bound to beta-adrenergic receptors on smooth muscle cells of the intestine causes them to relaxation
Epinephrine also binds to the alpha2-adrenergic receptor found on smooth muscle cells lining the blood vessels in the intestinal tract, skin, and kidneys causes the arteries to contraction (constriction).
Norepinephrine causes constriction of the smooth muscle in juxtaglomerular apparatus in the kidneys, leading to an inhibited flow to nephron
Nitroglycerine
Nitroglycerine is converted to NO, which relaxes blood vessels