HISTO REVISION NOTES
Nodes of Bizzozero are desmosomal junctions found between keratinocytes, especially prominent in the stratum spinosum of the epidermis. They are seen in the light miscroscope and they indicate the site of the desmosomal junctions.
The spinous cells in the stratum spinosum are called pricke cells and this is causes because of the desosomal junction found between the adjacent cell.
In the stratum granulosum, the keratinocytes contain keratohyaline granules which contains FILLAGRIN and TRICHOHYALINE.
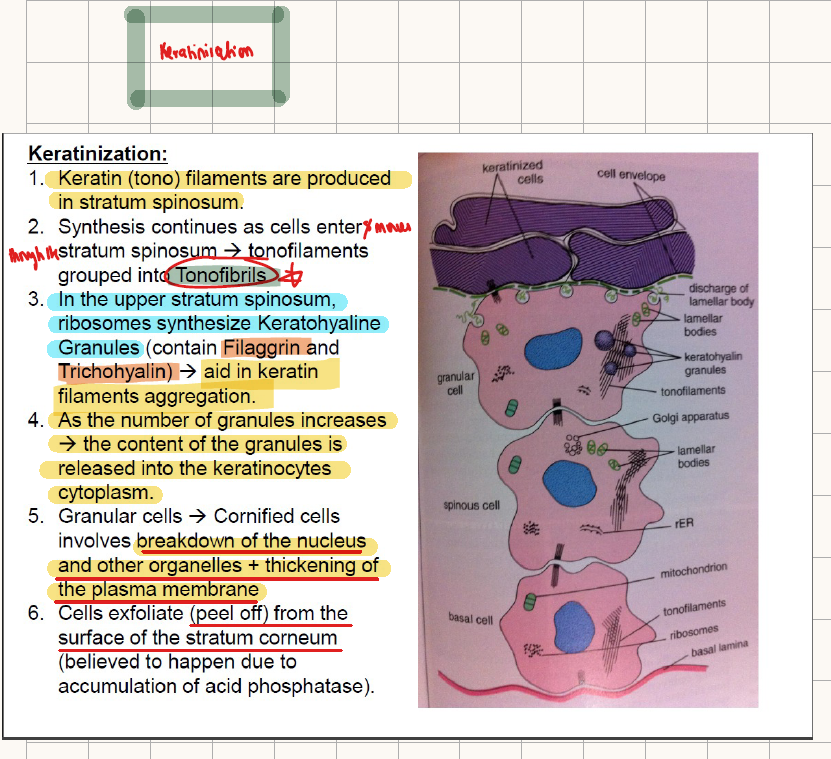
STEPS OF KERATINASATION:
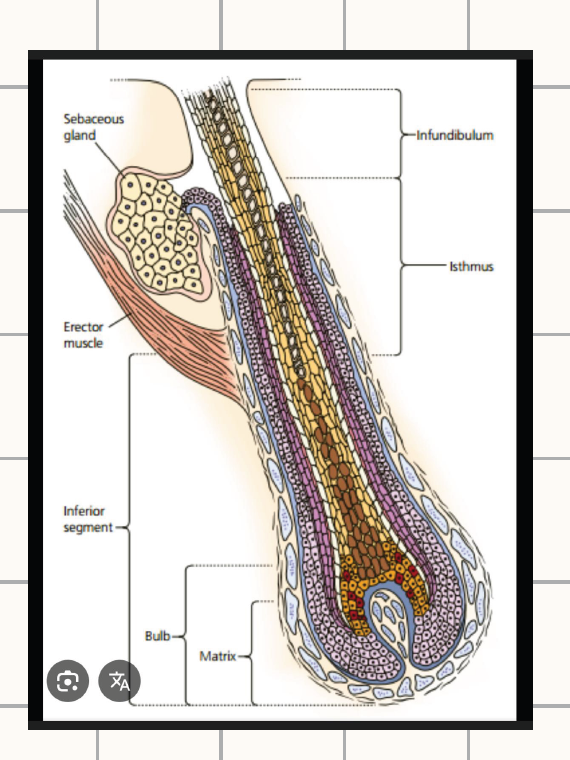
WHAT ARE THE PARTS OF THE HAIR FOLLCILE?
Infundibulum- extends from the opening of the hair follicle to the level of the sebaceous gland.
isthmus- extends from the level of the sebaceous gland to the attachment of the arrect pilli muscle.
Follicular bulge- this contains stem cells. It is a protrusion that is located close to the attachment of the arrector pilli muscle.
inferior segment- this extends from the point of attachment of the arrector pilli muscle to the base of the bulb of the hair follicle.
WHAT TYPE OF KERATIN DOES THE HAIR CONTAIN:- hard keratin
What type of keratin is found in the internal root sheath? SOFT KERATIN
WHAT ARE THE LAYERS OF THE INTERNAL ROOT SHEATH?
- Henles’ layer
-Huxley’s layer
- Internal root sheath

TAKE NOTES: The matrix cells are highly proliferating cells that produce the hair shaft and the internal root sheath
TAKE NOTE:
The basal lamina appears eosinophilic because it is rich in protein components, especially type IV collagen and glycoproteins, which bind eosin.
what are the types of secretion:
Merocrine
Apocrine
Holocrine


After holocrine secretion, the secretory cells dies and during the cells death they undergo nuclear changes such as:
Karyopyknosis: Shrinking and condensation of the nucleus.
Karyorrhexis: Fragmentation of the nucleus. Appearance: The condensed nucleus breaks into small, irregular pieces scattered in the cytoplasm.
Karolysis- Dissolution of the nucleus. Appearance: The chromatin fades away and the nucleus disappears completely due to enzymatic digestion.
TAKE NOTE: Difference between eccrine sweat gland acini and ducts
Myoepithelial cells → only in acini (secretory portion), not in ducts.
They are peripheral to the secretory epithelium, right on the basement membrane, and help with secretion
TAKE NOTE:
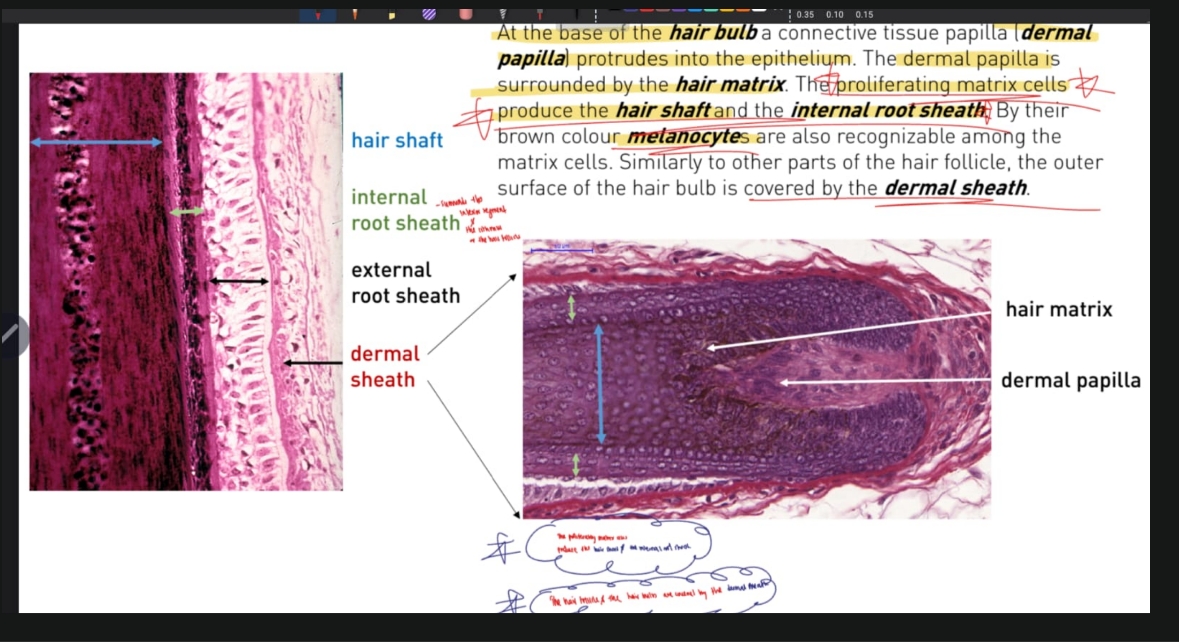
In the inferior segment and the isthmus, the hair shaft is surrounded by the internal root sheath and the external root sheath
The outer surface of the hair follicle and hair bulb is covered by DERMAL SHEATH.
NOTE:
Ruffini corpuscles are located in the reticular dermis, while Merkel discs are in the basal epidermis at the dermo-epidermal junction.
WHY STRIATED DUCTS HAVE BASAL STRIATION:
Why basal striations occur:
The epithelial cells of striated ducts have deep infoldings of the basal plasma membrane.
Numerous mitochondria are packed between these infoldings.
This arrangement creates the striped (striated) appearance seen under the microscope.
FUNCTION OF THE PRIMARY AND SECONDARY SENSORY NEURONS IN THE TASTE BUD.
Primary sensory neurons
These are the gustatory (neuroepithelial) cells within the taste bud.
Function:
Detect dissolved chemical substances (tastants).
Transduce the chemical stimulus into an electrical signal (receptor potential).
Release neurotransmitters onto sensory nerve endings.
They are not true neurons, but specialized epithelial receptor cells.
🔹 Secondary sensory neurons
These are the afferent nerve fibers of cranial nerves:
Facial nerve (VII) – anterior 2/3 of tongue
Glossopharyngeal nerve (IX) – posterior 1/3 of tongue
Vagus nerve (X) – epiglottis & pharynx
Function:
Receive signals from gustatory cells.
Conduct action potentials to the brainstem (nucleus of the solitary tract).
📌 Exam-friendly summary:
Primary sensory cell: Gustatory cell → reception & transduction
Secondary sensory neuron: Cranial nerve afferents → conduction to CNS
Nervous system:
What are schmidt lanterman clefts

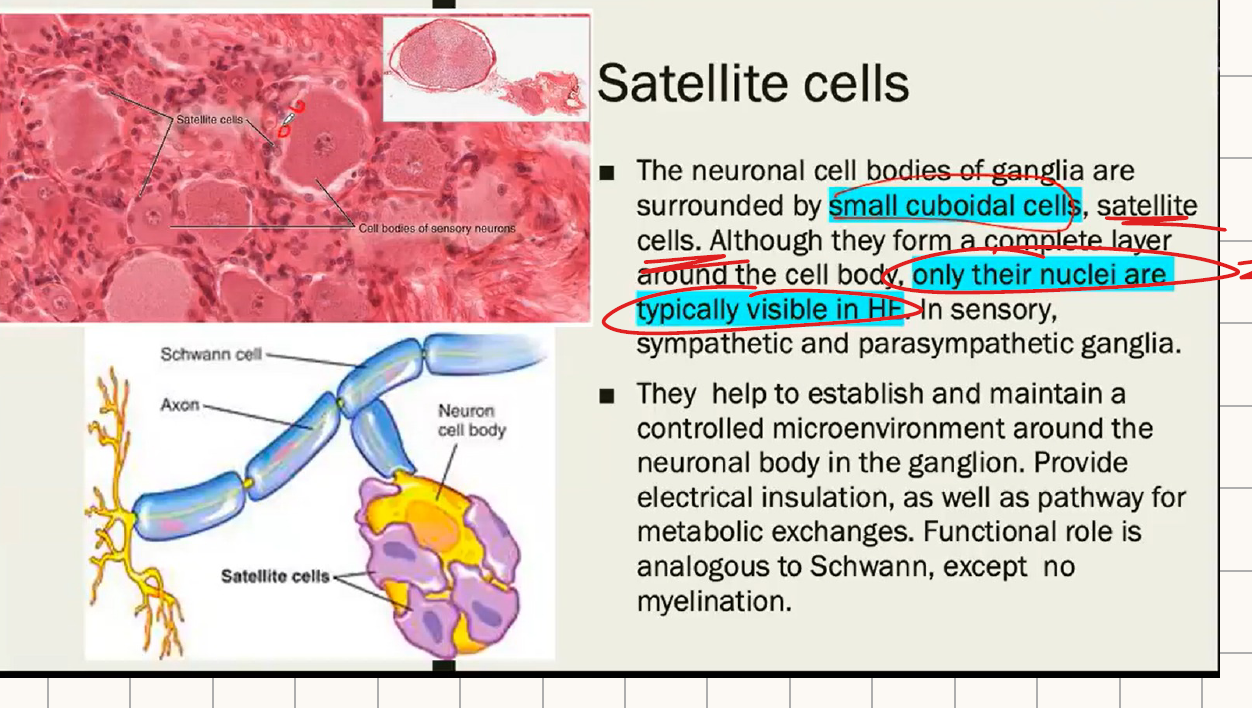
WHAT IS THE EXTERNAL AND INTERNAL GLIAL LIMITING MEMBRANE:
The glia limitans = EXTERNAL GLIA LIMITING MEMBRANE. It forms a barrier between the pia mater and the brain parenchyma.
Internal glia limitans = perivascular astrocyte layer that induces and maintains the BBB.




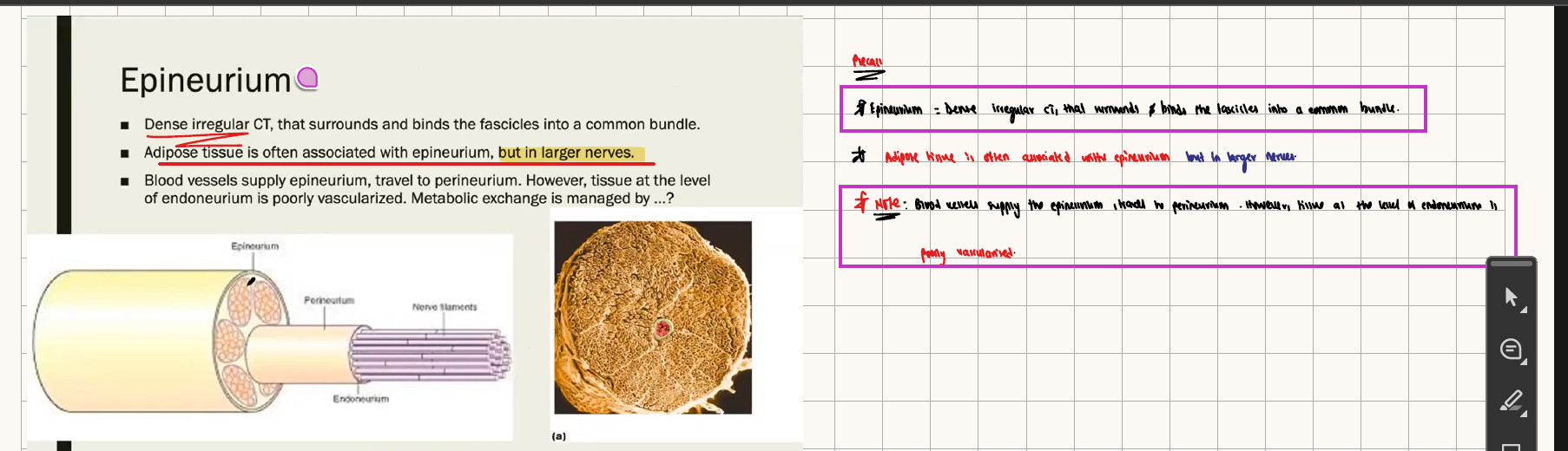
NEURO HISTO:
Spinal cord:
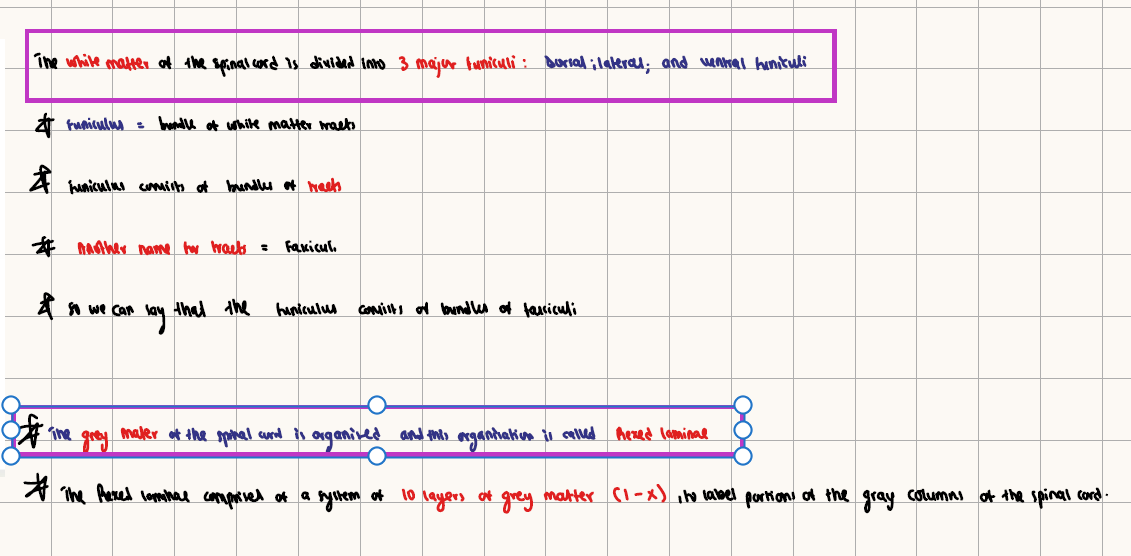
REXED LAMINAE-
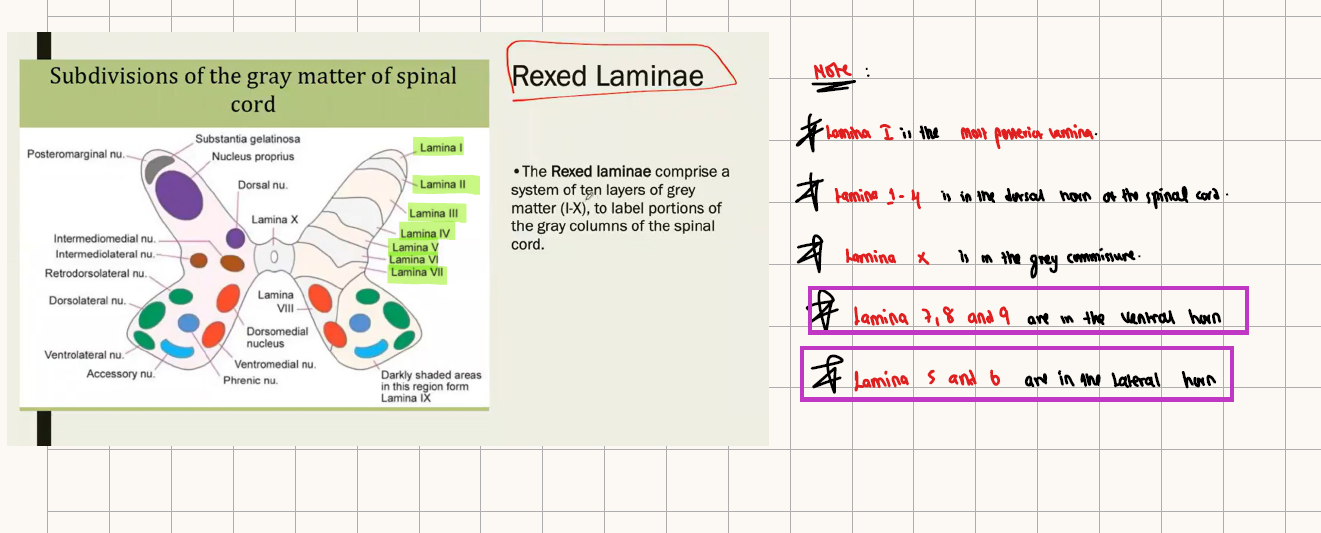
Lamina 1= Marginal zone
Lamina 2= substantia gelatinosa
Lamina 3= Nucleus proprious
Lamina 7 = contains Renshaw inhibitory interneuron cells.
Lamina 9 = contains Alpha motor neurons
What areRenshaw cells:
Location:
Rexed lamina VII of the spinal cord (intermediate zone)
Function:
Receive collateral branches from alpha motor neurons
Send glycinergic inhibitory signals back to the same alpha motor neuron and its neighbors
This process is called recurrent inhibition
Purpose:
Check and regulate alpha motor neuron activity
Prevent over-firing, which helps stabilize muscle contraction and motor output
📌 Exam tip:
Renshaw cells act as a negative feedback mechanism for alpha motor neurons, preventing excessive firing and ensuring smooth motor control.
What type of information does the following tracts carry:

WHERE DOES THE DECUSSATION IN THE CORTICOSPINAL TRACT OCCUR:

Lesion above the decussation——> contralateral deficit
Lesion below the decussation———> ipsilateral deficit
TAKE NOTE: the effect of parathyroid hormone is:
↑ Blood calcium
↓ Blood phosphate
Adrenal cortex (outer part) secretes:
Mineralocorticoids → aldosterone (zona glomerulosa)
Glucocorticoids → cortisol (zona fasciculata)
Androgens → DHEA (zona reticularis)
Adrenal medulla (inner part) secretes:
Catecholamines → epinephrine (adrenaline) and norepinephrine
Easy mnemonic
“GFR” for cortex layers:
Glomerulosa → Salt (mineralocorticoids)
Fasciculata → Sugar (glucocorticoids)
Reticularis → Sex (androgens)
📌 Exam-correct statement:
The adrenal cortex secretes mineralocorticoids and glucocorticoids, while the adrenal medulla secretes catecholamines.

TAKE NOTE:
Theca interna cells have LH (luteinizing hormone) receptors.
When LH binds, it stimulates the theca interna to:
Synthesize androgens (e.g., androstenedione, testosterone)
These androgens are the oestrogen precursors
Granulosa cells:
Have FSH receptors
Use aromatase to convert these androgens into oestrogens (estradiol).
PLACENTA:


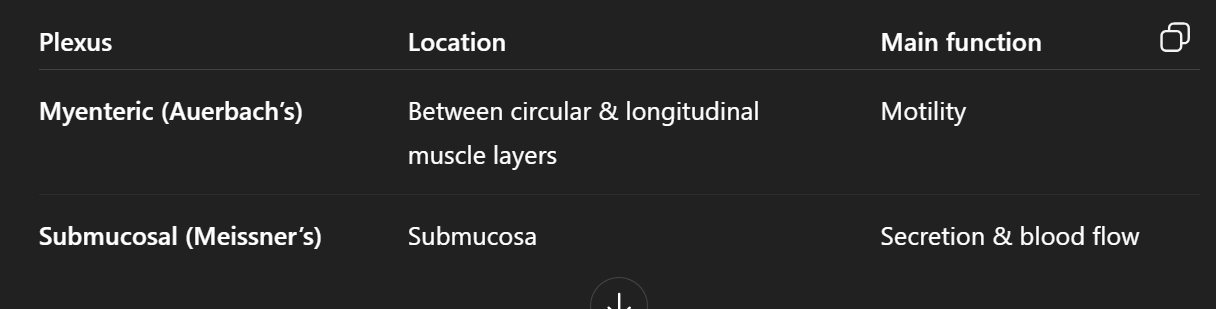
TYPES OF AUTONOMIC PLEXUS
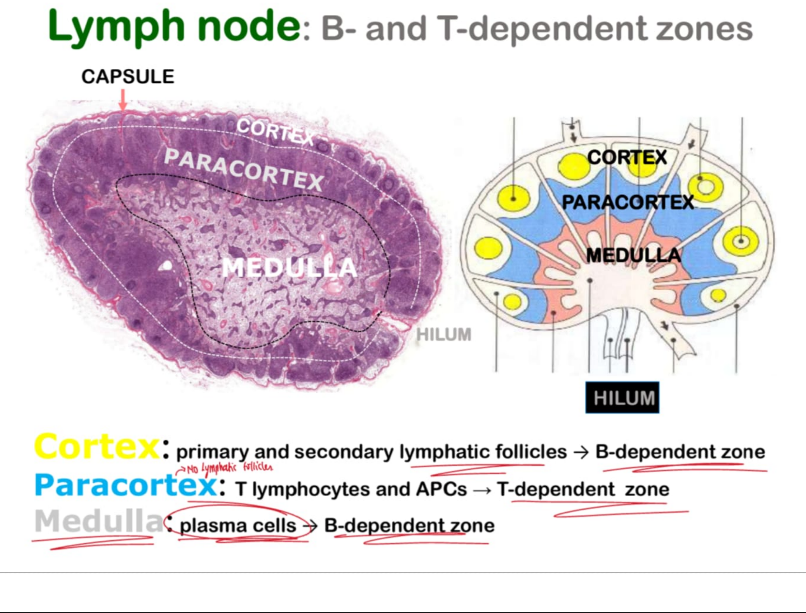
LYMPHATIC TISSUE:
QUESTION: Why is the germinative centre of the lymphatic nodule lightly stained?
Why they are pale
Vast number of large, immature B lymphocytes (centroblasts)
Dispersed euchromatin in their nuclei
Euchromatin = less densely packed DNA → allows active transcription
Stains lightly with H&E
WHAT ARE THE STEPS OF HOMING:
what h
Explanation: Lymphocyte homing
Homing is the process by which lymphocytes leave the bloodstream and enter specific tissues, especially secondary lymphoid organs. It involves several sequential steps:
1. Weak adhesion
Mediated by selectins on endothelial cells and their ligands on lymphocytes.
Causes lymphocytes to “catch” the endothelium lightly.
2. Rolling
Lymphocytes roll along the vascular endothelium due to weak interactions between selectins and their ligands.
This slows down the lymphocytes and allows them to sense chemokine signals.
3. Strong adhesion
Mediated by integrins on lymphocytes binding to ICAMs/VCAMs on endothelial cells.
Stops the rolling and anchors the lymphocyte firmly to the endothelium.
4. Extravasation (diapedesis)
Lymphocytes squeeze between endothelial cells into the tissue.
Guided by chemokine gradients to the proper compartment (e.g., T-cell zone or B-cell follicle in lymph nodes).
Quick exam line
Lymphocyte homing involves weak adhesion, rolling, strong adhesion, and extravasation, allowing lymphocytes to exit the blood and enter lymphoid tissues.
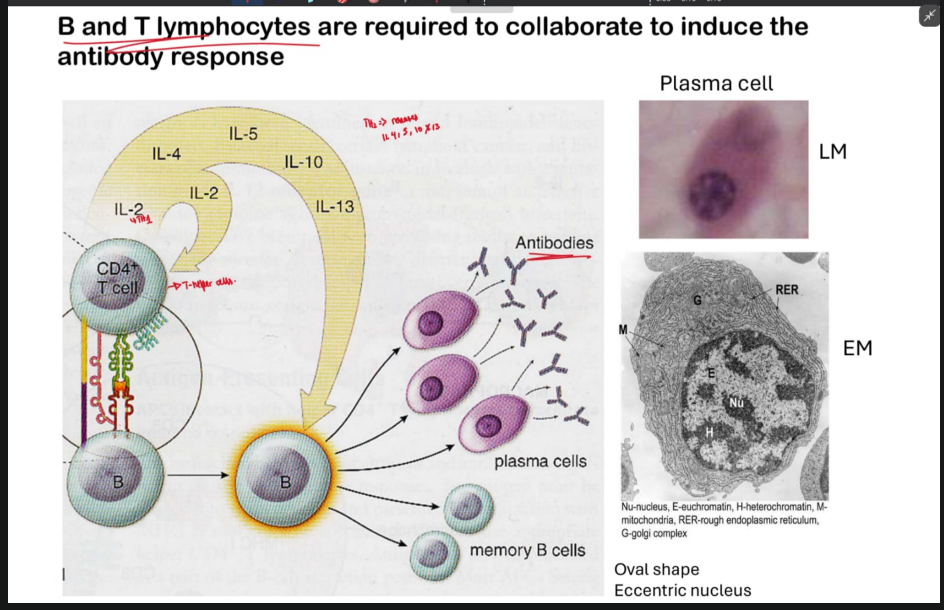
What happens when the cytokines released by the T helper cells bind to the cytokine receptor on the B cell?
When T-cell cytokines bind B-cell receptors, they activate the B cell, inducing proliferation, differentiation into plasma and memory cells. Then the plasma cells produce antibodies.
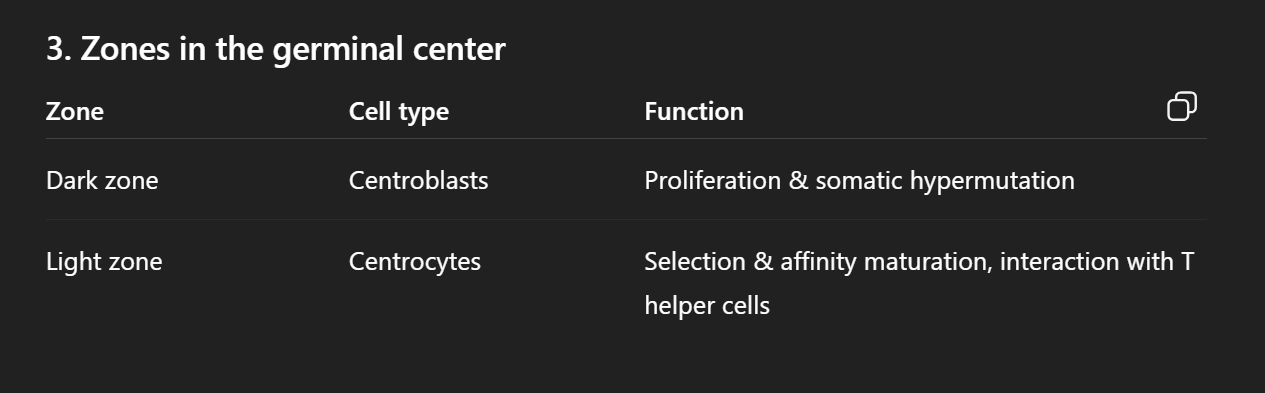
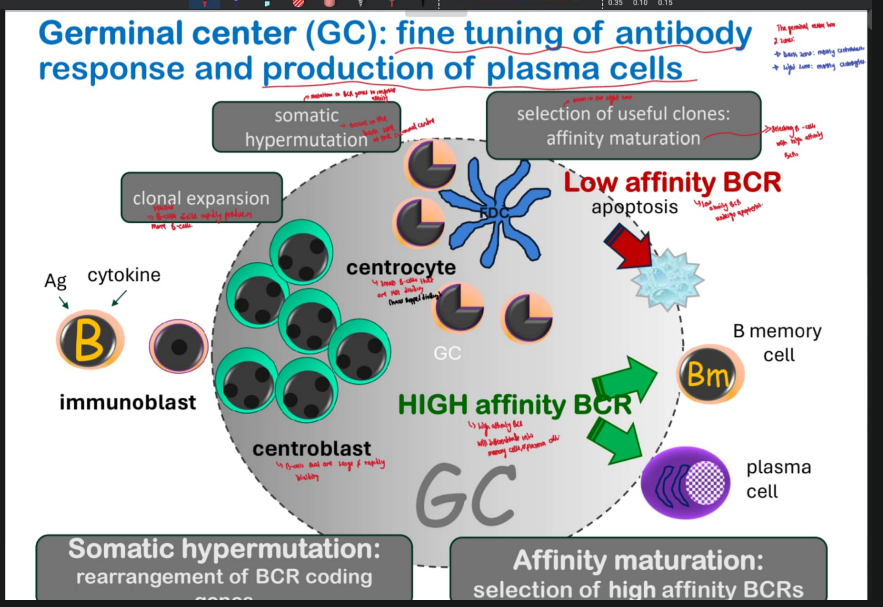
THE GERMINAL CENTRE HAS TWO ZONES:
THE MATURATION OF B CELLS OCCUR IN THE BOME MARROW
Sequence of B cell maturation- B cell maturation occurs in the bone marrow:

Steps of B cell activation, proliferation, and differentiation:

FOLLICULAR DENDRITIC CELLS:

Follicular dendritic cells (FDCs) are neither professional nor non-professional APCs.
Function:
They trap antigens in the form of immune complexes on their surface using complement receptors (CR1, CR2) and Fc receptors.
Display these intact antigens to B cells in the germinal center.
This interaction is critical for B cell selection, affinity maturation, and differentiation.
The Follicular dendritic cells (FDCs) are found in the light zone of the germinal centre.

Differences between MHC I and MHC II
MHC I normally displays self-peptides, but during infection, it presents viral or tumor peptides WHILE MHC II displays extracellular-derived antigens, not self-peptides.


What are regulatory T cells?
They are a special type of T cells whose main job is to supress the immune response and maintain tolerance
What is the function of Natural killer cells?
They are responsible for recognition and lysis of virus infected or tumour cells.
Natural killer cells have 2 major types of receptors on their surface:
Killer inhibitory receptor: these inhibit the NK cell killing. They recognise MHC class I molecules on normal cells. They bind and send a “don’t kill me” signal to the NK cell.
Killer activating receptor: They activate the NK cell killing. They recognise certain viral proteins, infected or tumour cells.
Cells of innate immunity:
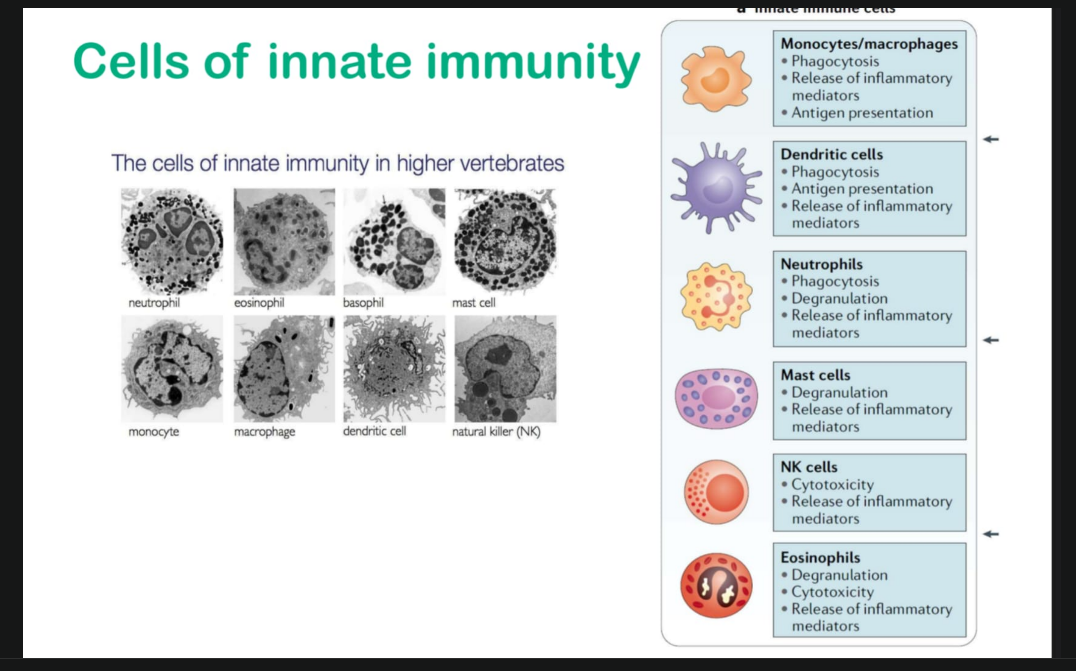
The innate immune cells:
Innate immune cells are non-specific, rapid-acting cells like neutrophils, macrophages, dendritic cells, NK cells, eosinophils, and basophils that provide the first line of defense and activate adaptive immunity.
HOW IMMUNE CELLS CAN DIFFERENTIATE BETWEEN SELF AND NON SELF CELLS:
Innate immune cells (like macrophages, dendritic cells, neutrophils) use pattern recognition receptors (PRRs) to discriminate self vs non-self.
Microorganisms like bacteria have pathogen associated molecular patterns (PAMPs) that are identified by pattern recognition receptors on macrophages.
the PRR on the macrophage/immune cell binds the PAMP.


SELF CELLS DON’T HAVE PAMP (Pathogen associated molecular patterns)
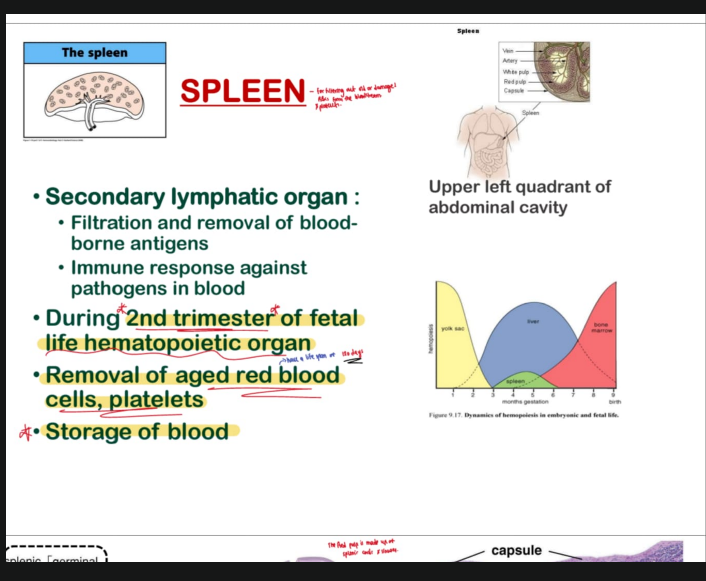
KEY NOTES OF REMEMBER ABOUT SPLEEN:
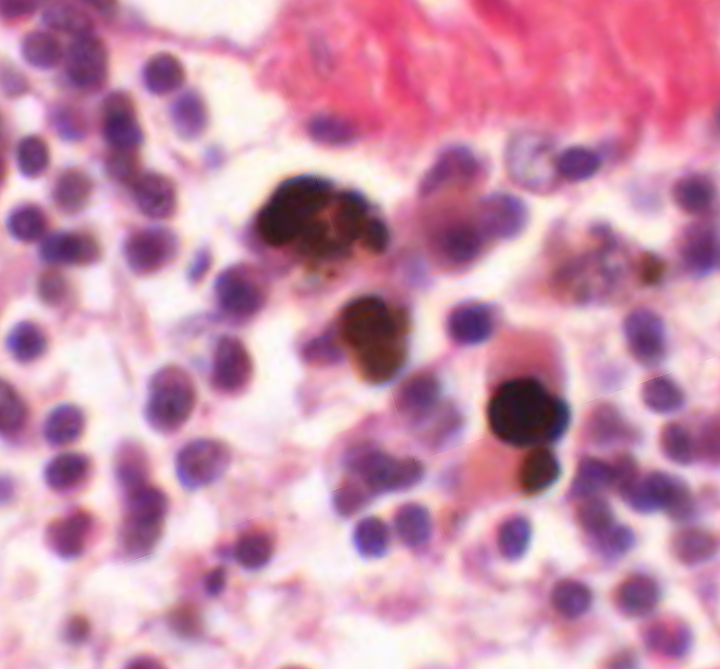
TAKE NOTE: The macrophages in the splenic cords are brown because of the iron compounds produced during degradation of phagocytosed red blood cells.
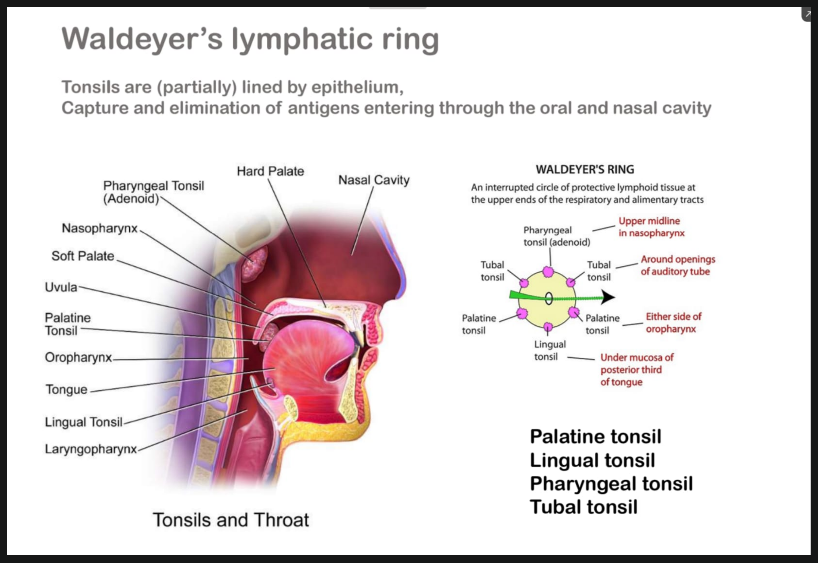
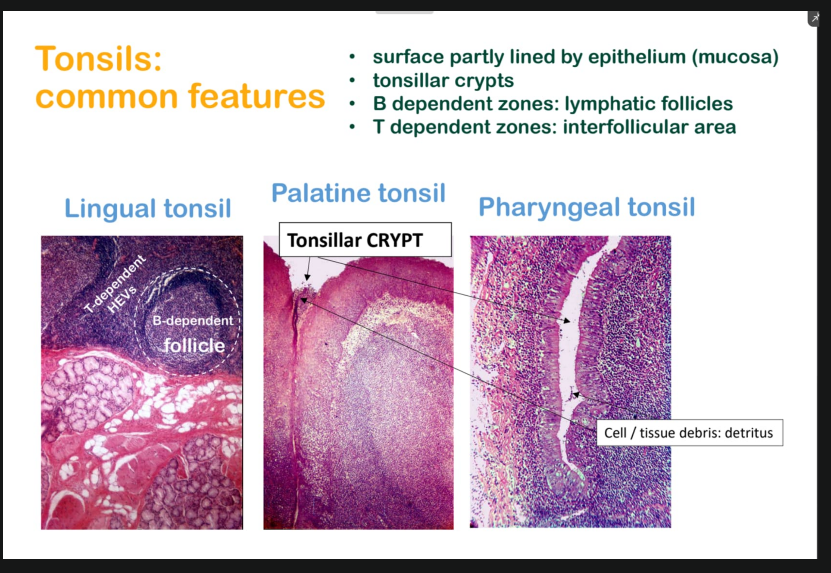
WALDEYERS RING
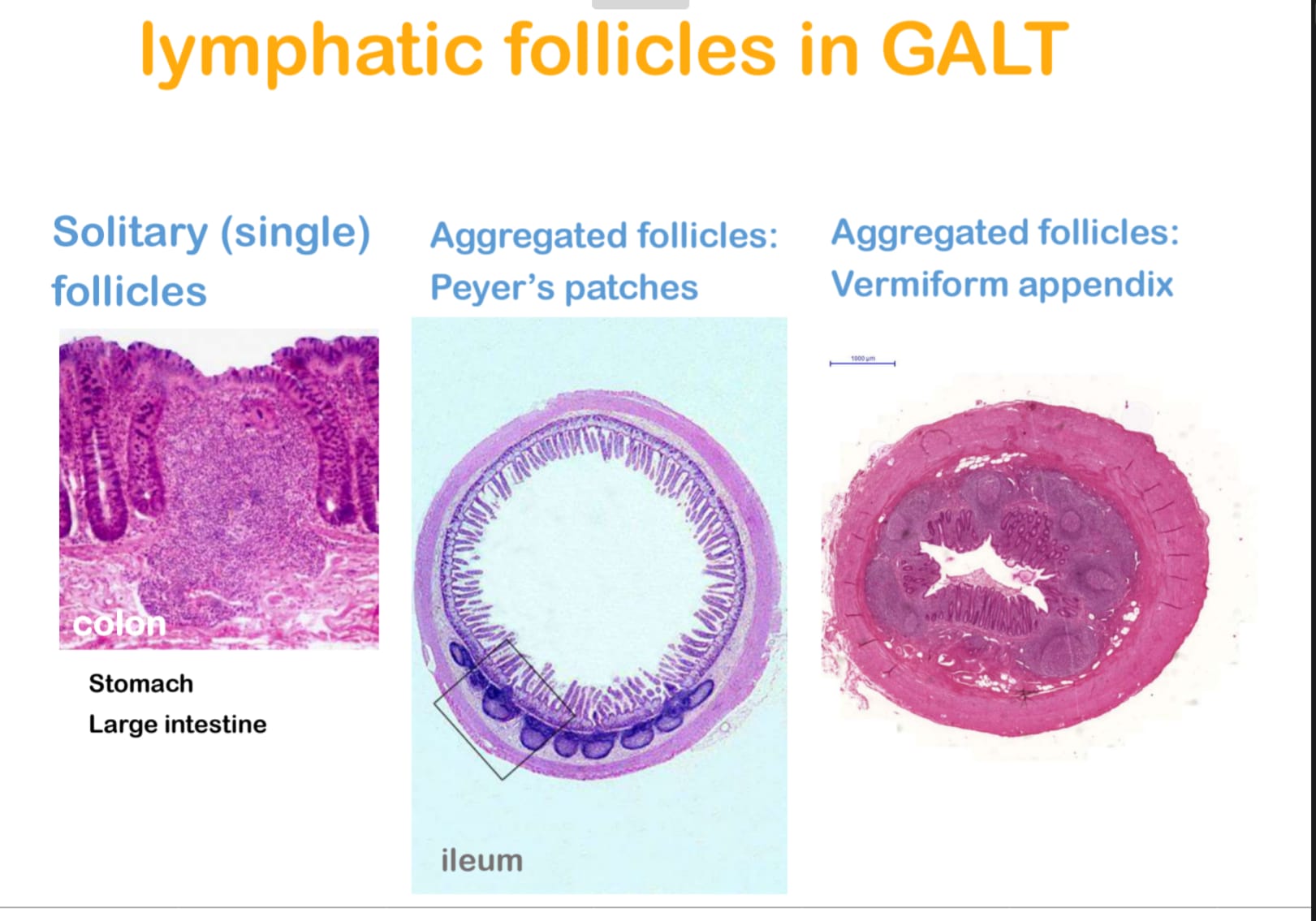
WHAT ARE MICROFOLD CELLS AND WHAT DO THEY DO?
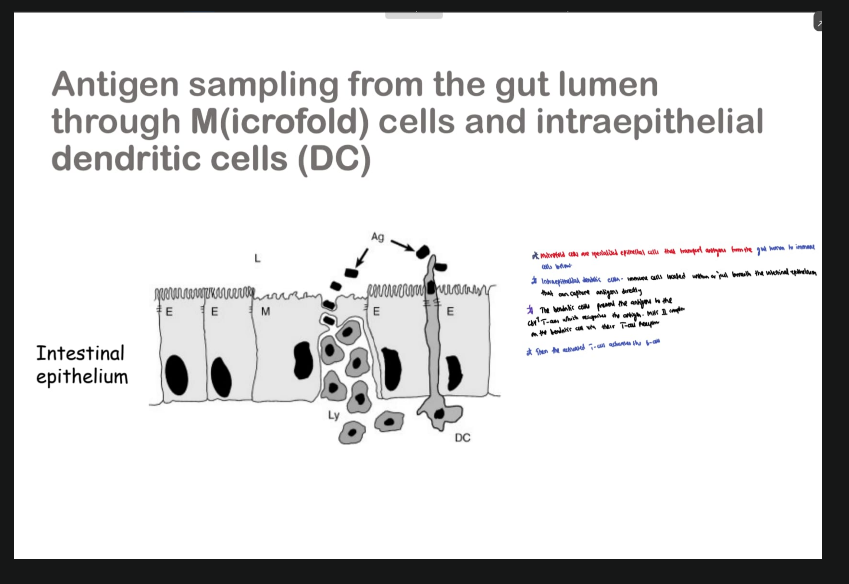
M cells take up antigens from the intestinal lumen
Antigens are passed to dendritic cells/macrophages in Peyer’s patches
Dendritic cells (professional APCs) process antigen
Antigen is presented on their MHC II to CD4⁺ T helper cells
Activated CD4⁺ T cells will activate the B cells
B cells undergo differentiation → plasma cells and memory B cells
TYPES OF MALT
GALT
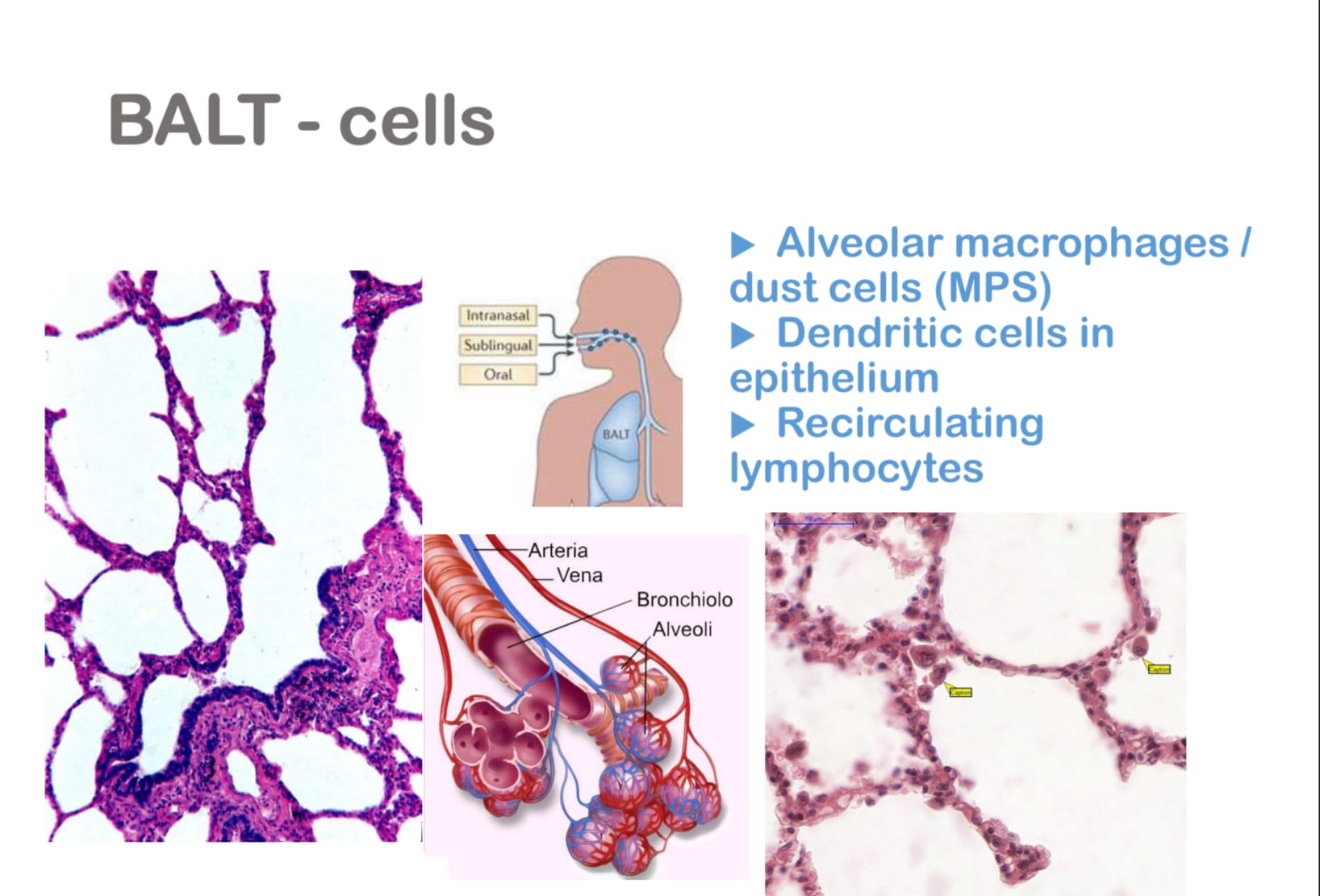
BALT
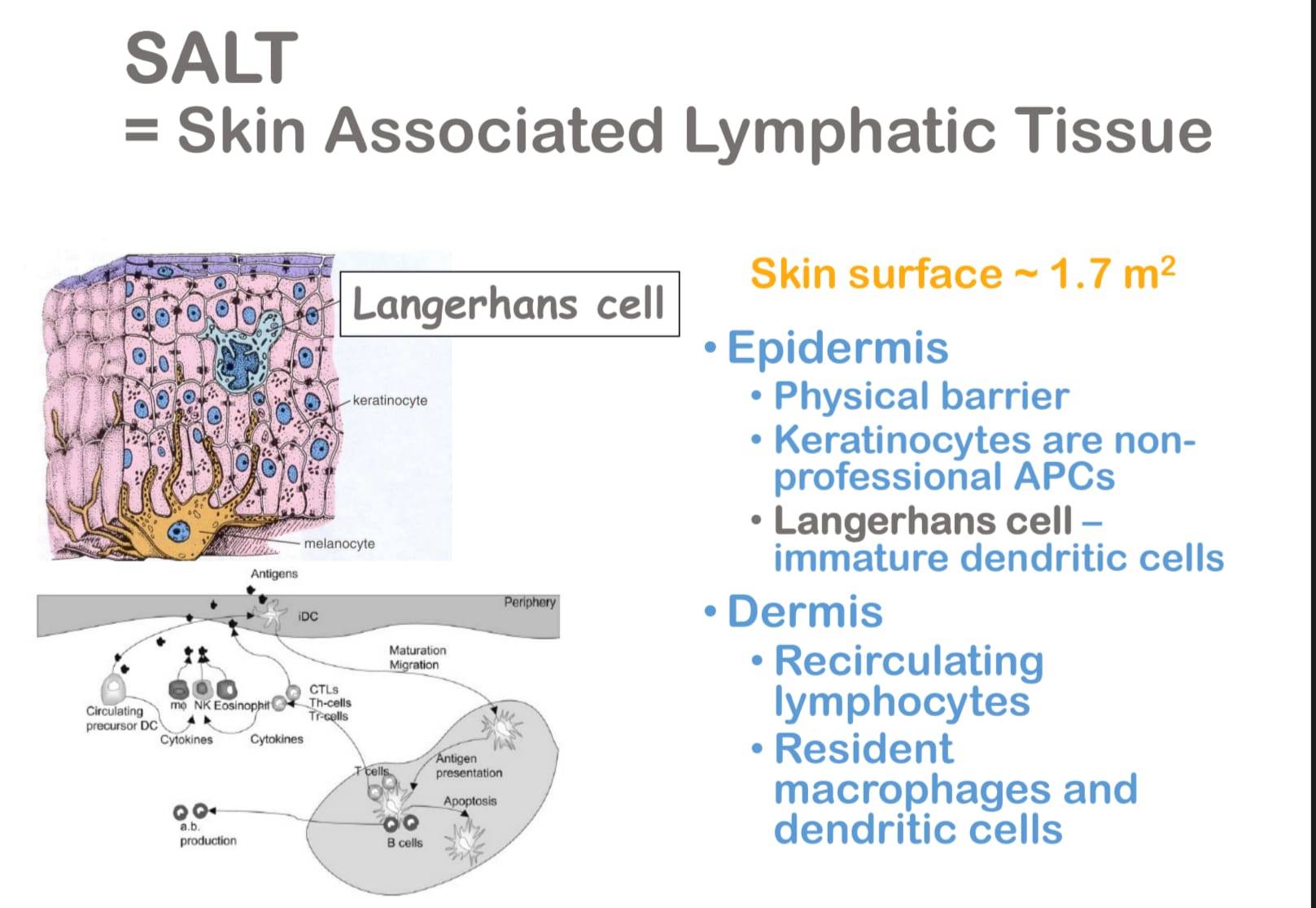
SALT
TAKE NOTE:
BALT consists of alveolar macrophages, dendritic cells, and recirculating B and T lymphocytes organized into lymphoid follicles, and functions in immune surveillance of the respiratory tract.
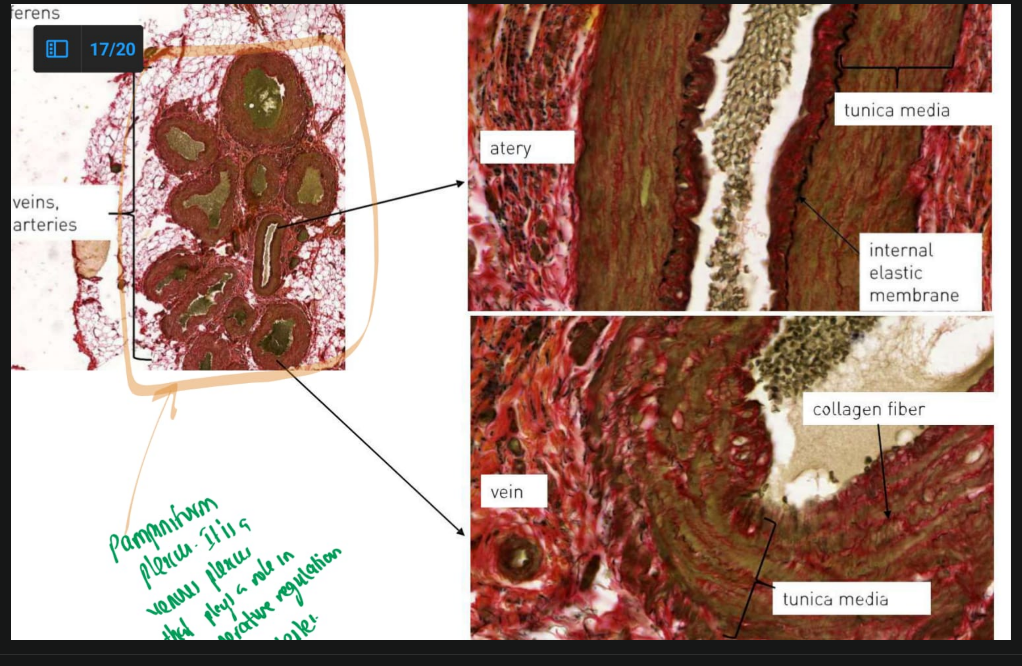
SPERMATIC CORD:

TAKE NOTE:
The testicular artery is a MUSCULAR ARTERY.
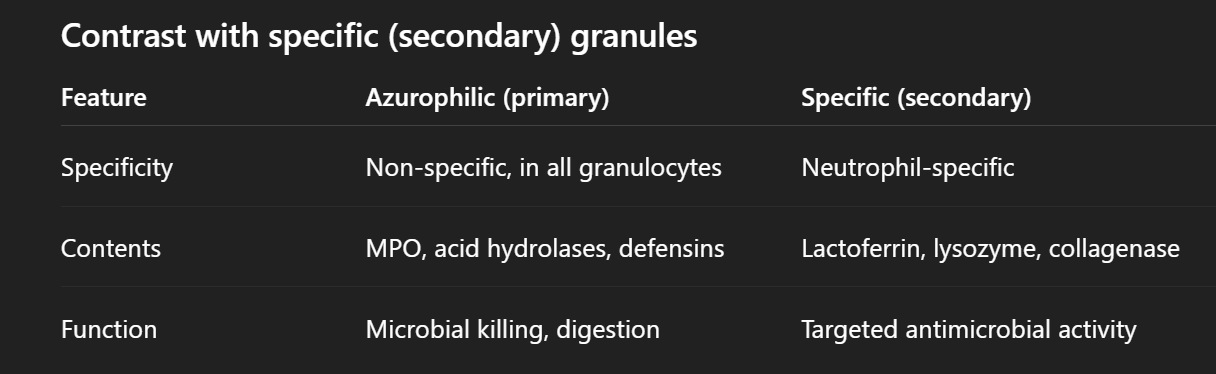
Blood smear
Differences between specific and non-specific granules (azurophilic granules):

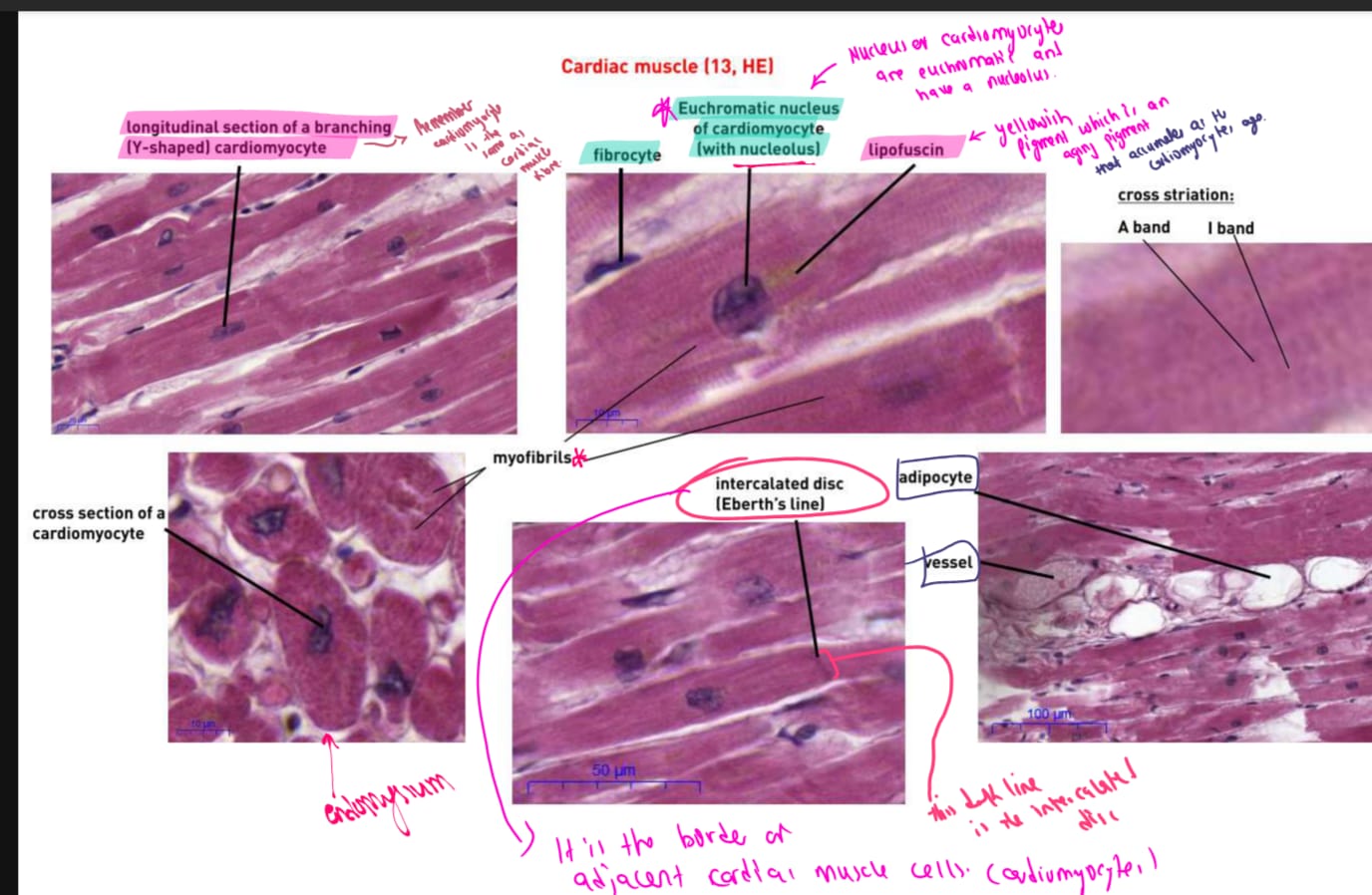
CARDIAC MUSCLE H&E

Definition
The mononuclear phagocyte system (MPS) is a network of phagocytic cells derived from monocytes that ingest and destroy pathogens, cellular debris, and foreign particles throughout the body.
Cells are mononuclear (single nucleus)
Derived from bone marrow monocytes
Key components / cells
Cell type | Location | Function |
|---|---|---|
Monocytes | Blood | Circulate and differentiate into macrophages in tissues |
Macrophages | Connective tissue | Phagocytosis, antigen presentation |
Kupffer cells | Liver | Phagocytose old RBCs, bacteria |
Alveolar macrophages | Lungs | Remove inhaled particles/pathogens |
Microglia | CNS | Immune surveillance in the brain |
Histiocytes | Connective tissue | Phagocytosis in tissues |
Osteoclasts | Bone | Bone remodeling (macrophage lineage) |
Functions
Phagocytosis – removal of microbes and debris
Antigen presentation – activate adaptive immunity
Secretion of cytokines – recruit other immune cells
Tissue repair – cleanup of damaged tissue
Exam-friendly line 📌
The mononuclear phagocyte system (MPS) is a network of monocytes and tissue macrophages that phagocytose pathogens and debris and help initiate immune responses.
Bile Flow Pathway
Bile canaliculi
Tiny channels between adjacent hepatocytes
Collect bile secreted by hepatocytes
Canals of Hering (intrahepatic bile ductules)
Small ducts that connect bile canaliculi to the interlobular bile ducts
Lined partly by hepatocytes and partly by cholangiocytes
Interlobular bile ducts
Found in the portal triads (with portal vein and hepatic artery)
Lined by cholangiocytes
Right and Left Hepatic Ducts
Collect bile from the respective lobes of the liver
Common Hepatic Duct
Formed by the union of the right and left hepatic ducts
Cystic Duct (optional pathway)
Connects to the gallbladder for storage
Bile can flow into the gallbladder or bypass it
Common Bile Duct
Formed by the union of the common hepatic duct and cystic duct
Carries bile toward the duodenum
Ampulla of Vater (hepatopancreatic ampulla)
The dilation where the common bile duct meets the main pancreatic duct
Major duodenal papilla
Opening into the second part of the duodenum
Controlled by the sphincter of Oddi
✅ Summary mnemonic (from hepatocyte to duodenum):
CanaliculI → Hering → Interlobular → Hepatic ducts → Common hepatic → Common bile → Ampulla → Duodenum
The neocortex has six histological layers, listed from superficial to deep:
Molecular layer (Layer I)
External granular layer (Layer II)
External pyramidal layer (Layer III)
Internal granular layer (Layer IV)
Internal pyramidal layer (Layer V)
Multiform (polymorphic or fusiform) layer (Layer VI)
Common mnemonic
“My Ex Girlfriend Is Pretty Mean”
Molecular
External granular
G (External pyramidal)
Internal granular
Pyramidal
Multiform
Clinical note
Layer IV is especially thick in primary sensory cortex
Layer V is especially thick in primary motor cortex (contains Betz cells)