CVS Overview
Identify the heart, blood vessels, and blood as the three principal
components of the CVS. Describe the anatomy and histological features of the heart, blood vessels and blood as the primary components of the cardiovascular system (CVS). Explain how the structural organization of the three major components of the
CVS supports its physiological function (e.g., myocardium in the heart,elasticity in arteries, viscosity of blood).
Heart - pumps blood around the body in two pumps with two functions. A myocardium which allows for forceful contractions
systemic circulation - comprises blood flow through the left heart & systemic blood vessels. left ventricle pumps O2 rich blood to all body organs using veins and aorta
pulmonary circulation - comprises blood flow through right heart & pulmonary blood vessels. right ventricle pumps O2 poor blood to the lungs using vena cava and arteries
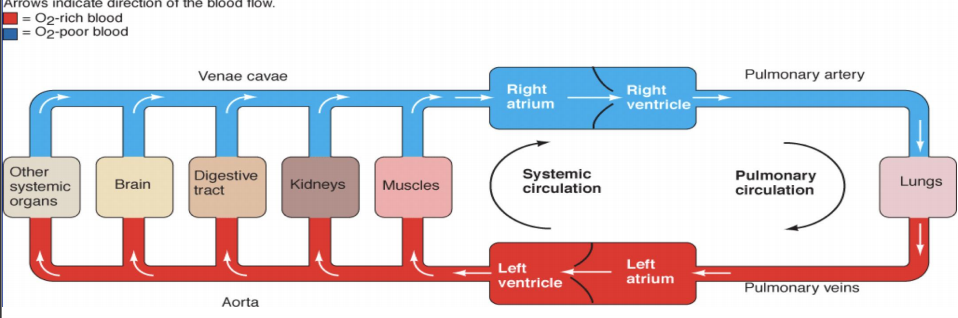
Blood vessels - tubular structures that transport blood and serve as closed system of delivering blood to and from tissues for nutrient and waste exchange. When the resistance changes in arterioles, blood flow to the organ is altered.
arteries - have high pressure and contain relatively small amounts of blood volume; carry blood from heart to the body tissues through arterioles
veins - have low pressure and contain the largest % of blood volume; carry blood from tissues back to heart through venules
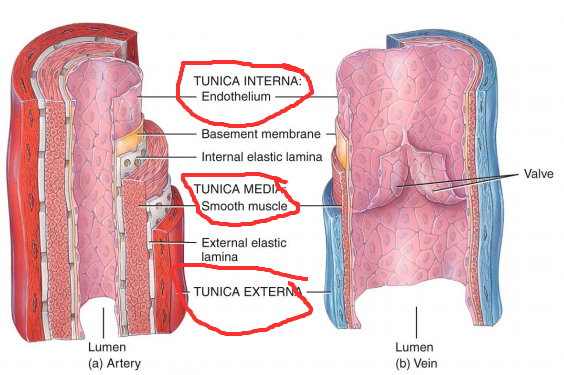
capillaries - thin walled blood vessels interposed between arteries and veins within the tissues and are the actual sites of exchange of nutrients, waste, and fluid while resting on basal lamina
Structure - Vessel wall consists of 3 layers (intima, media, and adventitia) which are made of endothelial cells, elastic fibers, collagen fibers, smooth muscle cell. Inside intima fibroblasts, nerve endings, blood cells, other extracellular components.
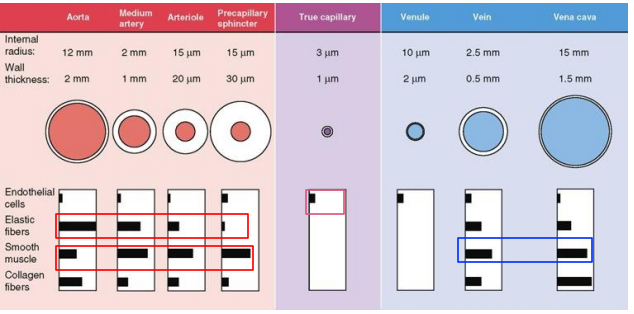
Blood - liquid connective tissue that transports dissolved blood gases immune cells, platelets
55% liquid plasma (water,proteins,solutes) and 45% cellular
includes RBC as oxygen transporters (erythrocytes), WBC as immune defense (leukocytes) and platelets as nutrient,hormone, and waste carriers (thrombocytes)
Explain the transition from high-pressure arteries to low-pressure veins and how this supports efficient circulation and nutrient exchange.
As blood flows through the pressure difference between the inlet and outlet vessel allows for serial compartments that feed in sequence of parallel compartments that feed individually.
Serial has total resistance equal to the sum of all resistances from arteries to arteriole to capillary to venule to vein. Parallel has 1/total resistance equal to the sum of 1/all resistances added together.
Explain how blood flow is directly proportional to the pressure gradient and inversely proportional to vascular resistance
Ohm’s law =
Magnitude of blood flow (Q) is directly proportional to the size of the pressure difference (ΔP) with the direction of flow is always from high to low. Blood flow from the left ventricle into the aorta and then from vena cava into right atrium. Q is inversely proportional to the resistance (R), thus increasing resistance by arteriolar vasoconstriction decreases flow and vasodilation increases flow
Discuss how resistance is influenced by factors such as blood viscosity, vessel length, and especially vessel radius (Poiseuille's Law).
Resistance (R) directly proportional to viscosity (η) of the blood and length (L) of blood vessels. Resistance inversely proportional to the radius (r4) of the blood vessel
Apply this understanding to explain conditions like hypertension or shock.
Hypertensive - increased resistance from vasoconstriction raising the pressure.
Shock - collapse in pressure gradient or vessel tone reducing flow.
Hemodynamics is the study of physical variables that define the containment and flow of blood. Laminar flow is orderly, streamlined, and ideal while turbulent flow occurs when disruption or irregularities occur at valves or clots. Turbulence does not occur until flow velocity is 2000+ to break lamina flow apart such as at branch point of large arteries, diseased and narrower arteries, and heart values (ASCVD/hyperlipidemia)
v = mean velocity, 2r = vessel diameter, P = blood density= n = blood viscosity
Estimate blood pressure from cardiac output, stroke volume, heart rate, and total peripheral vascular resistance
Blood pressure - force of circulating blood on the walls of the arteries, higher in the systemic arteries than pulmonary veins. arteries elastic due to the lamina while veins are like reservoirs
Cardiac Output (CO) - volume in L of blood pumped by heart per minute and a product of heart rate (beats/min) and stroke volume (volume/heartbeat)
CO at rest is 5 L/min in a 70 kg human
Relate mean arterial pressure (MAP) to cardiac output and total peripheral
resistance TPR
Use these formulas to conceptually estimate how changes in heart rate, stroke volume, or vascular tone effect blood pressure.
Anything that alter CO and TPR will alter MAP such as; autonomic nervous system,vasoactive substances,venous return,local metabolic activity , autoregulation
Ejection fraction (EF%) - measures how much blood of the total amount in the left ventricle is pumped out with each contraction and is normally 55 and 70%.
Low EF% shows signs of impaired contractility reducing SV and CO leading to lower BP and potential tissue hypoperfusion
Short-term: Baroreceptor reflex, autonomic nervous system
(sympathetic and parasympathetic eFFects)
Baroreceptors (carotid sinus and aortic arch), chemoreceptors, and low pressure receptors give neural input to vasomotor center in brainstem for analysis and determination of discharge by autonomic nervous system occur. May cause CO and TPR to adjust to keep MAP in normal range and changing HR and vessel diameter
Long-term: Renin-Angiotensin-Aldosterone System (RAAS), renal
regulation of blood volume
A decrease in blood volume causes BP to reduce which is sensed by juxtaglomerular cells of kidney to release renin. Renin converts angiotensin to angiotensin I then angiotensin-converting enzymes (ACE) converts I to II.
Angiotensin II serves as a vasoconstriction on adrenal cortex to release aldosterone to reabsorb sodium and water and increase K+ concentration in blood to raise BP back to normal levels.
Kidneys adjust blood volume by managing water and sodium excretion.
Describe the influence of vasoactive substances, venous return, active hyperemia on blood flow and on blood pressure,
Vasoactive substances - released from various cells and tissues in body like endothelium, endocrine glands, heart myocytes that may affect vascular smooth muscle tone.
Vasoconstrictors (catecholamines, angiotensin II, vasopressin, endothelin, thromboxane A2) will increase TPR and MAP.
Vasodilators (prostacyclin, nitric oxide, ANP) decrease TPR and MAP
Venous Return - serves a reservoir for the circulatory system and help regulate CO by way changing volume of blood that flows from systemic veins to right atrium every minute.
healthy heart pumps all blood returned to it CO=VR, but things like dehydration, hemorrhage, SNS, skeletal muscle and respiratory activity change VR and MAP.
Active Hyperemia - each tissue has the intrinsic ability to control its own local blood flow in proportion to their metabolic needs, thus can cause local chemical changes that can mediate metabolic vasodilation due to increased blood flow from increased activity.