Regulation of Stroke Volume and Heart Rate
autonomic nervous system regulates heart rate
sympathetic NS release noradrenaline plus circulating adrenaline from adrenal medulla, both act on B1 receptors on sinoatrial node, increases slope of the pacemaker potential, increases heart rate = tachycardia
parasympathetic NS, vagus nerve releases acetylcholine, acts on muscarinic receptors on sinoatrial node, hyperpolarises cells and decreases slope of pacemaker potential, decreases heart rate = bradycardia
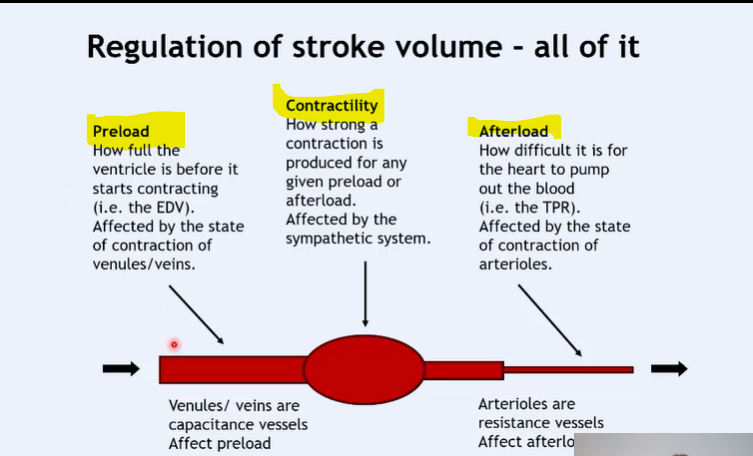
preload is affected by the end diastolic volume
increased venous return = increased EDV therefore increased stroke volume
decreased venous return = decreased EDV therefore reduced stroke volume
ensures self regulation - matches SV of left and right ventricles
afterload is the load against which the muscle tries to contract
if total peripheral resistances, stroke volume will go down (more energy is “wasted” building up enough pressure to open the aortic valve)
Cardiac output = heart rate x stroke volume
increases heart rate causes small increase in cardiac output but stroke volume starts decreasing
shortened cardiac interval cuts into rapid filling phase, reduced end diastolic volumes reduces preload and according to starling’s law, stroke volume is reduced
Control of cardiac output
HR increases via decreased vagal tone increased sympathetic tone
contractility increases via increased sympathetic tone alter ionotropic state and shortens systole
venous return increases…
total peripheral resistance falls…
cardiac output increases 4-6 times