Traumatic lesions in the CNS
Brain trauma is one leading cause of death of young adults in developed countries
Cause: traffic accidents, industrial accidents, or sports.
Cause of death in persons with head trauma is usually herniation due to mass effect, increased intracranial pressure.
Spinal trauma with the same causes is source of irreversible disability
Mechanism
1./Direct (the harmful agent affect directly the brain or spine, e.g. s bullet in the brain, strike on the head etc)
Indirect (acceleration or deceleration of the brain within the skull, e.g. by a car accident)
2,/ Closed (if the meninges are not opened to the environment, no dural tear, no CSF leak)
Open (if the intracranium opened, giving way to CSF leak out, and infectious agent into the skull)
Types of traumatic brain damage
Brain commotion
shaking of the brain within the skull, caused by direct or indirect, closed head trauma.
Symptoms:
brief unconsciousness (1-2 sec),
short amnestic period,
headache, dizziness, nausea, fatigue,
no focal signs.
No structural brain damage on CT or MR
Treatment: bedrest, painkillers (no specific treatment/hospitalisation)
Outcome: Usually total recovery in a few weeks.
Brain contusion
the brain smashed, when suddenly pushed to the inner surface of the skull,
causing structural brain damage,
oedema and haemorrhage
Symptoms: like in commotion,
with focal neurological signs,
condition is usually more severe
Dg: CT or MR demonstrates the
destroyed
brain tissue, haemorrhage and oedema.
Treatment: surgical removal of the
haematoma, osmodiuretics, supportive care
Outcome: varies on the severity of brain damage
Epidural bleeding.
(between the bone and the dura mater)
Arterial origin= usually rupture of the middle meningeal artery,
caused by temporal or parietal bone fracture
Symptoms: hyper-rapid development of severe symptoms (hemiparesis, anisochoria, decreased level of consciousness, coma or death)
Diagnosis: CT.
Treatment: urgent surgical removal, otherwise the patient dies in most cases.
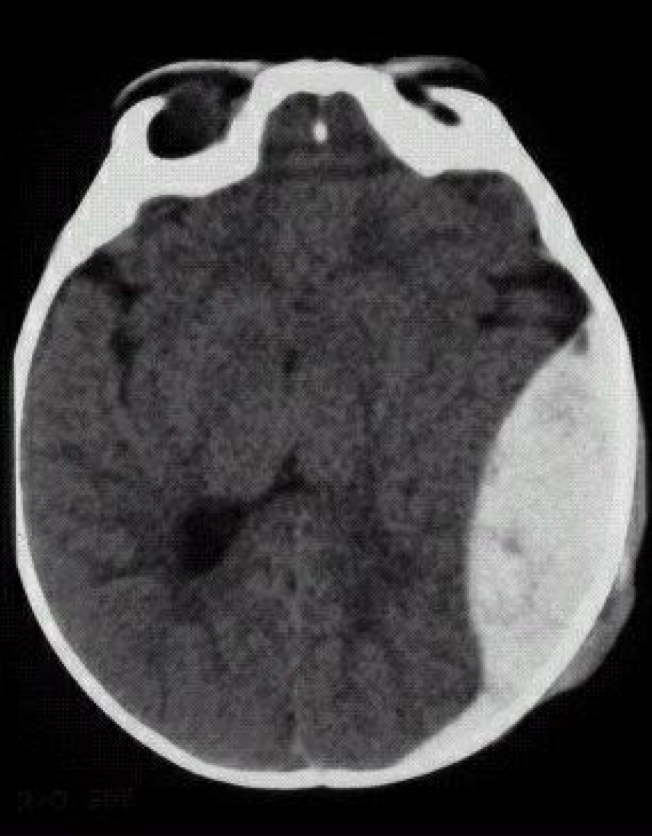
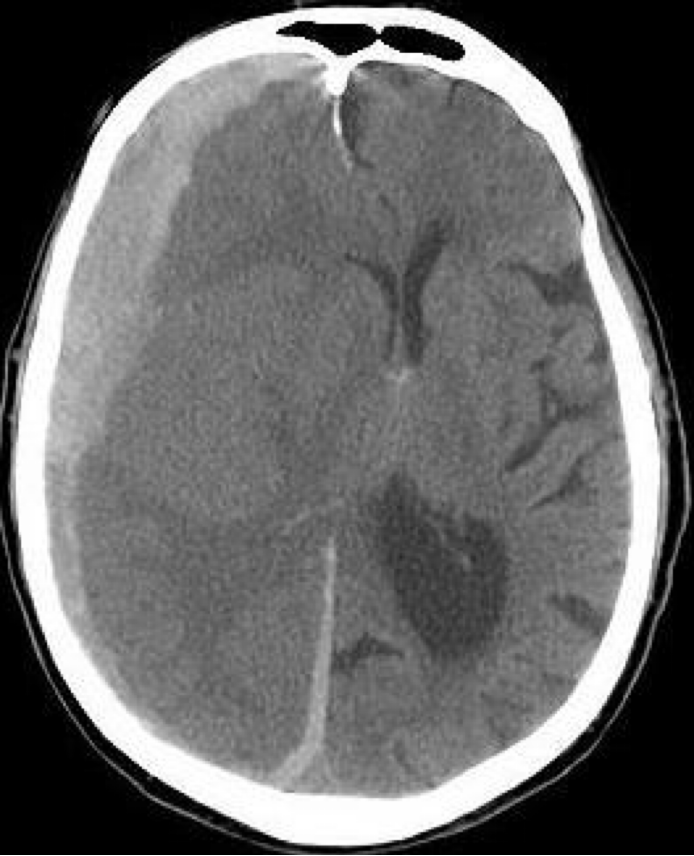
Subdural bleeding
(between the brain and dura mater)
acute, subacute, chronic
Variable latency of the development after head trauma: from hours to months.
Venous origin („bridging veins”, on the superior brain surface).
Skull fracture is not necessary.
Symptoms: less rapid, sometimes insidous growth.
non specific (headache, hemiparesis, dementia, seisures)
Diagnostics: CT.
Treatment: surgical removal.
1./ Posttraumatic epilepsy. Caused by the direct irritating effect of the haematoma on the brain cortex, or of the scar, formed after the healing of the brain contusion.
Early (within one week from injury)
Late (from one week to years)
2./ Prolonged headache.
3./ Fatigue.
4/. Irritability, concentration difficulties, depression.
5./ Personality changes
7./ Hormonal disorders.
8./Dementia (after repeated trauma, e.g. in contact sports)