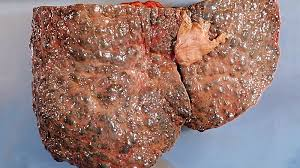
Wound Healing
Tissue Repair
Inflammation serves to remove the danger which is usually associated with tissue damage and death. This is a potential source of infection and impairs tissue repair. Dead tissue must be removed and or repaired. Damaged tissue can either be replaced like “new” or with a scar (“repair from Wish”). Tissue repair must be well controlled. If repair is excessive, new medical issues may arise (excessive scar formation = keloids/liver cirrhosis).
Tissue regeneration: lost tissue regrows, and occurs in tissues with high turnover (skin, gut, bone marrow), this rarely happens in organs with the exception of the kidneys and liver but this depends on the intact tissue scaffold. Requires that “tissue stem cells” survive.
Healing: a combination of regeneration and scar formation (replaced with fibrous tissue).
Regeneration and healing require tissue stem cells.
Growth Factors and Cytokines in wound healing
Growth factors and cytokines act as regulators.
Macrophages are believed to be the architects of wound healing and tissue repair.
Growth Factors affect cell proliferation, cell migration, angiogenesis, tissue matrix formation, and the deposit of collagen (fibrosis)
Wound Healing is a Multistep Process
- Inflammatory Phase: (24 hrs) Removal of damaged or dead tissue; neutrophils
- Proliferative Phase: (3-7 days) angiogenesis, granulation tissue formation, wound contraction; Macrophage
- Maturation: (weeks) tissue remodeling (collagen), removal of unneeded cells through apoptosis, reconstruction of the extracellular matrix, fibrous union
Types of Healing
Uncomplicated: (1st intention) edges are close, not infected, scabbing (epithelization) of the wound surface, angiogenesis, fibroblast and collagen deposition, remodeling, “good as new”
Complicated: (2nd intention) more significant gaps (infected wound, more tissue damage, foreign body), more inflammation, more granulation tissue, wound contraction becomes important mediated by myofibroblasts that contract at edges, healing is usually less than perfect and leaves a scar.
Locally impairs repair: impaired perfusion, infection, foreign body, hematomas (blood clots), denervations, necrotic tissues, mechanical stress, type of tissue, surgical technique
Systematically impairs repair: age, pre-existing conditions (diabetes, malnutrition, atherosclerosis), drugs (steroids, chemotherapy), genetic disorders, trauma, vitamin deficiency
Healing is incomplete (deficient scar)
Wound Dehiscence: edges of wound separate (re-open)
Ulcer formation: wound does not heal, no scab
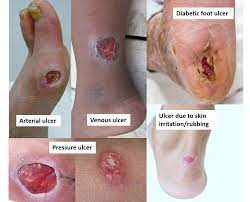
Excessive Scar Formation
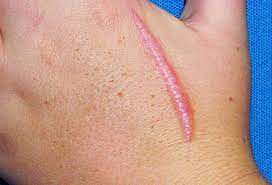
Hypertrophic scar: raised scar tissue that remains within the boundaries of the original wound
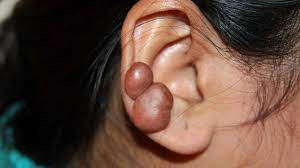
Keloid: overgrowth of scar tissue beyond the original wound
Aggressive: desmoid tumor (aggressive fibromatosis), benign tumors, but can grow aggressively and invade surrounding tissue, NOT cancer, and does not metastasize
Wound Contractions
after burns, tissue contracts
Result of continuous inflammation stimulus
Fibrosis (liver cirrhosis)