Shock
Introduction to Shock and Pharmaceutical Interventions
Discussion on pharmaceutical agents used to treat shock.
Overview of key topics:
Fluid replacement agents (blood and blood products)
Review of crystalloids and colloids
Vasoconstrictors vs. vasopressors
Anotropic agents
Treatment for anaphylaxis
Definition of Shock
Shock is defined as the inability of the body to deliver oxygen to cells.
This lack of oxygen leads to the following:
Cells are deprived of oxygen and cannot function properly.
Organs become functionally impaired due to insufficient oxygen.
Eventually, if untreated, this results in tissue death and leads to organ failure and body death.
Key signs include:
Inadequate oxygenation or perfusion at the tissue level.
Types of Shock
Anaphylactic Shock
Most severe allergic response.
Causes massive vasodilation and blood pooling away from the core.
Results in decreased cardiac output and oxygen delivery.
Cardiogenic Shock
Caused by the heart's inability to pump effectively.
Decreased cardiac output leads to inadequate blood supply to tissues.
Hypovolemic Shock
Result of significant volume loss due to:
Trauma and bleeding (internal or external)
Dehydration
Insufficient fluid volume leads to inadequate tissue perfusion.
Neurogenic Shock
Results from brain or nerve damage affecting the vascular system.
Disruption in nerve pathways prevents adequate oxygen delivery.
Septic Shock
Severe reaction to infection from bacteria or toxins.
Causes widespread systemic response inhibiting oxygen delivery to tissues.
Medical Emergency Status of Shock
Shock is a medical emergency requiring immediate intervention.
Non-specific symptoms complicate diagnosis, necessitating thorough history-taking to determine type and cause of shock.
Early stages of shock can be reversible if addressed promptly.
Importance of Early Recognition and Intervention
Body compensates for shock initially but can decompensate quickly.
Key indicators to monitor include blood pressure, which changes based on underlying shock type.
Treat underlying causes quickly to prevent progression to multi-organ failure and death.
Therapeutic Approaches in Shock Management
Fluid Replacement Therapy
Crystalloids: Electrolyte solutions (isotonic or hypotonic) used to manage shock symptoms:
Rapid administration of normal saline or lactated ringers to restore volume.
Colloids: Solutions containing serum proteins that enhance oncotic pressure, pulling fluids back into vascular space.
Example: Albumin as a colloid.

Blood Products: Necessary if hypovolemic shock is due to significant bleeding.
Examples include whole blood, packed red blood cells, platelets, fresh frozen plasma.

Use of Vasoconstrictors and Vasopressors
Indicated for shock scenarios with poor blood pressure due to vasodilation or hypotension.
Rapid IV administration of agents like norepinephrine to increase vascular resistance and blood pressure.

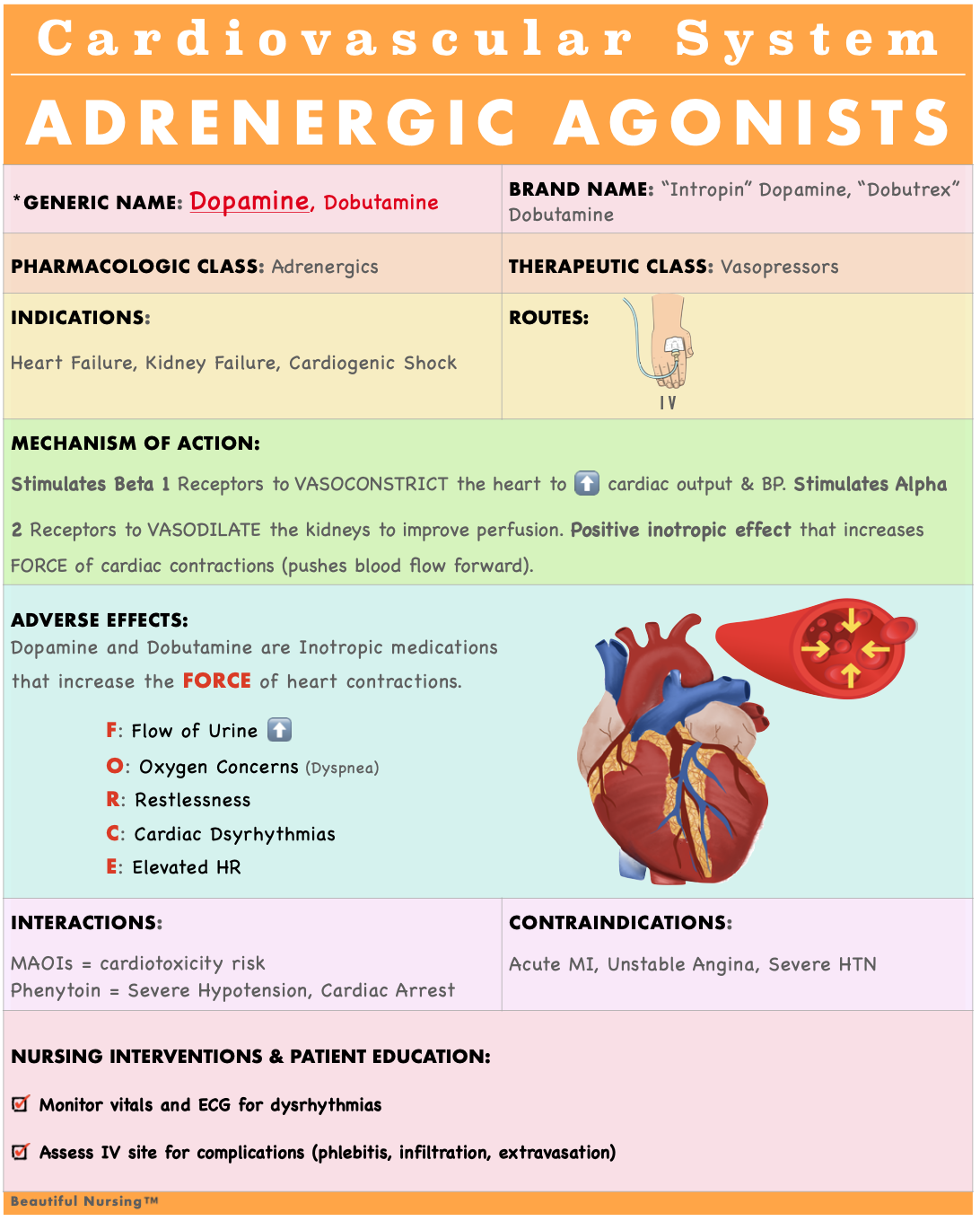
Inotropic Agents
Increased cardiac contractility, indicated in cardiogenic shock.
Common inotropic drug: dopamine for improving cardiac output.
Interventions for Anaphylaxis
Epinephrine: Emergency drug of choice during anaphylaxis.
Action includes bronchodilation, improving blood flow, and decreasing inflammatory response.
Follow-up medications may include antihistamines (diphenhydramine) and corticosteroids for prolonged management.

Nursing Considerations and Patient Education
Continuous monitoring of vital signs during fluid administration to avoid circulatory overload.
Patient Education:
Recognize signs of allergic reactions or circulatory overload (e.g., shortness of breath, edema).
Patients should report significant changes in status, especially symptoms of anaphylaxis.
Importance of offering pretreatment for mild to moderate allergic reactions before administering certain drugs.
Summary and Key Takeaways
Shock symptoms are non-specific; understanding underlying causes is crucial for effective intervention.
Critical interventions must prioritize identifying and correcting the cause to avoid irreversible consequences.
Emergency protocols and supportive care techniques, including BLS and ACLS, should be implemented as initial responses to shock situations.