Transport of oxygen and carbon dioxide
Adaptations of red blood cells
biconcave shape
increased surface area
no nucleus
able to transport more oxygen
Haemoglobin
4 polypeptide chains
each contains a haem prosthetic group
oxygen binds to these haem groups
Taking up oxygen
oxygen enters lungs
oxygen diffuses into blood plasma and enters the erythrocytes (RBC)
oxygen molecules bind to haemoglobin and are taken out of solution
oxyhaemoglobin
maintains a steep diffusion gradient so more oxygen can enter the bloood
Releasing oxygen
in the tissues oxygen is needed for respiration
oxyhaemoglobin must be able to release oxygen
dissociation
% saturation is a measure of how many oxygen molecules are bound
Oxyhaemoglobin dissociation curve
partial pressure
the relative pressure that a gas contributes to a mixture of gases
the more of a gas there is, the higher the partial pressure
units kPa
uptake/dissociation of oxygen produces an S shaped curve
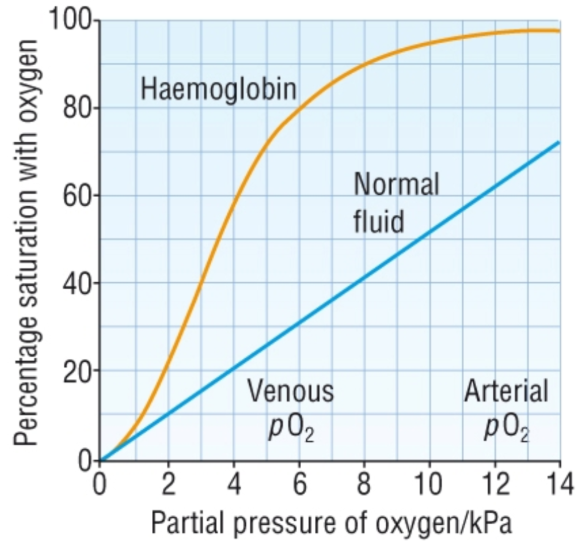
low pO2
difficult for first oxygen molecule to bind
pO2 increases
oxygen eventually binds
causes conformational change in haemoglobin molecule shape
easier for further oxygen molecules to bind
affinity of haemoglobin for oxygen increases
positive co-operativity
high pO2
curve levels off as last O2 molecule is more difficult to bind
eventually haemoglobin is fully saturated
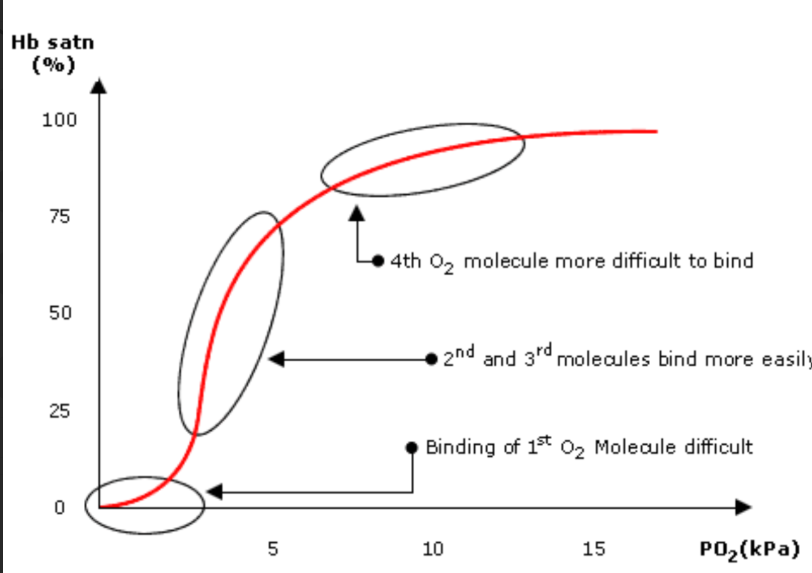
pO2 in lungs is enough to allow almost 100% saturation
pO2 in respiring tissues is low enough for oxygen to dissociate easily from the oxyhaemoglobin
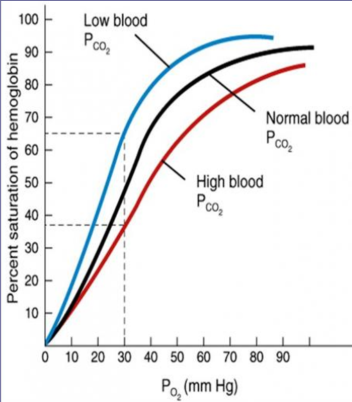
Bohr shift
low blood pCO2
haemoglobin picks up O2 easily
high blood pCO2
haemoglobin gives up O2 easily
curve shifts right with increasing pCO2
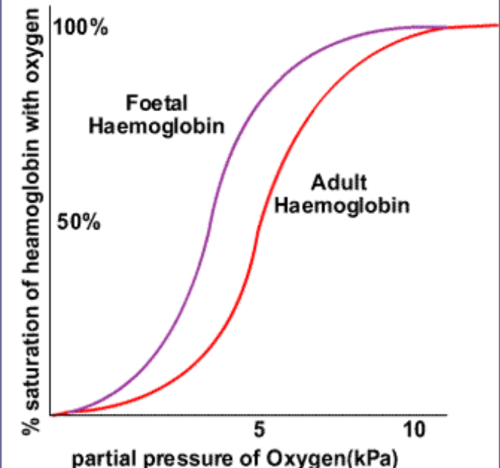
Foetal haemoglobin
foetal haemoglobin has a higher affinity for oxygen than maternal haemoglobin
oxygen passes to the foetus from the mother
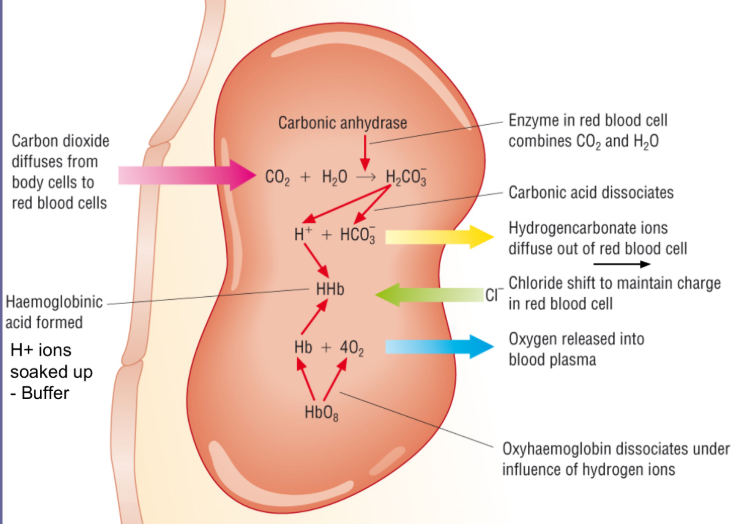
Transport of CO2
carbon dioxide produced by the respiring tissues is transported to the lungs to be removed during exhalation
5% dissolved in plasma
10-20% as carbaminohaemoglobin
75-85% as hydrogen carbonate ions in the cytoplasm of RBC
Transport of CO2 has hydrogen carbonate ions
at respiring tissues (pCO2 is high)
CO2 reacts with water carbonic acid (H2CO3)
catalysed by carbonic anhydrase
H2CO3 dissociates to form H+ and HCO3- ions
H+ binds to haemoglobin forming haemoglobinic acid
causes haemoglobin to release oxygen
prevents blood from becoming too acidic (H+ ions lower pH) so act as buffer
causes the Bohr effect
haemoglobin releases oxygen so it can diffuse into respiring tissues
chloride shift
HCO3- ions leave RBC and are transported via plasma while chloride ions enter RBC
maintains charge balance by preventing excessive positive charge in RBC
at the lungs (low pCO2)
HCO3- and H+ ions reform CO2
CO2 diffuses out of body via expiration